Heart disease and symptoms of its and clinical role
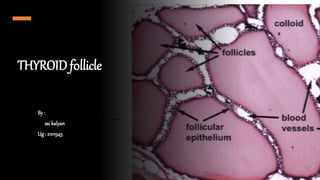
- 1. THYROID f0llicle By : saikalyan Ug : 2101945
- 2. Introdction : • The thyroid gland is a vital butterfly- shaped endocrine gland situated in the lower part of the neck • The thyroid gland, located anterior and inferior to the larynx, consists of two lobes united by an isthmus. • Each lobule contains a cluster of follicles, which are the structural and functional unit.. • It synthesizes the thyroid hormones thyroxine (tetra-iodothyronine or T4) and tri-iodothyronine (T3),
- 3. Microscopic structure of thyroid follicle • Follicle consist of layer of simple epithelium, enclosing cavity called the follicular cavity. • The cavity is usually filled with gel-like viscous iodine-rich material called colloid. • Interfollicular spaces are filled by reticular connective tissue, adipose tissue and blood vessels.
- 4. HISTOLOGY & COMPOSTION : • The parenchyma of the thyroid is composed of millions of rounded epithelial thyroid follicles of variable diameter, each with simple epithelium • thyroid follicle is surrounded by thin connective tissue stroma rich in fenestrated capillaries • The colloid stains pink with haematoxylin and eosin (H&E) staining, while the follicular cells have a purple appearance. • Among endocrine glands, thyroid is unique as it stores large quantity of its hormonal secretion extracellularly as colloid.
- 5. State of the follicle Linning epithelium Amount of collid Inactive /resting squamous abundant active cuboidal moderate Highly active Low columnar scanty Thyroid follicle at different levels of activity
- 6. Synthesis of Thyroid Hormone • Thyroid hormone synthesis begins with the recognition of thyroid-stimulating hormones (TSH) by TSH-receptors at the basolateral region of the follicular cells. • iodine is taken into the cell via Na+/I- symporters. • Iodine is used in the organification of tyrosine in the follicular lumen to form monoiodotyrosine (MIT). • MIT can then be organified to form diiodotyrosine (DIT). The enzyme thyrosine peroxidase (TPO), can subsequently link a MIT and a DIT molecule to form triiodothyronine (T3) or two DIT molecules to form thyroxine (T4).
- 7. Graves' Disease : • Graves disease is an autoimmune disorder that leads to an overactive thyroid gland (hyperthyroidism). • Due to the production of autoantibodies against the TSH receptor on the follicular epithelial cells. • These antibodies mimic the effects of TSH and cause overproduction and release of thyroid hormone. • The epithelial cells in this patient no longer surround round follicles of colloid. • these follicles are disappearing and the colloid is becoming depleted. Compare to normal thyroid. .
- 8. hypothyroidism • Hypothyroidism happens when the thyroid gland doesn't make enough thyroid hormone. This condition also is called underactive thyroid. • The thyroid parenchyma extensive infiltration of lymphocytes, leading to the destruction of thyroid follicles. • lymphocytes form aggregates, leading to the development of lymphoid follicles with germinal centers, which are a hallmark of the autoimmune response • phagocytose the degenerating thyroid follicular cells resulting destruction of the follicular architecture and impaired hormone synthesis.
- 9. References : • Histology, thyroid gland - statpearls - NCBI bookshelf. (n.d.-b). https://www.ncbi.nlm.nih.gov/books/NBK551659/ • Professional, C. C. medical. (n.d.-a). Hypothyroidism: Symptoms, causes, treatment & medication. Cleveland Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/12120- hypothyroidism • Loscalzo J, et al., eds. Hypothyroidism. In: Harrison's Principles of Internal Medicine. 21st ed. McGraw Hill; 2022. https://accessmedicine.mhmedical.com • Hypothyroidism. National Institute of Diabetes and Digestive and Kidney Diseases. https://www.niddk.nih.gov/health- information/endocrine-diseases/hypothyroidism . • Ross DS. Diagnosis of and screening for hypothyroidism in nonpregnant adults. https://www.uptodate.com/contents/search .