Effusions peritoneal fluids.pptx
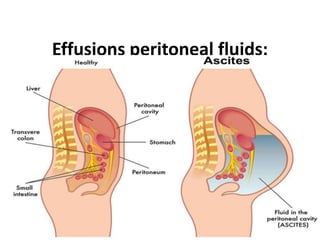
- 2. • Peritoneal effusion, or ascites, is a collection of fluid in the abdomen. This fluid collects in the lining of the lower abdomen, which is called the peritoneum. • With ascites, an abnormal amount of fluid builds up between the two layers of the peritoneum. • This fluid can put pressure on abdominal organs, potentially causing pain, swelling and other symptoms. • Based on severity, physicians classify peritoneal effusion into three categories: • Grade 1: The patient has a mild effusion, only detectable by ultrasound. • Grade 2: The patient has a moderate effusion, with equal amounts of abdominal swelling (distension) on each side of the abdomen. • Grade 3: The patient has a large effusion, with marked abdominal distension.
- 3. • Treatment may vary depending on the ascites classification and cause. Often, the cause is cirrhosis of the liver or cancer. • If cancer is the cause, it is considered malignant peritoneal effusion. • This diagnosis has related treatment options to help reduce fluid buildup and prevent it from recurring. • Peritoneal Effusion and Mesothelioma • Peritoneal effusion, or ascites, may be a symptom of peritoneal mesothelioma. Some research shows ascites in 60 – 100% of newly diagnosed peritoneal mesothelioma patients. This symptom may be one of the first things to make patients seek medical care. • Doctors may classify peritoneal mesothelioma cases based upon the presence of ascites. Patients can fall into two general classifications:
- 4. • Dry painful type: Patients have abdominal pain due to a large tumor in the abdomen. • Wet type: Patients present with ascites and increasing abdominal girth, not tumors. • Diagnostic tests may help doctors diagnose patients with ascites and, subsequently, peritoneal mesothelioma. Once a patient is diagnosed with mesothelioma, some treatments may seek to resolve peritoneal effusions. These treatments may help improve patients’ comfort and limit the recurrence of ascites.
- 5. Mesothelioma
- 6. Causes of Peritoneal Effusion • Multiple conditions may cause peritoneal effusion, including mesothelioma and other cancers. Non- malignant diseases related to abdominal organs may also cause ascites. • Peritoneal mesothelioma patients may develop ascites from fluid produced by aggressive tumors. This fluid accumulates in the abdominal cavity. If cancer cells migrate to the lymphatic system, they can block lymph drainage. This may also cause ascites.
- 7. Peritoneal Effusion Causes • Cancer, including mesothelioma • Cirrhosis (liver disease) • Dialysis • Heart failure • Pancreatic disease • Tuberculosis
- 8. Symptoms of Peritoneal Effusion • Peritoneal effusion may cause a range of symptoms, including abdominal pain and nausea. For some patients, the symptoms of ascites may be the first step towards another diagnosis. Individuals should seek medical care for stomach distention that feels full and painful. • Symptoms of Malignant Peritoneal Effusion • Abdominal pain • Dyspnea (difficulty breathing) • Fatigue • Impaired movement • Loss of appetite (anorexia) • Lower limb swelling • Nausea • Vomiting
- 9. • Common peritoneal mesothelioma symptoms may overlap with symptoms of ascites. Peritoneal mesothelioma symptoms include weight loss, a full abdomen, a general feeling of discomfort (malaise) and abdominal discomfort. Malignant peritoneal mesothelioma patients also report feeling overly full and/or nauseous. • As a patient’s underlying disease progresses, symptoms such as ascites may worsen. This may lead to increased abdominal discomfort. Talking with a healthcare provider at the onset of symptoms may help target the cause sooner. Some diseases, such as mesothelioma and other cancers, are more likely than others to lead to ascites.
- 10. Peritoneal Effusion Diagnosed: • Diagnosing ascites is an important first step in pinpointing the underlying condition. Doctors may use differential diagnosis to help rule out potential causes. • This process may include cytology testing to screen for cancer. The diagnostic process may help doctors rule out other effusion-causing cancers, such as ovarian cancer or breast cancer. • A sample of fluid collected from the pericardial sac using a procedure called a pericardiocentesis • The diagnosis of malignant peritoneal effusion may include any combination of the following: • Abdominal paracentesis (removal of fluid) followed by ascitic fluid analysis • Abdominal ultrasound • Blood tests • CT scan or other imaging tests • Fluid biopsy • Patient history • Physical examination • Tumor tissue biopsy
- 11. • If cancer has not already been diagnosed, doctors may order a tumor tissue biopsy and testing. • This allows doctors to differentiate between peritoneal effusion and malignant peritoneal effusion. • If diagnosed with mesothelioma, doctors may classify patients by cell type and stage. Depending on patients’ symptoms, doctors may use various methods for treating ascites.
