Leptospirosis Protocol for NABH accredition
•
0 likes•32 views
Leptospirosis Protocol for NABH accredition - prepared for Institute of Internal Medicine, Madras Medical College.
Report
Share
Report
Share
Download to read offline
Recommended
Acute pancreatitis / Epigastric pain

ACUTE PANCREATITIS- EPIGASTRIC PAIN
#surgicaleducator #epigastricabdominalpain #acutepancreatitis #usmle #babysurgeon #surgicaltutor
• Dear Viewers,
• Greetings from “Surgical Educator”
• Today I have uploaded a video on Acute Pancreatitis- a didactic lecture. I have already uploaded 2 more videos on the same topic, one in case based learning of abdominal pain and another one in image based questions for Hepato-biliary- pancreatic pathologies.
• It is one of the common surgical problems you see in surgical wards.
• I have discussed the various causes for Epigastric pain, etiology, pathology, clinical features, investigations, scoring systems, complications and treatment of Acute Pancreatitis.
• I have also included a mind map and a treatment algorithm for Acute Pancreatitis.
• I hope the video will be very useful and you will enjoy it.
• You can watch all my surgical teaching videos in the following link:
• youtube.com/c/surgicaleducator
• Thank you for watching the video.
Recommended
Acute pancreatitis / Epigastric pain

ACUTE PANCREATITIS- EPIGASTRIC PAIN
#surgicaleducator #epigastricabdominalpain #acutepancreatitis #usmle #babysurgeon #surgicaltutor
• Dear Viewers,
• Greetings from “Surgical Educator”
• Today I have uploaded a video on Acute Pancreatitis- a didactic lecture. I have already uploaded 2 more videos on the same topic, one in case based learning of abdominal pain and another one in image based questions for Hepato-biliary- pancreatic pathologies.
• It is one of the common surgical problems you see in surgical wards.
• I have discussed the various causes for Epigastric pain, etiology, pathology, clinical features, investigations, scoring systems, complications and treatment of Acute Pancreatitis.
• I have also included a mind map and a treatment algorithm for Acute Pancreatitis.
• I hope the video will be very useful and you will enjoy it.
• You can watch all my surgical teaching videos in the following link:
• youtube.com/c/surgicaleducator
• Thank you for watching the video.
Diagnosis and examination of swollen lymph nodes ppt.pptx

Diagnosis and examination of swollen lymph nodes, introduction to Clinics
Biliary emergencies.pptx

This is based on approach to a patient presenting to emergency department complaining of right hypochondriac pain. It includes anatomy, pathophysiology, epidemiology, clinical assessment, investigation, management, complication and disposition of a biliary infection.
Thrombocytopenia in pregnancy

The pathology of thrombocytopenia in pregnancy, risk factors, diagnosis, treatment etc.
Dengue Fever - Rational Management

This talk was delivered by Dr. Shashikiran Umakanth on 10 Jan, 2016 as part of CME on Infectious Diseases conducted by the Indian Medical Association, Udupi-Karavali branch, Karnataka, India.
Manievelraaman's APPROACH TO NEUROLOGICAL WEAKNESS

Manievelraaman's APPROACH TO NEUROLOGICAL WEAKNESS.
PPT used for PG symposium of M.D. General Medicine Post-Graduates
Parkinson Plus Syndrome - Multiple System Atrophy: Case Report

Parkinson Plus Syndrome - Multiple System Atrophy: Case Report.
Poster used in CMC MAC 2021.
ABSTRACT
A 61yr/Male, K/C/O T2DM & Parkinson’s disease(PD) on T.Metformin and T.Syndopa for 3 years, presented to us with complaints of unsteadiness of gait, dysarthria, bilateral upper limb tremor. These symptoms started gradually and has been there for last 3 years and it is progressive. Initially, it started as inability to write and difficulty in mixing food due to tremulousness of both hands which worsens with activity. Then it progressed to slurred speech and then to gait unsteadiness. Patient also has urinary incontinence for last 2 years. Patient’s symptoms are more in severity for last 6 months. On examination, patient was having orthostatic hypotension, cogwheel rigidity on bilateral wrist movement and pendular knee jerks. All cerebellar signs were present bilaterally including finger nose test abnormality, past pointing, dysdiadochokinesia, heel shin test abnormality, gross truncal ataxia, wide based gait, impaired tandem walking, gaze evoked nystagmus, scanning speech.
Presence of cerebellar signs, autonomic disturbances, poor response to syndopa, rapid progression, lack of resting tremor at presentation, symmetrical involvement, early speech and gait involvement - are usually NOT seen in PD. So, evaluated further. MRI Brain T2 showed classical cruciform hyperintensity in pons (Hot cross bun sign) & diffuse cerebellar atrophy. Hence the diagnosis MULTIPLE SYSTEM ATROPHY (MSA-C) - Shy Drager Syndrome. This shows the importance of identifying atypical features in PD.
More Related Content
Similar to Leptospirosis Protocol for NABH accredition
Diagnosis and examination of swollen lymph nodes ppt.pptx

