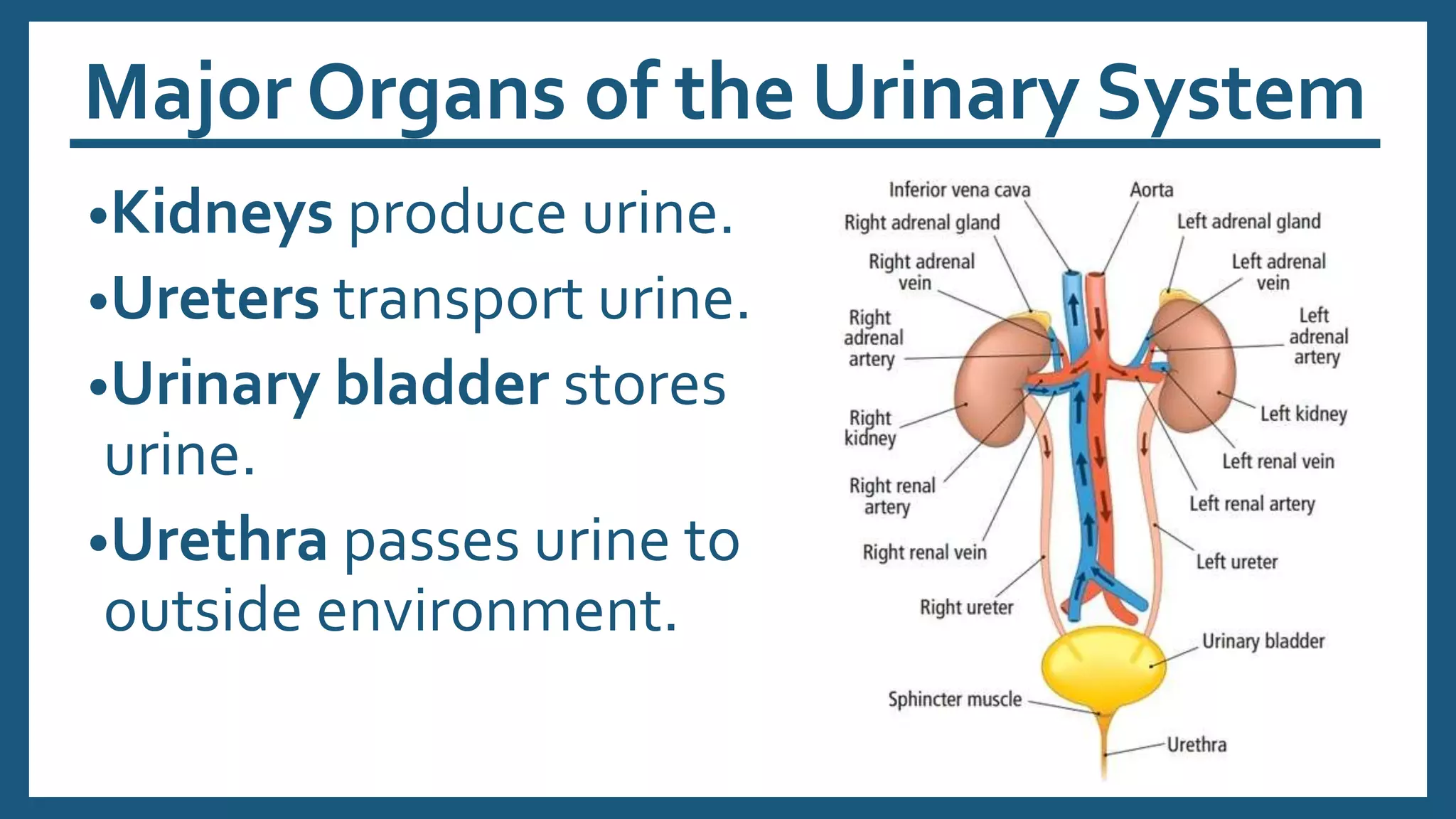
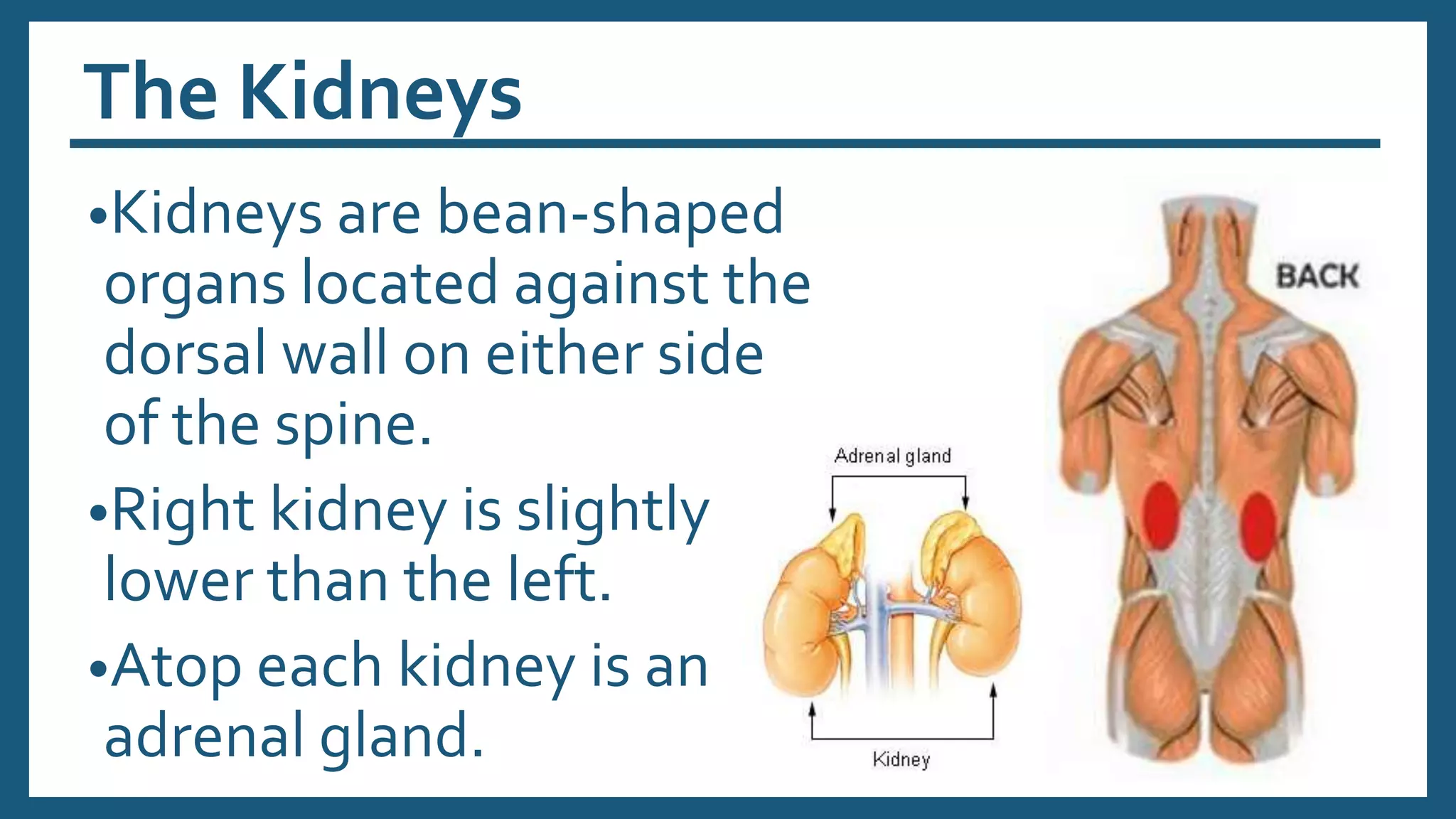
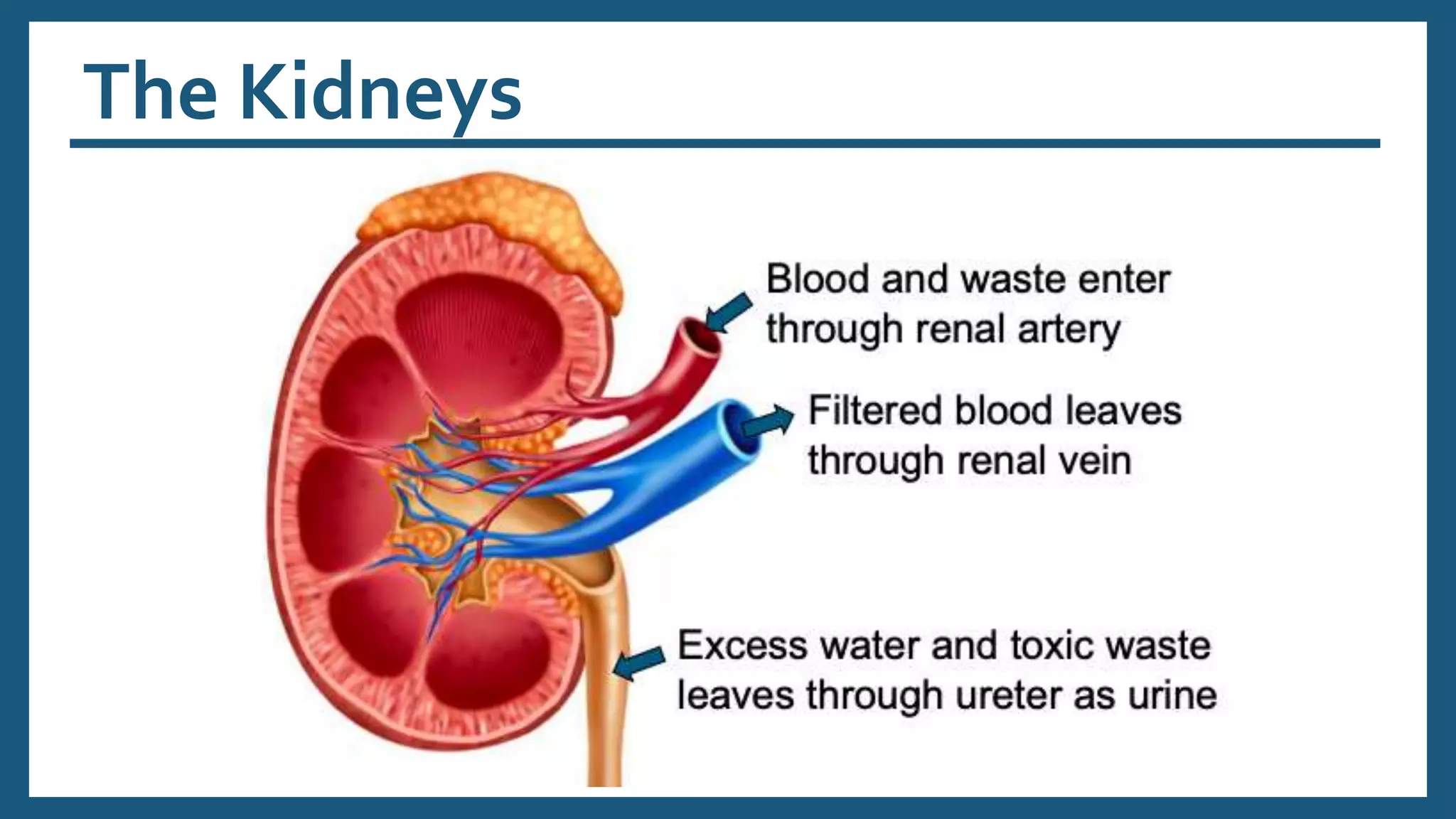