- 12. Peritoneal Effusion Treated: • For patients, their mesothelioma cancer treatments may also treat peritoneal effusions. Mesothelioma doctors may also use other methods to manage peritoneal effusion. Treatment methods for peritoneal effusion include: • Catheters and other drainage ports: Catheters are tubes that can allow fluid to drain out of the peritoneum. Some, such as shunts, can be implanted and used long- term. Some catheters go through the skin, draining fluid into an external container. Other catheters drain fluid from the peritoneum into another area of the body. Other types of drainage ports may also be used, such as peritoneal ports.
- 13. • Diuretics: Doctors may prescribe medication that increases the frequency of urination. This has shown a reduction in peritoneal fluid buildup for some patients. Diuretics may be more effective against ascites caused by cirrhosis versus cancer. • Hyperthermic intraperitoneal chemotherapy (HIPEC): Doctors use a heated, localized chemotherapy to treat peritoneal mesothelioma in this method. The chemotherapy is heated to a temperature that kills cancer cells without killing healthy cells. Often HIPEC is combined with cytoreductive surgery. • Palliative HIPEC: This method uses heated chemotherapy alone, not in combination with surgery. For some patients, it has shown complete resolution of ascites and improvement in quality of life.
- 14. • Paracentesis: In this method, doctors insert a needle into the abdominal cavity to drain the fluid buildup in the peritoneum. Paracentesis is the most common treatment for malignant peritoneal effusion. It is effective at relieving symptoms of abdominal discomfort, nausea, vomiting and breathing difficulty. This method provides temporary relief for 90% of patients. Symptoms may return quickly, so this method is frequently repeated. • Diuretics and paracentesis are the most common first- line treatments. These methods can help treat and manage peritoneal effusions. • Ascites may recur, resulting in patients receiving routine rounds of drainage or other treatment. In some of these cases, palliative care options may also help ease discomfort.
- 15. Reported Improvements From At- Home Drainage Treatment: • Cognitive function • Difficulty breathing • Emotional function • Fatigue • Insomnia • Loss of appetite • Nausea and vomiting • Pain • Quality of life • When managing peritoneal effusions and underlying diseases, early detection, diagnosis and treatment matter. These factors may lead to patients having different prognostic and treatment options. Individuals experiencing symptoms of peritoneal effusion should speak to a healthcare provider for further guidance.
- 16. Physical, Chemical: • Transudate • Most ascitic fluids are transudates and are caused by either congestive heart failure or hepatic cirrhosis. Typical fluid analysis results include: • Physical characteristics—fluid generally appears clear or straw-colored • Protein—less than 3 g/dL • Albumin level—low (typically evaluated as the difference between serum albumin and peritoneal fluid albumin, termed serum-ascites albumin gradient, or SAAG; values above 1.1 g/dL are considered evidence of a transudate.) • Lactate dehydrogenase (LD) fluid/serum ratio—less than 0.6 • Glucose—equal to glucose level in the blood • Cell count—few cells are present, usually lymphocytes • Specific gravity—less than 1.015
- 17. Exudate • Physical characteristics—fluid may appear cloudy • Protein—greater than 3 g/dL • Albumin level—higher than in transudates (typically with a SAAG less than 1.1 g/dL) • Lactate dehydrogenase (LD) fluid/serum ratio— greater than 0.6 • Glucose—less than 60 mg/dL • Cell count—increased • Specific gravity—greater than 1.015
- 18. • Exudates can be caused by a variety of conditions and diseases and usually require further testing to aid in the diagnosis. Infections, trauma, various cancers, or pancreatitis may cause exudates. The following is a list of additional tests that a healthcare practitioner may order depending on the suspected cause and typical results. • Physical characteristics – the normal appearance of a peritoneal fluid sample is usually straw-colored and clear. Abnormal appearances may give clues to conditions or diseases present and may include: • Yellow with liver disease, milky from obstruction of the lymphatic system, and greenish from bile • Reddish peritoneal fluid may indicate the presence of blood, most often due to trauma. • Cloudy peritoneal fluid may indicate the presence of microbes and/or white blood cells (WBCs), pointing to an infection. It may also indicate lymph system blockage or trauma.
- 19. Chemical tests – tests that may be performed in addition to albumin may include: • Glucose—typically about the same as blood glucose levels; may be lower with infection • Amylase—increased with pancreatitis • Tumor markers—to identify type of malignancy
- 20. Microscopic :
