cerebral aneurysm mohammad abu sad (1).pptx
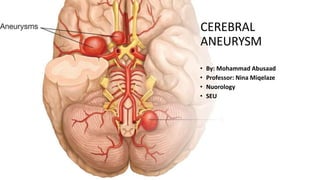
- 1. CEREBRAL ANEURYSM • By: Mohammad Abusaad • Professor: Nina Miqelaze • Nuorology • SEU
- 4. Cerebral Arteries A1-segment Anterior cerebral artery from carotid bifurcation to anterior communicating artery gives rise to the medial lenticulostriate arteries. A2-segment Part of anterior cerebral artery distal to the anterior communicating artery. P1-segment Part of the posterior cerebral artery proximal to the posterior communicating artery. The posterior communicating artery is between the carotid bifurcation and the posterior cerebral artery) P2-segment Part of the posterior cerebral artery distal to the posterior communicating artery
- 5. Middle Cerebral Artery • Horizontal M1-segment • gives rise to the lateral lenticulostriate arteries which supply part of head and body of caudate, globus pallidus, putamen and the posterior limb of the internal capsule. • Notice that the medial lenticulostriate arteries arise from the A1-segment of the anterior cerebral artery. • Sylvian M2-segment • Branches supply the temporal lobe and insular cortex (sensory language area of Wernicke), parietal lobe (sensory cortical areas) and inferolateral frontal lobe • Cortical M3-segment • Branches supply the lateral cerebral cortex
- 6. Aneurysms • They result from focal degeneration of the arterial wall. They are the most common cause of SAH. They are of 3 types : • Saccular (outpouching from arterial bifurcation) - Lacks internal elastic lamina • Fusiform (arterial dilatation) • Dissecting (pseudo-aneurysm)
- 7. SACCULAR ANEURYSM Berry like vesel outpouching arising from the bifurcation of the arteries. 80% of Intracranial aneurysms 85% - anterior circulations 15%- Posterior circulations.
- 8. FUSIFORM ANEURYSM • No definitive neck. • Long course of circumferential thickness. • Dolichoectasia . • Vertebrobasilar systemcommonly affected.
- 9. DISSECTING ANEURYSM • May be intracranial or extra-cranial. • Intracranial vertebralor posterior inferior cerebellar arteries – SAH • Extra-cranial carotid and vertebral arteries – Stroke (in young)
- 10. Presentation
- 11. INCIDENCE • General population is 0.5-5 % • Women >> Men • Increases with advancing age. • Genetic Predisposition. • Overall risk of rupture = 0.5-2 % per annum,
- 12. Risk Factor of Rupture • Daughtersac • Multi-lobulations • Irregular surface • Bottle-neck shape • Interval growth • Increase ratio of maximum • aneurysm diameter to parent vessel diameter.
- 13. Location • Most cerebral aneurysms arise from the circle of Willis and middle cerebral artery bifurcations. • Ninety percent involve the anterior circulation, and 10% the posterior circulation.
- 15. Giant Aneurysm Partially Thrombosed Giant aneurysm Leaking Giant aneurysm
- 16. Multiple aneurysm Multiple aneurysms are found in 15% to 30% of patients, Women: Men= 5:1 ratio, Most frequently involve the middle cerebral artery. Of the patients with multiple cerebral aneurysms, 75% have two, • 15% have three 10% have four or more.
- 18. • Bilateral symmetrical aneurysms are called Mirror Aneurysms, and • most often involve the ICA or the MCA bifurcations. • When one of multiple aneurysms ruptures and causes subarachnoid hemorrhage, it is most often the largest, although this is not always the case. • For instance, Nehls and colleagues have reported the propensity for anterior communicating aneurysms to rupture when several are present simultaneously.
- 19. Etiology Primary Causes Atherosclerosis • Hypertension • Smoking Abuse of cocaine, methamphetamine, ephedrine, heroin, and other drugs that produce arteritis or hypertension Vascular malformations - fibromuscular dysplasia, spontaneous cervical carotid or vertebral artery dissection, Takayasu's arteritis, neurofibromatosis I Connective tissue disorders, such as Marfan's syndrome and Ehlers- Danlos syndrome
- 20. Secondary Causes • Penetratingand nonpenetratingtrauma • Dissection (posttraumatic or otherwise) • Inflammation or mycosis due to septic • Neoplasm • infundibulumrepresents the residua of a developmental vessel that has undergone incomplete regression. • It most commonly involves the junction of the internal carotid artery and posterior communicating artery and less commonly involves the origin of the anterior choroidal artery from the internal carotidartery. • Infundibula are usually 3 mm or less in diameter.
