Embed presentation
Downloaded 145 times































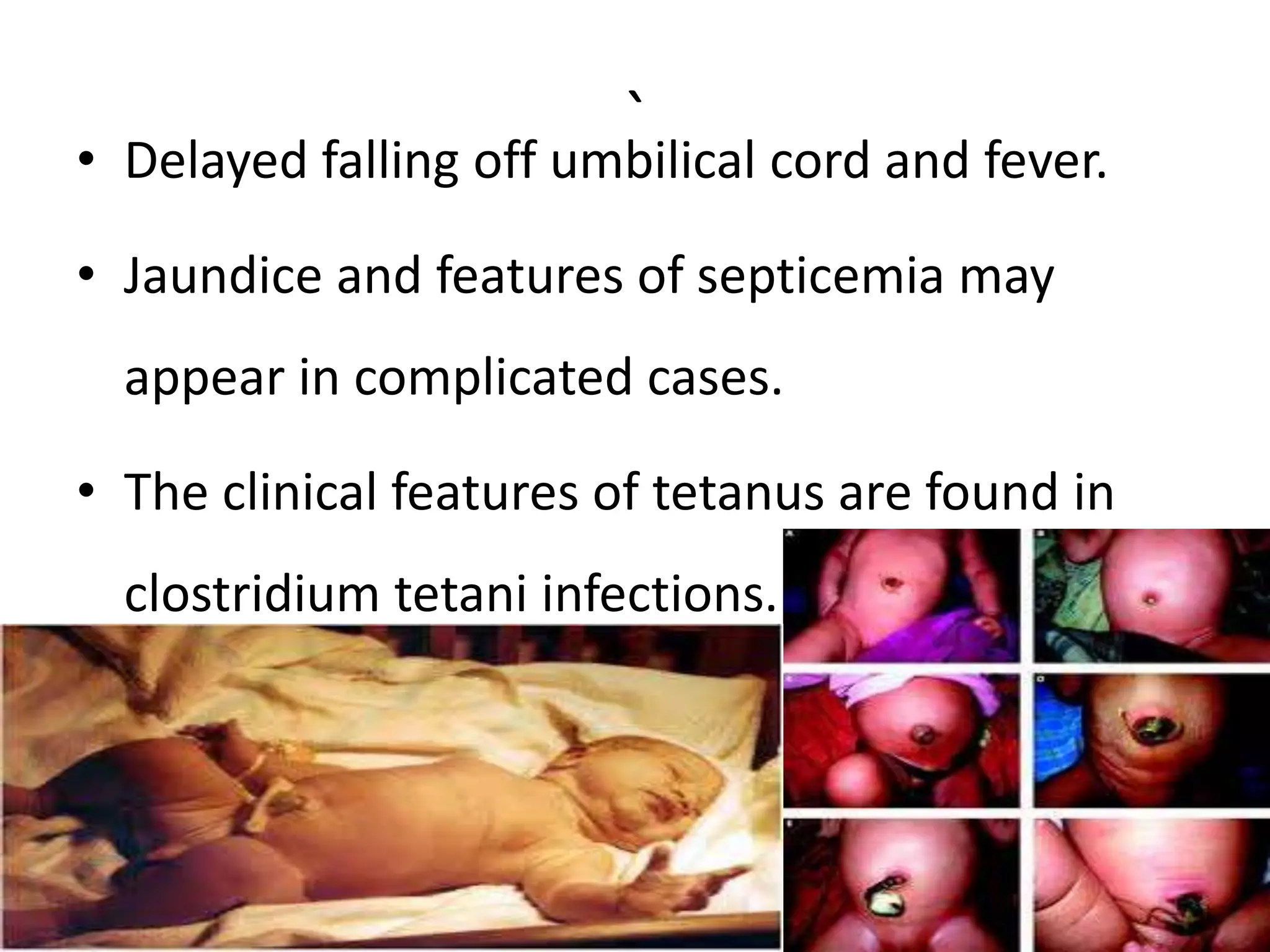






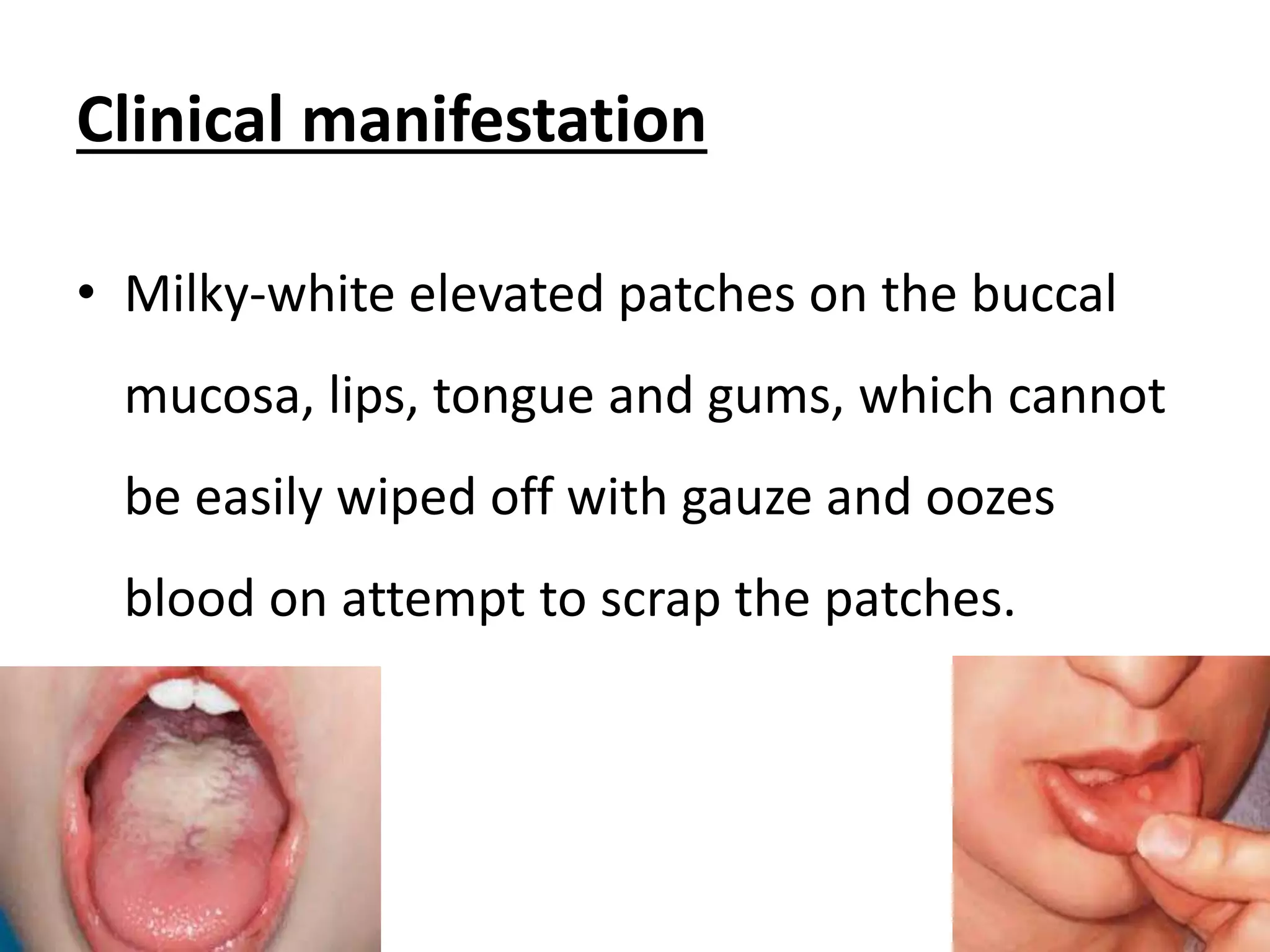
































































The seminar conducted by Mr. Abhijit Bhoyar provides comprehensive knowledge on neonatal infections, focusing on their prevention and management. It highlights common types of neonatal infections, their etiology, clinical features, and management strategies, emphasizing the importance of hygiene and early treatment. The presentation aims to equip students with the skills to care for neonates while understanding the risks and preventive measures against infections that can lead to severe outcomes.






































































































