Navigating Advances in Lupus Diagnosis and Treatment
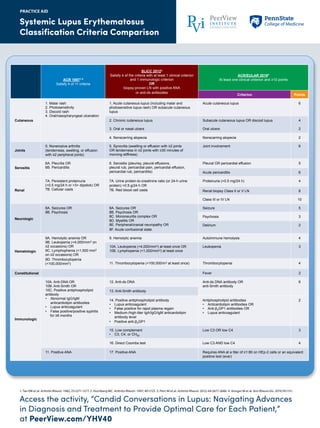
- 1. Access the activity, “Candid Conversations in Lupus: Navigating Advances in Diagnosis and Treatment to Provide Optimal Care for Each Patient,” at PeerView.com/YHV40 Systemic Lupus Erythematosus Classification Criteria Comparison PRACTICE AID 1. Tan EM et al. Arthritis Rheum. 1982; 25:1271-1277. 2. Hochberg MC. Arthritis Rheum. 1997; 40:1725. 3. Petri M et al. Arthritis Rheum. 2012; 64:2677-2686. 4. Aringer M et al. Ann Rheum Dis. 2019;78:1151. ACR 19971,2 Satisfy 4 of 11 criteria SLICC 20123 Satisfy 4 of the criteria with at least 1 clinical criterion and 1 immunologic criterion OR biopsy-proven LN with positive ANA or anti-ds antibodies ACR/EULAR 20194 At least one clinical criterion and 10 points Criterion Points Cutaneous 1. Malar rash 2. Photosensitivity 3. Discoid rash 4. Oral/nasopharyngeal ulceration 1. Acute cutaneous lupus (including malar and photosensitive lupus rash) OR subacute cutaneous lupus Acute cutaneous lupus 6 2. Chronic cutaneous lupus 3. Oral or nasal ulcers Subacute cutaneous lupus OR discoid lupus Oral ulcers 4 2 4. Nonscarring alopecia Nonscarring alopecia 2 Joints 5. Nonerosive arthritis (tenderness, swelling, or effusion with ≥2 peripheral joints) 5. Synovitis (swelling or effusion with 2 joints OR tenderness in 2 joints with 30 minutes of morning stiffness) Joint involvement 6 Serositis 6A. Pleuritis OR 6B. Pericarditis 6. Serositis (pleurisy, pleural effusions, pleural rub, pericardial pain, pericardial effusion, pericardial rub, pericarditis) Pleural OR pericardial effusion 5 Acute pericarditis 6 Renal 7A. Persistent proteinuria (>0.5 mg/24 h or >3+ dipstick) OR 7B. Cellular casts 7A. Urine protein-to-creatinine ratio (or 24-h urine protein) >0.5 g/24 h OR 7B. Red blood cell casts Proteinuria (>0.5 mg/24 h) 4 Renal biopsy Class II or V LN 8 Class III or IV LN 10 Neurologic 8A. Seizures OR 8B. Psychosis 8A. Seizures OR 8B. Psychosis OR 8C. Mononeuritis complex OR 8D. Myelitis OR 8E. Peripheral/cranial neuropathy OR 8F. Acute confusional state Seizure 5 Psychosis 3 Delirium 2 Hematologic 9A. Hemolytic anemia OR 9B. Leukopenia (<4,000/mm3 on 2 occasions) OR 9C. Lymphophenia (<1,500 mm3 on 2 occasions) OR 9D. Thrombocytopenia (<100,000/mm3 ) 9. Hemolytic anemia Autoimmune hemolysis 4 10A. Leukopenia (<4,000/mm3) at least once OR 10B. Lymphopenia (<1,000/mm3) at least once Leukopenia 3 11. Thrombocytopenia (<100,000/m3 at least once) Thrombocytopenia 4 Constitutional Fever 2 Immunologic 10A. Anti-DNA OR 10B. Anti-Smith OR 10C. Positive antiphospholipid antibody • Abnormal IgG/IgM anticardiolipin antibodies • Lupus anticoagulant • False positive/positive syphilis for 6 months 12. Anti-ds DNA Anti-ds DNA antibody OR anti-Smith antibody 6 13. Anti-Smith antibody 14. Positive antiphospholipid antibody • Lupus anticoagulant • False positive for rapid plasma regain • Medium-/high-titer IgA/IgG/IgM anticardiolipin antibody level • Positive anti- 2GP1 Antiphospholipid antibodies • Anticardiolipin antibodies OR • Anti- 2GP1 antibodies OR • Lupus anticoagulant 2 15. Low complement • C3, C4, or CH50 Low C3 OR low C4 3 16. Direct Coombs test Low C3 AND low C4 4 11. Positive ANA 17. Positive ANA Requires ANA at a titer of 1:80 on HEp-2 cells or an equivalent positive test (ever)
