Antibiotics lecture
•Download as PPT, PDF•
1 like•86 views
the spectrum of anitmicrobial activity action of antimicrobial drugs mechanism of antibiotics action inhibation of protein synthesis quinolones Antimeta metabolites
Report
Share
Report
Share
Recommended
Antibiotics

Antibiotics target bacteria and some other microorganisms. Broad-spectrum antibiotics affect a wide range of bacteria while narrow-spectrum antibiotics only target a few types. Antibiotics work by interfering with bacterial protein synthesis, membrane function, or nucleotide synthesis. Common side effects include diarrhea and nausea, while rare side effects include kidney stones or sensitivity to sunlight. Overuse of antibiotics has led to increased antibiotic resistance in disease-causing microbes.
Molecular mechanism of antibiotic resistance

Molecular mechanism of antibiotic resistanceRajasthan university of Veterinary and Animal Sciences, Bikaner
The document discusses various molecular mechanisms of antibiotic resistance in bacteria. It describes 3 main categories of resistance mechanisms: 1) preventing access to antibiotic targets through reduced permeability or increased efflux, 2) modifying antibiotic targets by genetic mutation or target protection/modification, and 3) directly inactivating antibiotics through hydrolysis or chemical modification. Recent studies have greatly expanded understanding of resistance genes and mechanisms, which can inform new drug development and clinical use of antibiotics.Antimicrobial drugs

This document provides an overview of current antibiotic drugs, organized by their mechanism of action. It begins by introducing penicillins like benzylpenicillin and amoxicillin, noting the rise of resistance. It then discusses beta-lactamase inhibitors that are combined with penicillins. The document also covers cephalosporins, carbapenems, glycopeptides, sulfonamides, tetracyclines, aminoglycosides, macrolides, and other antibiotic classes. It provides examples of common drugs for each class and their typical uses. The document concludes by discussing new approaches to developing antibiotics that target bacterial virulence factors or inhibit cell surface protein secretion.
Antimicrobial agent

This document discusses different classifications and mechanisms of antimicrobial agents. It describes how antibiotics can be classified based on their chemical structure, source, mechanism of action, spectrum of activity, and mode of action. The main mechanisms of antibiotic resistance are discussed, including production of enzymes to destroy antibiotics and alterations to cell membranes or metabolic pathways. Approaches to addressing resistance include proper antibiotic usage and selection based on accurate diagnosis and susceptibility testing.
Antimicrobials

This document discusses the mechanisms of action of antimicrobial drugs. It explains that antimicrobials work by inhibiting microbial growth and multiplication through various targets, including the cell wall, cell membrane, protein synthesis, intermediary metabolism, and nucleic acid metabolism. It provides examples of specific drugs that act on these various targets, such as betalactams which inhibit cell wall synthesis, polymixins which disrupt the cell membrane, and fluoroquinolones which inhibit DNA gyrase. The document aims to describe how antimicrobials are able to selectively kill pathogens while sparing host cells.
ANTIMICROBIAL DRUGS (Part 2) 

To understand the mechanisms of antimicrobial action and the classification of antimicrobial drugs.
To explain the process of microbial resistance.
To understand the spread of resistant microbes.
Outlines the prevention of microbial resistance.
Antibiotics and their mode of action ankush (2019 a109m)

Antibiotics are secondary metabolites produced by microorganisms that inhibit the growth of other microorganisms. Some key antibiotics include penicillin, discovered in 1928, and streptomycin, discovered in 1944. Antibiotics act through several modes of action including inhibition of cell wall synthesis, damage to cell membranes, and inhibition of protein and nucleic acid synthesis. Common classes of antibiotics include beta-lactams like penicillin which inhibit cell wall synthesis, macrolides like erythromycin which inhibit ribosomal translocation, and aminoglycosides like streptomycin which bind to ribosomal subunits and inhibit translocation. Each class has distinctive producers and modes of inhibitory action on bacterial growth and reproduction.
Basic principles of chemotherapy

Chemotherapy uses chemicals to inhibit the growth of microorganisms and is used with other treatments like biological therapies, hormonal therapy, radiation therapy, and surgery. Antibiotics are produced by microorganisms and kill or inhibit the growth of other organisms. Chemotherapeutic agents target parasitic cells while being innocuous to host cells by exploiting biochemical differences between the parasite and host. There are three classes of biochemical reactions in bacteria that can be targeted: class I involves energy production, class II small molecule synthesis, and class III macromolecule assembly. Differences between bacterial and human cells allow some class III reactions like peptidoglycan cell wall synthesis to be targeted.
Recommended
Antibiotics

Antibiotics target bacteria and some other microorganisms. Broad-spectrum antibiotics affect a wide range of bacteria while narrow-spectrum antibiotics only target a few types. Antibiotics work by interfering with bacterial protein synthesis, membrane function, or nucleotide synthesis. Common side effects include diarrhea and nausea, while rare side effects include kidney stones or sensitivity to sunlight. Overuse of antibiotics has led to increased antibiotic resistance in disease-causing microbes.
Molecular mechanism of antibiotic resistance

Molecular mechanism of antibiotic resistanceRajasthan university of Veterinary and Animal Sciences, Bikaner
The document discusses various molecular mechanisms of antibiotic resistance in bacteria. It describes 3 main categories of resistance mechanisms: 1) preventing access to antibiotic targets through reduced permeability or increased efflux, 2) modifying antibiotic targets by genetic mutation or target protection/modification, and 3) directly inactivating antibiotics through hydrolysis or chemical modification. Recent studies have greatly expanded understanding of resistance genes and mechanisms, which can inform new drug development and clinical use of antibiotics.Antimicrobial drugs

This document provides an overview of current antibiotic drugs, organized by their mechanism of action. It begins by introducing penicillins like benzylpenicillin and amoxicillin, noting the rise of resistance. It then discusses beta-lactamase inhibitors that are combined with penicillins. The document also covers cephalosporins, carbapenems, glycopeptides, sulfonamides, tetracyclines, aminoglycosides, macrolides, and other antibiotic classes. It provides examples of common drugs for each class and their typical uses. The document concludes by discussing new approaches to developing antibiotics that target bacterial virulence factors or inhibit cell surface protein secretion.
Antimicrobial agent

This document discusses different classifications and mechanisms of antimicrobial agents. It describes how antibiotics can be classified based on their chemical structure, source, mechanism of action, spectrum of activity, and mode of action. The main mechanisms of antibiotic resistance are discussed, including production of enzymes to destroy antibiotics and alterations to cell membranes or metabolic pathways. Approaches to addressing resistance include proper antibiotic usage and selection based on accurate diagnosis and susceptibility testing.
Antimicrobials

This document discusses the mechanisms of action of antimicrobial drugs. It explains that antimicrobials work by inhibiting microbial growth and multiplication through various targets, including the cell wall, cell membrane, protein synthesis, intermediary metabolism, and nucleic acid metabolism. It provides examples of specific drugs that act on these various targets, such as betalactams which inhibit cell wall synthesis, polymixins which disrupt the cell membrane, and fluoroquinolones which inhibit DNA gyrase. The document aims to describe how antimicrobials are able to selectively kill pathogens while sparing host cells.
ANTIMICROBIAL DRUGS (Part 2) 

To understand the mechanisms of antimicrobial action and the classification of antimicrobial drugs.
To explain the process of microbial resistance.
To understand the spread of resistant microbes.
Outlines the prevention of microbial resistance.
Antibiotics and their mode of action ankush (2019 a109m)

Antibiotics are secondary metabolites produced by microorganisms that inhibit the growth of other microorganisms. Some key antibiotics include penicillin, discovered in 1928, and streptomycin, discovered in 1944. Antibiotics act through several modes of action including inhibition of cell wall synthesis, damage to cell membranes, and inhibition of protein and nucleic acid synthesis. Common classes of antibiotics include beta-lactams like penicillin which inhibit cell wall synthesis, macrolides like erythromycin which inhibit ribosomal translocation, and aminoglycosides like streptomycin which bind to ribosomal subunits and inhibit translocation. Each class has distinctive producers and modes of inhibitory action on bacterial growth and reproduction.
Basic principles of chemotherapy

Chemotherapy uses chemicals to inhibit the growth of microorganisms and is used with other treatments like biological therapies, hormonal therapy, radiation therapy, and surgery. Antibiotics are produced by microorganisms and kill or inhibit the growth of other organisms. Chemotherapeutic agents target parasitic cells while being innocuous to host cells by exploiting biochemical differences between the parasite and host. There are three classes of biochemical reactions in bacteria that can be targeted: class I involves energy production, class II small molecule synthesis, and class III macromolecule assembly. Differences between bacterial and human cells allow some class III reactions like peptidoglycan cell wall synthesis to be targeted.
Antimicrobials

