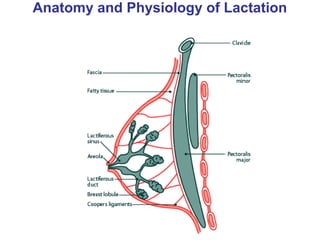
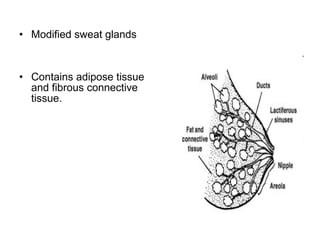
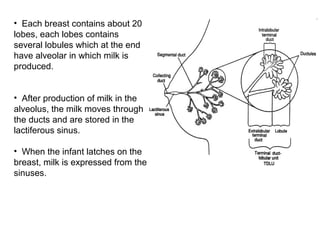
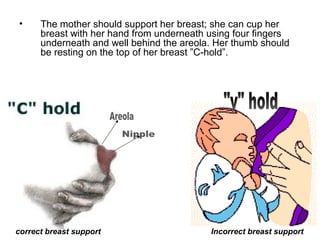
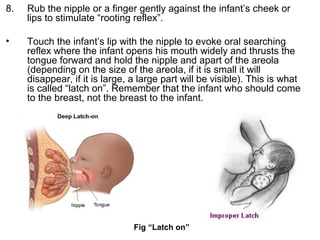
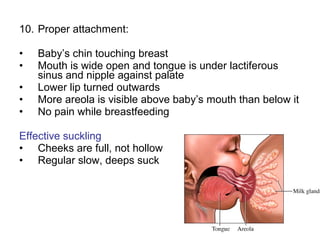
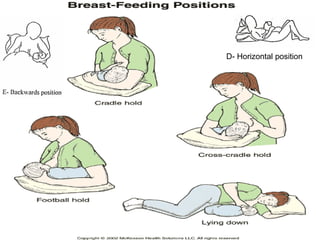
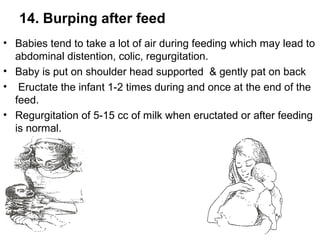
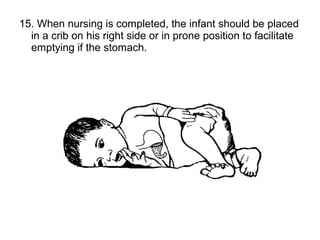
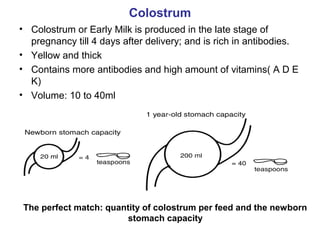
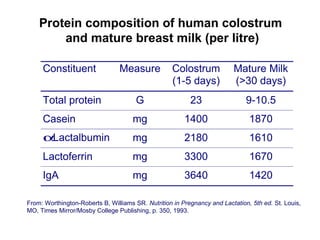
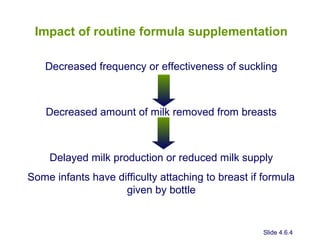
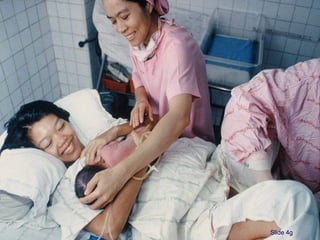
The document discusses breastfeeding and lactation management. It describes the anatomy and physiology of lactation, including the production of milk in the alveoli and its movement through ducts. The suckling hormonal reflex arc is explained, involving signals sent to the brain and release of prolactin and oxytocin in response to suckling. Advantages of breastfeeding are enumerated, such as immunological benefits from antibodies and growth factors. Proper techniques are outlined for breastfeeding, positioning, attachment and burping the infant. Guidelines are provided around breastfeeding frequency, exclusive breastfeeding for 6 months, and assessing milk supply. The composition of breast milk changes from colostrum to transitional to mature milk. Reasons for