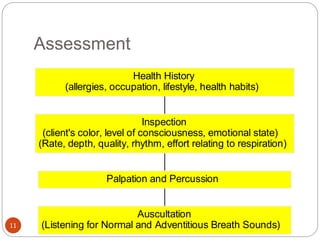
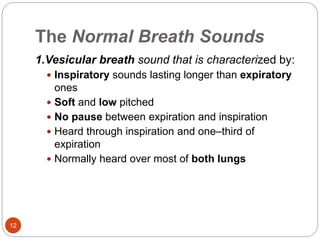
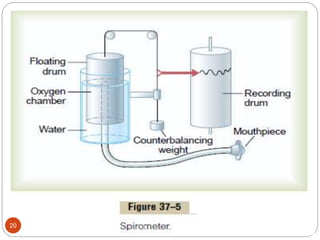
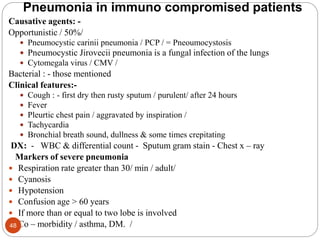
This document provides information on disorders of the respiratory system. It begins by describing the anatomy and functions of the respiratory system, including the conducting airways. It then discusses various upper and lower respiratory tract disorders like tonsillitis, pharyngitis, laryngitis, sinusitis, acute tracheo-bronchitis, and chronic bronchitis. For each disorder, it provides information on definition, causes, signs and symptoms, management, and nursing interventions. The document concludes with describing assessment techniques for respiratory disorders.