This document discusses antimicrobial resistance, which is one of the most important clinical problems today. It provides definitions of key terms like antibiotics, antimicrobials, and mechanisms of antibiotic resistance. The document also summarizes how resistance has developed and spread for certain microbes like MRSA and describes various mechanisms that bacteria use to develop resistance, such as modifying drug targets, inactivating antibiotics, or limiting drug uptake.
Antibiotics classification ppt

This document provides an overview of antibiotics, including:
1) It outlines the objectives of classifying commonly used antibiotics into six major classes, understanding their mechanisms of action, clinical uses, and side effects.
2) It summarizes the key characteristics and clinical uses of beta-lactams, aminoglycosides, fluoroquinolones, macrolides, tetracyclines, glycopeptides, and metronidazole.
3) It emphasizes the importance of considering pharmacokinetics and the site of infection when selecting an antibiotic to ensure it reaches the infection.
Antibiotic resistance mechanisms

This document discusses antibiotic resistance mechanisms. It defines antimicrobial resistance (AMR) as when microbes become insensitive to medicines, making infections harder to treat. AMR occurs through two main mechanisms: acquired resistance, where bacteria gain resistance genes, usually through overuse of antibiotics creating selective pressure; and intrinsic resistance, where bacteria innately resist certain drug classes. Bacteria develop resistance via decreased permeability, efflux pumps, enzymatic inactivation of drugs like beta-lactamases, and modifying drug targets. Resistance can be transmitted between bacteria through mutation or mobile genetic elements like plasmids.
Sk amd

The document discusses antimicrobial drug resistance (AMDR) and the mechanisms by which microbes develop resistance to antimicrobial medications. It describes classes of AMDR including resistance to antifungal, antiviral, antiprotozoal, and antibacterial drugs. Mechanisms of resistance include altering drug receptors or targets, reducing drug accumulation in cells, inactivating drugs, and developing resistant metabolic pathways. The document also summarizes the cellular and molecular mechanisms of antimicrobial action, including interfering with cell wall synthesis, plasma membrane integrity, nucleic acid synthesis, ribosomal function, and folate synthesis.
Importance of antibiotics and antiseptics , its types and application in the ...

IMPORTANCE OF ANTIBIOTICS AND ANTISEPTICS , ITS TYPES AND APPLICATION IN THE FIELD OF MICROBIOLOGY.
if found Aany mistake plz comment below
Antimicrobial Drugs

This document discusses antimicrobials and their uses. It defines antimicrobials as substances that reduce microbes like bacteria and molds. Antimicrobial drugs are classified based on the microorganisms they target or their function. Broad spectrum antimicrobials affect many types of microbes while narrow spectrum drugs target specific microbes. The document also discusses antimicrobial resistance and how microbes develop resistance. It provides streptomycin as an example antimicrobial drug, describing its discovery, mode of action in inhibiting protein synthesis, and production process. Streptomycin is derived from bacteria and was an early antibiotic used to treat tuberculosis. The document concludes that while antimicrobials are useful, their overuse can lead to increased antimicrobial resistance in micro
Antibiotics - Polypepetide Antibiotics 

Polypeptide antibiotics are a diverse class of natural antibiotics composed of amino acids joined by amide bonds. They are low molecular weight cationic polypeptides that act as powerful bactericidal agents against both gram-positive and gram-negative bacteria. Examples include gramicidin, bacitracin, polymyxin-B, and colistin. These antibiotics act by disrupting bacterial membranes through detergent-like and pseudophore formation mechanisms, leading to ion leakage and inactivation of endotoxins. In addition, chloramphenicol, vancomycin, and novobiocin are classified as miscellaneous antibiotics that have bactericidal properties through inhibition of protein synthesis or bacterial cell wall synthesis.
SAR-Systemic Acquired Resistance 

This document discusses systemic acquired resistance (SAR), a plant defense mechanism that confers broad-spectrum and long-lasting protection against pathogens. SAR involves the signal molecule salicylic acid and accumulation of pathogenesis-related proteins. It provides an alternative to hazardous chemical pesticides and has potential for sustainable agriculture. SAR is induced by necrotic pathogens and results in resistance throughout the plant via a signal transduction pathway involving salicylic acid.
ANTIMICROBIAL DRUGS

This document discusses antimicrobial drugs, including antibiotics. It describes how antibiotics are substances produced by microorganisms that inhibit the growth of other microbes. It outlines several antibiotic-producing microorganisms and explains the mechanisms of action of antimicrobial drugs, including inhibiting cell wall synthesis, protein synthesis, and nucleic acid synthesis. The document also discusses the spectrum of antimicrobial activity and lists some common side effects and safety concerns with antimicrobial use, such as toxicity, resistance, and interaction with other drugs.
Antimicrobial agents and mechanisms of action 2

This document discusses antimicrobial resistance and its mechanisms. It defines antimicrobial resistance and describes how it can arise through mutation or acquisition of genes. It covers various mechanisms of resistance such as production of inactivating enzymes, decreased permeability, efflux pumps, and modification of drug targets. It also discusses specific examples of resistance to beta-lactams, glycopeptides, and antibiotics that inhibit protein synthesis. Key terms related to drug-resistant organisms are defined.
Antimicrobial chemotherapy

This document discusses antimicrobial agents and chemotherapy. It begins by defining antibiotics as natural substances produced by microorganisms that suppress or kill other microorganisms. It then discusses antimicrobial agents, which include both naturally obtained and synthetic drugs that can attenuate microorganisms. Finally, it defines chemotherapeutic agents as drugs designed to inhibit or kill an infecting organism with minimal effect on the recipient. The document goes on to provide details on the classification, mechanisms, principles, development and prevention of antimicrobial resistance.
Antibiotic resistance

Relative or complete lack of effect of antimicrobial agent against a previously susceptible microbe/pathogen.
It is an evolutionary principal that organism adopt genetically to change in their environment.
since the doubling time of bacteria can be as short as 20 mnt, there may be many generations in even a few hours, providing ample opportunity for evolutionary adaptation.
The phenomenon of resistance imposes serious constraints on the options available for the treatment of many bacterial infections.
The resistance to chemotherapeutic agents can also develop in protozoa, in multicellular parasites and in population of malignant cells.
Today there are different strains of S. aureus resistant to almost every form of antibiotic in use.
12.COMPREHENSIVE OFANTIMICROBIAL AGENTS AND CHEMOTHERAPY ( CLASSIFICATION AND...

12.COMPREHENSIVE OFANTIMICROBIAL AGENTS AND CHEMOTHERAPY ( CLASSIFICATION AND...Saminathan Kayarohanam
Antimicrobial Agents and Chemotherapy (AAC) features interdisciplinary studies that build our understanding of the underlying mechanisms and therapeutic applications of antimicrobial and antiparasitic agents and chemotherapy.Mechanism Of Resistance Of Antibiotics

mechanism of resistance of antibiotics, ESBL, b lactums, enterobactericae, metallobactums, carbapenemases, types of mechanism of resistance, history of antibiotics and resistance
Mechanisms of Resistance to Antibiotics

1. Antimicrobial resistance arises through genetic mutations and the acquisition of resistance genes from other bacteria.
2. Resistance genes can be acquired horizontally via mobile genetic elements such as plasmids, leading to rapid spread.
3. Common resistance mechanisms include enzymatic inactivation of antibiotics, modification or protection of antibiotic targets, and efflux pumps that pump out antibiotics.
Antibiotics resistance

Antibiotics, Antibiotics Resistance, Action of Antibiotics, Mechanism of Antibiotics Resistance, Generation of Antibiotics
Antimicrobial agents and mechanisms of action 2

The document discusses antibiotic resistance mechanisms in bacteria. It describes several key mechanisms:
1. Production of enzymes that inactivate antibiotics through destruction or modification. This includes beta-lactamases that break down beta-lactam antibiotics.
2. Decreased permeability of the cell membrane, preventing antibiotic penetration.
3. Active efflux of antibiotics from the bacterial cell via efflux pumps.
4. Modification of antibiotic target sites, such as altered penicillin-binding proteins or modifications to ribosomes.
Resistance can arise through mutation or acquisition of resistance genes via horizontal gene transfer. Multiple resistance mechanisms can provide high-level or multidrug resistance.
Multiple Drug Resistance and Antibiotic Misuse In English.

