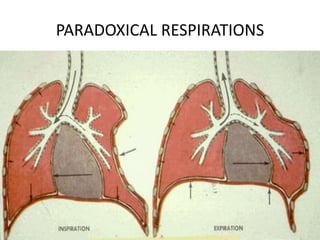
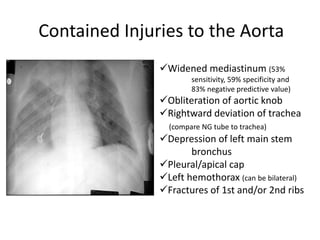
This document discusses various types of chest trauma, including penetrating and blunt injuries. It covers mechanisms of injury, specific injuries like rib fractures, pneumothorax, hemothorax, flail chest, and cardiac injuries. Management of life-threatening injuries like tension pneumothorax, pericardial tamponade, and tracheal disruptions are outlined. Imaging findings and treatments for many chest trauma injuries are also presented.