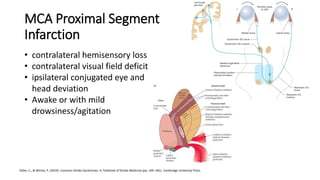
1. The document discusses the anatomy and branches of the middle cerebral artery (MCA), which supplies blood to the lateral surface of the brain.
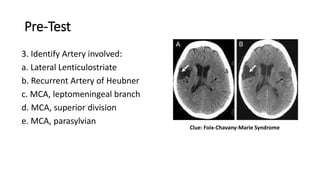
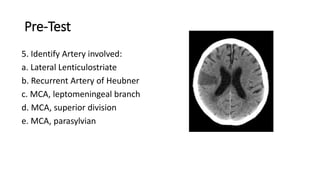
2. MCA territory infarctions are among the most common types of stroke, and can cause a range of neurological deficits depending on the specific branch occluded.
3. Infarctions in different MCA branches lead to characteristic clinical syndromes, such as expressive aphasia from left MCA superior division strokes or visual neglect from right MCA inferior division strokes.