The report on Multiple Drug Resistance and Antibiotic Misuse.
By: Nadia Hassan, Chandni Yaqoob and Mudassar Iqbal.
School of Biological Sciences, University of the Punjab.
Imipenem cilastatin training

IMIPEN® 500 (imipenem/cilastatin) is a broad-spectrum carbapenem antibiotic used as empirical monotherapy for serious bacterial infections in intensive care unit (ICU) patients. It is effective against both aerobic and anaerobic bacteria, including multidrug-resistant strains. Common serious infections treated with IMIPEN® 500 in the ICU include pneumonia, bloodstream infections, and urinary tract infections. It is administered intravenously in doses ranging from 500 mg to 1000 mg every 6 to 8 hours, depending on infection severity and patient risk factors.
Antibiotic

This document summarizes antibiotics and their mechanisms of action. It discusses how antibiotics were first coined by Waksman to refer to substances produced by microorganisms that inhibit or kill other microorganisms. It then describes the ideal properties of an antibacterial and provides classifications of antibiotics by origin (natural, semi-synthetic, synthetic) and mechanism of action (bactericidal, bacteriostatic). The document proceeds to explain various antibiotic targets and mechanisms in depth, including inhibition of cell wall synthesis, membrane synthesis, protein synthesis, nucleic acid formation, and metabolism. It also notes common antibiotic side effects and challenges in antibiotic research and treatment.
Antibiotics ppt

- Antibiotics selectively target microbial processes without harming human host cells. Proper antibiotic use and hand hygiene have improved patient outcomes.
- Many antibiotics are naturally produced by bacteria and fungi to inhibit competition. Major classes include penicillins, cephalosporins, aminoglycosides, tetracyclines, macrolides, and sulfonamides.
- Antibiotics work by inhibiting bacterial cell wall, protein, or nucleic acid synthesis. However, antibiotic resistance has emerged through various mechanisms and poses a growing challenge.
Antibiotics

This document discusses antimicrobial agents and antibiotics. It defines antimicrobial agents as chemicals that treat infectious diseases by inhibiting or killing pathogens. Ideal antimicrobial agents kill or inhibit pathogens, are not harmful to the host, cause no allergic reactions, and remain effective after storage and in tissues. The document then discusses different classes of antibiotics based on their source, mechanism of action, and targets, including cell wall synthesis inhibitors like penicillin and vancomycin, protein synthesis inhibitors like tetracyclines and chloramphenicol, and nucleic acid synthesis inhibitors like sulfonamides. It also addresses resistance acquisition through intrinsic, mutational or acquired genetic means.
More Related Content
What's hot
Antimicrobials

This document discusses antimicrobial resistance, which is one of the most important clinical problems today. It provides definitions of key terms like antibiotics, antimicrobials, and mechanisms of antibiotic resistance. The document also summarizes how resistance has developed and spread for certain microbes like MRSA and describes various mechanisms that bacteria use to develop resistance, such as modifying drug targets, inactivating antibiotics, or limiting drug uptake.
Antibiotics classification ppt

This document provides an overview of antibiotics, including:
1) It outlines the objectives of classifying commonly used antibiotics into six major classes, understanding their mechanisms of action, clinical uses, and side effects.
2) It summarizes the key characteristics and clinical uses of beta-lactams, aminoglycosides, fluoroquinolones, macrolides, tetracyclines, glycopeptides, and metronidazole.
3) It emphasizes the importance of considering pharmacokinetics and the site of infection when selecting an antibiotic to ensure it reaches the infection.
Antibiotic resistance mechanisms

This document discusses antibiotic resistance mechanisms. It defines antimicrobial resistance (AMR) as when microbes become insensitive to medicines, making infections harder to treat. AMR occurs through two main mechanisms: acquired resistance, where bacteria gain resistance genes, usually through overuse of antibiotics creating selective pressure; and intrinsic resistance, where bacteria innately resist certain drug classes. Bacteria develop resistance via decreased permeability, efflux pumps, enzymatic inactivation of drugs like beta-lactamases, and modifying drug targets. Resistance can be transmitted between bacteria through mutation or mobile genetic elements like plasmids.
Sk amd

The document discusses antimicrobial drug resistance (AMDR) and the mechanisms by which microbes develop resistance to antimicrobial medications. It describes classes of AMDR including resistance to antifungal, antiviral, antiprotozoal, and antibacterial drugs. Mechanisms of resistance include altering drug receptors or targets, reducing drug accumulation in cells, inactivating drugs, and developing resistant metabolic pathways. The document also summarizes the cellular and molecular mechanisms of antimicrobial action, including interfering with cell wall synthesis, plasma membrane integrity, nucleic acid synthesis, ribosomal function, and folate synthesis.
Importance of antibiotics and antiseptics , its types and application in the ...

IMPORTANCE OF ANTIBIOTICS AND ANTISEPTICS , ITS TYPES AND APPLICATION IN THE FIELD OF MICROBIOLOGY.
if found Aany mistake plz comment below
Antimicrobial Drugs

This document discusses antimicrobials and their uses. It defines antimicrobials as substances that reduce microbes like bacteria and molds. Antimicrobial drugs are classified based on the microorganisms they target or their function. Broad spectrum antimicrobials affect many types of microbes while narrow spectrum drugs target specific microbes. The document also discusses antimicrobial resistance and how microbes develop resistance. It provides streptomycin as an example antimicrobial drug, describing its discovery, mode of action in inhibiting protein synthesis, and production process. Streptomycin is derived from bacteria and was an early antibiotic used to treat tuberculosis. The document concludes that while antimicrobials are useful, their overuse can lead to increased antimicrobial resistance in micro
Antibiotics - Polypepetide Antibiotics 

Polypeptide antibiotics are a diverse class of natural antibiotics composed of amino acids joined by amide bonds. They are low molecular weight cationic polypeptides that act as powerful bactericidal agents against both gram-positive and gram-negative bacteria. Examples include gramicidin, bacitracin, polymyxin-B, and colistin. These antibiotics act by disrupting bacterial membranes through detergent-like and pseudophore formation mechanisms, leading to ion leakage and inactivation of endotoxins. In addition, chloramphenicol, vancomycin, and novobiocin are classified as miscellaneous antibiotics that have bactericidal properties through inhibition of protein synthesis or bacterial cell wall synthesis.
SAR-Systemic Acquired Resistance 

This document discusses systemic acquired resistance (SAR), a plant defense mechanism that confers broad-spectrum and long-lasting protection against pathogens. SAR involves the signal molecule salicylic acid and accumulation of pathogenesis-related proteins. It provides an alternative to hazardous chemical pesticides and has potential for sustainable agriculture. SAR is induced by necrotic pathogens and results in resistance throughout the plant via a signal transduction pathway involving salicylic acid.
ANTIMICROBIAL DRUGS

This document discusses antimicrobial drugs, including antibiotics. It describes how antibiotics are substances produced by microorganisms that inhibit the growth of other microbes. It outlines several antibiotic-producing microorganisms and explains the mechanisms of action of antimicrobial drugs, including inhibiting cell wall synthesis, protein synthesis, and nucleic acid synthesis. The document also discusses the spectrum of antimicrobial activity and lists some common side effects and safety concerns with antimicrobial use, such as toxicity, resistance, and interaction with other drugs.
Antimicrobial agents and mechanisms of action 2

This document discusses antimicrobial resistance and its mechanisms. It defines antimicrobial resistance and describes how it can arise through mutation or acquisition of genes. It covers various mechanisms of resistance such as production of inactivating enzymes, decreased permeability, efflux pumps, and modification of drug targets. It also discusses specific examples of resistance to beta-lactams, glycopeptides, and antibiotics that inhibit protein synthesis. Key terms related to drug-resistant organisms are defined.
Antimicrobial chemotherapy

This document discusses antimicrobial agents and chemotherapy. It begins by defining antibiotics as natural substances produced by microorganisms that suppress or kill other microorganisms. It then discusses antimicrobial agents, which include both naturally obtained and synthetic drugs that can attenuate microorganisms. Finally, it defines chemotherapeutic agents as drugs designed to inhibit or kill an infecting organism with minimal effect on the recipient. The document goes on to provide details on the classification, mechanisms, principles, development and prevention of antimicrobial resistance.
Antibiotic resistance

Relative or complete lack of effect of antimicrobial agent against a previously susceptible microbe/pathogen.
It is an evolutionary principal that organism adopt genetically to change in their environment.
since the doubling time of bacteria can be as short as 20 mnt, there may be many generations in even a few hours, providing ample opportunity for evolutionary adaptation.
The phenomenon of resistance imposes serious constraints on the options available for the treatment of many bacterial infections.
The resistance to chemotherapeutic agents can also develop in protozoa, in multicellular parasites and in population of malignant cells.
Today there are different strains of S. aureus resistant to almost every form of antibiotic in use.
12.COMPREHENSIVE OFANTIMICROBIAL AGENTS AND CHEMOTHERAPY ( CLASSIFICATION AND...