Diagnosis and examination of swollen lymph nodes, introduction to Clinics
Biliary emergencies.pptx

This is based on approach to a patient presenting to emergency department complaining of right hypochondriac pain. It includes anatomy, pathophysiology, epidemiology, clinical assessment, investigation, management, complication and disposition of a biliary infection.
Thrombocytopenia in pregnancy

The pathology of thrombocytopenia in pregnancy, risk factors, diagnosis, treatment etc.
Dengue Fever - Rational Management

This talk was delivered by Dr. Shashikiran Umakanth on 10 Jan, 2016 as part of CME on Infectious Diseases conducted by the Indian Medical Association, Udupi-Karavali branch, Karnataka, India.
Similar to Leptospirosis Protocol for NABH accredition (20)
Matthew Rosenfeld final presentation legionnaires 2015

Matthew Rosenfeld final presentation legionnaires 2015
Diagnosis and examination of swollen lymph nodes ppt.pptx

Diagnosis and examination of swollen lymph nodes ppt.pptx
More from Manievelraaman Kannan
Manievelraaman's APPROACH TO NEUROLOGICAL WEAKNESS

Manievelraaman's APPROACH TO NEUROLOGICAL WEAKNESS.
PPT used for PG symposium of M.D. General Medicine Post-Graduates
Parkinson Plus Syndrome - Multiple System Atrophy: Case Report

Parkinson Plus Syndrome - Multiple System Atrophy: Case Report.
Poster used in CMC MAC 2021.
ABSTRACT
A 61yr/Male, K/C/O T2DM & Parkinson’s disease(PD) on T.Metformin and T.Syndopa for 3 years, presented to us with complaints of unsteadiness of gait, dysarthria, bilateral upper limb tremor. These symptoms started gradually and has been there for last 3 years and it is progressive. Initially, it started as inability to write and difficulty in mixing food due to tremulousness of both hands which worsens with activity. Then it progressed to slurred speech and then to gait unsteadiness. Patient also has urinary incontinence for last 2 years. Patient’s symptoms are more in severity for last 6 months. On examination, patient was having orthostatic hypotension, cogwheel rigidity on bilateral wrist movement and pendular knee jerks. All cerebellar signs were present bilaterally including finger nose test abnormality, past pointing, dysdiadochokinesia, heel shin test abnormality, gross truncal ataxia, wide based gait, impaired tandem walking, gaze evoked nystagmus, scanning speech.
Presence of cerebellar signs, autonomic disturbances, poor response to syndopa, rapid progression, lack of resting tremor at presentation, symmetrical involvement, early speech and gait involvement - are usually NOT seen in PD. So, evaluated further. MRI Brain T2 showed classical cruciform hyperintensity in pons (Hot cross bun sign) & diffuse cerebellar atrophy. Hence the diagnosis MULTIPLE SYSTEM ATROPHY (MSA-C) - Shy Drager Syndrome. This shows the importance of identifying atypical features in PD.
Allergy Induced Acute Coronary Syndrome - Kounis Syndrome

