It Takes a Team for HCC: Improving Outcomes Through Multidisciplinary Collaboration & Modern Therapeutics
•
0 likes•70 views
Chair, Amit Singal, MD, MS, Anthony El-Khoueiry, MD, Ahmed Omar Kaseb, MD, CMQ, and Anjana Pillai, MD, prepared useful Practice Aids pertaining to hepatocellular carcinoma for this CME/MOC activity titled “It Takes a Team for HCC: Improving Outcomes Through Multidisciplinary Collaboration & Modern Therapeutics.” For the full presentation, downloadable Practice Aids, and complete CME/MOC information, and to apply for credit, please visit us at https://bit.ly/3AbNtC5. CME/MOC credit will be available until December 4, 2023.
Report
Share
Report
Share
Download to read offline
Recommended
Pioneering Precision Medicine in Bladder Cancer: Multidisciplinary Perspectiv...

Pioneering Precision Medicine in Bladder Cancer: Multidisciplinary Perspectiv...PVI, PeerView Institute for Medical Education
Chair and Presenter Neal D. Shore, MD, FACS, Sia Daneshmand, MD, and Guru P. Sonpavde, MD, prepared useful Practice Aids pertaining to bladder cancer for this CME/MOC/AAPA activity titled “Pioneering Precision Medicine in Bladder Cancer: Multidisciplinary Perspectives on Personalizing Patient Care.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/AAPA information, and to apply for credit, please visit us at https://bit.ly/40qGkJH. CME/MOC/AAPA credit will be available until December 28, 2024.Gi Cancer Symposium 2012 Report Presentation

Tonight’s speakers: Dr. Dan Sargent and Kim Ryan
Disclaimer: “This Report is not an official event of the 2012 Gastrointestinal Cancers Symposium. Not sponsored or endorsed by any of the cosponsoring organizations of the 2012 Gastrointestinal Cancers Symposium.”
New Thinking, New Strategies in Advanced Urothelial Carcinoma

i3 Health is pleased to make the speaker slides from this activity available for use as a nonaccredited self-study or teaching resource.
Colorectal Cancer Research & Treatment News - recap from the May 2014 ASCO co...

Colorectal Cancer Research & Treatment News - recap from the May 2014 ASCO co...Fight Colorectal Cancer
Dr. Cathy Eng delivers updates on current trials and studies impacting the treatment of colon and rectal cancer. Dalle linee guida dell'epatocarcinoma alla pratica clinica - Gastrolearning®

Gastrolearning XVI lezione
Dalle linee guida dell'epatocarcinoma alla pratica clinica - Prof. F. Trevisani (Università di Bologna).
Recommended
Pioneering Precision Medicine in Bladder Cancer: Multidisciplinary Perspectiv...

Pioneering Precision Medicine in Bladder Cancer: Multidisciplinary Perspectiv...PVI, PeerView Institute for Medical Education
Chair and Presenter Neal D. Shore, MD, FACS, Sia Daneshmand, MD, and Guru P. Sonpavde, MD, prepared useful Practice Aids pertaining to bladder cancer for this CME/MOC/AAPA activity titled “Pioneering Precision Medicine in Bladder Cancer: Multidisciplinary Perspectives on Personalizing Patient Care.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/AAPA information, and to apply for credit, please visit us at https://bit.ly/40qGkJH. CME/MOC/AAPA credit will be available until December 28, 2024.Gi Cancer Symposium 2012 Report Presentation

Tonight’s speakers: Dr. Dan Sargent and Kim Ryan
Disclaimer: “This Report is not an official event of the 2012 Gastrointestinal Cancers Symposium. Not sponsored or endorsed by any of the cosponsoring organizations of the 2012 Gastrointestinal Cancers Symposium.”
New Thinking, New Strategies in Advanced Urothelial Carcinoma

i3 Health is pleased to make the speaker slides from this activity available for use as a nonaccredited self-study or teaching resource.
Colorectal Cancer Research & Treatment News - recap from the May 2014 ASCO co...

Colorectal Cancer Research & Treatment News - recap from the May 2014 ASCO co...Fight Colorectal Cancer
Dr. Cathy Eng delivers updates on current trials and studies impacting the treatment of colon and rectal cancer. Dalle linee guida dell'epatocarcinoma alla pratica clinica - Gastrolearning®

Gastrolearning XVI lezione
Dalle linee guida dell'epatocarcinoma alla pratica clinica - Prof. F. Trevisani (Università di Bologna).
El futuro del tratamiento del cáncer renal metastásico: inmunoterapia y terap...

Ponencia en el primer simposio de la Asociación Colombiana de Hematología y Oncología (ACHO) de cáncer genitourinario, Bogotá, septiembre 23 y 24 de 2016.
Treatment of radioactive iodine-refractory metastatic differentiated thyroid ...

En el marco del Simposio de Cáncer de Cabeza y Cuello y Pulmón de la Asociación Colombiana de Hematología Oncología, ACHO, Bogotá, 28.07.2016
Actualización en el abordaje terapéutico ante un cáncer colorrectal metastásico

Ponencia en el VII Congreso internacional de coloproctología, Bogotá, 18.08.2016. Con énfasis en los estudios recientes en terapia antiangiogénica, y el impacto del lado del primario en el pronóstico (y aspectos predictivos) de la enfermedad metastásica.
Making an Impact in Bladder Cancer Care: Integrating the Latest Evidence and ...