12.COMPREHENSIVE OFANTIMICROBIAL AGENTS AND CHEMOTHERAPY ( CLASSIFICATION AND...Saminathan Kayarohanam
Antimicrobial Agents and Chemotherapy (AAC) features interdisciplinary studies that build our understanding of the underlying mechanisms and therapeutic applications of antimicrobial and antiparasitic agents and chemotherapy.Mechanism Of Resistance Of Antibiotics

mechanism of resistance of antibiotics, ESBL, b lactums, enterobactericae, metallobactums, carbapenemases, types of mechanism of resistance, history of antibiotics and resistance
Mechanisms of Resistance to Antibiotics

1. Antimicrobial resistance arises through genetic mutations and the acquisition of resistance genes from other bacteria.
2. Resistance genes can be acquired horizontally via mobile genetic elements such as plasmids, leading to rapid spread.
3. Common resistance mechanisms include enzymatic inactivation of antibiotics, modification or protection of antibiotic targets, and efflux pumps that pump out antibiotics.
Antibiotics resistance

Antibiotics, Antibiotics Resistance, Action of Antibiotics, Mechanism of Antibiotics Resistance, Generation of Antibiotics
Antimicrobial agents and mechanisms of action 2

The document discusses antibiotic resistance mechanisms in bacteria. It describes several key mechanisms:
1. Production of enzymes that inactivate antibiotics through destruction or modification. This includes beta-lactamases that break down beta-lactam antibiotics.
2. Decreased permeability of the cell membrane, preventing antibiotic penetration.
3. Active efflux of antibiotics from the bacterial cell via efflux pumps.
4. Modification of antibiotic target sites, such as altered penicillin-binding proteins or modifications to ribosomes.
Resistance can arise through mutation or acquisition of resistance genes via horizontal gene transfer. Multiple resistance mechanisms can provide high-level or multidrug resistance.
Multiple Drug Resistance and Antibiotic Misuse In English.

The report on Multiple Drug Resistance and Antibiotic Misuse.
By: Nadia Hassan, Chandni Yaqoob and Mudassar Iqbal.
School of Biological Sciences, University of the Punjab.
Imipenem cilastatin training

IMIPEN® 500 (imipenem/cilastatin) is a broad-spectrum carbapenem antibiotic used as empirical monotherapy for serious bacterial infections in intensive care unit (ICU) patients. It is effective against both aerobic and anaerobic bacteria, including multidrug-resistant strains. Common serious infections treated with IMIPEN® 500 in the ICU include pneumonia, bloodstream infections, and urinary tract infections. It is administered intravenously in doses ranging from 500 mg to 1000 mg every 6 to 8 hours, depending on infection severity and patient risk factors.
Antibiotic

This document summarizes antibiotics and their mechanisms of action. It discusses how antibiotics were first coined by Waksman to refer to substances produced by microorganisms that inhibit or kill other microorganisms. It then describes the ideal properties of an antibacterial and provides classifications of antibiotics by origin (natural, semi-synthetic, synthetic) and mechanism of action (bactericidal, bacteriostatic). The document proceeds to explain various antibiotic targets and mechanisms in depth, including inhibition of cell wall synthesis, membrane synthesis, protein synthesis, nucleic acid formation, and metabolism. It also notes common antibiotic side effects and challenges in antibiotic research and treatment.
What's hot (20)
Importance of antibiotics and antiseptics , its types and application in the ...

Importance of antibiotics and antiseptics , its types and application in the ...
12.COMPREHENSIVE OFANTIMICROBIAL AGENTS AND CHEMOTHERAPY ( CLASSIFICATION AND...

12.COMPREHENSIVE OFANTIMICROBIAL AGENTS AND CHEMOTHERAPY ( CLASSIFICATION AND...
Multiple Drug Resistance and Antibiotic Misuse In English.

Multiple Drug Resistance and Antibiotic Misuse In English.
Similar to Antibiotics lecture
Antibiotics ppt

- Antibiotics selectively target microbial processes without harming human host cells. Proper antibiotic use and hand hygiene have improved patient outcomes.
- Many antibiotics are naturally produced by bacteria and fungi to inhibit competition. Major classes include penicillins, cephalosporins, aminoglycosides, tetracyclines, macrolides, and sulfonamides.
- Antibiotics work by inhibiting bacterial cell wall, protein, or nucleic acid synthesis. However, antibiotic resistance has emerged through various mechanisms and poses a growing challenge.
Antibiotics

This document discusses antimicrobial agents and antibiotics. It defines antimicrobial agents as chemicals that treat infectious diseases by inhibiting or killing pathogens. Ideal antimicrobial agents kill or inhibit pathogens, are not harmful to the host, cause no allergic reactions, and remain effective after storage and in tissues. The document then discusses different classes of antibiotics based on their source, mechanism of action, and targets, including cell wall synthesis inhibitors like penicillin and vancomycin, protein synthesis inhibitors like tetracyclines and chloramphenicol, and nucleic acid synthesis inhibitors like sulfonamides. It also addresses resistance acquisition through intrinsic, mutational or acquired genetic means.
Antibiotics 091009034052-phpapp01

This document discusses antimicrobial agents and antibiotics. It defines antimicrobial agents as chemicals that treat infectious diseases by inhibiting or killing pathogens. Ideal qualities of antimicrobial agents are listed. Antibiotics are defined as substances derived from microorganisms or produced synthetically that destroy or limit microbial growth. Various classifications of antibiotics are described based on their source, spectrum of activity, route of administration, and mechanism of action. The major mechanisms of action discussed are inhibition of cell wall synthesis, cell membrane function, protein synthesis, and nucleic acid synthesis. Bacterial resistance both intrinsic and acquired is also summarized.
Antibiotics Gen

Antibiotics are metabolites produced by organisms that kill or inhibit the growth of other organisms. There are several classes of antibiotics that work through different mechanisms such as inhibiting bacterial cell wall synthesis, protein synthesis, or nucleic acid synthesis. Resistance can develop when antibiotics are overused or misused, allowing bacteria to mutate or acquire resistance genes. Proper use and preventing overuse can help reduce antibiotic resistance.
Antimicrobial Agents and Antimicrobial Resistance.pptx

The document discusses various aspects of antimicrobial drugs and antibiotic resistance. It defines key terms like antimicrobials, antibiotics, and describes different classes of antibiotics including their mechanisms of action and examples. It discusses factors that influence the effectiveness of antibiotics like spectrum of activity, toxicity and resistance development. It differentiates between acquired and intrinsic antibiotic resistance, and lists factors like overuse/misuse of drugs, poor infection control and inappropriate antibiotic usage as major causes of acquired antibiotic resistance.
Antibiotics and its mechanism of action

Antibiotics are chemical substances that kill or inhibit the growth of microorganisms. They can be classified based on their source (natural, semisynthetic, synthetic), spectrum of activity (broad or narrow), or mechanism of action. Common mechanisms include inhibition of cell wall synthesis, protein synthesis, nucleic acid synthesis, and cell membrane function. Examples provided include penicillins, cephalosporins, carbapenems, glycopeptides, aminoglycosides, macrolides, quinolones, sulfonamides, and metronidazole.
vsv6

Antibiotics can be categorized based on their mechanism of action, including those that inhibit protein synthesis, nucleic acid synthesis, and metabolism. Protein synthesis inhibitors include antibiotics that bind to the 30S or 50S ribosomal subunits, such as aminoglycosides, tetracyclines, chloramphenicol, and macrolides. Nucleic acid synthesis inhibitors include rifampin which inhibits RNA polymerase and quinolones which inhibit DNA gyrase. Antimetabolites like sulfonamides and trimethoprim inhibit steps in folic acid synthesis. Resistance can develop through various mechanisms such as altering the antibiotic target, inhibiting drug influx/efflux, or enzymatic inactivation.
Antimicrobial chemotherapy & bacterial resistance dr. ihsan alsaimary

This document discusses antimicrobial chemotherapy and antibiotic principles. It covers the major classes of antibiotics including cell wall active agents, protein synthesis inhibitors, nucleic acid synthesis inhibitors, and metabolic pathway inhibitors. It describes their mechanisms of action, spectra of activity, and common resistance mechanisms. Key points covered include the importance of appropriate antibiotic usage to prevent resistance, factors influencing antibiotic choice, and definitions of antibiotic properties.
Antimicrobial chemotherapy & bacterial resistance dr. ihsan alsaimary

This document discusses antimicrobial chemotherapy and antibiotic resistance. It provides definitions and principles related to antimicrobial agents, including their spectrum of activity, mechanisms of action against bacteria, and factors that influence antibiotic choice. The document addresses various classes of antibiotics like beta-lactams, glycopeptides, macrolides and their mechanisms. It also discusses concepts like minimum inhibitory concentration, combination therapy, and factors that can accelerate the development of antibiotic resistance.
Antimicrobial chemotherapy & bacterial resistance dr. ihsan alsaimary