- 2. Access the activity, “Candid Conversations in Lupus: Navigating Advances in Diagnosis and Treatment to Provide Optimal Care for Each Patient,” at PeerView.com/YHV40 Considerations in the Treatment of Systemic Lupus Erythematosus PRACTICE AID Treatment Goals1,2 Ensure long-term survival Achieve the lowest-possible disease activity Prevent organ damage Minimize drug toxicity Improve quality of life Educate patients about their role in disease management Medicines Commonly Used to Treat Lupus3 Class Example(s) Comments Corticosteroids Prednisone, prednisolone, methylprednisolone, and hydrocortisone • Steroid dosage should be kept at lowest level possible; once lupus symptoms respond to treatment, dose is gradually reduced • Adverse effects of glucocorticoids are both dose- and duration-dependent; adverse effects range from those that are not necessarily serious but are displeasing to patients (eg, Cushingoid appearance) to those that are life-threatening (eg, serious infections); some adverse effects, such as accelerated reductions in bone mineral density or early cataracts, may be largely asymptomatic until later manifestations develop that require medical attention (eg, acute vertebral collapse, cataract requiring surgical extraction) Antimalarials Hydroxychloroquine and chloroquine • In general, all patients with SLE with any degree and type of disease activity should be treated with hydroxychloroquine or chloroquine, unless these agents are contraindicated; there is a tendency to avoid the use of chloroquine because of increased risk of retinal toxicity • Benefits of hydroxychloroquine or chloroquine in SLE are broad and include relief of constitutional symptoms, fatigue, musculoskeletal manifestations, and mucocutaneous manifestations; as an add-on to certain immunosuppressives, it is thought that antimalarials may have additive benefits in more serious disease, and they are also known to be helpful in anticoagulation • Side effects from antimalarials are rare and usually mild and include upset stomach and changes in skin color; these typically go away after body adjusts to the medication; the possibility of retinal toxicity warrants clinician adherence to dosing and screening recommendations Biologics Belimumab, rituximab • Belimumab, approved in 2011, was the first treatment approved for SLE in over 60 years • Belimumab has been demonstrated to be effective in treatment of global lupus disease activity and lupus nephritis; it has also been shown to reduce autoantibodies Immunosuppressives Cyclophosphamide, azathioprine, mycophenolate mofetil, cyclosporine, tacrolimus, leflunomide, and methotrexate • Used to control more serious lupus activity that affects major organs, including the kidney, brain, cardiovascular system, and lungs • May be given in addition to, or instead of, steroid therapy to lower the dose of steroids needed and thus spare some of the undesirable side effects of steroid therapy • Hydroxychloroquine has also been shown to be beneficial in decreasing the risk of accelerated atherosclerosis, preeclampsia, and lupus nephritis • Rituximab, a B-cell–depleting chimeric monoclonal antibody, may be useful in patients with severely low platelet counts, hemolytic anemia, and refractory nephritis
- 3. Access the activity, “Candid Conversations in Lupus: Navigating Advances in Diagnosis and Treatment to Provide Optimal Care for Each Patient,” at PeerView.com/YHV40 Considerations in the Treatment of Systemic Lupus Erythematosus PRACTICE AID a Mild: constitutional symptoms/mild arthritis/rash ≤9% BSA/PLTs 50-100 x 103 /mm3 ; SLEDAI ≤6; BILAG C or ≤1 BILAG B manifestations. b Moderate: RA-like arthritis/rash 9%-18% BSA/cutaneous vasculitis ≤18% BSA; PLTs 20-50 x 103 /mm3 /serositis; SLEDAI 7-12; ≥2 BILAG B manifestations. c Severe: major organ-threatening disease (nephritis, cerebritis, myelitis, pneumonitis, mesenteric vasculitis; thrombocytopenia with platelets <20 x 103 /mm3 ; TTP-like disease or acute hemophagocytic syndrome; SLEDAI >12; ≥1 BILAG A manifestations. 