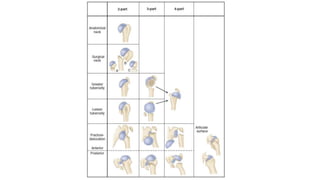
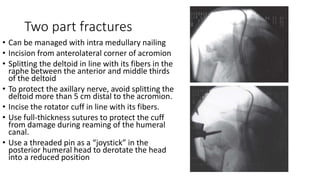
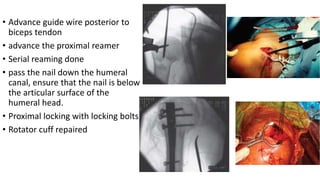
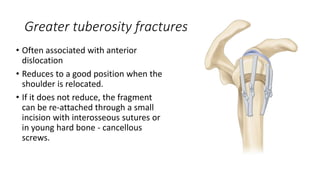
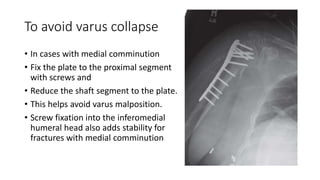
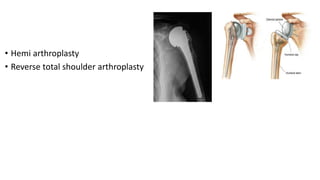
Proximal humerus fractures are common injuries, especially in older patients due to osteoporosis. They can be classified based on the number of bone fragments and degree of displacement. While undisplaced or minimally displaced fractures can often be treated non-operatively with immobilization, more displaced fractures usually require surgery such as open reduction and internal fixation with a locking plate or intramedullary nailing. The goal of both non-operative and operative treatment is to restore the anatomy and allow early range of motion exercises to prevent stiffness.