Allergy Induced Acute Coronary Syndrome - Kounis Syndrome: Case Report.
Poster used in CMC MAC 2021.
OBJECTIVE: To discuss a rare occurrence of allergic reaction to NSAID causing Myocardial Infarction.
BACKGROUND: A 21-year-old obese female with no other comorbidities was referred to us with history of chest pain, generalized urticarial rashes and itch suddenly following Inj.IM Diclofenac, which was given for heel pain relief. She was hemodynamically stable, but tachypneic, orthopneic and was having bilateral basal crepitations. ECG revealed significant ST depression & T inversion in II,III,aVF and V2-V6 and ST elevation in aVR. CXR showed pulmonary edema. Diagnosed as ACS following anaphylaxis and loading dose was given along with IM adrenaline, antihistamines, and steroids. Echo revealed global hypokinesia of LV. Cardiac enzymes were elevated. Meanwhile, she had a prompt relief of chestpain, but dyspnea worsened and warranted NIV support. Repeat ECG revealed regression of ST changes correlating with chest pain relief. After 2 days of NIV, patient’s dyspnea improved and weaned from NIV. CAG revealed normal epicardial coronaries. Serial cardiac enzyme levels showed falling trend and ECG was completely normal with no significant ST-T changes. Pre-discharge, repeat echo showed persistence of global hypokinesia. 2weeks later, repeat echo showed dramatic improvement with normal LV systolic function suggesting recovery from myocardial stunning.
RESULTS: This qualifies for the diagnosis of MINOCA (Myocardial Infarction with No Obstructive Coronary Arteries). In the setting of allergic trigger, vasospasm or coronary hypersensitivity is the underlying mechanism- described as KOUNIS SYNDROME.
CONCLUSION: ECG changes and chest discomforts that occur in allergic reactions are not always secondary to distributive/anaphylactic shock. Sometimes heart could be the primarily affected organ by the allergic reaction as in this case. Although <200cases reported globally until 2017, it’s suspected to be frequently overlooked, hence likely to be more prevalent.
Brugada Syndrome - A Cardiac Channelopathy: Case Report

Case Report: Brugada Syndrome - A Cardiac Channelopathy.
Poster used for presentation in CMC MAC 2021.
OBJECTIVE: To discuss an interesting case of Brugada syndrome presenting as seizures.
BACKGROUND: A 25-year-old well-informed male presented to us with complaints of seizure on day 3 of an acute febrile illness. He was conscious, oriented, GCS15/15 and system examinations were unremarkable. He had a similar history of seizure during fever 1 year back and was started on anti-epileptics since then and was treated with empirical antibiotics and CSF analysis, MRI brain with seizure protocol and EEG were completely normal during that episode. As described by patient, both episodes were very similar and was like darkening of visual field followed by LOC and bystanders witnessed few jerks involving both sides of body followed by regaining consciousness. This raised suspicion for syncope and ECG revealed RBBB-rSR’ pattern and saddleback STE in V1-V3(type2-brugada pattern-not diagnostic on its own). But on probing, patient revealed SCD in his father at age 42.
RESULTS: Echo revealed structurally normal heart. Expert opinion sought and flecainide challenge test revealed the classical type1 brugada pattern (diagnostic) with coved STE and T inversion in V1-V3 clinching the diagnosis of BRUGADA SYNDROME. Genetic testing for channelopathy was unremarkable. Type 1 Brugada pattern (on provocative testing) along with syncopal event and family history strongly warranted AICD insertion and patient opted for subcutaneous ICD. 6 months later, ICD interrogation revealed occurrence of 1 episode of NSVT, which fell below the ICD intervention threshold.
CONCLUSION: Brugada syndrome is a rare cardiac channelopathy with high risk of SCD in the absence of intervention. Events during fever and family history are very classical. It has male preponderance and more seen in Southeast Asia. All cases of suspected syncopal attacks warrant a thorough search for ECG markers of SCD.
Allergy Induced Myocardial Infarction - Kounis Syndrome / Coronary Hypersensi...

Allergy Induced Myocardial Infarction - Kounis Syndrome / Coronary Hypersensi...Manievelraaman Kannan
Case Presentation PPT - For TAPICON 2021
Case Report: Allergy Induced Myocardial Infarction - Kounis Syndrome / Coronary Hypersensitivity Disorder / Vasospastic Angina.
Abstract
A young female with no coronary risk factors presented to us with history of chest pain, generalized urticarial rashes and itch suddenly following Inj.IM Diclofenac, which was given for heel pain relief. She was hemodynamically stable, but tachypneic, orthopneic with bilateral basal crepitations.
ECG showed significant ST depression & T inversion in II,III,aVF and V2-V6 and ST elevation in aVR. CXR showed pulmonary edema. Echo revealed global hypokinesia of LV. Cardiac enzymes were elevated. Treated for acute coronary syndrome (ACS) and her pain got relieved. CAG showed normal epicardial coronaries. Repeat ECG showed regression of ST changes correlating with chest pain relief and enzymes were also falling.
Pre-discharge, ECG normalised but echo showed persistence of global hypokinesia. Two weeks later, repeat echo showed dramatic improvement with normal LV systolic function suggesting recovery from myocardial stunning.
This qualifies for the diagnosis of MINOCA (Myocardial Infarction with No Obstructive Coronary Arteries). In the setting of allergic trigger, vasospasm or coronary hypersensitivity is the underlying mechanism - described as KOUNIS SYNDROME.
ECG changes and chest discomforts that occur in allergic reactions are NOT ALWAYS SECONDARY to distributive/anaphylactic shock. Sometimes heart could be the primarily affected organ by the allergic reaction. It is frequently overlooked and its timely recognition and appropriate intervention will improve the outcome.TB Myeloradiculopathy

