This document discusses factors that influence the stability of complete dentures. It defines stability as the quality of a removable prosthesis to resist displacement from functional stresses. The three main factors discussed are:
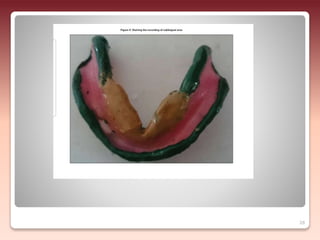
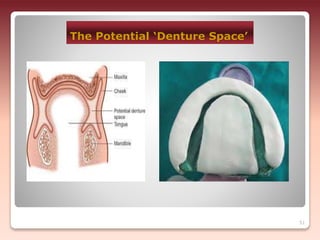
1) The relationship of the denture base to underlying tissues - Proper adaptation of the denture base to the residual ridges and surrounding tissues improves stability.
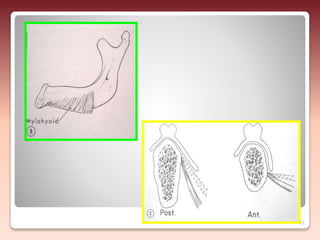
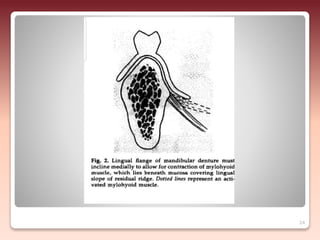
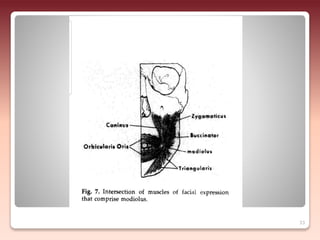
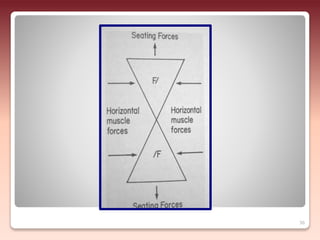
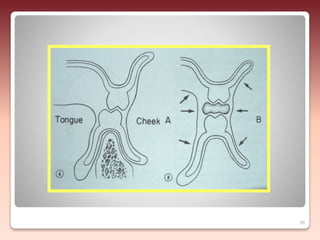
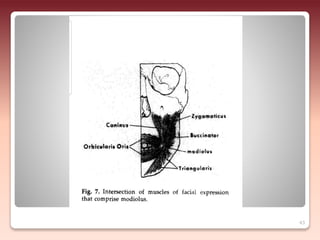
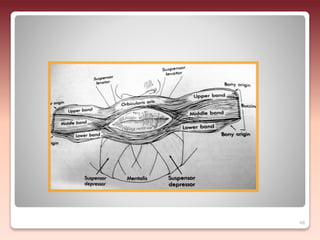
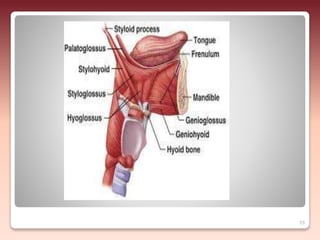
2) The relationship of the denture borders to surrounding muscles - Contouring the denture to allow free function of muscles like the buccinator and allowing muscles to help seat the denture enhances stability.
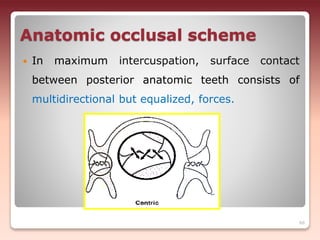
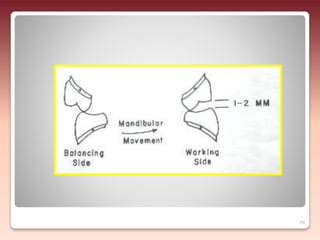
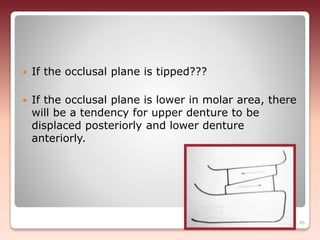
3) The relationship of opposing occlusal surfaces - Proper occlusal harmony contributes to resisting forces that could displace the dentures.