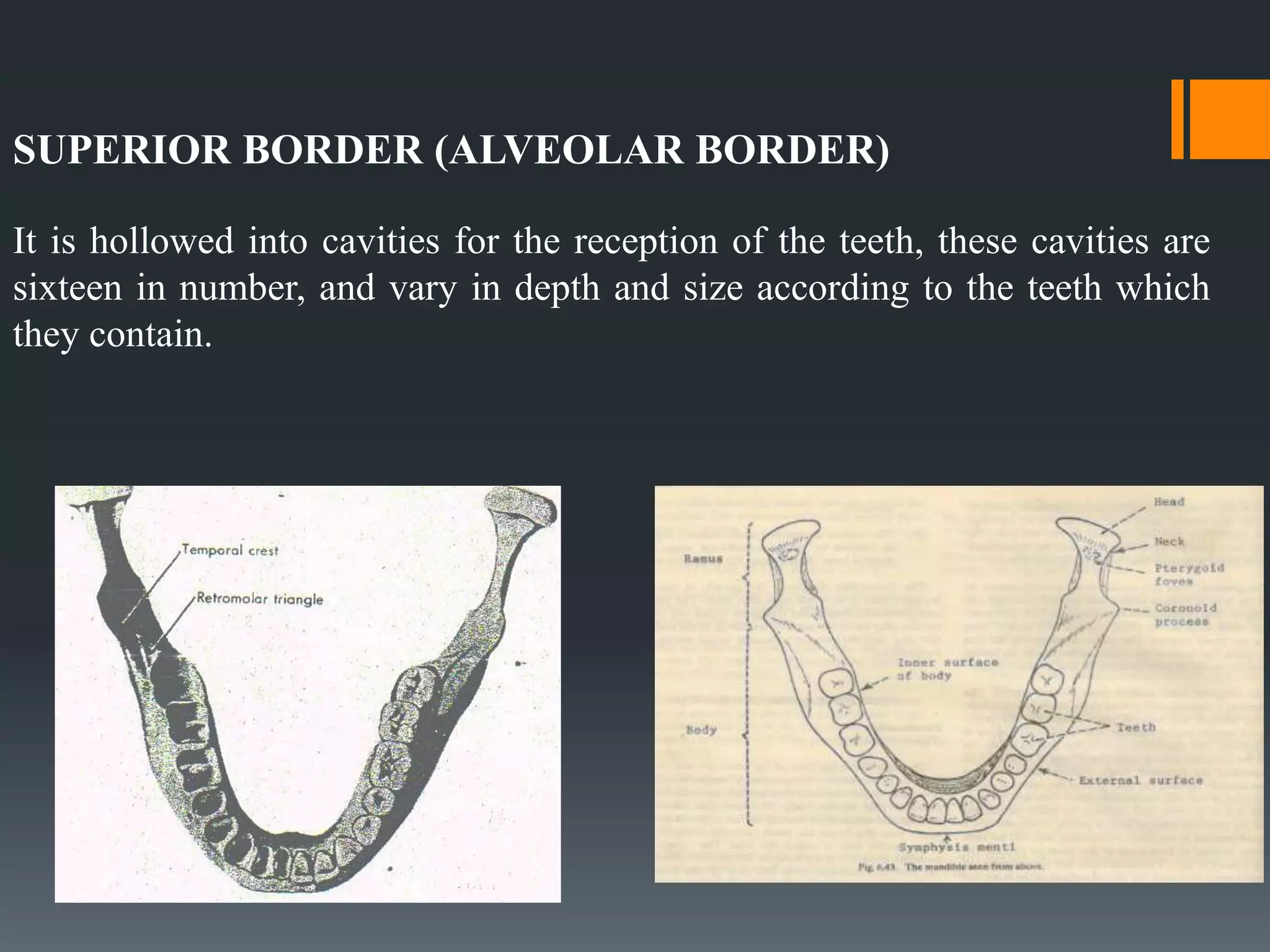
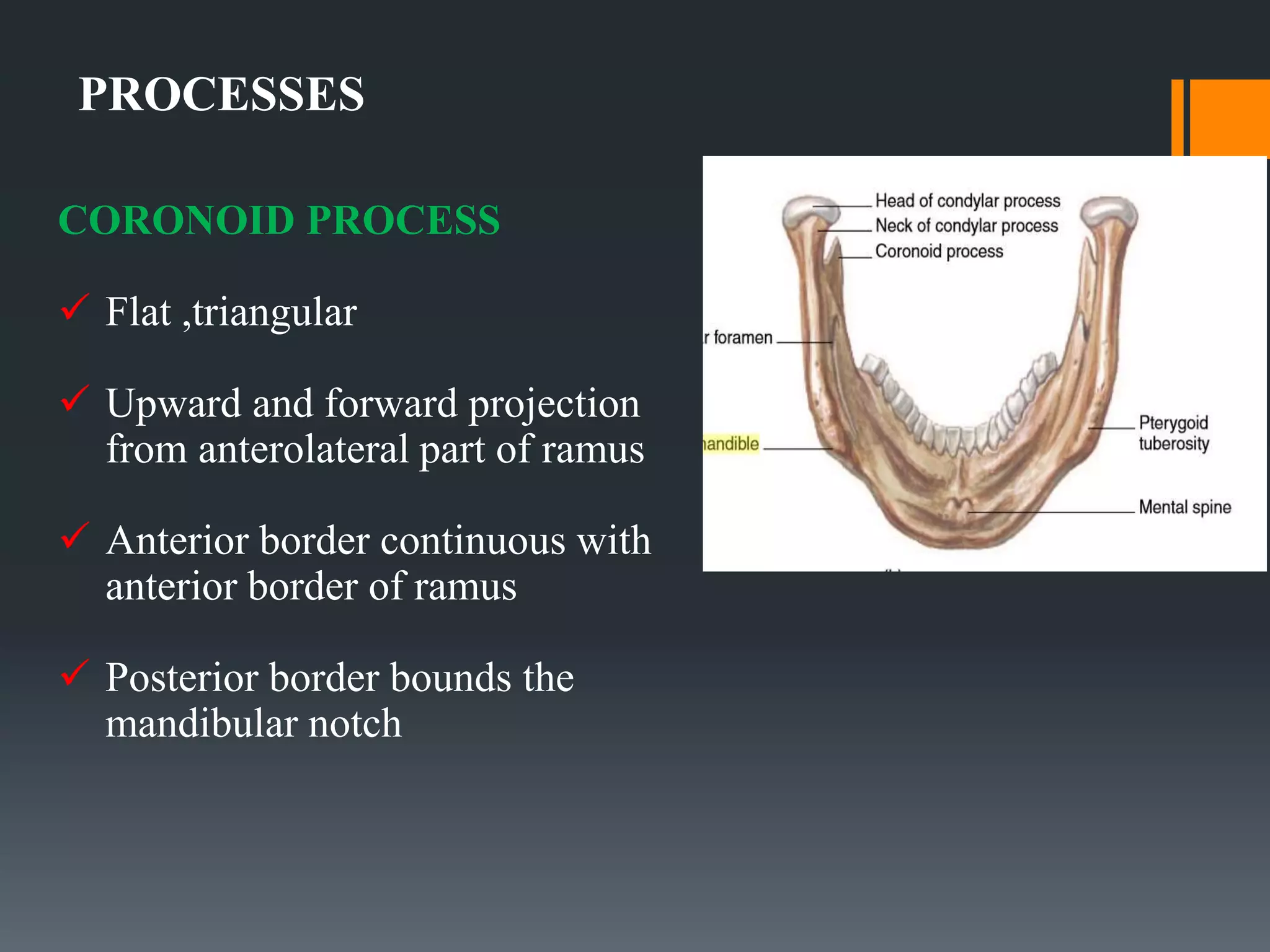
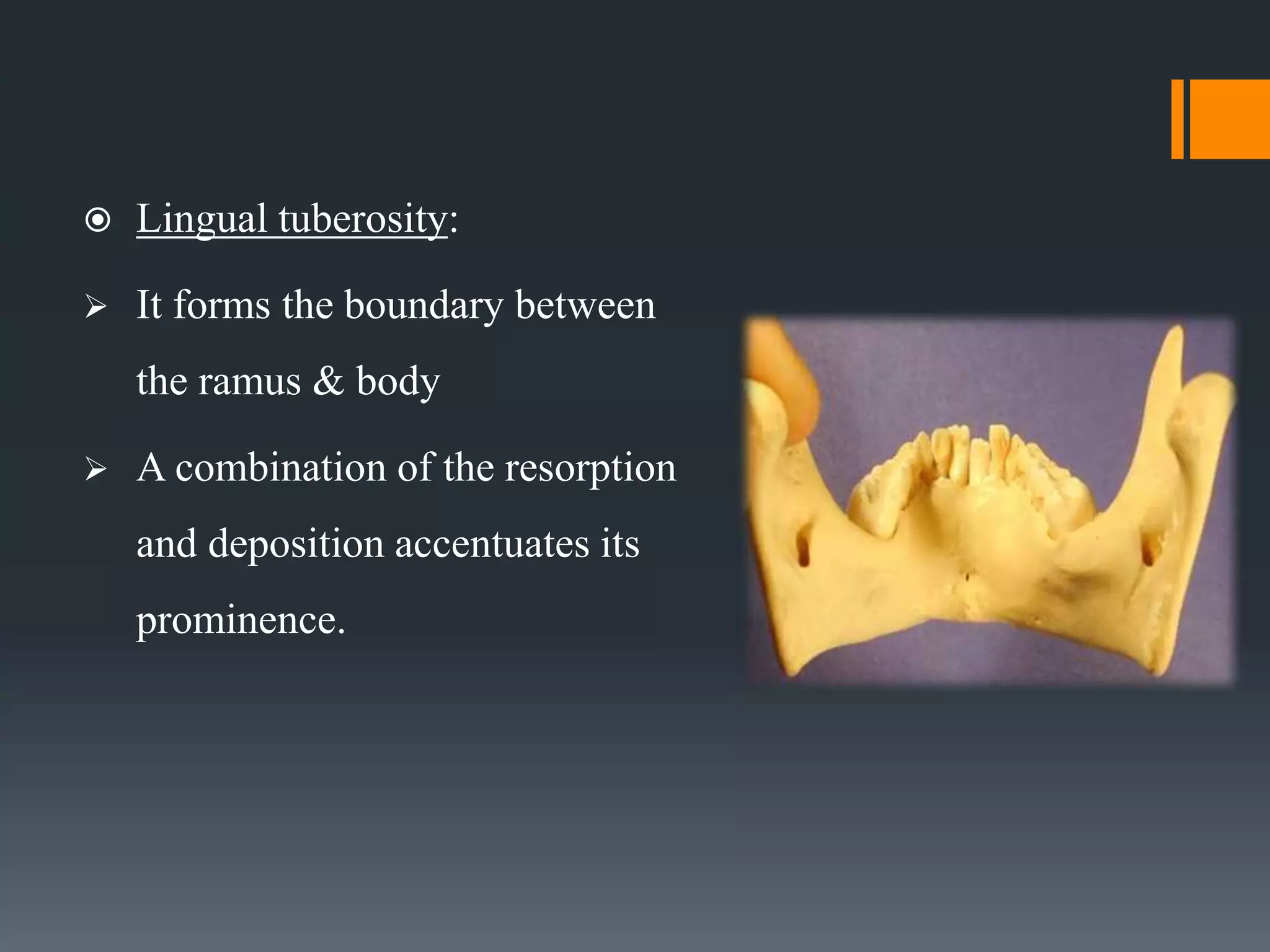
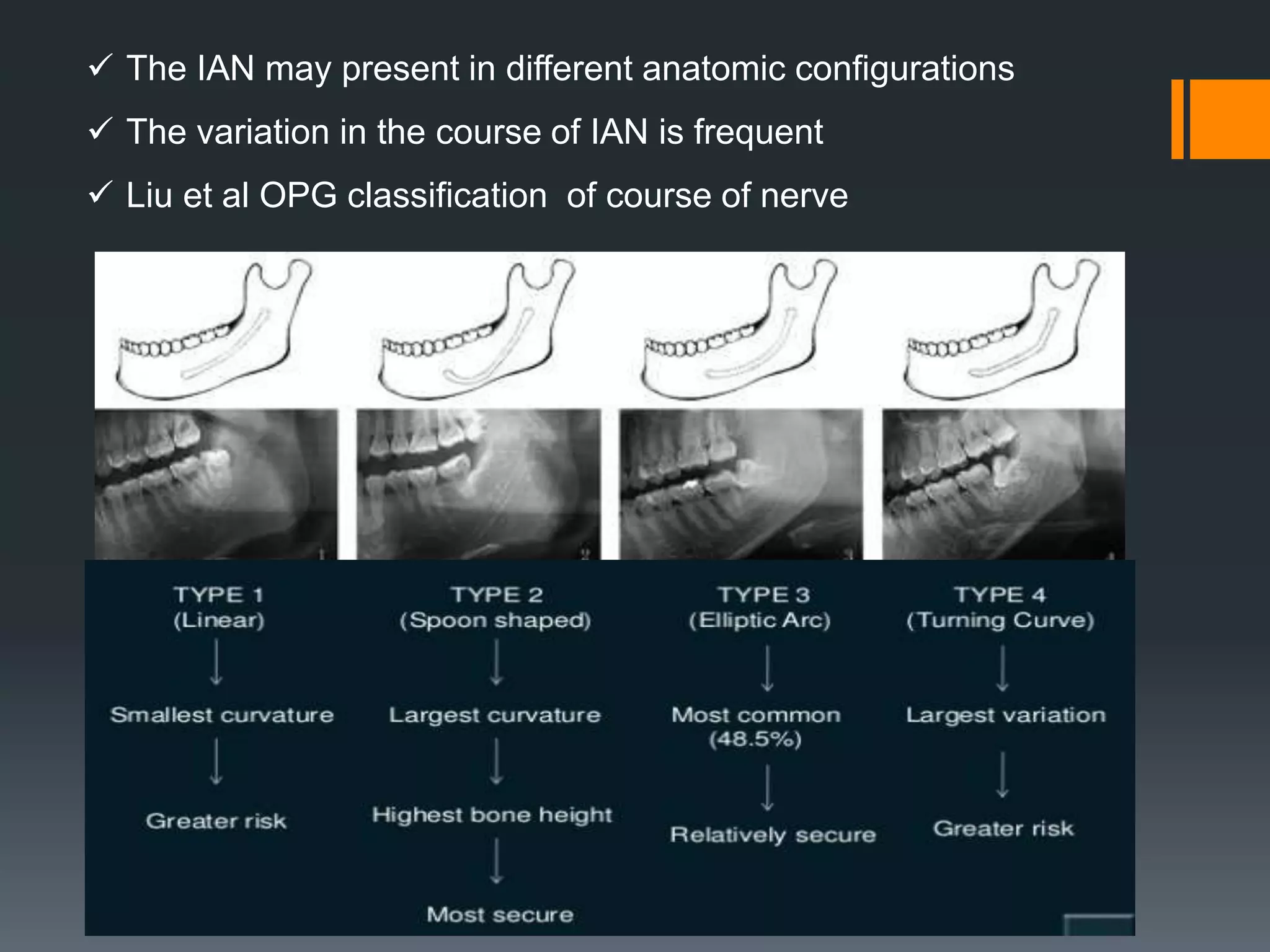
This document discusses the anatomy and importance of the mandible in implant placement. It begins by defining the mandible and its embryological development. It then describes the osteology and features of the body, rami, processes, borders and attachments in detail. It discusses the blood supply, nerve supply and growth of the mandible postnatally. Finally, it explains the applied anatomy of the mandible and importance of anatomical structures like the mandibular foramen, inferior alveolar canal, mental foramen and nerve, and mandibular incisive canal in safe implant placement.