- 21. Pathology • Pathologically, a number of patients with cerebral aneurysms demonstrate collagen type III abnormalities. • The walls of saccular cerebral aneurysms contain intima and adventitia, but the media and internal elastic membrane are thinned or absent. • Neoplasm: Pitutary adenoma – Growth hormone • Mycotic- spread of infection to vasa vasorum.
- 22. Features Need To Be Assessed • size: ideally 3 axis maximum size measurements • neck: maximal width of the neck of an aneurysm • the shape and lobulation • orientation: the direction in which the aneurysm points is often important in both endovascular and surgical planning
- 23. Cont…. • any smaller branches in the vicinity of an aneurysm • any branch taking off from the aneurysm • the presence of other aneurysms • relevant arterial variant anatomy (that may complicate or exclude endovasculartreatment
- 25. Imaging modalities • Computed tomography and CTA • MRI and MRA • DSA • Transcranial ultrasound • Earlier • Lumbar Puncture
- 26. Lumbar Puncture • Before CT, it was the only method to confirm the diagnosis of SAH but presently it is only indicated when CT is normal in patients with sudden, severe headache. • CSF is bloody not clearing with sequential tubes, Xanthrochromia is present after 1-2 days of SAH.
- 27. Computed Tomography • Acute SubarachnoidHemorrhage • The most important role for CT in the patient with a cerebral aneurysm is in the identification of ASAH, • Increased density within a cisternal space .
- 28. Cerebral Aneurysm • CT examination is secondarily important to identify cerebral aneurysms, typically 5 mm or larger in diameter. • The rate of identification of cerebral aneurysms - at least 67% for aneurysms 3 to 5 mm in diameter and to approach 100% for larger aneurysms. Giant aneurysms are most commonly identified in middle-age women; are typically located in the extradural carotid artery, the middle cerebral artery bifurcation, or the basilar summit; and usually manifest with mass effect
- 29. Cerebral Aneurysm • MRI is superior to CT for • the localization of cerebral aneurysms, • their relationship with adjacent structures, and • associated changes in neighboring brain tissue.
- 30. Management of intracranial aneurysms • The goal of preoperative management is • to stablize the patient for aneurysm obliteration and • prevent the development of systemic complications or secondary cerebral insults such as hypotension or hypoxia. • Ideally successful management of acutely ruptured aneurysm begins with adequate ventilation and oxygenation, normovolemia, hemodynamic stability, normoglycemia and ICP control.
- 31. • After initial stabilisation , a thorough radiographic evaluation is undertaken. • Surgical Methods: • Current surgical options include direct aneurysmal clippingand endovascular exclusion -- Surgical Clipping or Coil Embolization for the specific indications for treating an aneurysm surgically, endovascularly, or both).
- 32. Endovascular methods • GDC COILS - Of the various endovascular options currently available, Guglielmi detachable coils (GDCs) have had the largest influence with respect to treatment of subarachnoid hemorrhage; GDCs are first-line therapy nowdays. • These coils are soft, flexible, and can be contoured to the configuration of the aneurysm. • Sizes range from 2 to 20 mm in diameter and 2 to 30 cm in length. • Balloon embolization is efficacious in selected patients, but it has a higher incidence of complications than coil embolization.
- 33. Indications for endovascular treatment Posterior circulation aneurysms, especially basilar apex. Patients with poor clinical grade (ie, Hunt and Hess grades 4-5). Patients who are medically unstable. Symptomatic cavernous aneurysms. Small-neck aneurysms in the posterior fossa. Patients with vasospasm. Cases in which the aneurysm lacks a defined surgical neck (although these are also difficult to "coil") Patients with multiple aneurysms in different arterial territories if the surgical risk is high
- 34. Endovascular Procedure:Coiling • Step 1: Patient Preparation • Step 2: Insert the catheter
- 35. • Step 3: Locate the aneurysm
- 36. • Step 4:Insert the coil
- 37. • Stent placed in case of larger neck for the stabilization of the coil.
- 38. • Step 5: Check the coils • Step : Remove the catether
- 39. Evaluation after open /endovascular surgery MRI – MRI compatible clips Fatal cerebral hemorrhage if incompatible CTA superior to MRI DSA Catheter Angiography superior
- 40. THANK YOU