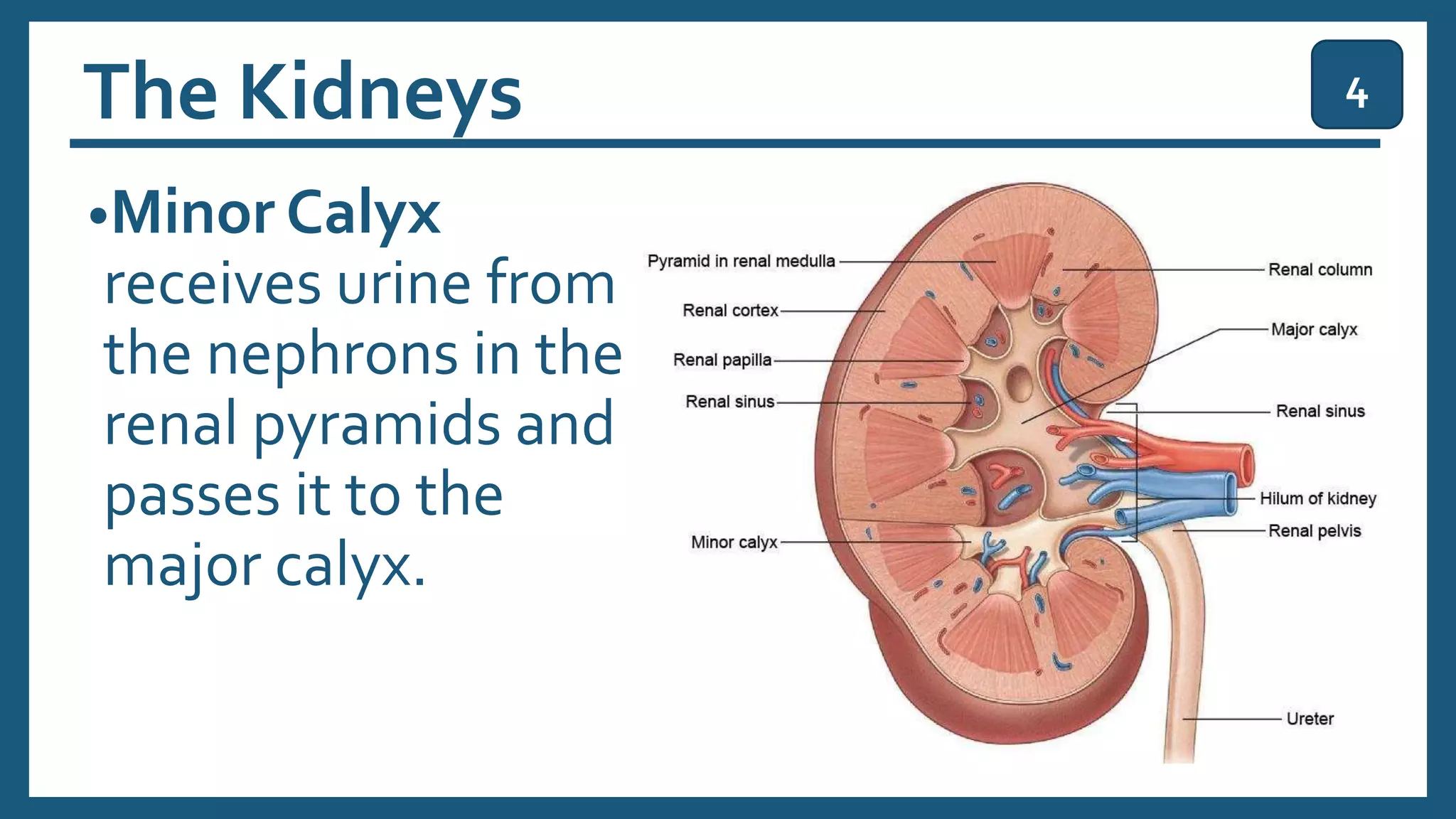
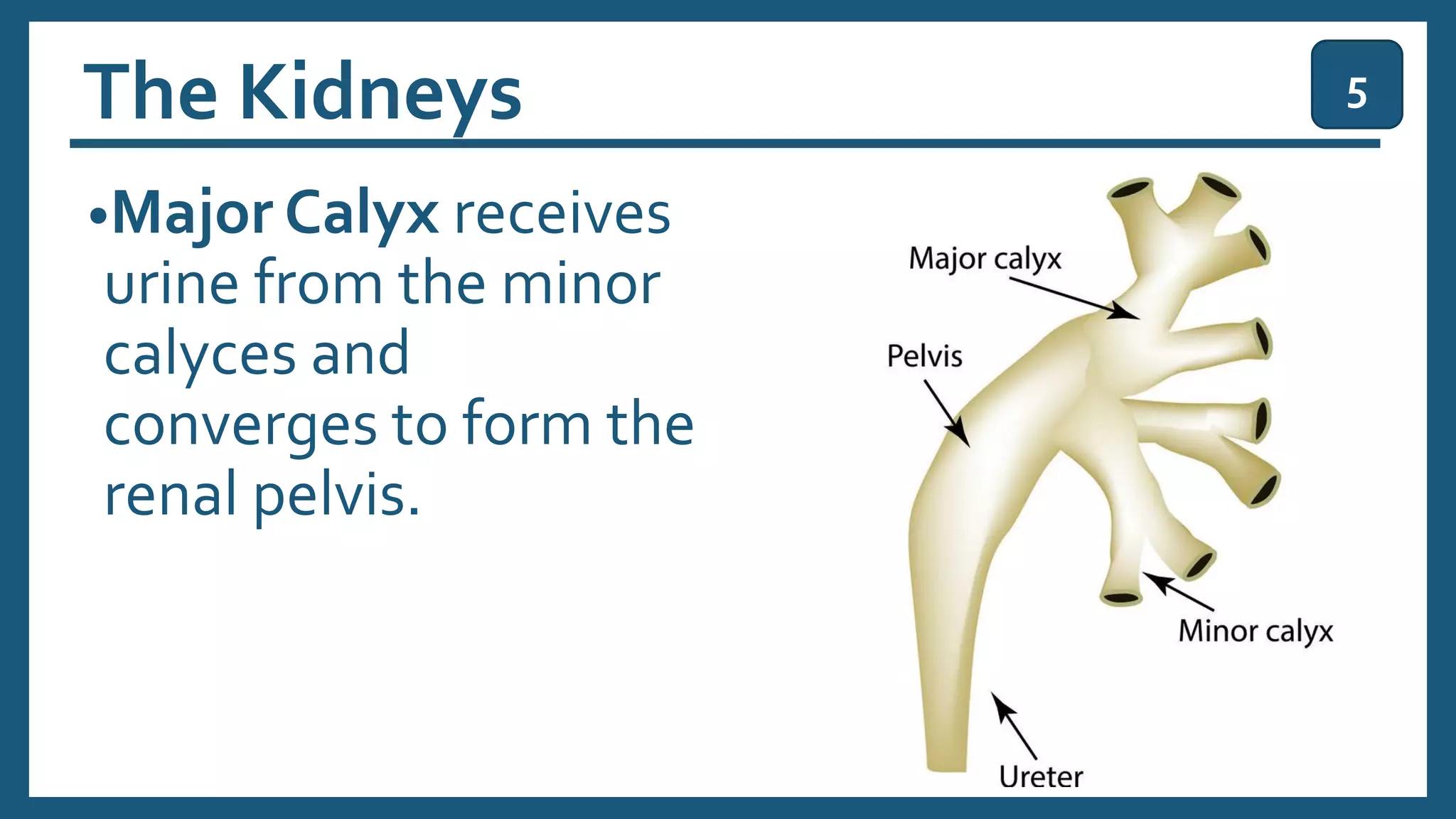
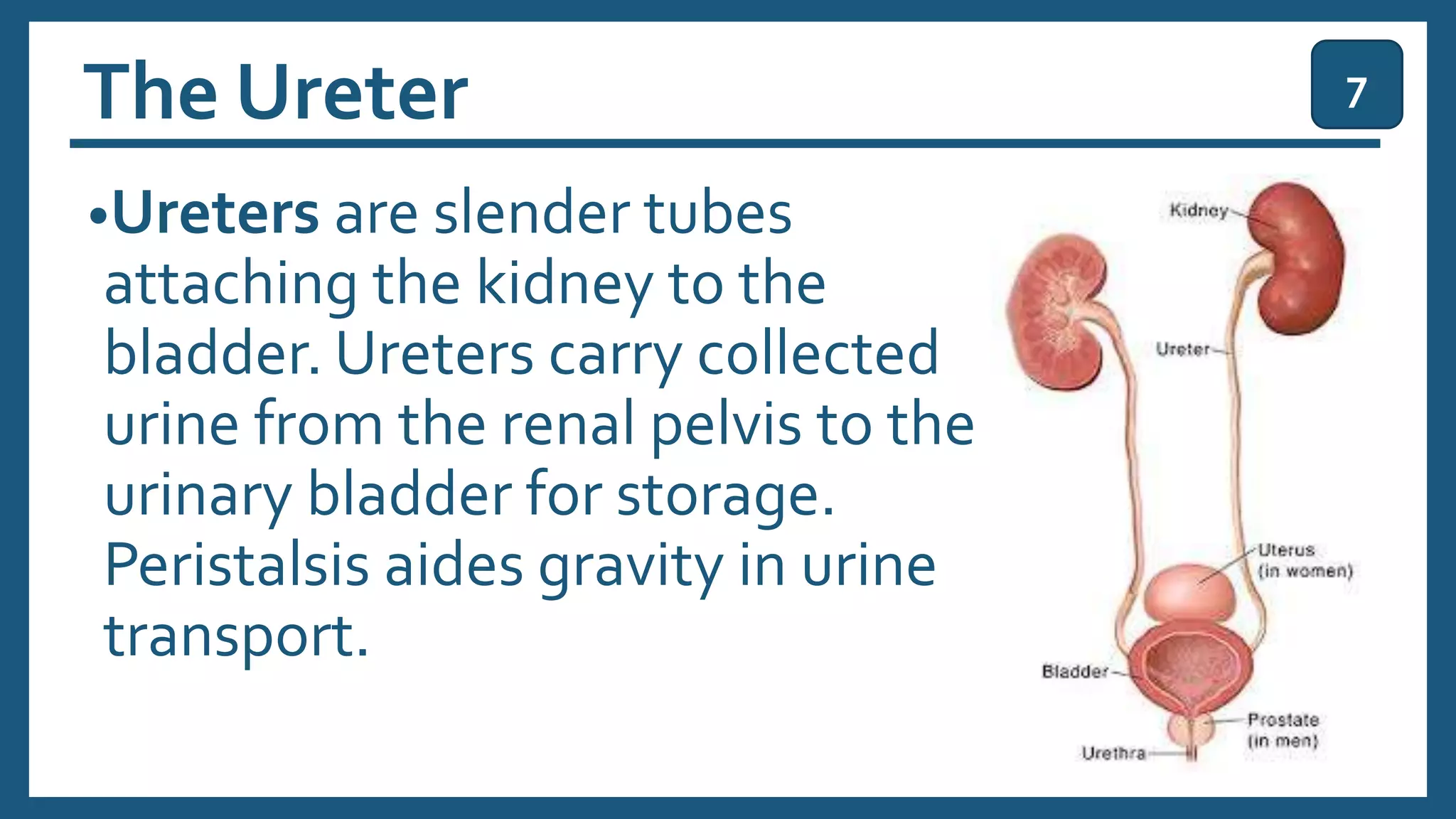
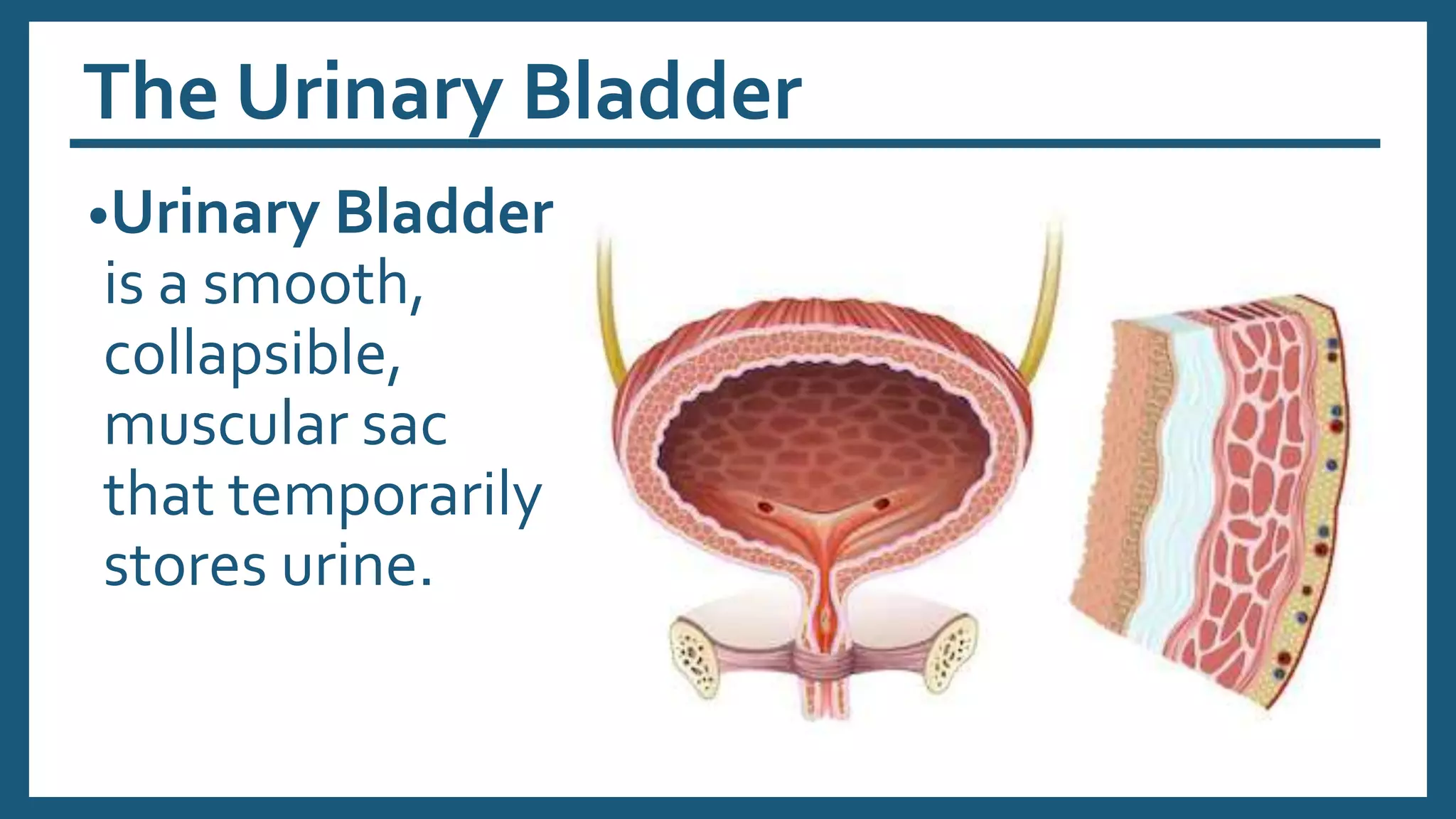
