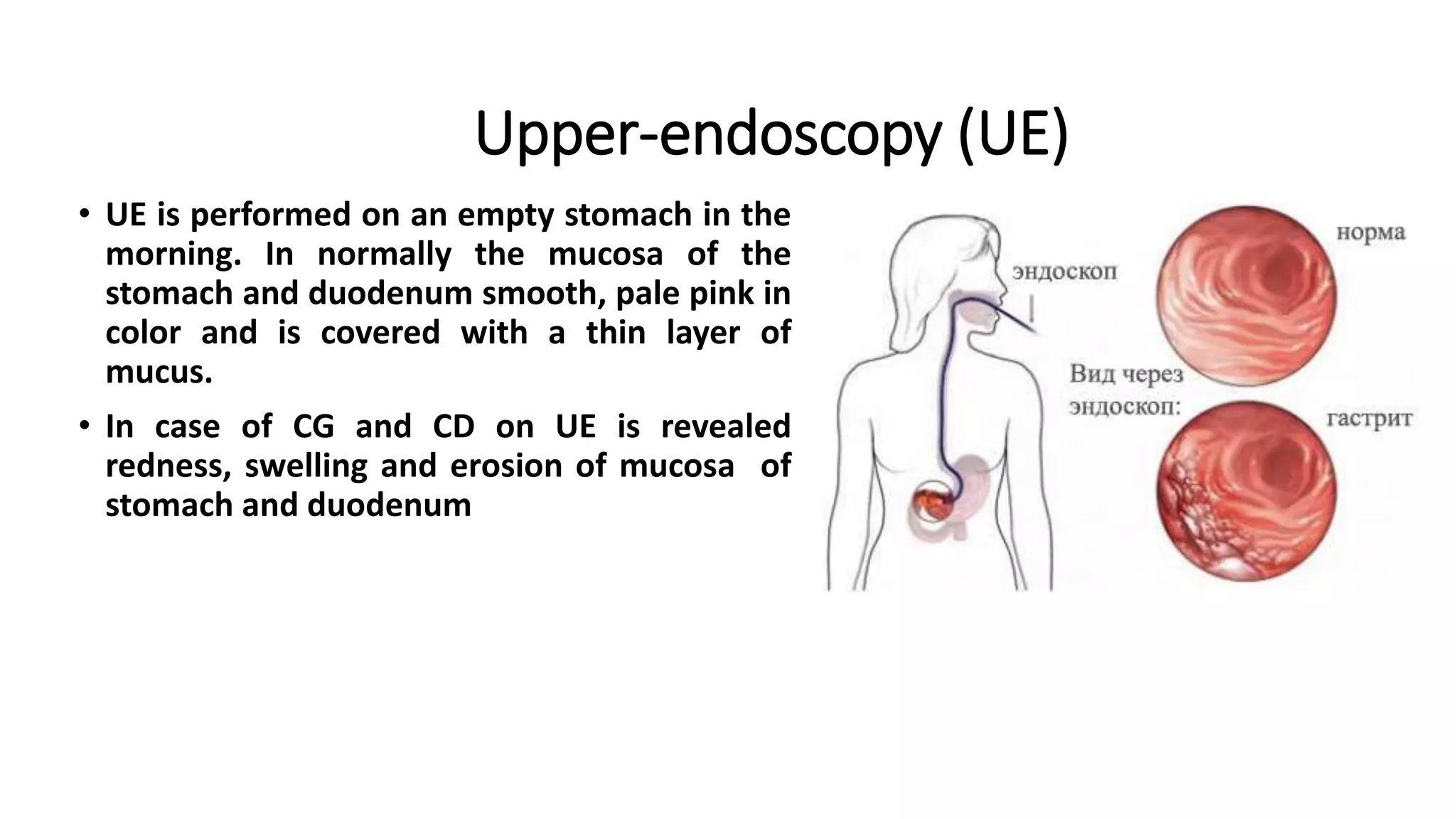
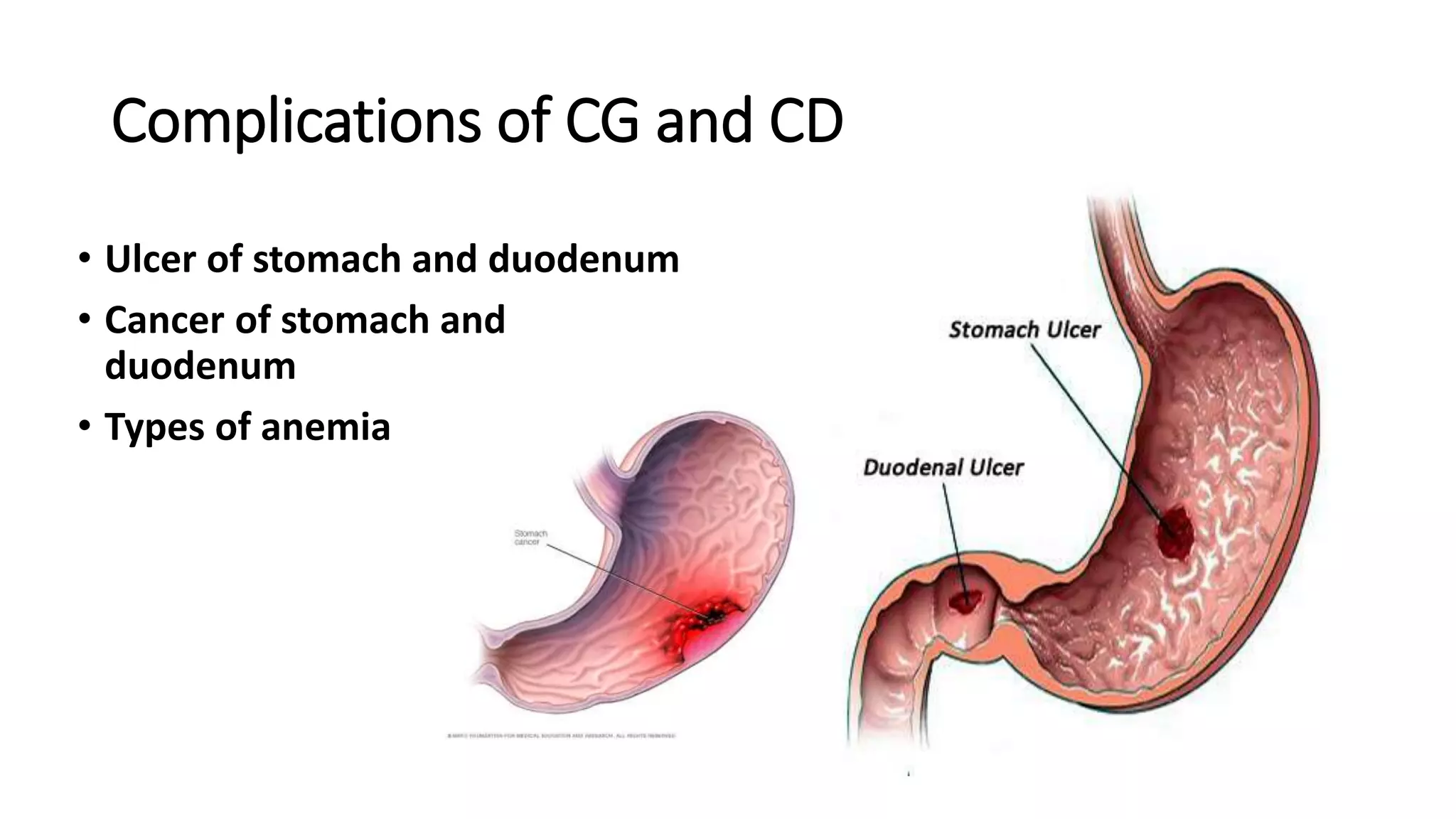
Chronic gastritis is a chronic inflammation of the gastric mucosa that commonly results from infection by Helicobacter pylori in 90% of cases. Other causes include NSAID use, smoking, stress, and ischemia. H. pylori infection leads to increased acid secretion and damage to the gastric epithelium. Chronic gastritis is classified based on location and cause, and is usually asymptomatic, though pain, dyspepsia, and fatigue may occur. Diagnosis involves endoscopy, biopsy, and urease testing. Treatment focuses on H. pylori eradication therapy using antibiotic combinations for 10-14 days along with diet and lifestyle modifications. Complications include ulcers, gastric cancer, and