This document discusses antimicrobial chemotherapy and antibiotic principles. It covers the major classes of antibiotics including cell wall active agents, protein synthesis inhibitors, nucleic acid synthesis inhibitors, and metabolic pathway inhibitors. It describes their mechanisms of action, spectra of activity, and common resistance mechanisms. Key points covered include the importance of appropriate antibiotic usage to prevent resistance, factors influencing antibiotic choice, and definitions of antibiotic properties.
Antibiotics

This document discusses antimicrobial agents and antibiotic resistance. It defines antimicrobial agents as chemicals that treat infectious diseases by inhibiting or killing pathogens. Ideal antimicrobial agents kill or inhibit pathogens without harming the host. The document then discusses different classes of antibiotics including their sources, mechanisms of action, and examples. It covers antibiotics that inhibit cell wall synthesis, cell membrane function, protein synthesis, and nucleic acid synthesis. The document concludes by discussing intrinsic and acquired antibiotic resistance in bacteria.
DOC-20240211-WA0014..pdf

This document discusses various classes of antibiotics and their mechanisms of action. It describes five main mechanisms: inhibition of cell wall synthesis, inhibition of cell membrane function, inhibition of protein synthesis, and inhibition of nucleic acid synthesis. For each mechanism, it provides examples of antibiotic classes that act through that mechanism, such as beta-lactams that inhibit cell wall synthesis and aminoglycosides that inhibit protein synthesis. It also describes the sources, spectra of activity, and modes of action for many individual antibiotic drugs.
Antibiotics lecture may 2010

This document summarizes various topics related to antimicrobial drugs, including:
- A brief history of antimicrobial drug discovery from Paul Ehrlich's discovery of Salvarsan 606 to treat syphilis to the discovery of sulfa drugs and penicillin.
- Key terminology used to describe antimicrobial drugs and their mechanisms of action, including categories like bacteriostatic, bactericidal, broad spectrum, narrow spectrum, and synergism.
- The main mechanisms of action that antibiotics use to kill or inhibit bacteria, including disrupting cell walls, inhibiting protein synthesis, and inhibiting nucleic acid synthesis.
- Examples of major classes of antibiotics that act through these different mechanisms, such as penicillins
Antibiotics 

This document provides an overview of antibiotics, including their history, classification, mechanisms of action, and principles of administration. It discusses how antibiotics are classified based on their targets in bacteria and spectra of activity. Common antibiotics are also reviewed, along with how bacteria can develop resistance through modifications to antibiotic targets, altered uptake or efflux, and antibiotic inactivation through enzymes. Proper dosing, timing, route, and monitoring of patients are important to achieve the desired therapeutic effects of antibiotics.
Antibiotics, short notes on antibiotics...

Antibiotics are natural compounds produced by microorganisms that inhibit the growth of other microorganisms. They can be classified as bactericidal, killing bacteria, or bacteriostatic, preventing bacterial multiplication. Antibiotics exhibit selective toxicity by targeting microbes without harming host cells. Common mechanisms of action include inhibition of cell wall synthesis, alteration of cell membranes, inhibition of protein synthesis, and inhibition of nucleic acid synthesis.
Pharma 4

Anti-infective agents are drugs designed to selectively target and kill invading microorganisms without harming the host's cells. Paul Ehrlich was the first scientist to develop a synthetic chemical with this property in the 1920s. Anti-infectives work by interfering with microbial cell walls, protein synthesis, DNA synthesis, or cell membranes. Their goal is to reduce microbial populations to levels the immune system can handle. Microbes can develop resistance by modifying drug targets or transport mechanisms. Careful dosing and limiting inappropriate use can help prevent resistance.
Antibiotics

This document provides an overview of antimicrobials (also known as antibiotics). It defines antimicrobials and discusses their classification as bactericidal or bacteriostatic. The document outlines the history of antimicrobial discovery and discusses their sources, selective toxicity, and modes of action. Key topics covered include the classification of antibiotics based on chemical structure and mechanism of action, as well as details on specific classes of antibiotics like penicillins, cephalosporins, carbapenems, and others.
Antibiotics and other chemotherapeutic agents -Antimicrobial spectrum and mod...

Different Antibiotics & chemotherapeutic agents - their mode of action on various microbes; drug resistance
Pharma 2

The document discusses anti-infective agents, which are drugs designed to selectively target and kill invading microorganisms without harming the host's cells. It provides a brief history of anti-infective development and outlines several mechanisms of action, including interfering with bacterial cell wall synthesis, protein synthesis, and DNA synthesis. The document also discusses anti-infective classification, acquiring resistance, treatment considerations, antibiotic classes, and specific aminoglycoside antibiotics.
Similar to Antibiotics lecture (20)
Antimicrobial Agents and Antimicrobial Resistance.pptx

Antimicrobial Agents and Antimicrobial Resistance.pptx
Antimicrobial chemotherapy & bacterial resistance dr. ihsan alsaimary

Antimicrobial chemotherapy & bacterial resistance dr. ihsan alsaimary
Antimicrobial chemotherapy & bacterial resistance dr. ihsan alsaimary

Antimicrobial chemotherapy & bacterial resistance dr. ihsan alsaimary
Antimicrobial chemotherapy & bacterial resistance dr. ihsan alsaimary

Antimicrobial chemotherapy & bacterial resistance dr. ihsan alsaimary
Antibiotics and other chemotherapeutic agents -Antimicrobial spectrum and mod...

Antibiotics and other chemotherapeutic agents -Antimicrobial spectrum and mod...
Antimicrobial drug’s types and classification .pdf

Antimicrobial drug’s types and classification .pdf
More from HandSome
Effective Presentation Skills .pdf

This document provides guidance on developing effective presentation skills. It discusses the key steps in preparing and delivering a presentation, including planning the presentation by determining the audience and goals, preparing the content and structure, practicing with visual aids, and presenting confidently with eye contact and engagement. Specific tips are provided for each step, such as using bullet points and simple designs for slides, varying voice pitch for emphasis, and rehearsing thoroughly. Common challenges like lack of practice and confidence are also addressed, along with factors for a successful presentation like being over-prepared and knowing the topic well.
Blood Collection Tube,ubi.

phlebotomy
different types of tubes used for blood specimen, uses advantages and disadvantages of different tubes.
Biochemistry hand made notes.pdf

This document contains an index of topics related to biochemistry including diet, vitamins, energy metabolism, lipid metabolism, carbohydrate metabolism, protein metabolism, and molecular biology. The index lists over 75 sub-topics ranging from hem biosynthesis and porphyria to DNA structure, replication, and gene transcription.
Sentence structure II (run-on, comma splice, fragment)

The document discusses three types of sentence errors: run-on sentences, comma splices, and sentence fragments. Run-on sentences improperly connect two independent clauses without proper punctuation. Comma splices join two independent clauses with only a comma. Sentence fragments are incomplete sentences missing a subject, verb, or both. The document provides examples and explanations of each error and methods to correct them, such as using periods, semicolons, conjunctions, or turning one clause into a dependent clause.
sentence structure part 1

The document discusses the 4 types of sentence structures: simple, compound, complex, and compound-complex. A simple sentence contains one independent clause. A compound sentence joins two independent clauses with a conjunction. A complex sentence contains one independent clause and at least one dependent clause. A compound-complex sentence contains at least two independent clauses and one or more dependent clauses. Examples are provided for each type of sentence structure.
Communication skills

Communication
Communication skills
Communication types
Communication styles
Communication types
Communication essential skills
Communication knowledge
Communication thinking
Communication ways
Communication levels
verbal Communication
nonverbal Communication
Self Disclosure
Parts of speech ( pdf drive )

Parts of speech
Noun
Pronoun
Adverb
Adjective
Interjection
Conjunction
Articles
Uses of Articles
Types of noun
types of pronoun
Ajective types
Adverb of time manner
adverb of place
examples of articles
Prepositions

The document provides examples of how various prepositions are used with time, place, verbs, adjectives, and idiomatic expressions in English. It lists over 50 individual prepositions like "on", "in", "at", "to", "from", "by", etc. and provides context examples to illustrate their usage related to time, place, or with certain verbs, adjectives, or expressions. The prepositions covered indicate time, location, direction, possession, and relationships between objects, people, or ideas in the English language.
.Mascular system 

.Mascular system
types
muscles
charactersitics
function of muscle
classification of muscles
sarcoplasmic organelles
structure of msucles
how to name muscle
neck muscle
intrinsic back muscle
extrinsic back muscles
anterior compartment of thih muscle
hamstring group muscles
IM injection common sites
muscular tension
Homeostasis 

