Ent part ii
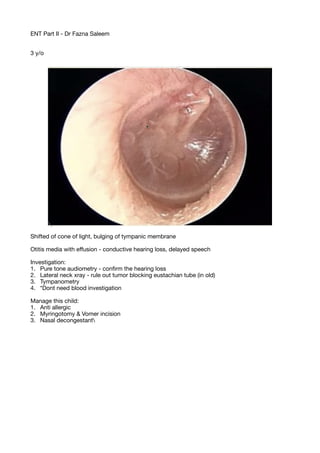
- 1. ENT Part II - Dr Fazna Saleem 3 y/o Shifted of cone of light, bulging of tympanic membrane Otitis media with e ff usion - conductive hearing loss, delayed speech Investigation: 1. Pure tone audiometry - con fi rm the hearing loss 2. Lateral neck xray - rule out tumor blocking eustachian tube (in old) 3. Tympanometry 4. *Dont need blood investigation Manage this child: 1. Anti allergic 2. Myringotomy & Vomer incision 3. Nasal decongestant
- 2. Tympanic membrane is retracted, Handle of malleus - more prominent, long process and short hand of incus Pathophysiology: Eustachian tube edema - negative pressure in middle ear Valsalva manuevre - no movement/ no changes in total perforation, movement present in TM retraction
- 3. On right side tympanogram shows curve is fl at and no value (type B) - fl uid in middle ear or tympanic membrane perforation The left side is normal tympanogram - Type A which is Normal
- 4. Elderly, chronic discharge, foul smelling Erythema, Cone of light slightly shifted, granulation tissue in (attic) pars fl accida, yellowish mass, no perforation, no pus, no discharge Most likely - CSOM Atticoantral type Cholesteatoma Management: Examination under microscope Audiometry , Pus culture and sensitivity, Mastoid xray Tx: Aural toilet, painkillers, systemic antibiotic, removal of granulation tissue by surgery (mastoidectomy)
- 5. Grommet tube / Tympanostomy tube Indication: 4. Otitis media with e ff usion 5. Retracted tympanic membrane - to allow ventilation 6.
- 6. Fever, ear pain, hearing loss Tympanic membrane shows tense and bulging, no perforation, erythematous Most likely: Acute otitis media
- 7. Cotton wool appearance Most likely: Otomycosis ( fungal infection ) CF: itchiness, irritation, discharge Investigation: Swab culture ssnsitivity, examination under microscope Mx: Aural toilet, Topical antifungal
- 9. Patient has on and o ff persistent discharge for 2 years, hearing loss Findings: Perforation of tympanic membrane on pars tensa, angle of malleus, pars fl accida is intact Dx: Inactive CSOM with tubotympanic (central perforation) Mx: Surgery (myringoplasty) - since it is inactive; no discharge, no fever
- 10. Pure tone audiometry of right ears shows air bone gap with moderate conductive hearing loss (Di ff erences should be more than 20 to be signi fi cant)
- 11. Pure tone audiometry of both ears is between 70-90, air conduction isair bone gap is present which suggest bilateral severe mix type of hearing loss of severe degree Possible causes: Conductive: Otitis media, externa, impacted ear wax, e ff usion, FB Sensorineural: labyrinthitis, ototoxicity drugs Audiometry fi ndings: 1. Conductive - bone conduction is Normal (C), air conduction is abnormal, (around 20), Positive Air bone gap 2. Sensorineural - Bone conduction is abnormal, Air conduction is abnormal, no air bone gap 3. Mix - bone conduction abnormal (below 20), air conduction is abnormal, present of air bone gap
- 12. Peak on negative zone, shows Type C tympanogram Causes: 1. Early Otitis media with e ff usion 2. Eustachian tube dysfunction
- 13. Redness/ Eythema on skin over mastoid Tenderness on mastoid bone Most likely: Acute mastoiditis Xray of mastoid bone - looking for air cells Culture and sensitvity for discharge Mx: Admit + IV Antibiotic, can change to oral antibiotic later
- 14. Face - unilateral palsy, angle mouth deviation towards left side, inable to closure of eyelids of right, nasolabial fold is less prominent on right side Most likely: Right facial nerve palsy Ear - redness, crusting, pinna vesicles Most likely: Herpes Zoster - Ramsay Hunt syndrome
- 15. Shows tympanic membrane with central perforation on pars tensa, with tympanic sclerosis (calcium sclerotic patches) Myringoplasty - graft from tragus/ subcutaneos fascia. Only repair the tympanic membrane without exploration Tympanoplasty - done in case when ossciles destroyed, atticoantral - so repair part of the middle ear with tympanic membrane repair (with exploration of middle ear)
- 16. Mass with pale, glossy appearance originate from above, no discharge, no mucus Most likely: Nasal polyp Nasal polyp vs turbinate Polyp - pale, glossy appearance Turbinate - fl eshy, originate from lateral wall Probe the mass - if painful (turbinate) Gross appearance - 2 types of nasal polyp: 1. Ethmoidal polyp 2. Anthrocoanal polyp
- 17. CT scan of Paranasal sinus - right maxillary sinus is denser (congested), left side is congested with hypoechoic area (normal - fi lled with air), hypertrophy of right turbinate Bilateral maxillary sinusitis (right side is more severe) CF: 1. Fever 2. Purulent nasal discharge 3. Headache
- 18. There is Perforated nasal septum with eryhthema surrounding peforation, no discharge Causative of perforation; 1. chronic infection like Tb 2. Sni ffi ng drugs 3. Trauma - surgical or nasal bone fracture Symptoms: 1. Whistling breathing 2. Crusting sensation 3. Epistaxis
- 19. Discoloration, erythema, swelling of left vestibule, some discharge, crusting formation Dx: Vestibulitis Mx: 1. Admit and IV antibiotic (due to Danger’s area) 2. Removal of crusting
- 20. Showing of bilateral septal hematoma (originate from medial wall) Causes: 1. Bleeding disorder 2. Nasal trauma 3. Surgery Investigation: 1. Blood coagulation pro fi le Tx: 1. Aspiration with wide bore needle or 2. Incision and drainage 3. To avoid recurrence - bilateral nasal packing + prophylactic antibiotic Complications: 1. Septal perforatio 2. Septal abscess
- 21. Xray of paranasal sinus, Waters view shows hyperdense of right maxillary sinus
- 22. History: 2 weeks of high fever, purulent nasal discharge Redness and edema around left eye Most likely dx: Periorbital cellulitis complication from Ethmoidal sinusitis Complications: Orbital cellulitis Orbital abscess Cavernous sinus thrombosis Investigation: 1. CT scan (to rule out complication and extend of diseases) 2. Naso endoscopy (to look for discharge, status of sinus, inferior meatus etc) Mx: 1. Admit and IV antibiotic 2. Monitor progress - if worsening - incision and drainage
- 23. Swelling at lower lobe of ear at angle of mandible, rounded swelling, surface is smooth, overlying skin is …, approximate size 2 by 2 cm, Di ff erential diagnosis: 1. Lymphadenopathy Investigation: 1. Full blood count 2. FNAC 3. USG of swelling - to see whether its fl uid- fi lled and rule out other diagnosis
- 24. A. Posterior Nasal Packing B. Posterior nasal bleeding due to uncontrolled htn, bleeding disorder,tumors C.
