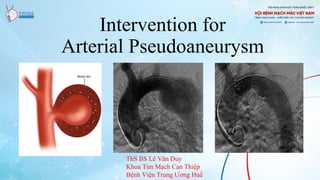
Intervention for Arterial Pseudoaneurysm
- 1. Intervention for Arterial Pseudoaneurysm ThS BS Lê Văn Duy Khoa Tim Mạch Can Thiệp Bệnh Viện Trung Ương Huế
- 2. Overview • The increase in the number of surgical and arteriographic procedures has caused a higher prevalence of pseudoaneurysms. • Conventional angiography is still the gold standard method for diagnosis, but other imaging modalities such as duplex Doppler ultrasonography, magnetic resonance angiography and computed tomographic angiography are useful in noninvasive detection. • Over the past few years, interventional radiological treatment has evolved and taken the place of surgery in management.
- 3. in this presentation, we will use 6 special case to discuss pseudoaneurysms and their appropriate treatment by interventional radiological methods. What for: 1. Understanding more cause, some apropriate strategies and suitable devices. 2. Sharing our experiences to deal some difficle cases at Hue Central Hospital.
- 4. • Pseudoaneurysms are common vascular abnormalities that occur from a defect in the arterial wall. • Blood leaks through the disrupted wall into the surrounding tissue, which leads to a persistent communication between the originating artery and the nearly cavity. • Pseudoaneurysms have a variety of causes, such as inflammation, trauma, and various iatrogenic causes such as surgery, percutaneous biopsy, drainage, and postcatheterization • Pseudoaneurysms may occur in any damaged vessel including the carotid, extremity and visceral arteries
- 5. Epidemiology • The reported incidence of postcatheterization pseudoaneurysms ranged from 0.05% to 2% • The increasing use of large-sized catheters and periprocedural anticoagulation and antiplatelet therapy has caused higher incidence of pseudoaneurysms
- 6. Ultrasonography • US is a useful, easy, cost-effective method and mostly the first choice in diagnosis of femoral artery pseudoaneurysms. • A prospective study proved high sensitivity (94%) and specificity (97%) for the diagnosis of peripheral pseudoaneurysms by using duplex.
- 8. CT Scaner • Contrast-enhanced helical CT angiography has been reported as a convenient imaging modality in the detection of neck, chest, abdomen, pelvis and extremity pseudoaneurysms • Hemorrhage may be detected with intermediate or high attenuation adjacent to the pseudoaneurysm. Thrombosis can also be seen as high attenuation within the sac in unenhanced CT scans • High attenuation adjacent to the pseudoaneurysm reveals the most serious complication, rupture
- 9. Conventional angiography • Conventional angiography continues to be the standard method for the diagnosis of pseudoaneurysm • conventional angiography provides endovascular treatment options including embolization and stent-graft placement. • Deciding on the appropriate treatment option for a pseudoaneurysm is an important issue. Angiography helps to solve this problem. • Donor artery, the neck of the pseudoaneurysm, vascular supply, and collateral vascular structures can be evaluated with angiography. Sacrification of the donor artery and the treatment choice depend on these conditions
- 10. Treatment • As a general consensus, symptomatic pseudoaneurysms should be treated. • On the other hand, it is a controversial issue that asymptomatic pseudoaneurysms should be treated or followed up. • Depending on size and location, it is reported in the literature that some pseudoaneurysms may undergo non-surgical treatment: ultrasound guided compression (USGC), thrombin therapy, arterial embolisation, endovascular stent graft insertion
- 11. Surgical treatment • Disadvantages: long hospitalization time, requirement of general anesthesia and bad wound healing in patients with comorbidities. • Surgery has higher morbidity and mortality rates compared to interventional radiological treatment options. • Complications: bleeding, infection, myocardial infarction, and death…
- 12. • With technological development, interventional radiological treatment methods have taken the first place in the treatment of pseudoaneurysms. • Nevertheless, surgery is still the gold standard treatment method in infected pseudoaneurysms, rapid growth, ischemia, neuropathy, and failure of percutaneous or endovascular treatment
- 15. Percutaneous thrombin injection • Thrombin, which is the active form of prothrombin,converts inactive fibrinogen into fibrin. • Fibrindirectly takes part in the formation of a thrombus.
- 16. Endovascular approach • Endovascular management helps to eliminate the pseudoaneurysms from the circulation. • There are two main methods in general practice: embolization and stent placement • Placement of covered stents should be performed in large-diameter and relatively smooth vessels due to the need of stiffer and larger systems
- 17. Vascular access and Closure
- 18. Case 1 • Bệnh nhân nam 40 tuổi, có tiền sử tăng huyết áp vào viện vì đau ngực • CT scanner: túi giả phình động mạch chủ lớn sau động dưới đòn trái • Được chỉ định can thiệp đặt stentgraft động mạch chủ sau khi phẫu thuật mở rộng vùng landingzone
- 19. Case 1
- 22. Case 2 • Bệnh nhân nữ 28 tuổi đang điều trị lao màng phổi và cột sống. Phát hiện đau nhiều vùng thượng vị xuyên ra sau lưng • CT Scaner: phát hiện túi giả phình lớn ở đoạn trên động mạch chủ bụng, trên thân tạng; dọa vỡ/vỡ • Sử dụng miếng phụ stentgraft ĐMC ngực phủ kín hoàn toàn túi phình, phía trên ĐM thân tạng
- 23. Case 2
- 25. Case 3 • Bệnh nhân nam 30 tuổi, vào viện vì vết thương thấu bụng do dao đâm. Được phẫu thuật cầm máu, xúc rửa ổ bụng. • CT Scaner: ghi nhận túi giả phình lớn ở động mạch thận trái • Chỉ định: đặt Coverstent (BeGraft)
- 26. Case 3
- 29. Case 4 • Bệnh nhân nam 35 tuổi, vào viện vì chấn thương gia tốc vùng ngực. Sau đó được dẫn lưu tràn khí màng phổi. • CT Scaner: phát hiện túi giả phình ĐM dưới đòn phải, ĐM đốt sống bên trái ưu thế • Chỉ định: đăt stent Coverstent nong bằng bóng (BeGraft)
- 30. Case 4
- 32. Case 5 • Bệnh nhân nam 50 tuổi, u đầu tụy, đã phẫu thuật bóc U • CT Scaner hậu phẫu kiểm tra: phát hiện túi giả phình lớn ở động mạch mạc treo tràng trên, doa vỡ/ vỡ • Chỉ định: đặt coverstent tự bung
- 33. Case 5
- 36. Case 6 • Bệnh nhân nam 50 tuổi đang điều trị áp xe vùng thắt lưng đùi đã phẫu thuật • CT Scaner: túi giả phình ĐM chậu chung phải • Chỉ định: đặt Coverstent nong bằng bóng
- 37. Case 6
- 39. Conclusion 1. The increase in the number of surgical and arteriographic procedures has caused higher prevalence of pseudoaneurysms recently. 2. Diagnosis and optimal management are crucial due to the fact that pseudoaneurysms have life-threatening complications if not treated. 3. Radiology offers alternative minimally invasive techniques that are associated with lower morbidity and mortality rates and have taken the place of surgery in the treatment