A case of Acute onset areflexic flaccid paraparesis with paresthesia with bladder involvement
COLLOID CYST OF BRAIN / CNS SPACE OCCUPYING LESIONS - BENIGN

ALL HYPERDENSITIES IN CT BRAIN ARE NOT BLEEDS.
THIS IS COLLOID CYST OF BRAIN - IDENTIFIED BY TYPICAL HISTORY AND APPROPRIATE LOCATION OF CYST
Allergic Acute Coronary Syndrome - KOUNIS SYNDROME

CASE REPORT OF A YOUNG OTHERWISE HEALTHY FEMALE WHO DEVELOPED ACUTE CORONARY SYNDROME (ACS) FOLLOWING DICLOFENAC INJECTION
Abnormal Uterine Bleeding (AUB) -Etiopathogenesis

A brief note on WHAT causes AUB and WHY it does so.
Micturition reflex / Neural control of Urination

physiology and pathology of the reflex that mediates micturition (urination)
More from Manievelraaman Kannan (11)
Manievelraaman's APPROACH TO NEUROLOGICAL WEAKNESS

Manievelraaman's APPROACH TO NEUROLOGICAL WEAKNESS
Parkinson Plus Syndrome - Multiple System Atrophy: Case Report

Parkinson Plus Syndrome - Multiple System Atrophy: Case Report
Allergy Induced Acute Coronary Syndrome - Kounis Syndrome

Allergy Induced Acute Coronary Syndrome - Kounis Syndrome
Brugada Syndrome - A Cardiac Channelopathy: Case Report

Brugada Syndrome - A Cardiac Channelopathy: Case Report
Allergy Induced Myocardial Infarction - Kounis Syndrome / Coronary Hypersensi...

Allergy Induced Myocardial Infarction - Kounis Syndrome / Coronary Hypersensi...
COLLOID CYST OF BRAIN / CNS SPACE OCCUPYING LESIONS - BENIGN

COLLOID CYST OF BRAIN / CNS SPACE OCCUPYING LESIONS - BENIGN
Allergic Acute Coronary Syndrome - KOUNIS SYNDROME

Allergic Acute Coronary Syndrome - KOUNIS SYNDROME
Recently uploaded
NVBDCP.pptx Nation vector borne disease control program

NVBDCP was launched in 2003-2004 . Vector-Borne Disease: Disease that results from an infection transmitted to humans and other animals by blood-feeding arthropods, such as mosquitoes, ticks, and fleas. Examples of vector-borne diseases include Dengue fever, West Nile Virus, Lyme disease, and malaria.
The Electrocardiogram - Physiologic Principles

These lecture slides, by Dr Sidra Arshad, offer a quick overview of the physiological basis of a normal electrocardiogram.
Learning objectives:
1. Define an electrocardiogram (ECG) and electrocardiography
2. Describe how dipoles generated by the heart produce the waveforms of the ECG
3. Describe the components of a normal electrocardiogram of a typical bipolar lead (limb II)
4. Differentiate between intervals and segments
5. Enlist some common indications for obtaining an ECG
6. Describe the flow of current around the heart during the cardiac cycle
7. Discuss the placement and polarity of the leads of electrocardiograph
8. Describe the normal electrocardiograms recorded from the limb leads and explain the physiological basis of the different records that are obtained
9. Define mean electrical vector (axis) of the heart and give the normal range
10. Define the mean QRS vector
11. Describe the axes of leads (hexagonal reference system)
12. Comprehend the vectorial analysis of the normal ECG
13. Determine the mean electrical axis of the ventricular QRS and appreciate the mean axis deviation
14. Explain the concepts of current of injury, J point, and their significance
Study Resources:
1. Chapter 11, Guyton and Hall Textbook of Medical Physiology, 14th edition
2. Chapter 9, Human Physiology - From Cells to Systems, Lauralee Sherwood, 9th edition
3. Chapter 29, Ganong’s Review of Medical Physiology, 26th edition
4. Electrocardiogram, StatPearls - https://www.ncbi.nlm.nih.gov/books/NBK549803/
5. ECG in Medical Practice by ABM Abdullah, 4th edition
6. Chapter 3, Cardiology Explained, https://www.ncbi.nlm.nih.gov/books/NBK2214/
7. ECG Basics, http://www.nataliescasebook.com/tag/e-c-g-basics
Physiology of Chemical Sensation of smell.pdf