Homeostasis refers to the maintenance of a stable internal environment in the body. It involves negative feedback loops that counteract changes to keep properties like temperature and pH levels within normal ranges. The concept of homeostasis was introduced by Walter Cannon in 1930 and forms the basis of physiology. It works through a cyclical system of receptors that detect changes, a control center that activates effectors to correct deviations and restore balance. Most processes use negative feedback loops while some emergency responses employ positive feedback. Disruptions to homeostasis can cause illness.
Hormones

Hormones are chemical messengers secreted by endocrine glands directly into the bloodstream to regulate bodily functions. The major endocrine glands include the pituitary gland, thyroid gland, adrenal glands, pancreas, testes and ovaries. Hormones function through a process of biosynthesis in endocrine tissues, storage and secretion, transport through blood to target cells, recognition by cell receptors, signal transduction, cellular response, and hormone breakdown. Hormones are classified as steroid hormones, peptide hormones, or amino acid-derived hormones based on their chemical structure and include molecules like insulin, growth hormone, and thyroxine.
BONES OF EAR

The document discusses the auditory ossicles, which are three small bones in the middle ear - the malleus, incus, and stapes. It describes the role of each bone in transmitting sound vibrations from the eardrum to the inner ear. The malleus is attached to the eardrum and transmits vibrations to the incus, which then passes them to the stapes to reach the inner ear. Together, the three bones mechanically transmit sound through a chain reaction of vibrations. The ossicles also help regulate loud sounds by contracting muscles that reduce the eardrum's vibration. Disorders can occur from conditions like otosclerosis or genetic disorders.
Nutritional classification of bacteria

This document discusses the nutritional classification of bacteria into three main categories:
1) Photoheterotrophs, which use light energy but cannot use CO2 as their sole carbon source and obtain energy from organic compounds. Purple non-sulphur bacteria are examples.
2) Chemoheterotrophs, which obtain carbon and energy from organic compounds like glucose. There are saprophytic, parasitic, and symbiotic chemoheterotrophs.
3) Saprophytic bacteria obtain nutrients from decaying organic matter by secreting enzymes. Parasitic bacteria cause diseases in plants and animals. Symbiotic bacteria like nitrogen-fixing rhizobia live in plants and provide fixed nitrogen in exchange
Carbohydrates

Carbohydrates classidications and examples
isomersims and types of isomerisms
Ketoses
aldoses
chain isomer position isomer
structural isomer
chiral
reducing sugars
monosaccharide
disaccharide
polysaccharide
More from HandSome (16)
Sentence structure II (run-on, comma splice, fragment)

Sentence structure II (run-on, comma splice, fragment)
Recently uploaded
一比一原版(UoA毕业证)昆士兰科技大学毕业证如何办理

UoA毕业证学历书【微信95270640】办文凭{昆士兰科技大学毕业证}Q微Q微信95270640UoA毕业证书成绩单/学历认证UoA Diploma未毕业、挂科怎么办?+QQ微信:Q微信95270640-大学Offer(申请大学)、成绩单(申请考研)、语言证书、在读证明、使馆公证、办真实留信网认证、真实大使馆认证、学历认证
办理国外昆士兰科技大学毕业证书 #成绩单改成绩 #教育部学历学位认证 #毕业证认证 #留服认证 #使馆认证(留学回国人员证明) #(证)等
真实教育部认证教育部存档中国教育部留学服务中心认证(即教育部留服认证)网站100%可查.
真实使馆认证(即留学人员回国证明)使馆存档可通过大使馆查询确认.
留信网认证国家专业人才认证中心颁发入库证书留信网永久存档可查.
昆士兰科技大学昆士兰科技大学毕业证文凭证书毕业证 #成绩单等全套材料从防伪到印刷从水印到钢印烫金跟学校原版100%相同.
国际留学归国服务中心:实体公司注册经营行业标杆精益求精!
国外毕业证学位证成绩单办理流程:
1客户提供办理昆士兰科技大学昆士兰科技大学毕业证文凭证书信息:姓名生日专业学位毕业时间等(如信息不确定可以咨询顾问:我们有专业老师帮你查询);
2开始安排制作昆士兰科技大学毕业证成绩单电子图;
3昆士兰科技大学毕业证成绩单电子版做好以后发送给您确认;
4昆士兰科技大学毕业证成绩单电子版您确认信息无误之后安排制作成品;
5昆士兰科技大学成品做好拍照或者视频给您确认;
6快递给客户(国内顺丰国外DHLUPS等快递邮寄昆士兰科技大学昆士兰科技大学毕业证文凭证书)。闷不乐的样子父亲特意带山娃去找三楼房东家的儿子小伍玩小伍比山娃小一岁虎头虎脑的很霸气父亲让山娃跟小伍去夏令营听课山娃很高兴夏令营就设在附近一所小学山娃发现那所小学比自己的学校更大更美操场上还铺有塑胶跑道呢里面很多小朋友一班一班的快快乐乐原来城里娃都藏这儿来了怪不得平时见不到他们山娃恍然大悟起来吹拉弹唱琴棋书画山娃都不懂却什么都想学山娃怨自己太笨什么都不会斟酌再三山娃终于选定了学美术当听说每月要交感
The Ultimate Guide in Setting Up Market Research System in Health-Tech

How to effectively start market research in the health tech industry by defining objectives, crafting problem statements, selecting methods, identifying data collection sources, and setting clear timelines. This guide covers all the preliminary steps needed to lay a strong foundation for your research.
"Market Research it too text-booky, I am in the market for a decade, I am living research book" this is what the founder I met on the event claimed, few of my colleagues rolled their eyes. Its true that one cannot over look the real life experience, but one cannot out beat structured gold mine of market research.
Many 0 to 1 startup founders often overlook market research, but this critical step can make or break a venture, especially in health tech.
But Why do they skip it?
Limited resources—time, money, and manpower—are common culprits.
"In fact, a survey by CB Insights found that 42% of startups fail due to no market need, which is like building a spaceship to Mars only to realise you forgot the fuel."
Sudharsan Srinivasan
Operational Partner Pitchworks VC Studio
Overconfidence in their product’s success leads founders to assume it will naturally find its market, especially in health tech where patient needs, entire system issues and regulatory requirements are as complex as trying to perform brain surgery with a butter knife. Additionally, the pressure to launch quickly and the belief in their own intuition further contribute to this oversight. Yet, thorough market research in health tech could be the key to transforming a startup's vision into a life-saving reality, instead of a medical mishap waiting to happen.
Example of Market Research working
Innovaccer, founded by Abhinav Shashank in 2014, focuses on improving healthcare delivery through data-driven insights and interoperability solutions. Before launching their platform, Innovaccer conducted extensive market research to understand the challenges faced by healthcare organizations and the potential for innovation in healthcare IT.
Identifying Pain Points: Innovaccer surveyed healthcare providers to understand their difficulties with data integration, care coordination, and patient engagement. They found widespread frustration with siloed systems and inefficient workflows.
Competitive Analysis: Analyzed competitors offering similar solutions in healthcare analytics and interoperability. Identified gaps in comprehensive data aggregation, real-time analytics, and actionable insights.
Regulatory Compliance: Ensured their platform complied with HIPAA and other healthcare data privacy regulations. This compliance was crucial to gaining trust from healthcare providers wary of data security issues.
Customer Validation: Conducted pilot programs with several healthcare organizations to validate the platform's effectiveness in improving care outcomes and operational efficiency. Gathered feedback to refine features and user interface.
Monopoly PCD Pharma Franchise in Tripura

Our company incorporates various drug formulations covering pharma tablets, syrups, capsules, gels, sachets, ointments, creams, injectables.
Mental Health and Physical Wellbeing.pdf

Mental Health and well-being Presentation. Exploring innovative approaches and strategies for enhancing mental well-being. Discover cutting-edge research, effective strategies, and practical methods for fostering mental well-being.
English Drug and Alcohol Commissioners June 2024.pptx

Presentation made by Mat Southwell to the Harm Reduction Working Group of the English Drug and Alcohol Commissioners. Discuss stimulants, OAMT, NSP coverage and community-led approach to DCRs. Focussing on active drug user perspectives and interests
U Part Wigs_ A Natural Look with Minimal Effort Jokerwigs.in.pdf

Joker Wigs has been a one-stop-shop for hair products for over 26 years. We provide high-quality hair wigs, hair extensions, hair toppers, hair patch, and more for both men and women.
2024 Media Preferences of Older Adults: Consumer Survey and Marketing Implica...

