GROUP NO 2 PPT.pptx
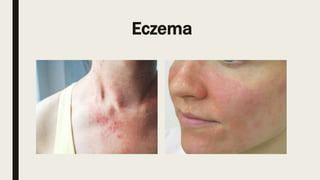
- 1. Eczema
- 2. Group Members • HUMAIRA MUSHTAQ • ROOFIA MUJTABA KHAN • SABAAMANULLAH • SAMEERAAHMED • SARA SHAH • SANIA SOHAIL • SYEDA RAMEESHA RIZVI • WAJIHA DILSHAD • YUSRA SHUJA • ZOHA HABIB • ZOHA KHALID
- 3. INTRODUCTION ■ A condition where patches of skin become inflamed, itchy, red, cracked and rough. ■ Interchangeable terms ‘eczema’ and ‘dermatitis’. ■ “Eczema” meaning ‘to boil’ describes the characteristic tiny bubble like blisters of the condition. ‘Dermatitis’ means ‘inflammation of the skin’. ■ A common convention is to describe as: ‘eczema’ those that are endogenous or constitutional. ‘dermatitis’ those that are exogenous or due to contact.
- 4. PATHOPHYSIOLOGYAND CLINICAL FEATURES ■ The histological features of eczema/dermatitis are similar, regardless of cause and differ in the acute and chronic phases. ■ In acute stage, fluid escapes from dilated dermal blood vessels to produce edema, or swelling in the epidermis. ■ This collects into vesicles or tiny blisters, particularly where the skin is thick, as on the palms and soles causing exudation and crusting. ■ The chronic stage shows less edema and vesiculation and more thickening of the epidermis and horny layers. ■ These layers produced by prolonged rubbing and scratching by the sufferer.
- 5. TYPES OF ECZEMA 1. ACUTE ECZEMA/DERMATITIS: – Red, hot, swollen and itchy skin. – Papules and tiny blisters, sometimes coalesce to form large ones. – Exudation and crusting. – Scaling.
- 6. TYPES OF ECZEMA 2. CHRONIC ECZEMA/DERMATITIS: – Drier skin, becoming more scaly. – Lichenification ( dry, thickened, leathery skin with exaggerated skin markings, due to rubbing and scratching). – Painful fissures.
- 7. CLINICALTYPES 1. ATOPIC ECZEMA: – Common skin disorder of childhood. – Term ‘atopy’ describes an exaggerated susceptibility to form IgE to allergen. – Etiology genetic, environmental and immunological factors. – Epidermal Langerhans cell have high-affinity IgE receptors through which theT-helper cells release cytokinin and produce skin inflammation. – Mostly affects the face and flexures like front of elbows and wrist.Also affects the back of knees. – Detected by radio-allergosorbent test.
- 8. CLINICALTYPES – Epidermal Langerhans cell have high-affinity IgE receptors through which theT-helper cells release cytokinin and produce skin inflammation. – Mostly affects the face and flexures like front of elbows and wrist. Also affects the back of knees. – Detected by radio-allergosorbent test.
- 9. CLINICALTYPES Provoking Factors Extreme Temperature Irritants: soap, detergents, shower gels Stress Infection (bacterial or viral) Allergens (contact, food, inhaled, airborne)
- 10. CLINICALTYPES 2. CONTACT DERMATITIS There are 2 types of contact dermatitis: Contact Dermatitis Allergic (cell mediated immune or type IV reaction Primary irritant (wear and tear or irritation)
- 11. CLINICALTYPES Allergic contact dermatitis ■ Usually hands. ■ Burning, pruritus, pain. ■ Dry and fissured skin. Irritant contact dermatitis ■ Usually exposed areas of skin. ■ Pruritus is dominant symptom. ■ Vesicles and bullae.
- 12. CLINICALTYPES a) ALLERGIC CONTACT DERMATITIS: CAUSES: Metal e.g. nickel Topical medicaments (antibiotics, antihistamines and local anesthetics); creams, ointment bases and preservatives Dyes Plants Rubber compounds In industry: resins, plastics and cement frequently cause problems.