Title: Sense of Smell
Presenter: Dr. Faiza, Assistant Professor of Physiology
Qualifications:
MBBS (Best Graduate, AIMC Lahore)
FCPS Physiology
ICMT, CHPE, DHPE (STMU)
MPH (GC University, Faisalabad)
MBA (Virtual University of Pakistan)
Learning Objectives:
Describe the primary categories of smells and the concept of odor blindness.
Explain the structure and location of the olfactory membrane and mucosa, including the types and roles of cells involved in olfaction.
Describe the pathway and mechanisms of olfactory signal transmission from the olfactory receptors to the brain.
Illustrate the biochemical cascade triggered by odorant binding to olfactory receptors, including the role of G-proteins and second messengers in generating an action potential.
Identify different types of olfactory disorders such as anosmia, hyposmia, hyperosmia, and dysosmia, including their potential causes.
Key Topics:
Olfactory Genes:
3% of the human genome accounts for olfactory genes.
400 genes for odorant receptors.
Olfactory Membrane:
Located in the superior part of the nasal cavity.
Medially: Folds downward along the superior septum.
Laterally: Folds over the superior turbinate and upper surface of the middle turbinate.
Total surface area: 5-10 square centimeters.
Olfactory Mucosa:
Olfactory Cells: Bipolar nerve cells derived from the CNS (100 million), with 4-25 olfactory cilia per cell.
Sustentacular Cells: Produce mucus and maintain ionic and molecular environment.
Basal Cells: Replace worn-out olfactory cells with an average lifespan of 1-2 months.
Bowman’s Gland: Secretes mucus.
Stimulation of Olfactory Cells:
Odorant dissolves in mucus and attaches to receptors on olfactory cilia.
Involves a cascade effect through G-proteins and second messengers, leading to depolarization and action potential generation in the olfactory nerve.
Quality of a Good Odorant:
Small (3-20 Carbon atoms), volatile, water-soluble, and lipid-soluble.
Facilitated by odorant-binding proteins in mucus.
Membrane Potential and Action Potential:
Resting membrane potential: -55mV.
Action potential frequency in the olfactory nerve increases with odorant strength.
Adaptation Towards the Sense of Smell:
Rapid adaptation within the first second, with further slow adaptation.
Psychological adaptation greater than receptor adaptation, involving feedback inhibition from the central nervous system.
Primary Sensations of Smell:
Camphoraceous, Musky, Floral, Pepperminty, Ethereal, Pungent, Putrid.
Odor Detection Threshold:
Examples: Hydrogen sulfide (0.0005 ppm), Methyl-mercaptan (0.002 ppm).
Some toxic substances are odorless at lethal concentrations.
Characteristics of Smell:
Odor blindness for single substances due to lack of appropriate receptor protein.
Behavioral and emotional influences of smell.
Transmission of Olfactory Signals:
From olfactory cells to glomeruli in the olfactory bulb, involving lateral inhibition.
Primitive, less old, and new olfactory systems with different path
SURGICAL ANATOMY OF THE RETROPERITONEUM, ADRENALS, KIDNEYS AND URETERS.pptx

For educational purposes for medical students and registrars in Urology
ABDOMINAL TRAUMA in pediatrics part one.

