More Related Content Similar to RIGHT HEART CATHETERISTION 1.ppt Similar to RIGHT HEART CATHETERISTION 1.ppt (20) More from PDT DM CARDIOLOGY More from PDT DM CARDIOLOGY (20) 1. Copyright © 2011 American Heart Association.
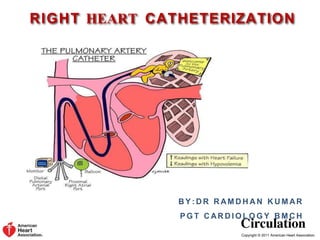
RIGHT HEART CATHETERIZATION
B Y : D R R AM D H A N K U M AR
P G T C AR D I O L O G Y B M C H
12. Copyright © 2011 American Heart Association.
Equipment
Pulmonary Artery (Swan-Ganz) Catheter
These are 7F to 7.5F system catheters and are available as
femoral vein insertion to continuous cardiac output
catheters.
18. Copyright © 2011 American Heart Association.
Technique- Micropuncture
Insertion site: Internal jugular vein, subclavian vein, antecubital vein, or
femoral vein
Vein entered using a needle (preferably micropuncture) and preferably under
ultrasound guidance (especially for internal jugular vein)
After ensuring that the needle is indeed in a vein (dark, non-pulsatile flow or
checking pressure or oxygen saturation), the guidewire is introduced into the
micropuncture needle and the needle exchanged for a micropuncture sheath
If there is difficulty in wiring and the micropuncture wire needs to be
removed, remove both the needle and the wire as a unit
Attempting to remove just the guidewire can result in the guidewire tip
shearing off the needle tip with subsequent guidewire embolization
Exchange the micropuncture catheter for the introducer sheath
19. Copyright © 2011 American Heart Association.
Technique
Preparing the catheter
Flush the proximal and distal ports with saline to ensure an
air free system and place stopcocks on the ends.
Fill the balloon inflation syringe with 1.5 cc of air and inflate
the balloon under saline to ensure no air leaks in the balloon.
20. Copyright © 2011 American Heart Association.
Inserting the catheter
The pulmonary artery (PA) catheter can be inserted either
under fluoroscopic guidance (preferred) or under the
guidance of the pressure wave forms.
Fluoroscopic guidance is recommended in patients with
markedly enlarged RA or RV, severe tricuspid
regurgitation, or in those with left bundle branch block.
A PA catheter with the balloon inflated is designed to be
flow-directed and will follow the direction of blood flow (right
atrium to pulmonary arteries).
21. Copyright © 2011 American Heart Association.
The catheter should be advanced to the
vena cava/RA junction, the approximate
distance (as measured on the PA catheter)
from the site insertion is below.
The catheter should be advanced to
the vena cava/RA junction, the
approximate distance (as measured
on the PA catheter) from the site
insertion is below.
The catheter should be advanced to the vena cava/RA junction,
the approximate distance (as measured on the PA catheter)
from the site insertion is below.
22. Copyright © 2011 American Heart Association.
Technique
Inserting the catheter
Once a PCWP tracing is seen, deflate the balloon.
The catheter should be withdrawn 1-2 cm to remove any
redundant length or loop in the RA or RV. Keep the tip in a
position where full or near full inflation volume is necessary
to produce a wedge tracing.
The balloon should be deflated and the pressure wave form
seen should now be that of the PA. If still the PCWP, it is
likely that the catheter is distal and should be retracted until
a PA pressure tracing is seen.
23. Copyright © 2011 American Heart Association.
Technique
The ideal position of the catheter is the zone 3 region of the
lung (lower zone).
For subsequent wedge tracings, the balloon should be inflated
with the minimum amount of air to produce a wedge tracing.
Excess can cause “overwedging” where the PCWP will be
higher due to transmittal of pressure from the balloon and
with loss of characteristic waveforms.
Removing the catheter
The catheter should always be removed with the balloon
deflated to avoid damaging the valves.
25. Copyright © 2011 American Heart Association.
Technique
Precaution
Always advance the catheter with the balloon inflated (catheter is flow-directed,
also reduces ventricular irritability and ectopy).
Never leave the catheter wedged in the PA for longer than necessary, to avoid the
risk of pulmonary artery rupture/pulmonary infarction.
Do not overinflate the balloon.
If wedge is obtained at volumes <1.0cc, pull the catheter back to a position where
full or near-full inflation volume (1.0 to 1.5cc) produces a wedge tracing.
Before balloon reinflation, always check the waveform to ensure no distal
migration.
