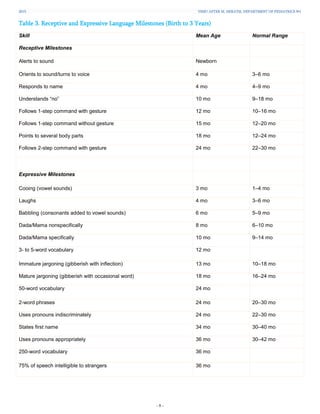
A 12-month-old girl is not yet walking, which concerns her parents. She can pull herself up and stand while holding furniture but does not cruise. Her development was previously assessed as normal. Development is assessed across five domains: gross motor, fine motor, language, social, and self-help skills. Milestones for a 12-month-old include walking, pincer grasp, and social skills like joint attention. Screening tests could further assess her development. Developmental delay is defined as skills significantly below what is expected for age.



![2016 YSMU AFTER M. HERATSI. DEPARTMENT OF PEDIATRICS №1
- 5 -
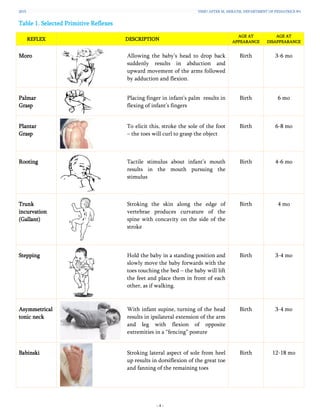
Table 2. Selected Postural Reactions
REACTION DESCRIPTION
AGE AT
APPEARANCE
AGE AT
DISAPPEARANCE
Righting
Reactions
These allow the body to maintain normal postural relationships of
the head, trunk, and extremities during all activities. The different
reactions appear at different ages, beginning shortly after birth and
ranging up to 12 months of age.
Never
Protective
Equilibrium
Response
When gently pushed toward one side
while in a sitting position, infants
increase trunk flexor tone toward that
side to regain their center of gravity and
extend the arm on the same side to
protect against falling.
4-6 mo Never
Parachute
Refactions
When held in ventral suspension and
suddenly lowered (downward
parachute), infants extend their arms as
if to protect themselves from a fall;
similar reactions are seen with forward
and backward stimulation.
8–10 mo Never
Gross Motor Skills
During the first year of life, the ultimate goal of gross
motor development is walking. The first step toward
this goal is head control. By 6 months of age, children
are able to sit without support for a few seconds (Figure
2). At 9 to 10 months of age, children are able to pull
themselves to a standing position, and by 12 to 17
months of age, they are able to walk. Children then
learn to run, negotiate stairs, hop on one foot, and skip
— in that order.
Figure 2. Stages in the development of sitting. A, Head
control. B, “Tripod sitting.” C, Head steady and back
straight without support
Variation
There is wide variability in the ‘normal ranges’. This is
particularly so with walking – normal children may
walk from 11–18 months (Figure 3). If they bottom
shuffle (instead of crawling), they generally walk late
as bottom shuffling is so efficient.
Figure 3. Windows of milestone achievement expressed in months
[WHO Motor Development Study. Acta Pædiatrica, 2006; Suppl 450: 86_/95]](https://image.slidesharecdn.com/3-180325072919/85/3-pediatric-development-5-320.jpg)