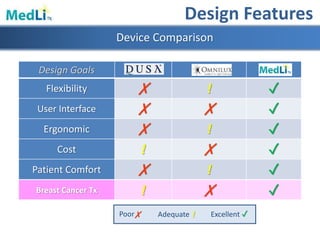
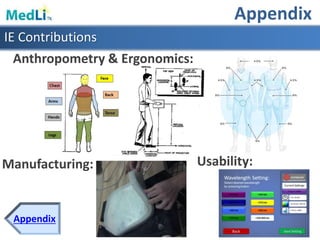
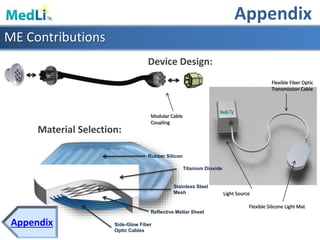
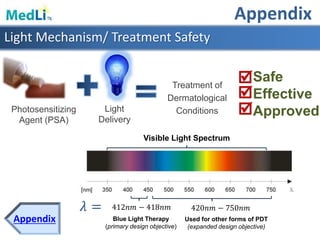
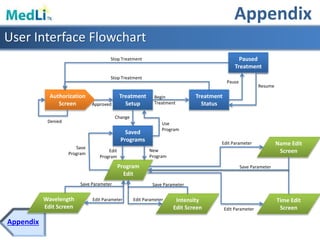
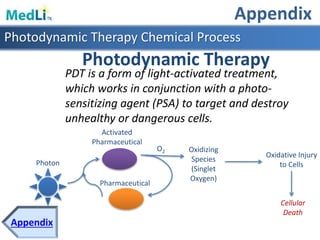
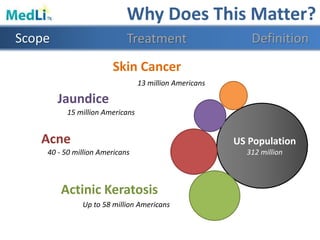
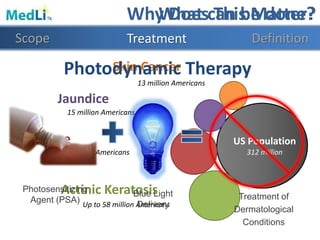
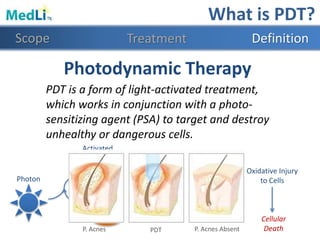
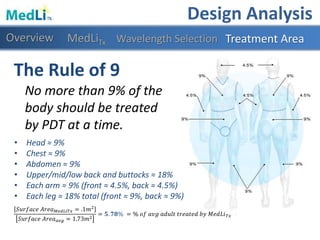
This document provides information about a proposed photodynamic therapy (PDT) device called MedLiTx. PDT uses a photosensitizing agent and light to target and destroy unhealthy cells. The document outlines the scope of dermatological conditions treated by PDT and existing challenges. It then describes the design goals and criteria for MedLiTx, which include flexibility, low cost, ease of use, and patient comfort. Details provided include the device design, wavelength selection, treatment areas, and user interface. Comparisons show MedLiTx meets design goals better than existing devices. Appendices provide additional technical details.















![𝑹𝑾𝑳 = 𝐿𝐶 × 𝐻𝑀 × 𝑉𝑀 × 𝐷𝑀 × 𝐴𝑀 × 𝐹𝑀 × 𝐶𝑀
= 10 × 7.2 × 1.11 × .87 × .55 × .95 × 1 =
Height ≈ 72 in
Load Constant ≈ 10Lb
Coupling Multiplier= 1
Vertical Location ≈ 36 in
Asymmetry Angle ≈ 140°
Horizontal Multiplier=7.2
Frequency Multiplier=.95
Vertical Travel Distance ≈ 36 in
Distance Multiplier=.82+(1.8/36)=.87
Asymmetry Multiplier=1-.0032*140=.552
Vertical Multiplier= 1-(.003*[36-75])=1.117
NIOSH Lifting Limit Formula
Based on the design specifications the Recommended Weight Limit is:
𝟑𝟔. 𝟔𝟗 𝑳𝒃=
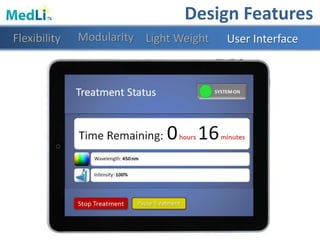
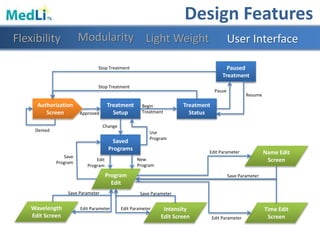
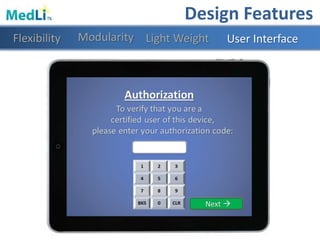
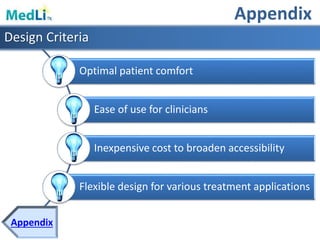
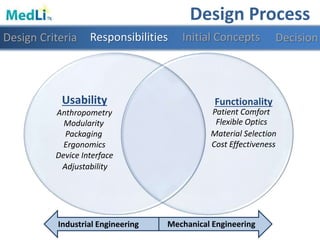
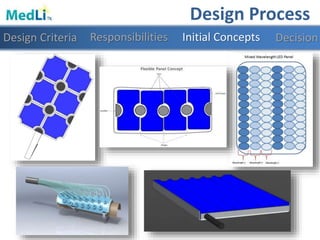
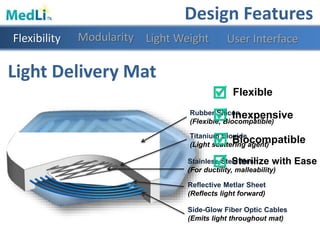
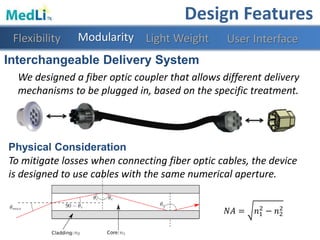
Design Features
Modularity Light WeightFlexibility User Interface](https://image.slidesharecdn.com/b9025cf4-86ba-48fd-b8d3-b372c4e5e705-151103160459-lva1-app6891/85/PDT-Final-Presentation-27-320.jpg)