Abdominal trauma in pediatrics refers to injuries or damage to the abdominal organs in children. It can occur due to various causes such as falls, motor vehicle accidents, sports-related injuries, and physical abuse. Children are more vulnerable to abdominal trauma due to their unique anatomical and physiological characteristics. Signs and symptoms include abdominal pain, tenderness, distension, vomiting, and signs of shock. Diagnosis involves physical examination, imaging studies, and laboratory tests. Management depends on the severity and may involve conservative treatment or surgical intervention. Prevention is crucial in reducing the incidence of abdominal trauma in children.
KDIGO 2024 guidelines for diabetologists

KDIGO guidelines 2024 for evaluation and management of CKD, related to diabetes and management of diabetic kidney disease
Role of Mukta Pishti in the Management of Hyperthyroidism

Muktapishti is a traditional Ayurvedic preparation made from Shoditha Mukta (Purified Pearl), is believed to help regulate thyroid function and reduce symptoms of hyperthyroidism due to its cooling and balancing properties. Clinical evidence on its efficacy remains limited, necessitating further research to validate its therapeutic benefits.
Novas diretrizes da OMS para os cuidados perinatais de mais qualidade

Novas diretrizes da OMS para os cuidados perinatais de mais qualidadeProf. Marcus Renato de Carvalho
Recomendações da OMS sobre cuidados maternos e neonatais para uma experiência pós-natal positiva.
Em consonância com os ODS – Objetivos do Desenvolvimento Sustentável e a Estratégia Global para a Saúde das Mulheres, Crianças e Adolescentes, e aplicando uma abordagem baseada nos direitos humanos, os esforços de cuidados pós-natais devem expandir-se para além da cobertura e da simples sobrevivência, de modo a incluir cuidados de qualidade.
Estas diretrizes visam melhorar a qualidade dos cuidados pós-natais essenciais e de rotina prestados às mulheres e aos recém-nascidos, com o objetivo final de melhorar a saúde e o bem-estar materno e neonatal.
Uma “experiência pós-natal positiva” é um resultado importante para todas as mulheres que dão à luz e para os seus recém-nascidos, estabelecendo as bases para a melhoria da saúde e do bem-estar a curto e longo prazo. Uma experiência pós-natal positiva é definida como aquela em que as mulheres, pessoas que gestam, os recém-nascidos, os casais, os pais, os cuidadores e as famílias recebem informação consistente, garantia e apoio de profissionais de saúde motivados; e onde um sistema de saúde flexível e com recursos reconheça as necessidades das mulheres e dos bebês e respeite o seu contexto cultural.
Estas diretrizes consolidadas apresentam algumas recomendações novas e já bem fundamentadas sobre cuidados pós-natais de rotina para mulheres e neonatos que recebem cuidados no pós-parto em unidades de saúde ou na comunidade, independentemente dos recursos disponíveis.
É fornecido um conjunto abrangente de recomendações para cuidados durante o período puerperal, com ênfase nos cuidados essenciais que todas as mulheres e recém-nascidos devem receber, e com a devida atenção à qualidade dos cuidados; isto é, a entrega e a experiência do cuidado recebido. Estas diretrizes atualizam e ampliam as recomendações da OMS de 2014 sobre cuidados pós-natais da mãe e do recém-nascido e complementam as atuais diretrizes da OMS sobre a gestão de complicações pós-natais.
O estabelecimento da amamentação e o manejo das principais intercorrências é contemplada.
Recomendamos muito.
Vamos discutir essas recomendações no nosso curso de pós-graduação em Aleitamento no Instituto Ciclos.
Esta publicação só está disponível em inglês até o momento.
Prof. Marcus Renato de Carvalho
www.agostodourado.com
micro teaching on communication m.sc nursing.pdf

Microteaching is a unique model of practice teaching. It is a viable instrument for the. desired change in the teaching behavior or the behavior potential which, in specified types of real. classroom situations, tends to facilitate the achievement of specified types of objectives.
Integrating Ayurveda into Parkinson’s Management: A Holistic Approach

Explore the benefits of combining Ayurveda with conventional Parkinson's treatments. Learn how a holistic approach can manage symptoms, enhance well-being, and balance body energies. Discover the steps to safely integrate Ayurvedic practices into your Parkinson’s care plan, including expert guidance on diet, herbal remedies, and lifestyle modifications.
Light House Retreats: Plant Medicine Retreat Europe

Our aim is to organise conscious gatherings and retreats for open and inquisitive minds and souls, with and without the assistance of sacred plants.
Recently uploaded (20)
NVBDCP.pptx Nation vector borne disease control program

NVBDCP.pptx Nation vector borne disease control program
Thyroid Gland- Gross Anatomy by Dr. Rabia Inam Gandapore.pptx

