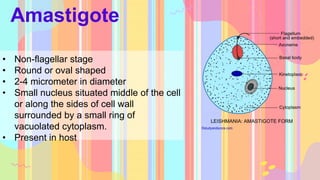
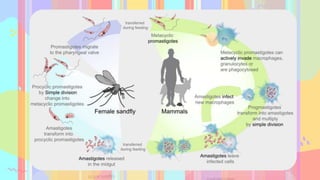
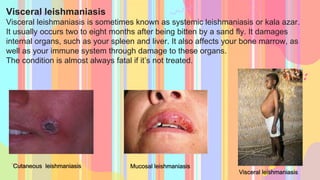
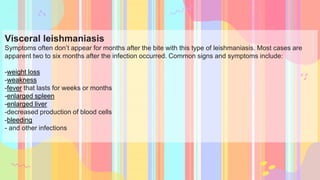
Leishmania is a genus of protozoan parasites that causes leishmaniasis, a significant vector-borne disease transmitted by sandflies. The lifecycle involves two hosts: a definitive host (humans) and an intermediate host (sandflies), with several forms of the disease including cutaneous, mucocutaneous, and visceral leishmaniasis. Preventative measures focus on avoiding sandfly bites through protective clothing, repellents, and environmental controls.