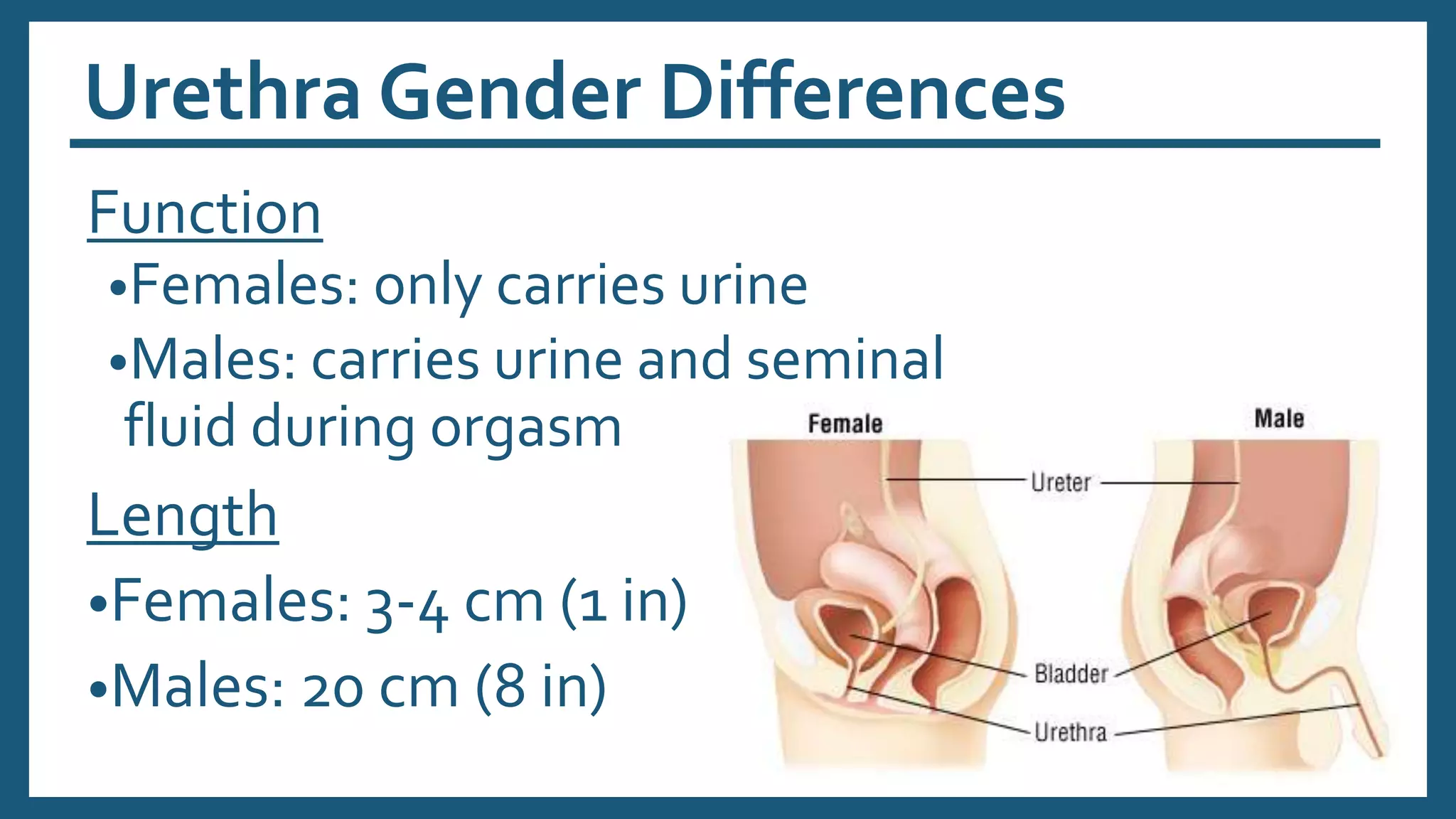
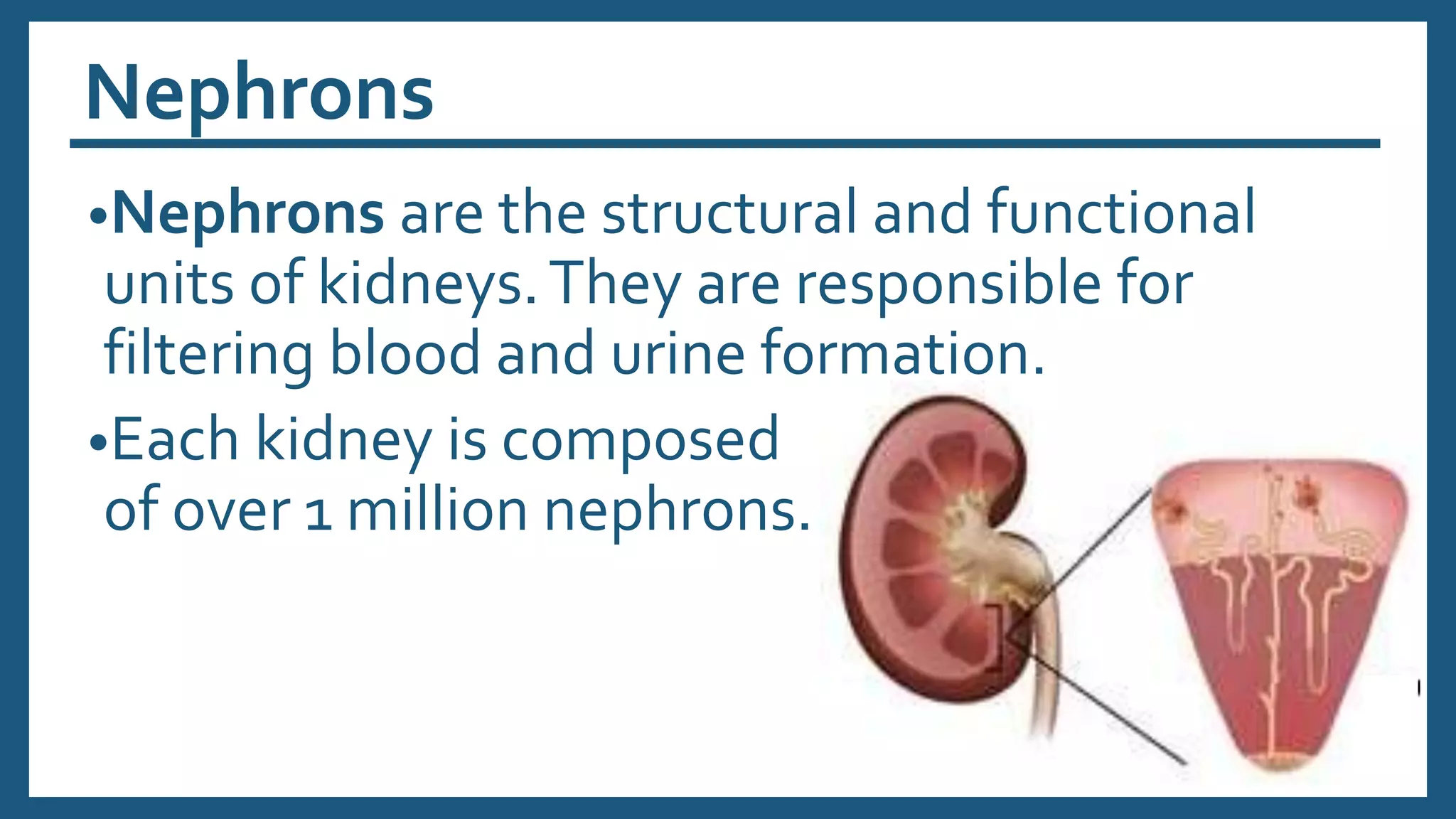
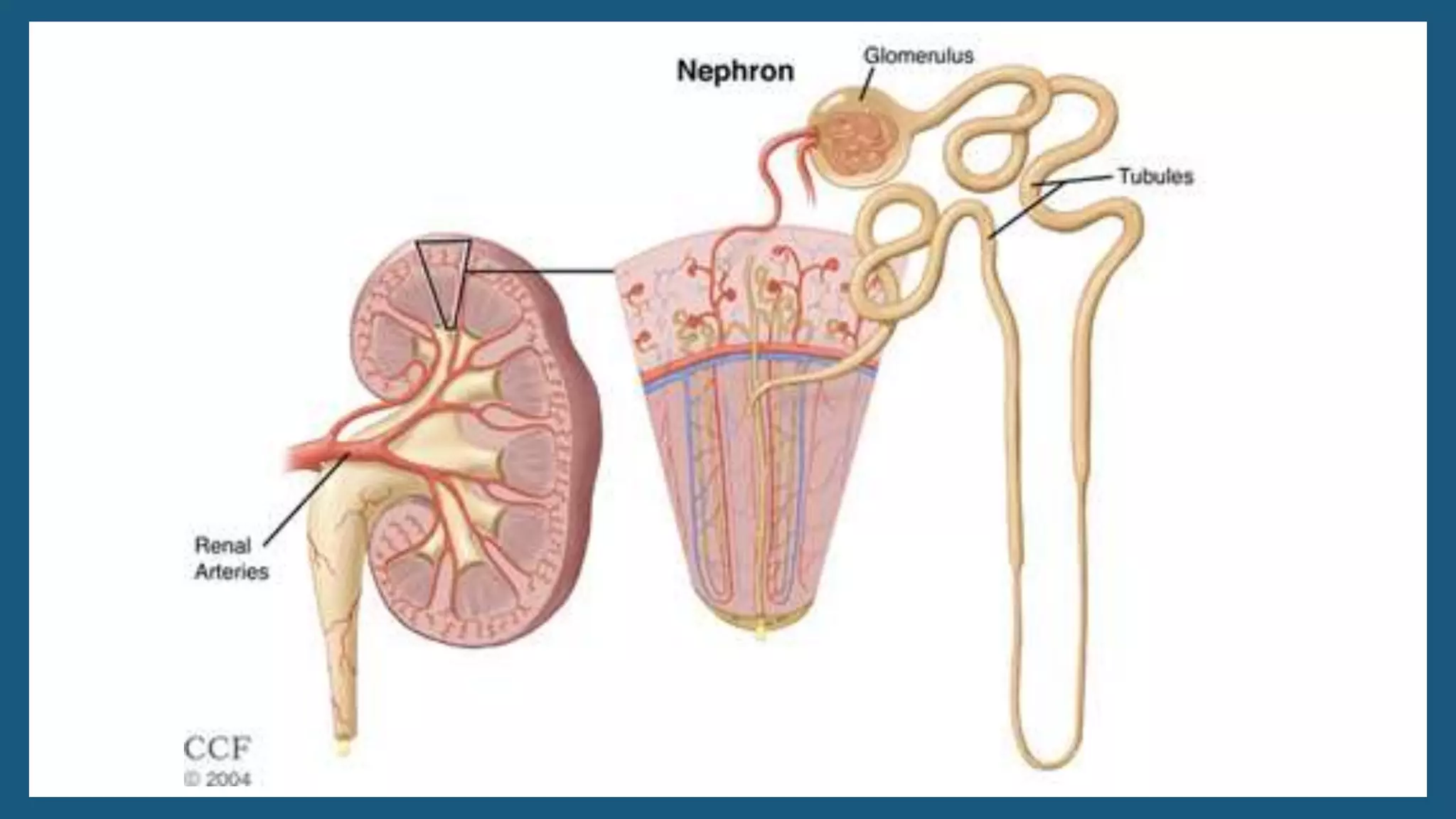
