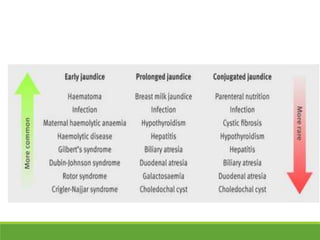
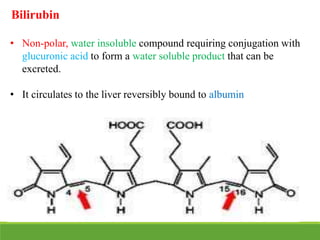
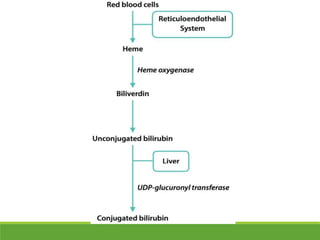
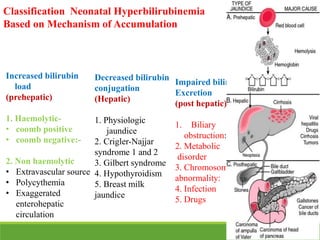
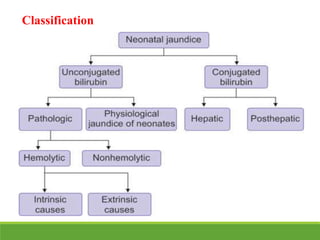
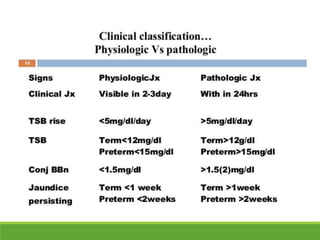
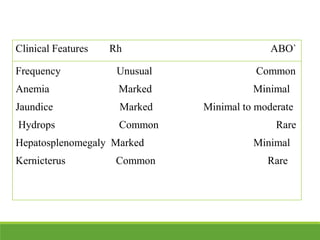
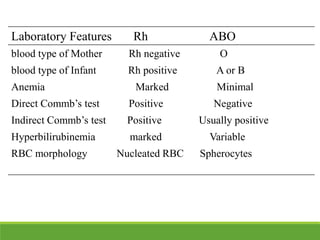
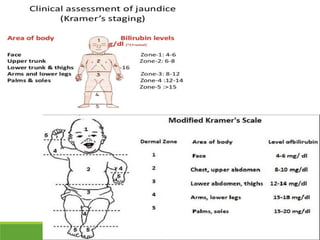
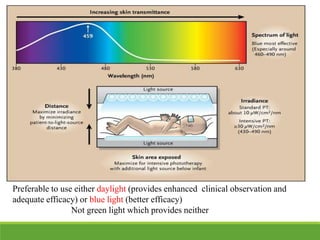
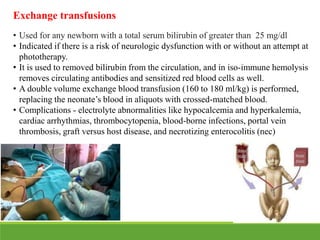
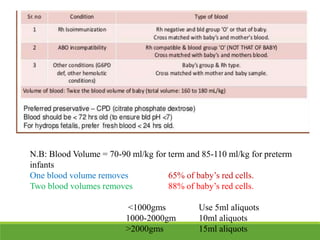
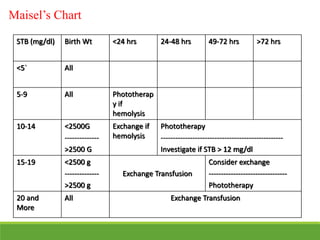
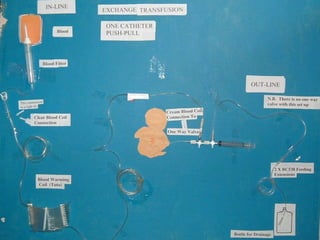
La ictericia neonatal es una condición común en recién nacidos, que se manifiesta como una coloración amarillenta de la piel y los ojos debido a niveles elevados de bilirrubina. Factores como el nacimiento prematuro, hematomas al nacer y la incompatibilidad de grupos sanguíneos pueden aumentar el riesgo de ictericia. Esta condición puede clasificarse como fisiológica o patológica, con diferentes mecanismos y tratamientos necesarios según la causa subyacente.