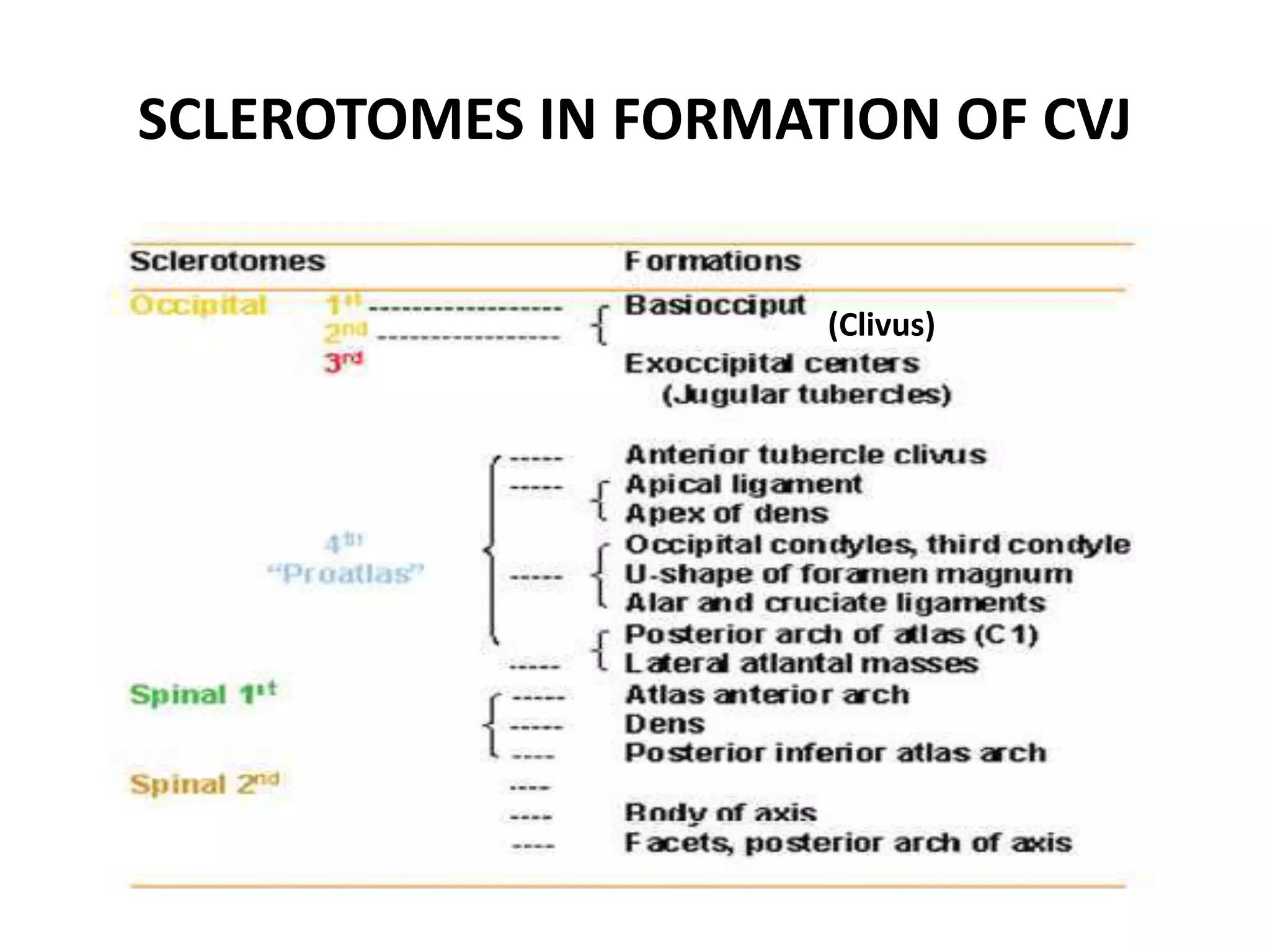
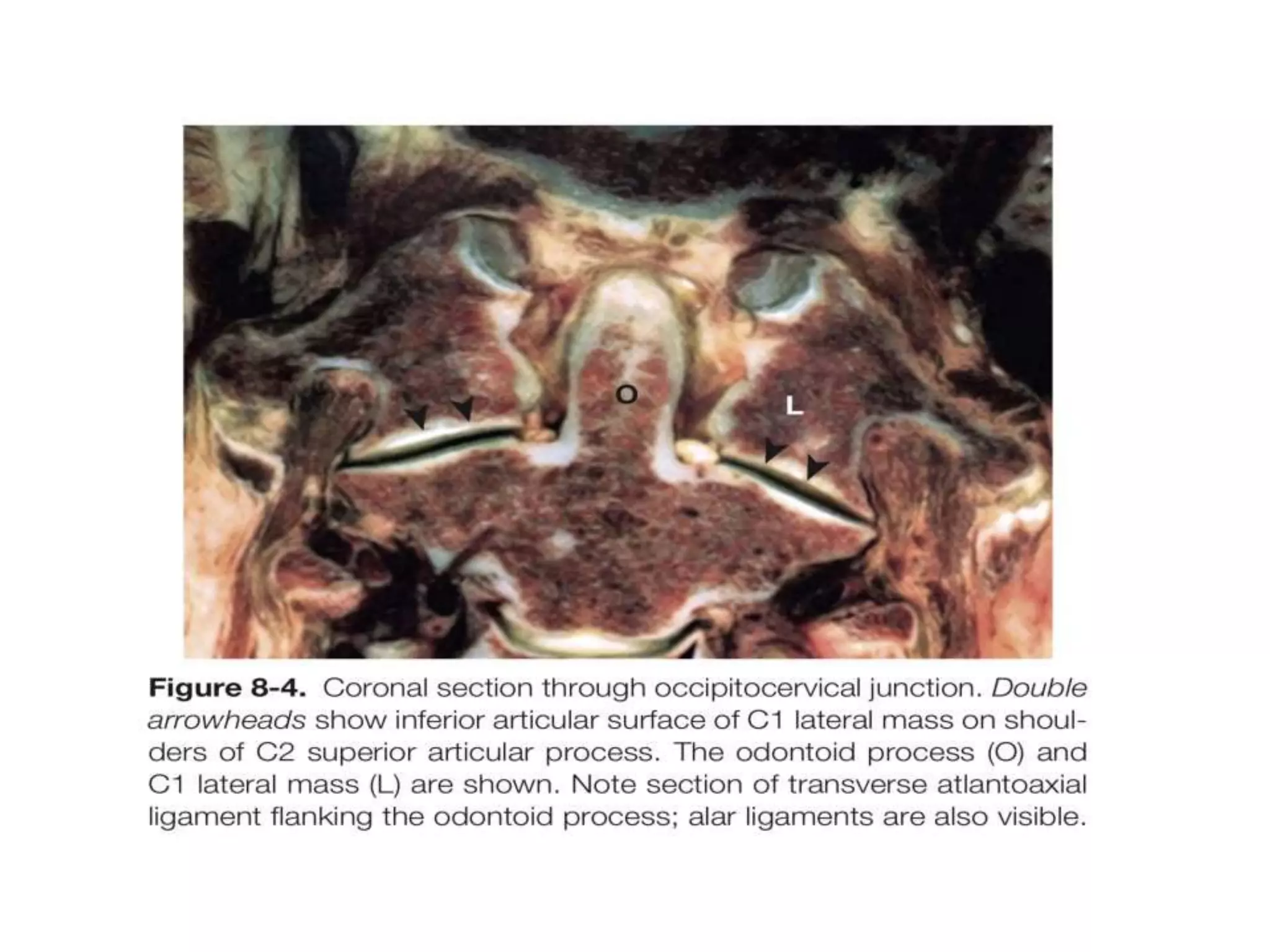
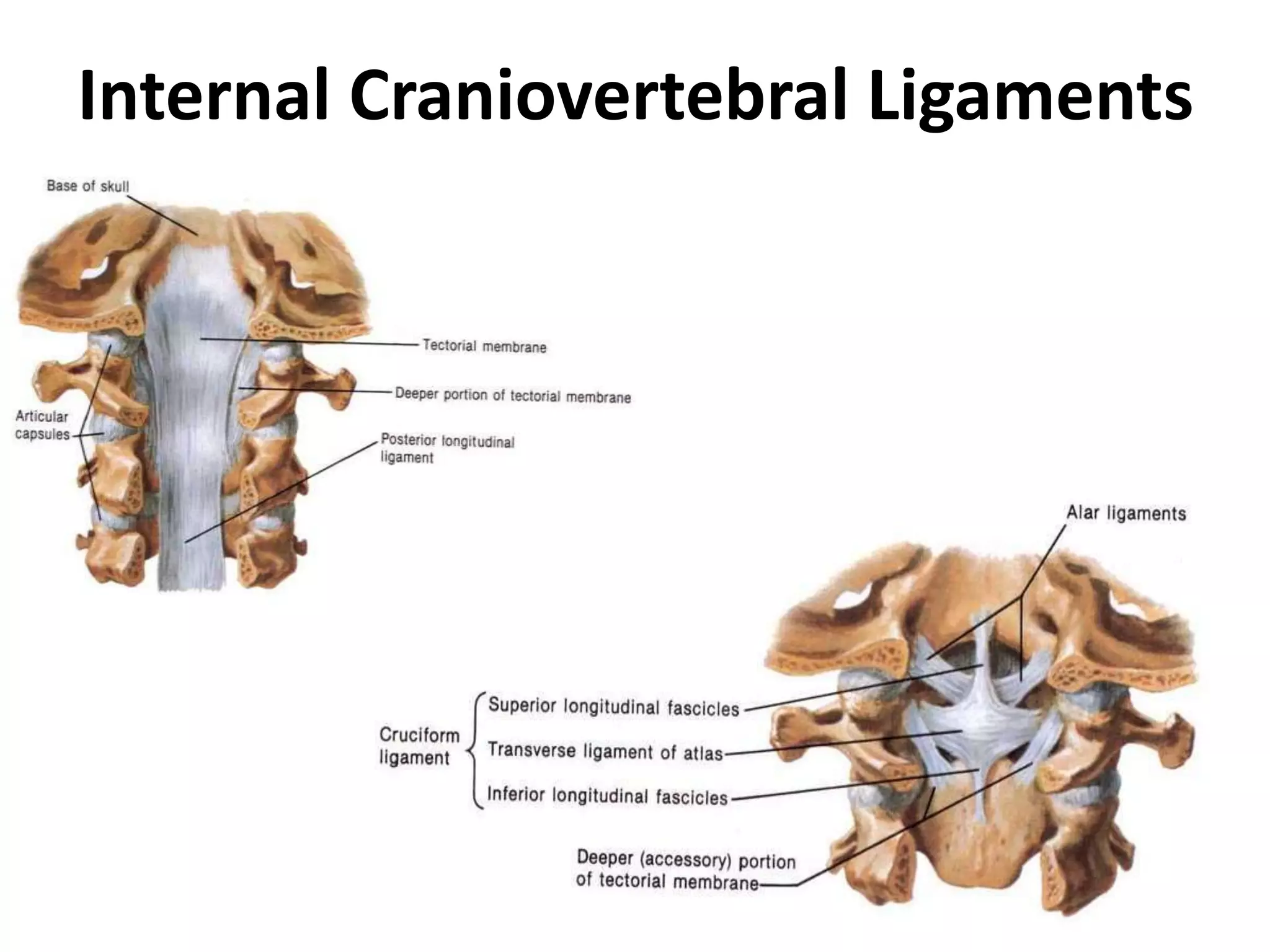
