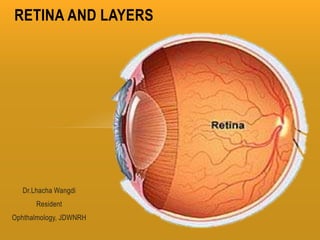
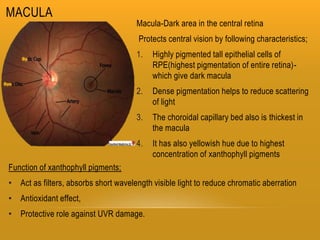
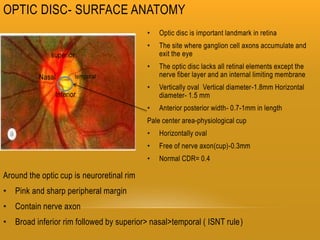
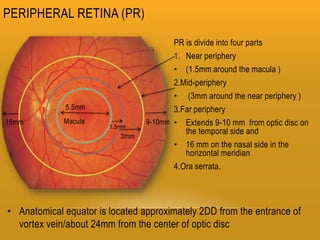
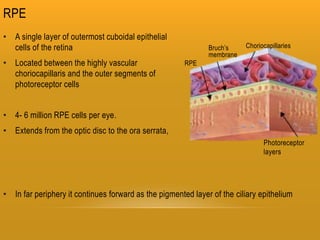
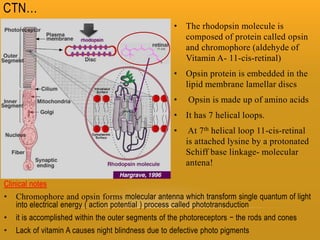
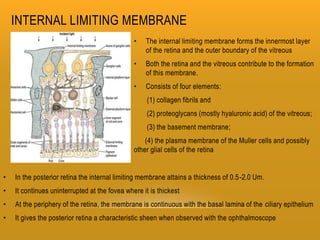
The retina has 10 layers and contains photoreceptors that convert light into neural signals. The macula contains the highest density of cones and allows for sharp central vision. The fovea within the macula contains only cones laid out single file, allowing for the highest visual acuity. Photoreceptors synapse with bipolar and horizontal cells in the outer plexiform layer. The retinal pigment epithelium supports the photoreceptors and forms the blood-retina barrier.