When it comes to creating marketing strategies that target older adults, it is crucial to have insight into their media habits and preferences. Understanding how older adults consume and use media is key to creating acquisition and retention strategies. We recently conducted our seventh annual survey to gain insight into the media preferences of older adults in 2024. Here are the survey responses and marketing implications that stood out to us.
Health Tech Market Intelligence Prelim Questions -

The Ultimate Guide to Setting up Market Research in Health Tech part -1
How to effectively start market research in the health tech industry by defining objectives, crafting problem statements, selecting methods, identifying data collection sources, and setting clear timelines. This guide covers all the preliminary steps needed to lay a strong foundation for your research.
This lays foundation of scoping research project what are the
Before embarking on a research project, especially one aimed at scoping and defining parameters like the one described for health tech IT, several crucial considerations should be addressed. Here’s a comprehensive guide covering key aspects to ensure a well-structured and successful research initiative:
1. Define Research Objectives and Scope
Clear Objectives: Define specific goals such as understanding market needs, identifying new opportunities, assessing risks, or refining pricing strategies.
Scope Definition: Clearly outline the boundaries of the research in terms of geographical focus, target demographics (e.g., age, socio-economic status), and industry sectors (e.g., healthcare IT).
3. Review Existing Literature and Resources
Literature Review: Conduct a thorough review of existing research, market reports, and relevant literature to build foundational knowledge.
Gap Analysis: Identify gaps in existing knowledge or areas where further exploration is needed.
4. Select Research Methodology and Tools
Methodological Approach: Choose appropriate research methods such as surveys, interviews, focus groups, or data analytics.
Tools and Resources: Select tools like Google Forms for surveys, analytics platforms (e.g., SimilarWeb, Statista), and expert consultations.
5. Ethical Considerations and Compliance
Ethical Approval: Ensure compliance with ethical guidelines for research involving human subjects.
Data Privacy: Implement measures to protect participant confidentiality and adhere to data protection regulations (e.g., GDPR, HIPAA).
6. Budget and Resource Allocation
Resource Planning: Allocate resources including time, budget, and personnel required for each phase of the research.
Contingency Planning: Anticipate and plan for unforeseen challenges or adjustments to the research plan.
7. Develop Research Instruments
Survey Design: Create well-structured surveys using tools like Google Forms to gather quantitative data.
Interview and Focus Group Guides: Prepare detailed scripts and discussion points for qualitative data collection.
8. Sampling Strategy
Sampling Design: Define the sampling frame, size, and method (e.g., random sampling, stratified sampling) to ensure representation of target demographics.
Participant Recruitment: Plan recruitment strategies to reach and engage the intended participant groups effectively.
9. Data Collection and Analysis Plan
Data Collection: Implement methods for data gathering, ensuring consistency and validity.
Analysis Techniques: Decide on analytical approaches (e.g., statistical
Pneumothorax and role of Physiotherapy in it.

This particular slides consist of- what is Pneumothorax,what are it's causes and it's effect on body, risk factors, symptoms,complications, diagnosis and role of physiotherapy in it.
This slide is very helpful for physiotherapy students and also for other medical and healthcare students.
Here is a summary of Pneumothorax:
Pneumothorax, also known as a collapsed lung, is a condition that occurs when air leaks into the space between the lung and chest wall. This air buildup puts pressure on the lung, preventing it from expanding fully when you breathe. A pneumothorax can cause a complete or partial collapse of the lung.
CHAPTER 1 SEMESTER V COMMUNICATION TECHNIQUES FOR CHILDREN.pdf

Here are some key objectives of communication with children:
Build Trust and Security:
Establish a safe and supportive environment where children feel comfortable expressing themselves.
Encourage Expression:
Enable children to articulate their thoughts, feelings, and experiences.
Promote Emotional Understanding:
Help children identify and understand their own emotions and the emotions of others.
Enhance Listening Skills:
Develop children’s ability to listen attentively and respond appropriately.
Foster Positive Relationships:
Strengthen the bond between children and caregivers, peers, and other adults.
Support Learning and Development:
Aid cognitive and language development through engaging and meaningful conversations.
Teach Social Skills:
Encourage polite, respectful, and empathetic interactions with others.
Resolve Conflicts:
Provide tools and guidance for children to handle disagreements constructively.
Encourage Independence:
Support children in making decisions and solving problems on their own.
Provide Reassurance and Comfort:
Offer comfort and understanding during times of distress or uncertainty.
Reinforce Positive Behavior:
Acknowledge and encourage positive actions and behaviors.
Guide and Educate:
Offer clear instructions and explanations to help children understand expectations and learn new concepts.
By focusing on these objectives, communication with children can be both effective and nurturing, supporting their overall growth and well-being.
一比一原版(USF毕业证)旧金山大学毕业证如何办理

USF毕业证offer【微信95270640】《旧金山大学毕业证购买》《如何办理USF毕业证旧金山大学文凭学历》Q微信95270640实体公司,专业可靠,办理毕业证办美国成绩单,做加拿大文凭学历认证,办新西兰学位证,学位证书是什么?《制作旧金山大学毕业证多少钱》《USF学历证书丢了怎么办理》办澳洲文凭认证,办留信网认证(网上可查,实体公司,专业可靠)
专业为留学生办理旧金山大学旧金山大学硕士学位证成绩单【100%存档可查】留学全套申请材料办理。本公司承诺所有毕业证成绩单成品全部按照学校原版工艺对照一比一制作和学校一样的羊皮纸张保证您证书的质量!
如果你回国在学历认证方面有以下难题请联系我们我们将竭诚为你解决认证瓶颈
1所有材料真实但资料不全无法提供完全齐整的原件。【如:成绩单丶毕业证丶回国证明等材料中有遗失的。】
2获得真实的国外最终学历学位但国外本科学历就读经历存在问题或缺陷。【如:国外本科是教育部不承认的或者是联合办学项目教育部没有备案的或者外本科没有正常毕业的。】
3学分转移联合办学等情况复杂不知道怎么整理材料的。时间紧迫自己不清楚递交流程的。
如果你是以上情况之一请联系我们我们将在第一时间内给你免费咨询相关信息。我们将帮助你整理认证所需的各种材料.帮你解决国外学历认证难题。
国外旧金山大学旧金山大学硕士学位证成绩单办理方法:
1客户提供办理信息:姓名生日专业学位毕业时间等(如信息不确定可以咨询顾问:我们有专业老师帮你查询旧金山大学旧金山大学硕士学位证成绩单);
2开始安排制作旧金山大学毕业证成绩单电子图;
3旧金山大学毕业证成绩单电子版做好以后发送给您确认;
4旧金山大学毕业证成绩单电子版您确认信息无误之后安排制作成品;
5旧金山大学成品做好拍照或者视频给您确认;
6快递给客户(国内顺丰国外DHLUPS等快读邮寄)。头贼脑的倒也逗人喜爱日上三竿时山娃总爱窜进自家瓜棚里跟小伙伴们坐着聊天聊着聊着便忍不住往瓜田里逡巡一番抱起一只硕大的西瓜用石刀劈开抑或用拳头砸开每人抱起一大块就啃啃得满嘴满脸猴屁股般的红艳大家一个劲地指着对方吃吃地笑瓜裂得古怪奇形怪状却丝毫不影响瓜味甜丝丝的满嘴生津遍地都是瓜横七竖八的活像掷满了一地的大石块摘走二三只爷爷是断然发现不了的即便发现爷爷也不恼反而教山娃辨认孰熟孰嫩孰甜孰淡名义上是护瓜吃
Management of Post Operative Pain: to make doctors conscious about the benefi...

Multimodal analgesia.
Daughter's of Dr Ranjit Jagtap (Poulami & Aditi)

The story of Dr. Ranjit Jagtap's daughters is more than a tale of inherited responsibility; it's a narrative of passion, innovation, and unwavering commitment to a cause greater than oneself. In Poulami and Aditi Jagtap, we see the beautiful continuum of a father's dream and the limitless potential of compassion-driven healthcare.
Fit to Fly PCR Covid Testing at our Clinic Near You

A Fit-to-Fly PCR Test is a crucial service for travelers needing to meet the entry requirements of various countries or airlines. This test involves a polymerase chain reaction (PCR) test for COVID-19, which is considered the gold standard for detecting active infections. At our travel clinic in Leeds, we offer fast and reliable Fit to Fly PCR testing, providing you with an official certificate verifying your negative COVID-19 status. Our process is designed for convenience and accuracy, with quick turnaround times to ensure you receive your results and certificate in time for your departure. Trust our professional and experienced medical team to help you travel safely and compliantly, giving you peace of mind for your journey.www.nxhealthcare.co.uk
FACIAL NERVE

The facial nerve, also known as cranial nerve VII, is one of the 12 cranial nerves originating from the brain. It's a mixed nerve, meaning it contains both sensory and motor fibres, and it plays a crucial role in controlling various facial muscles, as well as conveying sensory information from the taste buds on the anterior two-thirds of the tongue.
India Home Healthcare Market: Driving Forces and Disruptive Trends [2029]![India Home Healthcare Market: Driving Forces and Disruptive Trends [2029]](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
![India Home Healthcare Market: Driving Forces and Disruptive Trends [2029]](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
According to the TechSci Research report titled "India Home Healthcare Market - By Region, Competition, Forecast and Opportunities, 2029," the India home healthcare market is anticipated to grow at an impressive rate during the forecast period. This growth can be attributed to several factors, including the rising demand for managing health issues such as chronic diseases, post-operative care, elderly care, palliative care, and mental health. The growing preference for personalized healthcare among people is also a significant driver. Additionally, rapid advancements in science and technology, increasing healthcare costs, changes in food laws affecting label and product claims, a burgeoning aging population, and a rising interest in attaining wellness through diet are expected to escalate the growth of the India home healthcare market in the coming years.
Browse over XX market data Figures spread through 70 Pages and an in-depth TOC on "India Home Healthcare Market”
https://www.techsciresearch.com/report/india-home-healthcare-market/15508.html
India Medical Devices Market: Size, Share, and In-Depth Competitive Analysis ...