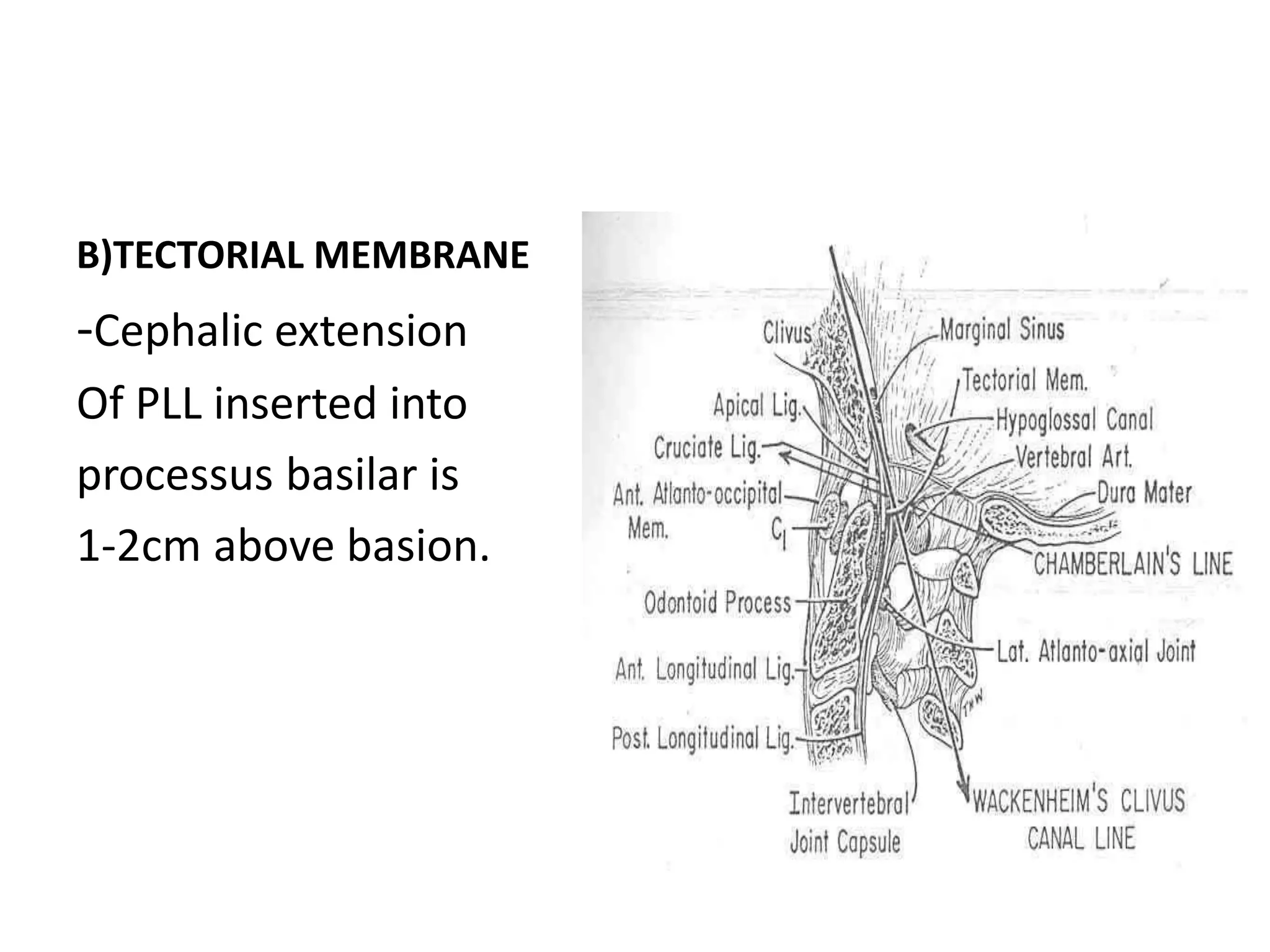
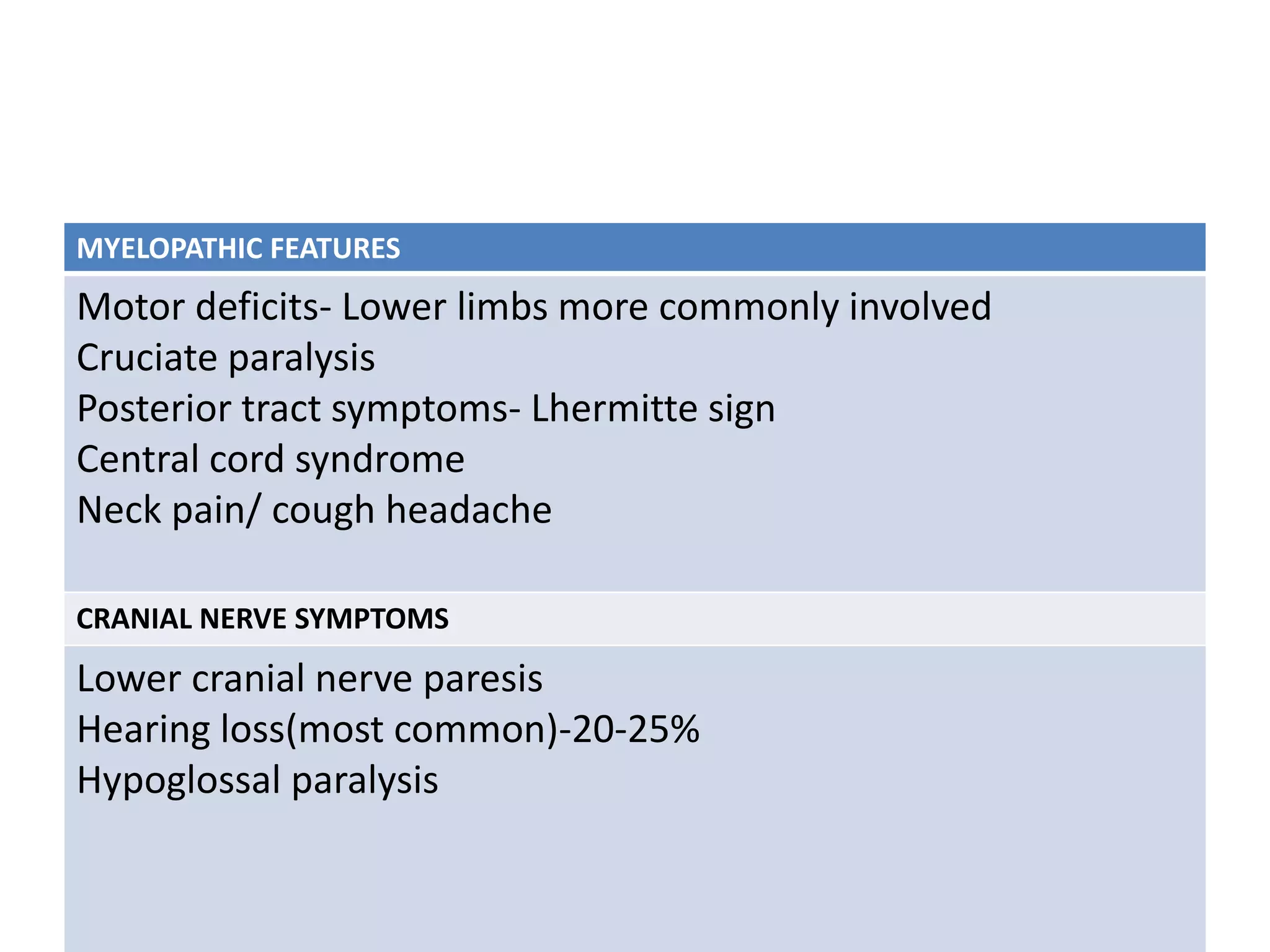
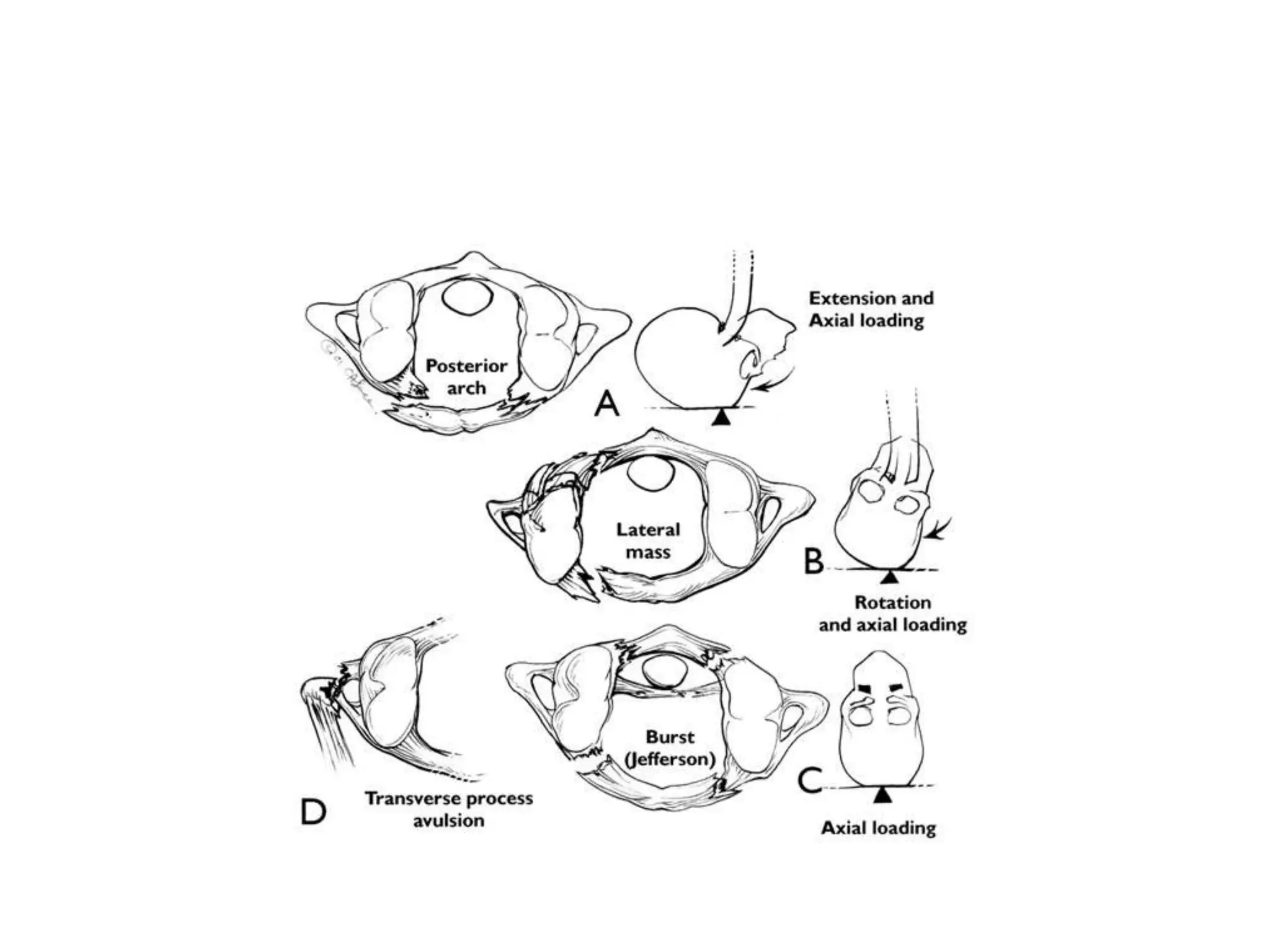
The document discusses the embryology, anatomy, and biomechanics of the craniovertebral junction (CVJ). It covers the development of the occiput, atlas, and axis from somites. It describes the ossification centers and joints of the CVJ. It outlines the ligaments stabilizing the CVJ and defines the normal range of motion. It also reviews clinical presentations of CVJ anomalies like platybasia, basilar invagination, and atlantoaxial dislocation.