GI-Bleeding.ppt
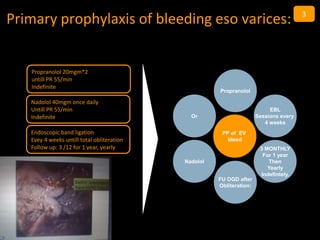
- 1. Primary prophylaxis of bleeding eso varices: Propranolol FU OGD after Obliteration: 3 MONTHLY For 1 year Then Yearly Indefintely. Or Nadolol EBL Sessions every 4 weeks PP of EV bleed Propranolol 20mgm*2 untill PR 55/min Indefinite Nadolol 40mgm once daily Untill PR 55/min Indefinite Endoscopic band ligation Evey 4 weeks untill total obliteration Follow up: 3 /12 for 1 year, yearly 3
- 2. Management of acute variceal bleeding: Endoscopic Intervention EBL Sclerotherapy Sigestaken Tube temponade Cyanoacrylate Injection Sclerotherapy For gastric Varices. Antibiotics: Ceftriaxone Ciprofloxacin 5 days Vasoconstrictor Octreotite Somatostatin Telipresin 5 days Esophageal stenting Acute variceal Bleeding. 4
- 3. Secondary prophylaxis( prevention of recurrent) of bleeding EV: propranolo Nadolol Cyanoacrylate for GV EBL for EV Interventional Radiology for GV Isosorbide Secondary prophylaxis Propranolol Same as for primary prophylaxis. Nadolol Same as for primary prophylaxis. Isosorbide dinitrate 10 mgm*10-20 mgm*2 EBL Same as for primary prophylaxis. Cyanoacrylate injection sclerotherapy or IR for gastric varices not EBL. 5
- 4. Portal Hypertensive Gastropathy •PHT- related ectatic gastric mucosal vessels mostly in fundus & body of the stomach. Definition: GEV , Child class& prior variceal endoscopic therapy Chronic blood loss leading to IDA rather than acute bleeding Iron supplementation;BB,Shunt therapy(surgeryorTIPS) Same. Predictors of its presence Prsentation Treatment: Prophylaxis 14
- 5. Acute Lower Gastrointestinal Bleeding Bleeding distal to the ligament of Treitz for <less than 3 days. The colon is the most common site of bleeding. The incidence increases with age, with mean of 63-77 years. LGIB accounts for 20% of all episodes of GIB. Most episodes of LGIB will stop without intervention. The most common causes of acute LGIB are diverticulosis, angiectasia, ischemic colitis, perianal disease. The most frequent causes of chronic LGIB are neoplasms, angiectasia, IBD.
- 6. Causes in Our locality: Perianal diseases(piles/Fissure) IBD(UC>CD) Infectious colitis Neoplasms(adenoma or cancer) Solitary rectal ulcer syndrome (SRUS) Meckel’s diverticulum. Ischemic colitis. Angiodysplasia
- 7. Hemorrhoids/ fissures: Bleeding after/or with defecation Pain & bleeding with defecation Careful perianal exam+ anoscopy assist in the diagnosis Piles Fissure 1 2
- 8. Acute LGIB: Management algorythm Initial evaluation/ resuscitation Triage to OP vs Ward vs ICU Mild scanty bleeding Anorectal pathology susspected Rigid Anoscopy or sigmoidoscopy to confirm diagnosis Outpatient management Anorectal pathology(piles/fissure) is the most common pathology in our locality But this should be diagnosed on solid basis not to miss serious pathologies as IBD or cancer.
- 9. Severe bleeding Severe exanguinating bleeding Emergency angiography for bleeding control by gel form or coils Or emergency surgical consult. If emergency angio succeeded just observe for recurrence but if fails refer to surgery SURGERY Severe exanguinating bleeding needs urgent action either emergency surgery or emegency therapeutic interventional radiology. Acute LGIB: Management algorythm
- 10. Moderate severe bleeding Consider NGT aspirate Bloody NGT aspirate Risk for UGIB OGD If +ve treat accordingly Most of the cases of LGIB fall in this category & require 1st NGT aspiration & if +ve bloody aspirate , urgent upper GIT endoscopy. Acute LGIB: Management algorythm
- 11. Moderate severe bleeding NGT not done or –ve aspirate Polyethelene glycol(PEG) solution laxative for preparation for emergency colonoscopy in few hours. Colonoscopy within 12-24 hours Manage according to colonoscopic findings If the NGT aspirate is not bloody or NGT was not inserted, urgent prep with PEG is needed for urgent colonoscopy within12-24 hours. Acute LGIB: Management algorythm
- 12. Moderate severe bleeding On colonoscopy bleeding site & cause is identified so treat as appropriate. If the colonoscopy identifies the site/cause of bleeding the problem is solved Acute LGIB: Management algorythm
- 13. Moderate severe bleeding If On colonoscopy there is visual impairment because of ongoing bleeding Angiography. If on colonoscopy there was visual impairment due to bloody field urgent angiography is indicated fordiagnosis & therapy. Acute LGIB: Management algorythm
- 14. Moderate severe bleeding On colonoscopy bleeding site not identified but bleeding had stopped OGD Or Repeat colonoscopy Or SI evaluation /Or Others( RBC scan,angiography) for rebleeding. If on colonoscopy the bleeding had stopped & no lesion was identified, upper GI endoscopy is considered(if had already been done) or RBC scan/angigraphy Is done fordiagnosis/treatment specially if bleeding recurred. Acute LGIB: Management algorythm