Thyroid Gland- Gross Anatomy by Dr. Rabia Inam Gandapore.pptx
SURGICAL ANATOMY OF THE RETROPERITONEUM, ADRENALS, KIDNEYS AND URETERS.pptx

SURGICAL ANATOMY OF THE RETROPERITONEUM, ADRENALS, KIDNEYS AND URETERS.pptx
Pharynx and Clinical Correlations BY Dr.Rabia Inam Gandapore.pptx

Pharynx and Clinical Correlations BY Dr.Rabia Inam Gandapore.pptx
Role of Mukta Pishti in the Management of Hyperthyroidism

Role of Mukta Pishti in the Management of Hyperthyroidism
Maxilla, Mandible & Hyoid Bone & Clinical Correlations by Dr. RIG.pptx

Maxilla, Mandible & Hyoid Bone & Clinical Correlations by Dr. RIG.pptx
Novas diretrizes da OMS para os cuidados perinatais de mais qualidade

Novas diretrizes da OMS para os cuidados perinatais de mais qualidade
Integrating Ayurveda into Parkinson’s Management: A Holistic Approach

Integrating Ayurveda into Parkinson’s Management: A Holistic Approach
Light House Retreats: Plant Medicine Retreat Europe

Light House Retreats: Plant Medicine Retreat Europe
Leptospirosis Protocol for NABH accredition
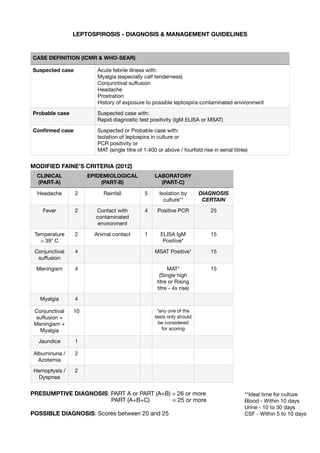
- 1. LEPTOSPIROSIS - DIAGNOSIS & MANAGEMENT GUIDELINES MODIFIED FAINE’S CRITERIA (2012) PRESUMPTIVE DIAGNOSIS: PART A or PART (A+B) = 26 or more PART (A+B+C) = 25 or more POSSIBLE DIAGNOSIS: Scores between 20 and 25 CASE DEFINITION (ICMR & WHO-SEAR) Suspected case Acute febrile illness with: Myalgia (especially calf tenderness) Conjunctival su ff usion Headache Prostration History of exposure to possible leptospira-contaminated environment Probable case Suspected case with: Rapid diagnostic test positivity (IgM ELISA or MSAT) Con fi rmed case Suspected or Probable case with: Isolation of leptospira in culture or PCR positivity or MAT (single titre of 1:400 or above / fourfold rise in serial titres) CLINICAL (PART-A) EPIDEMIOLOGICAL (PART-B) LABORATORY (PART-C) Headache 2 Rainfall 5 Isolation by culture** DIAGNOSIS CERTAIN Fever 2 Contact with contaminated environment 4 Positive PCR 25 Temperature > 39* C 2 Animal contact 1 ELISA IgM Positive* 15 Conjunctival su ff usion 4 MSAT Positive* 15 Meningism 4 MAT* (Single high titre or Rising titre - 4x rise) 15 Myalgia 4 Conjunctival su ff usion + Meningism + Myalgia 10 *any one of the tests only should be considered for scoring Jaundice 1 Albuminuria / Azotemia 2 Hemoptysis / Dyspnea 2 **Ideal time for culture Blood - Within 10 days Urine - 10 to 30 days CSF - Within 5 to 10 days
- 2. Leptospirosis - Suspected / Probable / Con fi rmed 90% of cases are Mild Leptospirosis (Fever, myalgia, conjunctival suffusion, headache BUT NO JAUNDICE) Around 10% cases are Moderate / Severe Leptospirosis (Fever, myalgia, conjunctival suffusion, headache + JAUNDICE +/- Multi-organ involvement Based on clinical spectrum OP Treatment Doxycycline 100mg PO BD x 7 days or Amoxicillin 500mg PO TDS x 7 days or Ampicillin 500mg PO TDS x 7days or Azithromycin 500mg PO OD x 3 days Other supportive Rx* *advise adequate hydration, bed rest, antipyretics etc. RED FLAG SIGNS (tachypnea, tachycardia disproportionate to fever, shock, altered sensorium, oliguria, bleeding manifestations etc.) IP Treatment (Antibiotic Rx +/- Organ speci fi c Rx) Antibiotic therapy: Penicillin 1.5 million units IV QID x 7 days or Ceftriaxone 1g IV BD x 7 days or Doxycycline 200mg IV stat, then 100mg IV BD x 7days (Doxycycline contraindicated in pregnancy) Organ speci fi c therapy: RENAL: renal involvement is common. Mild - only proteinuria and no