- 13. CLINICALTYPES DIAGNOSIS: First and most important step is: • Detailed history • Note the pattern and distribution of rash Common patterns include: • Metal fastenings in clothes such as zips and jeans studs (nickel allergy) • Gloves • Rash around eyes indicate airborne allergens from plants, nail varnish or strike anywhere matches (which release phosphorous sesquisulfide vapor) • Allergens in local application of medicaments
- 14. CLINICALTYPES If confirmation or further investigation is required, patch testing is useful. • The skin is examined for an eczematous reaction under the test patches at 48 hours and 96 hours, which indicates delayed hypersensitivity. • Once the allergy is confirmed, – Must avoid the allergen – Since this type of allergy is lifelong – And dermatitis persists as long as contact continues.
- 15. CLINICALTYPES b) PRIMARY IRRITANT DERMATITIS CAUSES: Common cause of hand eczema, particularly seen in housewives, nurses, hairdressers, caterers and those who work with oils and greases in industry. It occurs due to contact with anything that dehydrates the skin and removes the natural protective oils from the skin, allowing evaporation of water and penetration of irritants.
- 16. CLINICALTYPES DIAGNOSIS: No allergy is involved in this type and therefore patch testing is not usually indicated unless a co-existing allergy is suspected.
- 17. OTHER ECZEMAS 1. SEBORRHOEIC ECZEMA: • This involves areas of the body with a high density of sebaceous glands. • Areas it involves are face, scalp and upper trunk. • It occurs after puberty when these glands become active. • It is due to an overgrowth pityrosporum , a yeast that is normal commensal on the skin. • The skin is red with greasy yellow scales and the scalp shows severe dandruff.
- 18. OTHER ECZEMAS 2. DISCOID ECZEMA: • As the name suggests, this occurs in circular patches. • These characteristically occur on the forearms and lower legs and are intensely itchy. • They are frequently excoriated and become secondarily infected.
- 19. OTHER ECZEMAS 3. STASIS ECZEMA: • This is usually the result of varicose veins, venous stasis and edema in the lower leg. • It is particularly around the ankle and may progress to varicose ulceration. • The patient with varicose eczema is particularly at risk of developing allergic contact dermatitis to topical medicaments such as antibiotics and vehicles.
- 20. OTHER ECZEMAS 4. ASTEATOSIS ECZEMA: • This means “lacking in oil”. • It is typically found in elderly in whom the skin becomes over dry, perhaps aggravated by the use of soap.
- 21. TREATMENT The same basic principles of treatment apply regardless of the type of eczema. 1. EMOLLIENTS: • The mainstay of eczema treatment is the use of liberal quantities of moisturizers as, in all types. • Adequate use of emollients will reduce the requirement of typical steroid, both in quantity and potency. • A soap substitute such as emollient cream should be applied before, during and after bathing.
- 22. TREATMENT 2. TOPICAL CORTICOSTEROIDS: • Eczema is an inflammatory and immunological condition. So treatmemts must be anti inflammatory and directed at modifying the immune response, which in many case means corticosteroids mostly topical • Topical steroids developed over the past 50 years have revolutionised the treatment of inflammatory dermatitis but, it is apparent that with great potency greater will be the chances of adverse effects.
- 23. TREATMENT • For e.g.: Epidermal Atrophy ( thinning), telangiectasia ( prominent surface blood vessels ), striae ( stretch marks), and premature aging due to collagen loss. Reduce growth rates in children after prolonged use have been reported. • As a result primary care doctors and their patients are now only too well aware of the potential hazards of steroid usage. • The aim of topical steroid therapy is to control the eczema using a potent application if necessary, under close supervision, and then to maintain control using a drug of lowest effective potency.
- 24. TREATMENT 3. OTHERTOPICAL IMMUNOMODULATORS: • Two calcineurin inhibitors have been introduced for the treatment of atopic eczema. • Calcineurin is a cytotoxic enzyme involved in activation ofT-lymphocytes. • Macrolide antibiotics, tacrolimus, pimecrolimus are of low molecular weight to penetrate the stratum corneum of the skin, particularly when its barrier function is impaired in eczema.
- 25. TREATMENT a)TACROLIMUS: It is comparable in efficacy to potent topical steroids. It is available only as an ointment. It may produce a burning sensation in the skin at the beginning of the treatment. Systemic absorption is negligible.