According to TechSci Research report, “India Medical Devices Market Industry Size, Share, Trends, Competition, Opportunity and Forecast, 2019-2029,” the India Medical Devices Market was valued at USD 15.35 billion in 2023 and is anticipated to witness impressive growth in the forecast period, with a Compound Annual Growth Rate (CAGR) of 5.35% through 2029. This growth is driven by various factors, including strategic collaborations and partnerships among leading companies, a growing population, and the increasing demand for advanced healthcare solutions.
Recent Trends
Strategic Collaborations and Partnerships
One of the most significant trends driving the India Medical Devices Market is the increasing number of collaborations and partnerships among leading companies. These alliances aim to merge the expertise of individual companies to strengthen their market position and enhance their product offerings. For instance, partnerships between local manufacturers and international companies bring advanced technologies and manufacturing techniques to the Indian market, fostering innovation and improving product quality.
Browse over XX market data Figures and spread through XX Pages and an in-depth TOC on " India Medical Devices Market.” - https://www.techsciresearch.com/report/india-medical-devices-market/8161.html
Solution manual for managerial accounting 18th edition by ray garrison eric n...

Solution manual for managerial accounting 18th edition by ray garrison eric n...rightmanforbloodline
Solution manual for managerial accounting 18th edition by ray garrison eric noreen and peter brewer_compressed
Solution manual for managerial accounting 18th edition by ray garrison eric noreen and peter brewer_compressednurs fpx 4050 assessment 4 final care coordination plan.pdf

nurs fpx 4050 assessment 4 final care coordination plan.pdf
Data-Driven Dispensing- Rise of AI in Pharmacies.pdf

Imagine AI making your pharmacy experience smoother, safer, and more personalized.
Recently uploaded (20)
The Ultimate Guide in Setting Up Market Research System in Health-Tech

The Ultimate Guide in Setting Up Market Research System in Health-Tech
English Drug and Alcohol Commissioners June 2024.pptx

English Drug and Alcohol Commissioners June 2024.pptx
U Part Wigs_ A Natural Look with Minimal Effort Jokerwigs.in.pdf

U Part Wigs_ A Natural Look with Minimal Effort Jokerwigs.in.pdf
2024 Media Preferences of Older Adults: Consumer Survey and Marketing Implica...

2024 Media Preferences of Older Adults: Consumer Survey and Marketing Implica...
Health Tech Market Intelligence Prelim Questions -

Health Tech Market Intelligence Prelim Questions -
CHAPTER 1 SEMESTER V COMMUNICATION TECHNIQUES FOR CHILDREN.pdf

CHAPTER 1 SEMESTER V COMMUNICATION TECHNIQUES FOR CHILDREN.pdf
Management of Post Operative Pain: to make doctors conscious about the benefi...

Management of Post Operative Pain: to make doctors conscious about the benefi...
Fit to Fly PCR Covid Testing at our Clinic Near You

Fit to Fly PCR Covid Testing at our Clinic Near You
India Home Healthcare Market: Driving Forces and Disruptive Trends [2029]![India Home Healthcare Market: Driving Forces and Disruptive Trends [2029]](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
![India Home Healthcare Market: Driving Forces and Disruptive Trends [2029]](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
India Home Healthcare Market: Driving Forces and Disruptive Trends [2029]
India Medical Devices Market: Size, Share, and In-Depth Competitive Analysis ...

India Medical Devices Market: Size, Share, and In-Depth Competitive Analysis ...
Solution manual for managerial accounting 18th edition by ray garrison eric n...

Solution manual for managerial accounting 18th edition by ray garrison eric n...
nurs fpx 4050 assessment 4 final care coordination plan.pdf

nurs fpx 4050 assessment 4 final care coordination plan.pdf
Data-Driven Dispensing- Rise of AI in Pharmacies.pdf

Data-Driven Dispensing- Rise of AI in Pharmacies.pdf
Antibiotics lecture
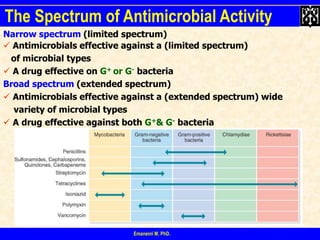
- 1. Emaneini M. PhD. The Spectrum of Antimicrobial Activity Narrow spectrum (limited spectrum) Antimicrobials effective against a (limited spectrum) of microbial types A drug effective on G+ or G- bacteria Broad spectrum (extended spectrum) Antimicrobials effective against a (extended spectrum) wide variety of microbial types A drug effective against both G+& G- bacteria
- 2. Emaneini M. PhD. The Action of Antimicrobial Drugs Bactericidal Kill microbes directly Bacteriostatic Prevent microbes from growing
- 3. Emaneini M. PhD. Mechanisms of Antibiotics Action
- 4. Emaneini M. PhD. 1- Inhibition of Cell Wall Synthesis 2- Injuring the Plasma Membrane 3- Inhibition of Protein Synthesis 4- Inhibition of Nucleic Acid Synthesis 5- Inhibiting the Synthesis of Essential Metabolites Mechanisms of Antibiotics Action
- 5. Emaneini M. PhD. Inhibition of Cell Wall Synthesis Transpeptidases, Carboxypeptidases, Transglycosylases Penicillin-binding proteins (PBPs( β-Lactam antibiotics: generally are bactericidal agents
- 6. Emaneini M. PhD. 1- Beta-Lactam Antibiotics Penicillins Cephalosporins 2- Glycopeptides Vancomycin 3- Lipopeptides Daptomycin 4- Polypeptides Bacitracin Inhibition of Cell Wall Synthesis
- 7. Emaneini M. PhD. Inhibition of Cell Wall Synthesis Isoniazid, Ethionamide, Ethambutol, & Cycloserine Used for the treatment of mycobacterial infections Isoniazid Isonicotinic acid hydrazide [INH]) Bactericidal; Blocks mycolic acid synthesis Ethionamide Derivative of INH Blocks mycolic acid synthesis Ethambutol Interferes with the synthesis of arabinogalactan in the cell wall Cycloserine Inhibits D-alanine-Dalanine synthetase & Alanine racemase
- 8. Emaneini M. PhD. Injuring the Plasma Membrane 1- Lipopeptides Daptomycin 2- Polypeptides Polymyxins
- 9. Emaneini M. PhD. Inhibition of Protein Synthesis
- 10. Emaneini M. PhD. Chloramphenicol Broad spectrum Bacteriostatic Blocking peptide elongation Binding reversibly to the peptidyl transferase (50S) Only for the treatment of typhoid fever Can produce aplastic anemia (1 per 24,000 treated patients) Resistance: plasmid-encoded chloramphenicol acetyltransferase
- 11. Emaneini M. PhD. Inhibition of Nucleic Acid Synthesis 1- Quinolones 2- Rifampin 3- Metronidazole
- 12. Emaneini M. PhD. Synthetic Inhibit bacterial DNA gyrases (II) or topoisomerases (IV) Nalidixic acid Fluoroquinolones: Ciprofloxacin Levofloxacin Gatifloxacin Resistance: mutations in chromosomal genes of DNA gyrases (II) or topoisomerases (IV) Quinolones
- 13. Emaneini M. PhD. Antimetabolites Sulfonamides Preventing the synthesis of the folic acid Compete with p-aminobenzoic acid Mammalian organisms do not synthesize folic acid Treatment of Nocardia, Chlamydia, & some protozoa infections Sulfacetamide Sulfadiazine Sulfisoxazole R Group