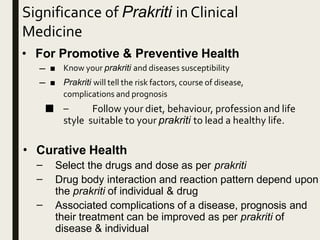
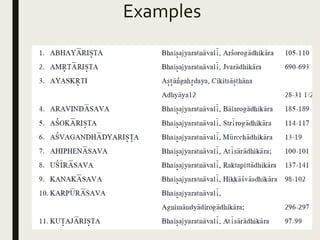
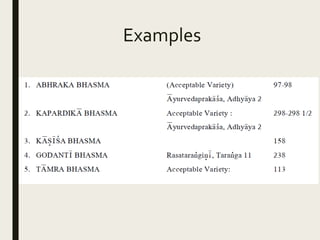
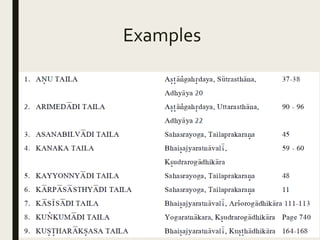
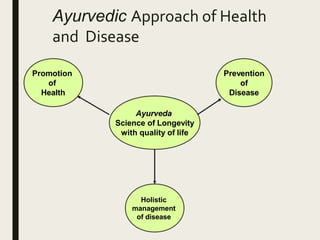
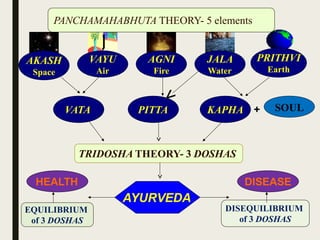
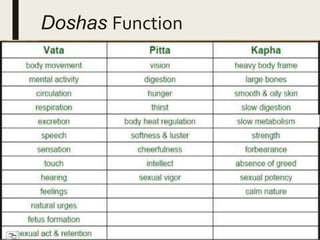
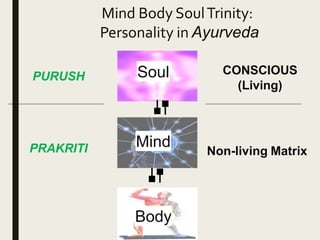
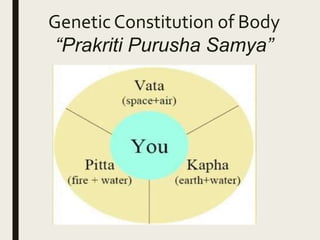
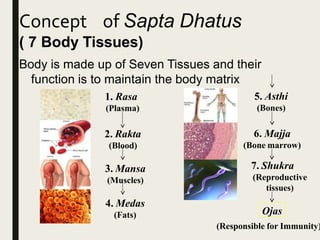
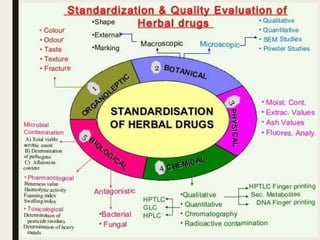
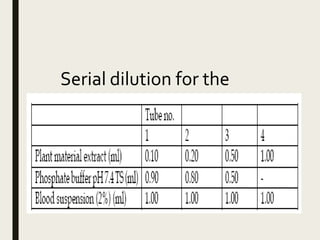
The document provides an overview of Ayurveda, a traditional Indian system of medicine that focuses on the holistic balance of body, mind, and spirit to promote health and prevent disease. It explores various Ayurvedic formulations, their preparation, and quality control, alongside the philosophical foundations rooted in the Vedas. Additionally, it discusses the significance of doshas, prakriti, and the principles of treatment, emphasizing the benefits of Ayurveda in physical, psychological, and spiritual health.