- 25. A. Saddle nose deformity B. Nasal bone fracture, trauma, nasal tumor, septal abscess C. Surgical procedure - rhinoplasty or septoplasty or septorhinoplasty
- 26. Nasal endoscopic pictures show middle meatus with purulent discharge Nasal polyp
- 27. Greyish, glistening, pale - polyp
- 28. Findings: Swelling over mandible which is size, shape, surface, skin, Most likely: Pleomorphic adenoma (swelling of parotid gland) Investigation; 1. FNAC 2. USG
- 29. Deviated Nasal Septum (bony projection) Hematoma - should be on both side
- 30. Bilateral, Sessile swelling on anterior 1/3 to posterior 2/3 junction of vocal cord Dx: Vocal cord nodules Mx: Voice rest, speech therapy Usually singer, teacher
- 31. Findings: Uvula is enlarged, tonsils is bilaterally enlarged, no exudate Grading of tonsils: 1. Grade 1 - cover the anterior pillar 2. Grade 2 - just reach the posterior pillar 3. Grade 3 - cant visualize the posterior pillar 4. Grade 4 - both of tonsils reach midline
- 32. Lateral neck xray shows Thumb sign appearance Acute epiglotitis CF: 1. Stridor 2. Drooling of saliva (severe odynophagia) 3. High fever, toxic looking 4. Sign - tripod sign (chin lifted - to increase airway) Management: 1. ABC - secure airway, secure IV line 2. Admit the patient 3. IV antibiotics with O2 supplementation No endoscopy, no tongue depression
- 33. Tonsillectomy Indications: 1. Recurrent infection of tonsil 2. Recurrent peritonsilar abscess 3. Obstructive symptoms with chronic hypertrophied tonsils Contraindications: 1. Bleeding disorder 2. Active infection on going Complications 1. Injury to other structures (tooth, oropharyngeal) 2. Aspiration 3. Hemorrhage Late complications: Secondary bleeding, infarction Check for Hb, coagulation pro fi le
- 34. Findings: Oropharynx wall - edematous vesicular lesion, cobblestone appearance Diagnosis: Chronic pharyngitis Features: 1. Uneasiness of throat 2. Foreign body sensation Management: Antiseptic gargling Cauterisation - to remove hypertophy (in very severe cases)
- 35. 1. Tracheostomy 2. Indication: Epiglotitis, laryngeal edema, prolong intubation, laryngeal tumors, laryngomalacia, retained secretion in lung, spinal trauma, bulbar palsy, respiratory insu ffi ciency, fi brosis, chronic lung diseases 3. 4 complications: Injury to RLN, hemorrhage, injury to thyroid, subcutaneous emphysema (very common), apnoea (less CO2 to drive for respiration- which lead to paradoxical apnoea) 4. Post operative management and care - make sure no bleeding, daily dressing, supply with oxygen, regular suction
- 36. Left side of soft palate is swollen, uvula shifted to right Diagnosis: Peritonsilar abscess (Quinsy) Causes; 1. Recurrent tonsillitis 2. Foreign body throat Management: 1. Admit 2. Analgesics 3. Incision and drainage
- 37. Single, Unilateral, Pedunculated swelling on anterior 1/3 of right vocal cord Dx: Vocal cord polyp Symptoms; 1. Diplophonia 2. Hoarseness of voice 3. Dysphonia 4. Stridor 5. Obstructive symptoms Treatment: 1. Mainstay - surgery (microlaryngeal surgery with poypectomy)
- 38. Nasopharynx shows edematous lesion with bleeding, shiny and bulging appearance which arise from fossa of Rosenmüller Dx: Nasopharyngeal carcinoma Symptoms: Early 1. Unexplained epistaxis 2. Unexplained lymph node swelling 3. Commonest cranial nerve involvement (abducens nerve - lateral rectus palsy - medial squint) Late presentation 1. Naso obstruction (late presentation, when mass is big) 2. Hearing loss Treatment: 1. Radiotherapy and chemotherapy
