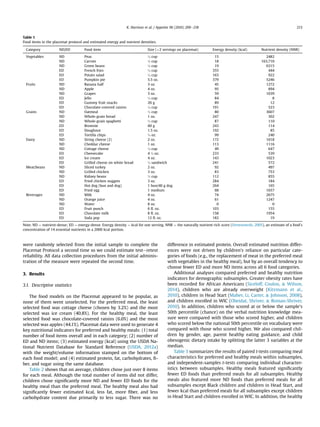
The Placemat Protocol is a novel measure designed to assess preschoolers' developing schemas of healthy meals. It involves children creating two pretend meals using highly realistic toy food models - a preferred meal and a healthy meal. The researcher can then analyze various dimensions of the meals created, such as nutritional content. The study aimed to validate this measure by comparing the nutritional profiles of the preferred vs. healthy meals and examining correlations with other measures of nutrition knowledge and dietary behaviors. Results showed children's healthy meals contained fewer calories, less fat and sugar, and more fiber than their preferred meals, supporting the validity of the Placemat Protocol as a developmentally appropriate way to measure preschoolers' understanding of healthy eating.