- 26. TREATMENT b) PIMECROLIMUS: It is less potent then tacrolimus but penetrate stratum corneum more efficiently. It is available as a cream. It appears to inhibit flares of atopic eczema.
- 27. TREATMENT 4. ANTIBIOTICS: • Swabs should be taken from infected patient before starting oral antibiotics. • Choice of antibiotics to cover Staphylococcus aureus is erythromycin or flucloxacillin, should be given for 10 days. • Chronic infection require long term treatment. • Herpes simplex virus should be treated with acyclovir.
- 28. TREATMENT 5. DRYINGAGENTS: • In vesicular or weeping eczema the blister and oozing areas are dried using potassium permanganate baths, soaks or wet compresses. • Crystals or tablets are added to warm water to produce purplish-pink color. • Skin soaked for at least 15 minutes. • This appears to have astringent and antiseptic defect.
- 29. TREATMENT 6. ANTI HISTAMINES: • Pruritus is one of the distressing feature of eczema which can be treated from the short term use of sedative anti-histamine at night.
- 30. TREATMENT 7. COAL FOR PREPARATIONS: • Tar is an effective antipruritic. • Tar creams and ointments are useful in treatment of discoid eczema.
- 31. TREATMENT 8. BANDAGING: • In atopic eczema, bandages can be used to prevent scratching and to keep ointments and creams in contact with the skin. • A wet wrapping bandage is also a technique made up of emollient and steroids and used to keep inner layer of skin moist and gives soothing effect. • To control varicose eczema, compression bandaging or graduated support stockings are probably used.
- 32. TREATMENT 9. TOPICAL IMIDAZOLES: • Many imidazole drugs are used to treat eczema. • Ketoconazole is most widely used to reduce the population of pityrosporum ovale and controls seborrhoeic eczema and dandruff. It is available in shampoo or creams.
- 33. TREATMENT 10. SYSTEMICTHERAPIES: a) Systemic steroids: Oral corticosteroids are used as a short term treatment in acute eczema which is now very rare. This type of management is required in conditions like acute exacerbation eczema, acute allergic contact dermatitis and erythrodermic eczema. of atopic
- 34. TREATMENT b) Cyclosporine: It is an immunosuppressant drug extremely effective in the treatment of chronic eczema mainly used in adult patients and also in children. ItsTherapeutic range is 2.5-5mg/kg. When the drug is stopped, eczema may tends to relapse and to avoid such cases intermittent courses can be very useful. Its adverse reactions include hypertension and renal impairment. There are number of drugs that interact with cyclosporine and must be used with caution. Topical preparation of cyclosporine cannot be used to treat eczema due to poor skin penetration.
- 35. TREATMENT c) Azathioprine: It is an antimitotic drug used as steroid sparing agent to treat severe resistant eczema at a dose of 50-150mg per day. It acts more slowly than cyclosporine but widely used for long term treatment. It suppresses bone marrow and proper monitoring should be done with regular blood tests.
- 36. TREATMENT d) Other immune modulators: Interferon-gamma has been used in cases of severe refractory eczema and includes unpleasant flu like side effects. Methotrexate has also been used in unresponsive adult atopic eczema but has never been evaluated in clinical trials.
- 37. TREATMENT e) Evening primrose oil: It is used to treat resistant eczema especially where extreme dryness is the major problem.
- 38. TREATMENT 11. PHOTOTHERAPY:- • PUVA - for atopic patients. • UVB - in dry stage. • Narrow band UVB therapy is effective ans safer than PUVA. • Side effects:- burning, premature ageing and increase risk of cancer.
- 39. TREATMENT 12. OTHERTHERAPIES:- • DIET: under supervision of a dietitian. • CHINESE HERBAL MEDICINE: According to patients conditions. • ALTERNATIVETHERAPIES: hypnotherapy, yoga, psychotherapy.
- 40. PATIENT CARE ■ Effect on life of patients - appearance, loss of sleep. ■ Advice. ■ Cool cotton clothing - suitable for eczema. ■ House dust mite precautions. ■ Emollient application. ■ Exposure to water, detergents, oils, greases, degreaser may result in recurrence.