1. van Vollenhoven RF et al. Ann Rheum Dis. 2014;73:958-967. 2. Bertsias G et al. Ann Rheum Dis. 2008;67:195-205. 3. https://www.lupus.org/resources/medications-used-to-treat-lupus. 4. Fanouriakis A et al. Ann Rheum Dis. 2019;78:736-745. Treatment of Nonrenal SLE: EULAR Recommendations4 Sun protection Vaccinations Exercise No smoking Body weight Blood pressure Lipids Glucose Antiplatelet anti-coagulants (in aPL-positive patients) Remission SLEDAI = 0 HCQ No GC OR Low disease activity SLEDAI 4 HCQ Pre 7.5 mg/d Immunosuppressives (in stable doses and well tolerated) Adjunct Target HCQ GC PO/IM GC PO/IV MTX/AZA BEL CYC RTX Milda First line Refractory Moderateb First line Refractory Severec First line Refractory CNI MMF Grade A Grade B Grade C Grade D Given the clinical heterogeneity of SLE and the unpredictable disease course, the therapeutic approach is highly variable and is generally guided by the predominant disease manifestations. In general, all patients with SLE with any degree and type of disease activity should be treated with an antimalarial (eg, hydroxychloroquine); additional therapy is based upon the severity of disease and the combination of manifestations.
- 4. Access the activity, “Candid Conversations in Lupus: Navigating Advances in Diagnosis and Treatment to Provide Optimal Care for Each Patient,” at PeerView.com/YHV40 Management of Reproductive Health in SLE: 2020 Recommendations and Good Practice Statements from the ACR1 PRACTICE AID a Recommendation for IUD use includes women receiving immunosuppression therapy. 1. Sammaritano LR et al. Arthritis Care Res (Hoboken). 2020;72:461-488. Use of Contraception SLE: Moderate-high disease activity IUDsa, progestin implant, DMPA, or progestin-only pill over combined estrogen–progestin contraceptives AVOID estrogen patch SLE: Low disease activity IUDsa, progestin implant, combined estrogen and progesterone pill, progestin-only pill (less effective), vaginal ring, or DMPA IUDs or progestin implant preferred over other hormonal contraceptives AVOID estrogen patch Special Circumstances • Use of mycophenolate medications requires an IUD or combination of two other forms of contraception • Avoid DMPA in patients at risk for osteoporosis Strongly recommend Conditionally recommend Conditionally recommend against • Discuss contraception and pregnancy planning at initial or early visit with women of reproductive age and counsel regarding efficacy and safety • Recommend barrier methods if more effective methods are contraindicated • Recommend emergency (post-coital) contraception when necessary Pregnancy Counseling, Assessment, and Management • Counsel RMD patients regarding improved maternal and pregnancy outcomes when disease is quiescent/low activity before pregnancy • Comanagement with rheumatology and other specialists preferred Assess patients considering pregnancy High disease activity Treat to control disease activity and reassess when quiescent/low disease activity Low disease activity Change to pregnancy-compatible medications and observe for efficacy and tolerance Assess patients beginning early in pregnancy SLE Continue HCQ (if on) Start HCQ (if not on and no contraindication) Low-dose aspirin Laboratory assessment of disease activity at least once per trimester Strongly recommend Conditionally recommend Conditionally recommend against