RFT derangement: No intervention Severe - AKI: Fluid management +/- diuretics, electrolyte correction, avoid nephrotoxic drugs, avoid hypotension and hypovolemia +/- RRT (if indicated by standard RRT guidelines) HEPATIC: acute liver failure is rare. Avoid precipitating factors of hepatic encephalopathy - drugs (hepatotoxic drugs, sedatives etc.), hypovolemia, hypokalemia, alkalosis, constipation, UGI bleeding. Jaundice, Hepatomegaly: No intervention Hepatic encephalopathy: lactulose, rifaximin etc. LUNG: Most dangerous complication ARDS / Pulmonary hemorrhage: Continuous O2 therapy, Mechanical ventilation (if indicated) HEART: Myocarditis / Arrhythmia: treatment of speci fi c arrhythmia Shock: treat hypovolemia with fl uid replacement. If not responding, add dopamine or dobutamine. HEMATOLOGICAL: Thrombocytopenia: Platelet transfusion (if indicated) Coagulopathy: Vit.K 5-10mg IV x 3 days +/- Fresh Frozen Plasma DIC: FFP +/- blood transfusion NEUROLOGICAL: Aseptic meningitis: Symptomatic and supportive management. Hypokalemic paralysis: IV Potassium supplementation MUSCULOSKELETAL: Myalgia / Myositis / Rhabdomyolysis : Monitor CPK levels, adequate hydration, monitor urine output and serum electrolytes. Arthralgia: No intervention +/- analgesic-antipyretics All Absent Any one or more is present Always rule out other tropical diseases. Mixed infections are common. Important differential diagnosis include: -Malaria -Scrub typhus -Dengue -Hepatitis -Enteric fever etc.
- 3. Leptospirosis Zoonotic Pathogenic spirochete – Leptospira interrogans Rodents and Cattle excrete these organisms in their urine, which contaminates soil and waterbodies Mode of transmission: contact of abraded skin or mucous membrane with contaminated environment Incubation period: Average 5-14 days with a range 2- 30 days Risk factors: o Heavy rainfall and water logging o Natural disasters like floods o Seasonal – at the onset of monsoon o Farmers o Agricultural field workers o Fishermen o Sewer workers o Livestock handlers o Mason o Residence in endemic area Presentation spectrum: o Anicteric Leptospirosis: (90%) – Mild form presents like Acute undifferentiated fever o Icteric Leptospirosis: (5-10%) – Moderate-Severe form o Weil’s Disease (0-5%) – Severe form When to suspect Leptospirosis? o Acute febrile illness + Risk factors + one or more of the following: Headache Myalgia Prostration Calf muscle tenderness Conjunctival suffusion Oliguria / Frothy urine Jaundice Haemorrhagic manifestations Meningeal irritation Nausea, Vomiting, Abdominal pain, Diarrhoea Lab investigations to support diagnosis: (Blood, CSF, Urine sample) o MAT titre of 100/200/400 or above based on endemicity (preferred) o IgM based immune assays o Seroconversion or Four-fold rise in MAT titre between acute and convalescent sera o Direct isolation of organism o PCR test
- 4. Lab investigations to assess severity: o CBC, ESR o RFT, LFT o S. Electrolytes o Urine Routine examination o CPK o CXR, ABG Management: o IVF and correction of electrolytes o Mild cases: Tab. Doxycycline 100mg PO BD X 7 days (preferred) or Tab. Azithromycin 500mg PO OD X 3 days o Moderate / Severe cases: Inj. Penicillin 1.5 million units IV or IM Q6H X 7 days or Inj. Ceftriaxone 2g IV OD X 7 days o Chemoprophylaxis: Tab. Doxycycline 200mg PO once a week or Tab. Azithromycin 250mg PO once/ twice a week
- 5. DIAGNOSTIC: A + B = /> 26 OR A + B + C = /> 25 POSSIBLE: A + B = Between 20 to 25 CRITERIA