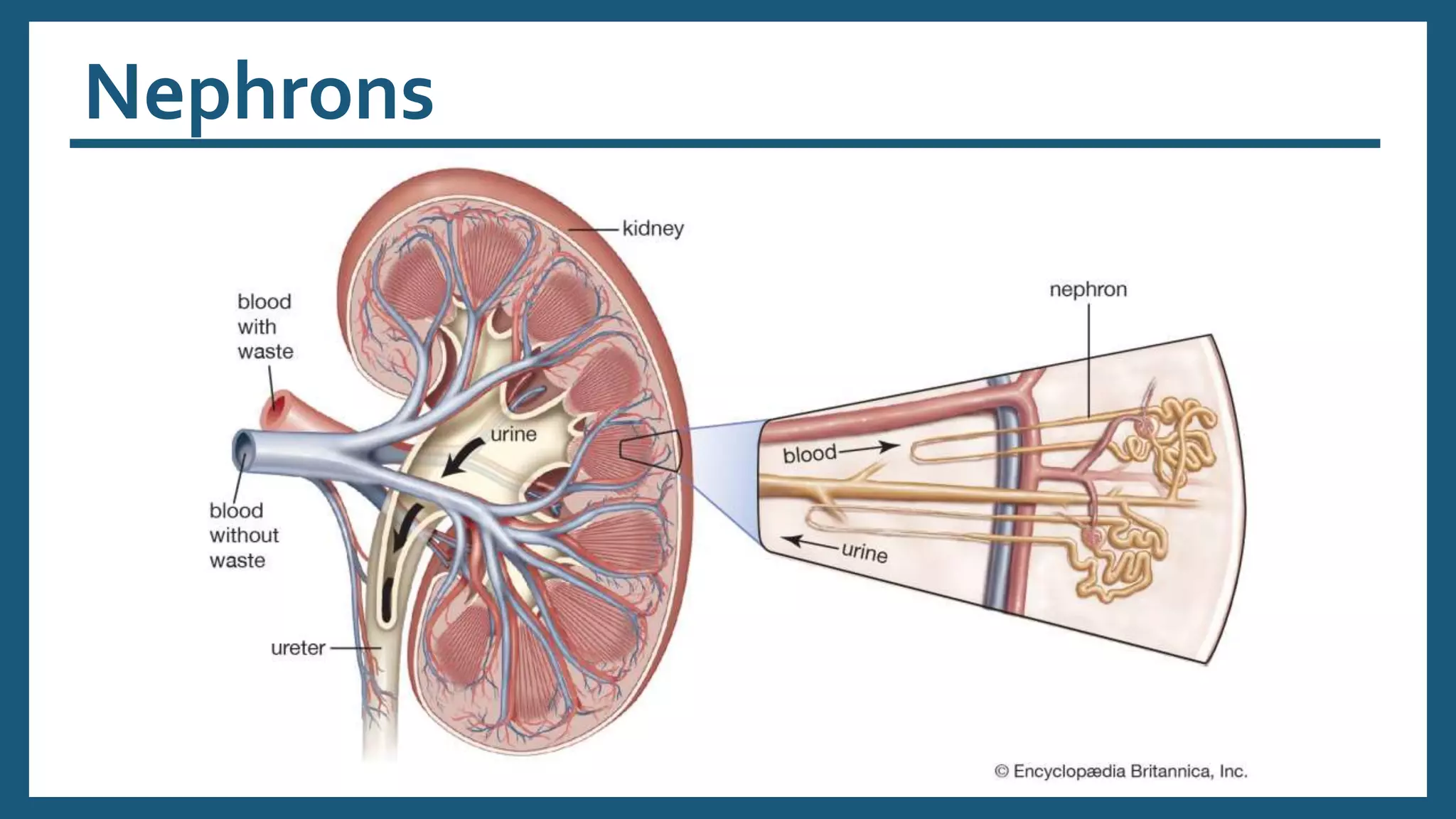
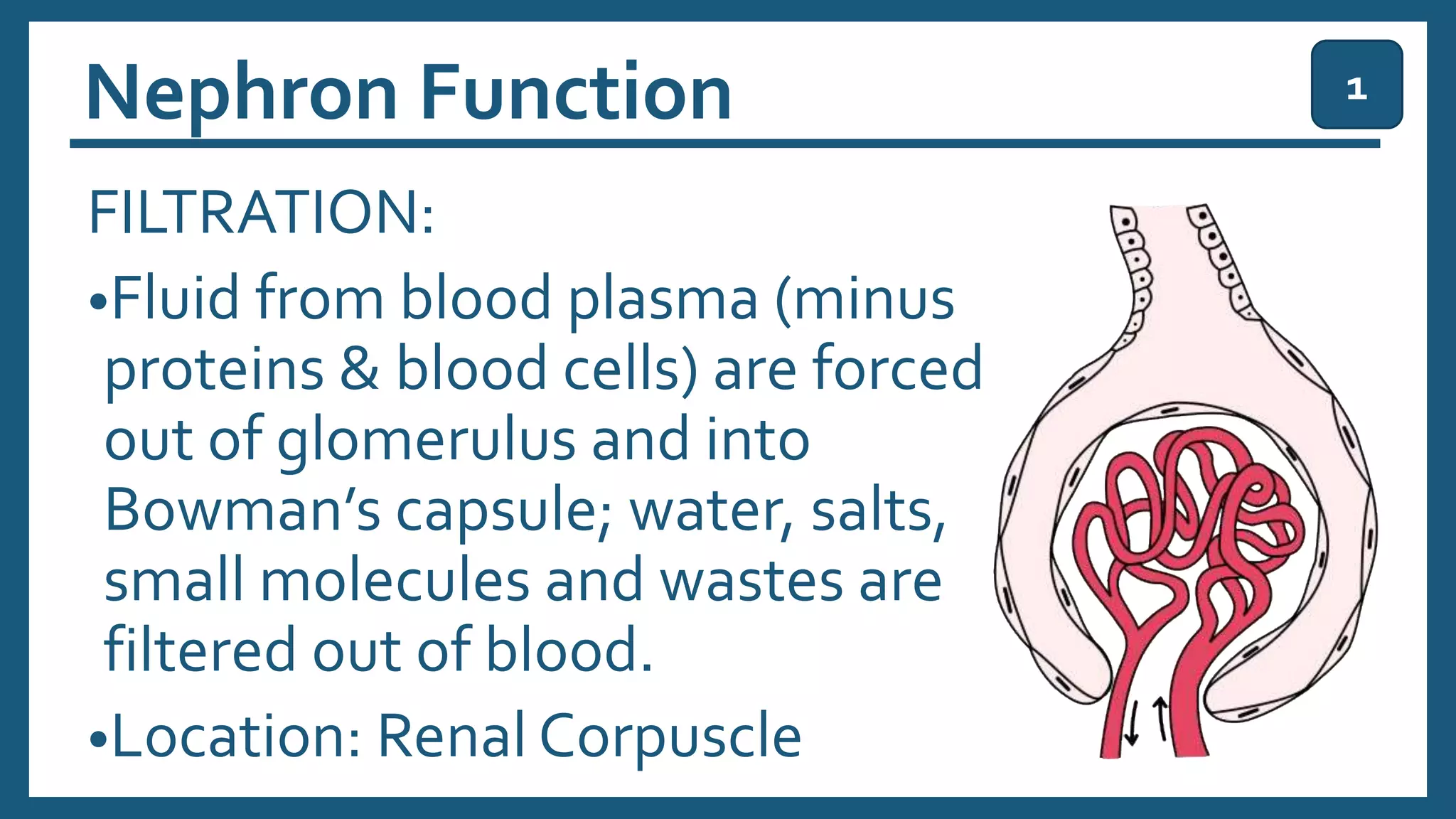
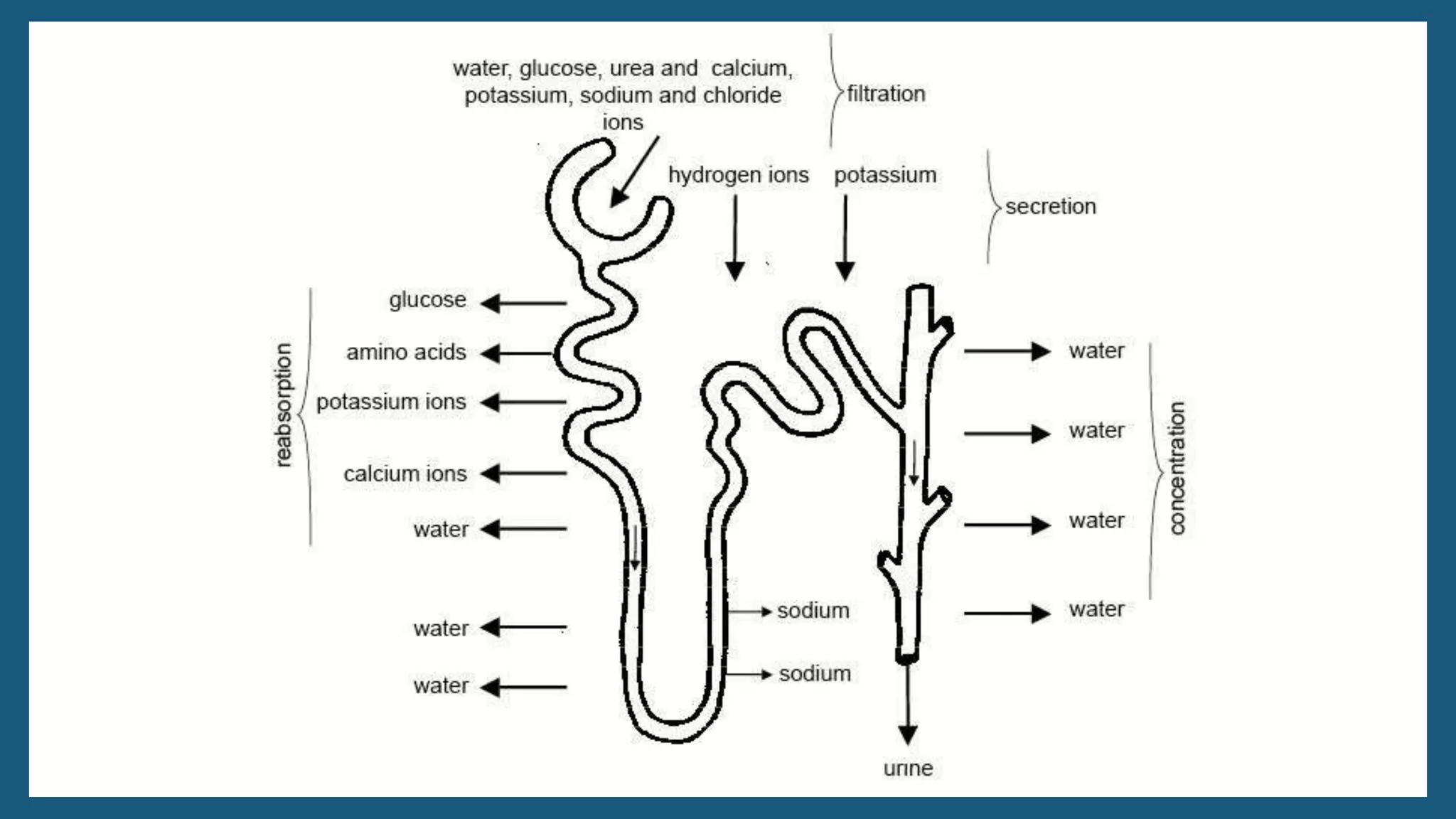
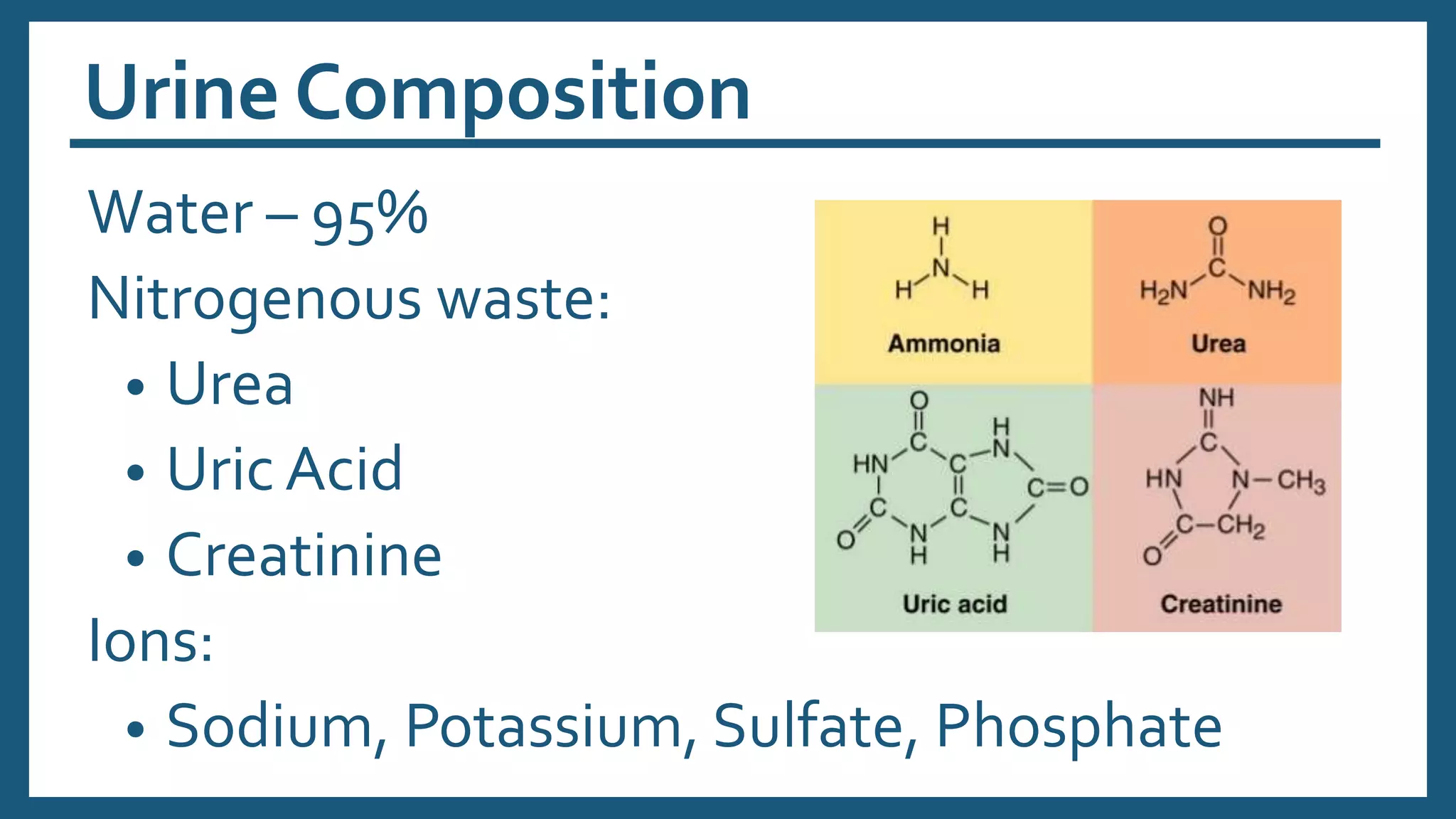
The document provides an overview of the urinary system, including its general functions, major organs, urine formation process, urine composition, micturition, urinalysis, homeostasis, and aging effects. It describes the kidneys' roles in excretion, regulation of blood volume and pressure, electrolyte and pH balance, and hormone release. The major organs - kidneys, ureters, bladder, and urethra - and their structures and functions are defined. Urine formation via nephron filtration, reabsorption and secretion is explained in detail.