Mechanisms of coagulation B.pharmacy 2 semester
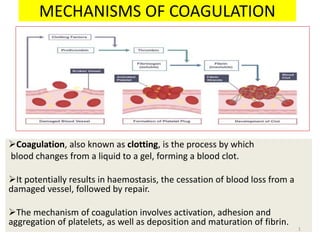
- 1. MECHANISMS OF COAGULATION Coagulation, also known as clotting, is the process by which blood changes from a liquid to a gel, forming a blood clot. It potentially results in haemostasis, the cessation of blood loss from a damaged vessel, followed by repair. The mechanism of coagulation involves activation, adhesion and aggregation of platelets, as well as deposition and maturation of fibrin. 1
- 2. 2
- 3. 3
- 4. 4
- 5. 5
- 6. 6
- 7. INTRINSIC PATHWAY FOR THE FORMATION OF PROTHROMBIN ACTIVATOR • During the injury, the blood vessels are ruptured. Endothelium is damaged and collagen under the endothelium is exposed. (Collagen is the most abundant protein in the human body, found in the bones, muscles, skin, and tendons. Its provide strength and structure.) 1. When factor XII(12) comes and contact with this collagen, it is converted into activated factor XII. (FACTOR 12+COLLAGEN=ACTIVATED FACTOR 12) 2. The activated factor XII converts factor XI(11) into activated factor XI. 3. The activated factor XI activates factor IX(9) in the presence of factor IV(4)(calcium ions) 4. The activated factor IX activates factor VIII(8) in the presence of factor IV (calcium ions) 5. Both these activated factor VIII(8) and factor IV(4) (calcium ions) activates the factor X(10). 6. Here the platelets which are release from the damaged blood vessels contact with collagen and activates and releases phospholipids. (PLATELETS+COLLAGEN=PHOSPHOLIPIDS) 7. Now the activated factor X(10) reacts with platelets phospholipids and activated factor V(5) to form prothrombin activator. This needs the presence of calcium ions (ca++). 7
- 8. EXTRINSIC PATHWAY FOR THE FORMATION OF PROTHROMBIN ACTIVATOR • In this pathway the formation of prothrombin activator initiated by the tissue thromboplastin (factor III) , which are released from damaged tissues. • Now the tissue thromboplastin converts factor X into activated factor X in the presence of factor VII(7) and factor IV (calcium ions) (ca++). • Now the activated factor X(10) reacts with activated factor V(5) to form prothrombin activator. This needs the presence of calcium ions (ca++). 8
- 9. • Blood clot is all about thrombin formation. Once thrombin is formed definitely colt is formed. • Prothrombin activator which are formed from intrinsic and extrinsic pathways converts prothrombin(factor II) into thrombin. In the presence of calcium ions (factor IV). • Once formed thrombin initiates the formation of more thrombin molecules. • The initially formed thrombin activates factor V. • This factor V in turn accelerates formation of both intrinsic and extrinsic pathways prothrombin activator, which converts prothrombin into thrombin. 9
- 10. • Thrombin converts inactivated fibrinogen (factor I) into activated fibrinogen. The activated fibrinogen is called fibrin monomer. • Fibrin monomer forms loosely arranged strands of fibrin. • Later these loose strands are modified and formed into dense and tight fibrin threads by fibrin stabilizing factor (factor XIII) in the presence calcium ions. • All the tight fibrin threads are arranged to form a meshwork of stable clot. 10
- 11. 11