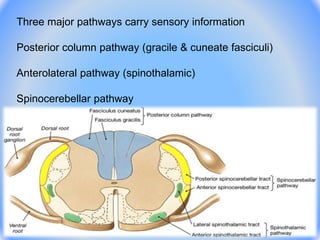
This document summarizes the pain pathway in the human body. It begins with an introduction to pain and its characteristics. It then discusses the different types of pain sensations conducted by different nerve fibers. It explains Gate Control Theory and the differences between somatic and visceral sensory function. It provides details on pain receptors, the pathway of sensory impulses from receptors to the brain, and examples of tooth pulp pain and referred pain. It concludes with management strategies for pain.