1) The document describes a simulation activity designed to improve the turnaround time for laboratory tests in an emergency department. Participants form groups to pass a tennis ball representing a lab test between steps in the testing process.
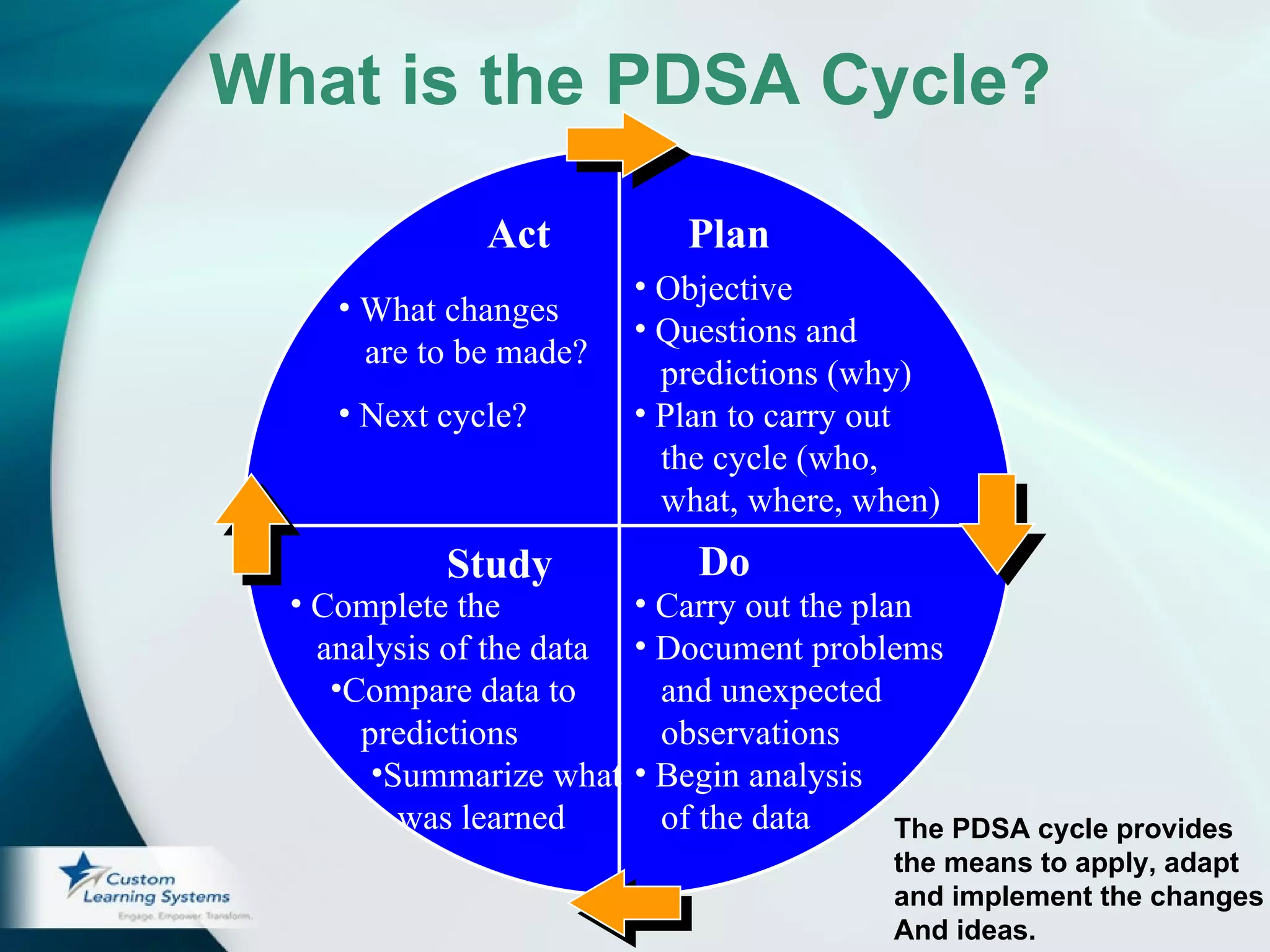
2) The goal is to cut the time in half through testing changes using Plan-Do-Study-Act cycles. Participants identify potential changes, test them on a small scale, and analyze the results to plan further improvements.
3) The document discusses using rapid PDSA cycles to test changes, collecting data to learn what works and adapt the changes to the local environment with the goal of accelerating improvement.