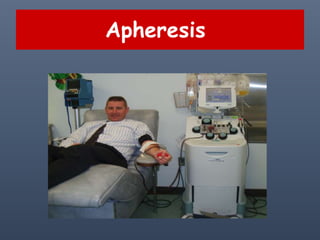
Apherisis
- 1. Apheresis
- 2. Overview • Derives from Greek, “to carry away” • A technique in which whole blood is taken and separated extracorporealy, separating the portion desired from the remaining blood. • This allows the desired portion (e.g., plasma) to be removed and the reminder returned.
- 3. Definition • Apheresis “a taking away” is a medical technology in which the blood of a donor or patient is passed through an apparatus that separates out one particular constituent and returns the remainder to the circulation.
- 5. Principle of Operation • Blood reaching equilibrium after application of centrifugal force: Plasma (1.025-1.029 specific gravity) Platelet (1.040) Mononuclear (lymph, mono, PBSC,blast) (1.070) Granulocyte (neut, baso, eos) (1.087) Neocyte RBC RBC (1.093-1.096)
- 6. Principle of Operation • Intermittent flow – Blood processed in discrete batches • complete a cycle before beginning the next one •Needs to empty before next batch • Continuous flow – All fractions can be removed in ongoing manner
- 9. Anticoagulant • Citrate • Chelates calcium and block calcium dependent clotting factor reactions – Ensures extracorporeal blood remains in fluid state – Minimize activation of platelets and clotting factors
- 10. 1. Centrifugation (specific gravity) a) Intermittent flow IFC b) Contineous flow CFc 2. Immunoadsorption Apheresis by membrane filteration 3. Photopheresis the separation of lymphocytes by apheresis, and treatment of the cells with ultraviolet radiation. Methods
- 12. Applications
- 13. Component collections - Plateletpheresis - Leucopheresis - Erythrocytapheresis - Plasmapheresis - Stem cell collection
- 15. Therapeutic Procedure -Therapeutic cytapheresis -Therapeutic plasma exchange 1) Paraproteins (Waldenstorm’s Macroglobulinem 2) Autoantibodies 3) Lipids (LDL in familial hypercholesterolemia; 4) Toxins or drugs (that are bound to albumin) 5) Circulating immune complexes (CIC)
- 16. Therapeutic Cytapheresis 1. Plateletpheresis the platelet count can be decreased by 60% of the initial value. 2. Leucopheresis : e.g leukemia 3. Lymphocytespheresis . 4. Erythrocytapheresis : e.g SCA, severe parasitemia 5. Stem cells harvesting, Donor or patient.
- 17. Therapeutic Plasmapheresis It is the removal and retention of the plasma with return of all cellular components to the patient. Recommended 1-1.5 plasma volumes be exchanged
- 18. Drug Removal • Can remove: – tobramycin,vancomycin, propranolol • May reduce plasma levels of enzymes that metabolize drugs • May reduce plasma levels of proteins that bind and transport drugs
- 19. Donation Criteria Donors for apheresis procedure must meet the criteria applicable as the donors for normal donation. CBC, ABO and Rh typing, andtibody screening and testing for transfusion transmitted diseases SHOULD BE DONE. A drug history should be obtained; donors who have taken aspirin or aspirin containing medications within 3 days of donation should be temporarily deferred.
- 20. Donation Interval The interval between platelet donations should be at least 48 hours, with no more than two donations in a week and 24 donations in a year. plasmapheresis donors may donate as often as every 48 hours but not more than twice in a 7-day period.
- 21. Total blood volume according to body mass/ml rate Newborn82-86 ml/kg Premature89-105 ml/kg Infant73-82 ml/kg 70ml/kg Adult Extracorporeal volume (ECV) and TBV ECV not more than 15% of TBV
- 22. Evidence based Guidelines For Therapeutic Apheresis By American Society for Apheresis ASFA Category I: Considered primary or standard therapy usually on basis of controlled trials Category II: Supportive or adjunctive to other therapy
- 23. Evidence based Guidelines For Therapeutic Apheresis Category III: Insufficient data to determine effectiveness; results of clinical trials may be conflicting or uncontroled anecdotal reports of efficacy Category IV: do not respond to apheresis therapy
- 24. Guidelines for Therapeutic Cytapheresis Leukemia with hyperleukocytosis syndrome Sickle cell syndrome Thrombocytosis Cutaneous T-cell lymphoma Hairy cell leukemia Hyperparasitemia (e.g., malaria) Peripheral blood stem cell collections for Hematopoitic reconstitution Category I Category II
- 25. Life-threatening hemolytic Transfusion reactions Multiple sclerosisSickle cell disease Leukemia without hyperleukocytosis syndromes Hypereosinophilia Category IVCategory III
- 26. Guidelines for Therapeutic Plasmapheresis Category I Category II Thrombotic Thrombocytopenic Purpra (TTP). Coagulation factor inhibitors Homozygous familial hypercholesterolemia Hyperviscosity syndrome Postransfusion purpura Rapidly progressive glomerulonephritis Chronic inflammatory demyelinating polyneuropathy Cold agglutinin Drug overdose and poisoning (protein-bound toxins) HUS
- 27. AIDS (for symptoms of immunodeficiency) Aplastic anemia Rheumatoid arthritis ABO-incompatible organ or marrow transplantation Maternal treatment of Maternal-fetal incompatibility (HDN) Transfusion refractorines due to Alloantibodies (RBC, platelet, HLA) Warm autoimmune hemolytic anemia Category III Category IV
- 28. Adverse Effects of Apheresis 1- Citrate toxicity 2- Vascular complications hematoma, sepsis, phlebitis, neuropathy. 3- Hypervolemia. 4- Allergic reaction. 5- Haemolysis. 6 -Air embolus.
- 29. 7- Depletion of clotting factors. 8- Circulatory and respiratory distress. 9- transfusion transmitted diseases. 10- loss of lymphocytes. 11- depletion of proteins and immunoglobulin
- 30. Fluid replacement during apheresis • When an apheresis system is used for therapy, the system is removing relatively small amounts of fluid (not more than 10.5 mL/kg body weight). • That fluid must be replaced to keep correct intravascular volume
- 31. Conclusion Donation & Therapeutic Apheresis is safe and easy effective methods to be used when needed. A well-trained and experienced team can overcome the technical difficulties in order to complete the procedures without complications. Policy and procedure of Donors Apheresis And Therapeutic Apheresis should be in place.
- 32. Thanks
