Madura foot ppt
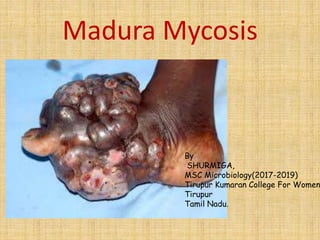
- 1. Madura Mycosis By SHURMIGA, MSC Microbiology(2017-2019) Tirupur Kumaran College For Women Tirupur Tamil Nadu.
- 2. Definition • Madura foot or mycetoma (tumour-like) • Chronic granulomatous disease characterised by localised infection of subcutaneous tissues and sometimes bone characterised by discharging sinuses filled with organisms like actinomycetes or fungi.
- 3. History • Gill first described the disease in the Madura district of India in 1842. • Hence the term Madura foot.
- 4. Pathophysiology • Typically present in agricultural workers(hands shoulders and back – from carrying contaminated vegetation and other burdens).
- 5. • Individuals who walk barefoot in dry , dusty conditions • People who work in rural areas where they are exposed to acacia trees or cactus thorns containing the etiologic agents.
- 6. • Spread occurs through skin facial planes and can involve the bone. • Two thirds arise on the foot , but can involve the hands , back or shoulders. • Following initial injury , the disease – follows a slow chronic course over many years with painless swelling and intermittent discharge of pus.
- 7. • There may be a deep itching sensation • Pain may occur due to secondary bacterial infection or bone invasion • After some years, massive swelling of the area occurs , with induration , skin rupture and sinus trace formation. As the infection spreads, old sinuses close and new ones open
- 10. Causes • Due to fungi – eumycetoma (40%) or • Actinomycetes – (actinomycetoma) 60% • Actinomycetoma may be due to Actinomadura madurae Actinomadura pelletieri Streptomyces somaliensis Nocardia species
- 11. • Eumycetoma is often due to Madurella mycetomi , Pseudallescheria boydi (Scedosporium apiospermum) , Cladophialophora
- 14. Clinical features • Slow spreading skin infection • Local swelling • Small hard painless nodules • Ulceration • Pus discharge • Scarred skin & discoloration • Itching • Pain and burning sensation
- 17. Lab studies • Direct microscopy • Blood – leukocytosis & neutrophilia • Culture of exudates • Skin biopsy • Serology • DNA sequencing has been used for identification in difficult cases.
- 18. Microscopy • Serosanguinous fluid containing the granules examined using – 10% KOH and Parker ink or calcofluor white mounts • Tissue sections stained using H&E(Hematoxylin and Eosin stain) , PAS(Periodic Acid Shiffs Stain) and Grocott’s methenamine silver(GMS). • Actinomycotic grains contains very fine filaments. • Fungal grains contain short hyphae (branched filaments) that are often swollen
- 22. Culture • Sabouraud’s dextrose agar or mycobiotic agar to isolate fungi • Blood agar to isolate bacteria • Agar plates are cultured at 25-30 degree celcius and 37 degree celcius for up to six weeks . Fungi grow more quickly than actinomycetes.
- 24. Serology • (1) Immunodiffusion tests eumycotic mycetoma infections. • (2) Counterimmunoelectrophoresis • (3) Enzyme-linked immunosorbent assay (ELISA) • (4) Western blot.
- 25. Imaging • Plain x-rays assess for evidence of bone involvement • CT scan may be more sensitive in the early stages • MRI scans better assessment of the degree of bone and soft tissue involvement; and may be useful in evaluating the differential diagnosis of the swelling .
- 26. Bone radiography • Once mycetoma has invaded the bone, the following changes may be observed: • Cortical thinning is due to compression from the outside by the mycetoma. • Multiple lytic lesions or cavities may be large and few in number with well-defined margins (eumycetoma) or small and numerous with ill defined margins(actinomycetoma). • Osteoporosis may occur in late stages.
- 28. Ultrasonography • Single or multiple thick-walled cavities with hyper reflective echoes and no acoustic enhancement • In eumycetoma, the hyper reflective echoes are sharp, corresponding to the grains in the lesion. • In actinomycetoma, the hyper effective echoes are fine and closely aggregated and commonly settle at the bottom of the cavities.
- 30. Treatment Due to the slow ,relatively pain –free progression of the disease, mycetoma is often at an advanced stage when diagnosed. • Antifungals • Antibiotics • Treatment of any secondary infections • Amputation-in severe cases
- 31. Amputation
- 32. Medical • Actinomycetomas usually respond better to medical treatment than eumycetomas • Therapy is suggested for 1-2 years (or greater) for complete eradication • The current treatment of actinomycetoma is trimethoprim-sulfamethoxazole 7.5-40mg/kg daily in 3 oral doses for several months or years.
- 33. Eumycetoma • Ketoconazole 400mg daily • Itraconazole 300mg daily • Amphotericin B 50 mg daily • Terbinafine • External beam radiotherapy in doses ranging from 3.5-14 Gy has been considered successful treatment in a few selected cases.
- 35. Surgical • Excision of the affected tissues • Localized mycetoma lesions that can be excised completely without residual disability. • Disease process more extensive than suggested by superficial lesion- so apparently healthy tissue removed to avoid recurrence • Surgical reduction of large lesions can improve the patient’s response to medical treatment.
- 36. • Scalp lesion- rapidly fatal so attended without delay • Extensive surgery may have to be followed by skin grafting/plastic surgery • To cover large open area /improve functions • Extensive bone involvement often warrents surgical amputation.
- 37. Complications • Secondary bacterial infection • Immonucompromised patients may can develop invasive infection • This can cause increased pain and disability as well as osteomyelitis, septicaemia, which my be fatal if untreated. • Lymphatic obstruction and fibrosis may cause lymph oedema • In advanced cases, deformities or ankylosis may occur • Chronic neglected infection may necessitate amputation.
- 38. • Complications may result from toxicity due to prolonged antimicrobial of antifungal therapy. • Actinomycetoma can be cured with the appropriate antibiotic therapy but eumycetoma has a high rate of recurrence and can require amputation.
- 39. Epidemology • Endemic in the tropics and subtropics • More common in men than in women • The male-to-female ratio is 3:1 • Particularly those aged 20 to 50
- 40. Madura foot