Never withdraw the catheter with the balloon inflated to avoid valvular damage.
26. Copyright © 2011 American Heart Association.
Technique
Precaution
Never use fluids (saline) to inflate the balloon.
In situations where multiple attempts at advancing the catheter to the PA
fail, a 0.025” guidewire can be used under fluoroscopic guidance to help
advance the catheter to the PA.
Always maintain catheter tip in a main branch of the PA.
If performed via the internal jugular or the subclavian vein route and
without fluoroscopic guidance, chest x-ray should be obtained post
procedure to rule out pneumothorax and to verify catheter position.
Never flush catheter with balloon wedged in the PA.
28. 0 100 200 300 400 500 600 700 800
0
1
5
30
Atrial
Systole
Ventricular Systole Ventricular Diastole
EKG
Time (msec)
Pressure
(mm Hg)
P
QRS
Complex
T
P
PA Pressure
Dicrotic
Notch
Right Ventricular
Pressure
a
c
v
x
y
Right Atrial
Pressure
Cardiac
Cycle
Right Sided
Pressures
29. Copyright © 2011 American Heart Association.
Pressure Recordings
Always record pressure at end expiration (except in
patients on PEEP).
Under normal conditions, pressures will be lower in
inspiration due to decrease in intrathoracic pressure.
30. Copyright © 2011 American Heart Association.
Before any pressure measurements are taken, it is imperative
to perform zeroing and referencing of the system.
Zeroing- accomplished by opening the system to air so as
to equilibrate with atmospheric pressure.
Referencing- accomplished by ensuring that the air-fluid
interface of the transducer is at the level of the patient
heart (phlebostatic axis) (4th intercostal space midway
between anterior and posterior chest wall)
For every inch the heart is offset from the reference
point of the transducer, a 2mm Hg of error will be
introduced. If the heart is lower than the transducer,
the pressure will be erroneously low and if the heart is
higher, the pressure will be erroneously high.
32. Copyright © 2011 American Heart Association.
Pressure Recordings
Performed by briefly opening and closing
the valve in the continuous flush device.
This produces a square wave pattern on the
oscilloscope, an initial steep rise followed by
a plateau, followed by steep fall below
baseline which is then followed by
oscillations. The pattern determines optimal
versus suboptimal damping
Optimal Damping
Fast flush test / Square wave testing
33. Copyright © 2011 American Heart Association.
Optimal damping- usually 1.5 to 2
oscillations before returning to baseline.
This is ideal.
Over damping- None to <1.5 oscillations
before retuning to baseline. Common cause
- air bubbles. Underestimation of systolic
pressure. Diastolic pressure may not be
affected.
Under damping- >2 oscillations before
returning to baseline. Common cause -
excessive tube length, multiple stopcocks in
the circuit, etc. Overestimated systolic
pressure and underestimated diastolic
pressure
Optimal Damping
Over Damping
Under Damping
34. Copyright © 2011 American Heart Association.
Pressure Recordings
PCWP reflects left atrial pressure and hence the left ventricular end diastolic
pressure as long as ventricular compliance is normal or unchanging.
PCWP > LVEDP: Mitral valve stenosis or regurgitation, left atrial
myxoma, pulmonary vascular disease/embolism, increased pulmonary
vascular resistance, cor pulmonale.
PCWP < LVEDP: Early stages of diastolic dysfunction, aortic
regurgitation, decreased ventricular compliance due to myocardial
ischemia/infarction, positive pressure ventilation, etc.
Site Normal Values
(mm Hg)
Mean Pressure
(mm Hg)
Right Atrium 0-8 4
Right Ventricle 15-25/0-8 5-12
Pulmonary Artery 15-25/8-12 10-20
PCWP 9-23/1-12 6-12
37. Copyright © 2011 American Heart Association.
Pressure Wave Interpretations
Wave pattern Mechanism Condition
Cannon ‘a’ wave AV dissociation Complete heart block, ventricular
tachycardia, AVNRT
Tall ‘a’ wave Increased atrial pressure Mitral or tricuspid stenosis
No ‘a’ wave Loss of atrial kick Atrial fibrillation
Tall ‘v’ wave Increased volume during
ventricular systole
Mitral or tricuspid insufficiency,
VSD
Loss of ‘y’ descent Equalization of diastolic
pressures
Cardiac tamponade
Exaggerated ‘y’
descent
Rapid diastolic filling Constrictive pericarditis
RA/ PCWP
AVNRT = Atrioventricular Nodal Reentry Tachycardia; VSD = Ventricular Septal Defect
Editor's Notes kjcskcjakcakckl