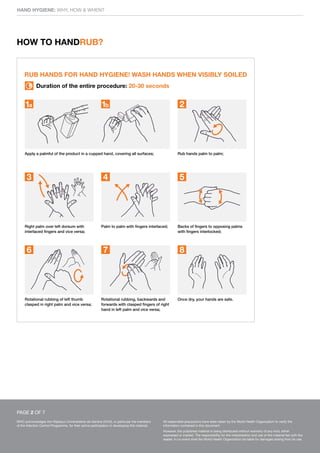
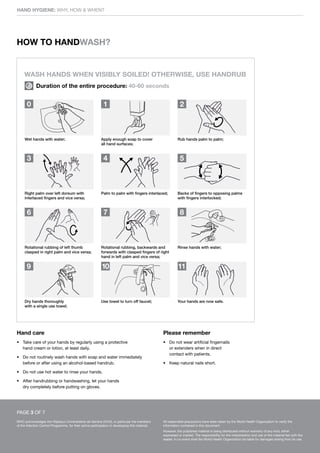
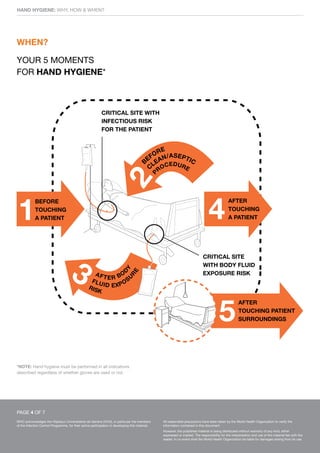
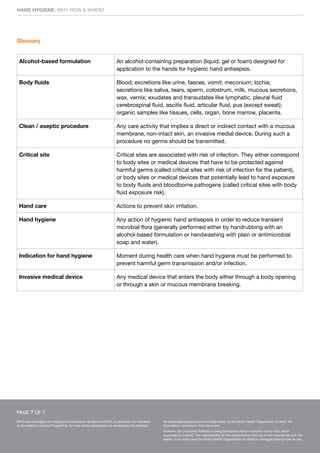
This document discusses hand hygiene in healthcare settings. It explains that hand hygiene is the most important way to prevent the transmission of harmful germs and healthcare-associated infections, as hands are the main way germs spread. It describes how and when healthcare workers should clean their hands, either by rubbing with an alcohol-based handrub if hands are not visibly dirty, or washing with soap and water if dirty. The five key moments for hand hygiene are outlined as before touching a patient, before clean procedures, after body fluid exposure risks, after touching a patient, and after touching the patient's surroundings. Glove use does not replace hand hygiene.