Making an Impact in Bladder Cancer Care: Integrating the Latest Evidence and ...PVI, PeerView Institute for Medical Education
Chair and Presenters Matthew D. Galsky, MD, Shilpa Gupta, MD, and Andrea Necchi, MD, prepared useful Practice Aids pertaining to bladder cancer for this CME/MOC/AAPA/IPCE activity titled “Making an Impact in Bladder Cancer Care: Integrating the Latest Evidence and Modern Therapeutic Advances Across the Disease Continuum.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/AAPA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3QlbwW0. CME/MOC/AAPA/IPCE credit will be available until February 26, 2025.STEREOTACTIC BODY RADIATION THERAPY USING CYBERKNIFE® FOR LIVER METASTASES: A...

Zhi-Yong Yuan, MD, PhD
Chun-Lei Liu, MD Ma0-Bin Meng, MD, PhD
CyberKnife Center, Department of Radiation Oncology, Tianjin Medical University Cancer Institute & Hospital
Hitting the Target in HER2-Positive Metastatic Colorectal Cancer

i3 Health is pleased to make the speaker slides from this activity available for use as a non-accredited self-study or teaching resource.
This slide deck will share the latest data and strategies for hitting the target in HER2-positive metastatic colorectal cancer. Dr. Christopher Lieu, Associate Professor at the University of Colorado Cancer Center, explores actionable targets to inform personalized care plans, guideline-recommended combination and sequencing strategies, adverse event monitoring and management, and more.
STATEMENT OF NEED
An estimated 153,020 new cases of colorectal cancer (CRC) are diagnosed annually, and 52,550 people die of the disease (Siegel et al, 2023). Approximately 22% of patients present with metastatic disease, which is associated with a dismal 5-year survival rate of 15% (SEER, 2022). Targeting biomarkers is a key strategy for expanding therapeutic options and improving outcomes in metastatic CRC. Human epidermal growth factor receptor 2 (HER2) amplification status and treatments targeting HER2 are some of the most recent additions to the arsenal of targeted therapy for this disease. This activity chaired by Christopher Lieu, MD, Associate Director of Clinical Research at the University of Colorado Cancer Center, will provide expert perspectives and practical guidance on treating HER2-positive metastatic CRC.
TARGET AUDIENCE
Oncologists, gastroenterologists, nurse practitioners, physician assistants, oncology nurses, and other health care professionals involved in the treatment of patients with colorectal cancer (CRC).
LEARNING OBJECTIVES
Upon completion of this activity, participants should be able to
Distinguish actionable targets that can inform personalized care plans in metastatic CRC
Evaluate practice guidelines on treatment combinations and sequences for patients with metastatic CRC
Appraise emerging efficacy and safety data on novel targeted therapies for patients with HER2-positive metastatic CRC
Assess strategies for optimizing the safety and tolerability of novel targeted therapies for HER2-positive metastatic CRC
Breaking the Paradox: Expanding Options and New Questions in HCC Management—M...

Breaking the Paradox: Expanding Options and New Questions in HCC Management—M...PVI, PeerView Institute for Medical Education
Richard S. Finn, MD, Anthony El-Khoueiry, MD, and Josep M. Llovet, MD, PhD, prepared useful practice aids pertaining to hepatocellular carcinoma for this CME activity titled "Breaking the Paradox: Expanding Options and New Questions in HCC Management: Mapping the Pathways to Better Patient Outcomes." For the full presentation, monograph, complete CME information, and to apply for credit, please visit us at http://bit.ly/2HU6L5K. CME credit will be available until February 14, 2020.Breaking New Ground in RCC Management: Expert Guidance on Leveraging Therapeu...

Breaking New Ground in RCC Management: Expert Guidance on Leveraging Therapeu...PVI, PeerView Institute for Medical Education
Chair, Sumanta Kumar Pal, MD, FASCO, David F. McDermott, MD, and Tian Zhang, MD, MHS, prepared useful Practice Aids pertaining to renal cell carcinoma for this CME/MOC activity titled “Breaking New Ground in RCC Management: Expert Guidance on Leveraging Therapeutic Strategies.” For the full presentation, downloadable Practice Aids, and complete CME/MOC information, and to apply for credit, please visit us at http://bit.ly/3AB7i5r. CME/MOC credit will be available until March 16, 2024.Advanced & metastatic bladder cancer - Dr Alok Gupta

This presentation discusses case scenarios of how to manage advanced and metastatic urinary bladder cancer.
Epatocarcinoma: nulla di nuovo sotto il sole - Gastrolearning®

Gastrolearning II modulo/13a lezione
Epatocarcinoma: nulla di nuovo sotto il sole
Relatore: Prof. Massimo Colombo (Milano)
Discussants: Prof. F. Farinati (Padova), Prof.ssa E. Villa (Modena), Prof. A. Grieco (Roma).
Liver

CyberKnife is an option in inoperable or medically not suitable for surgery
& in patient with progression / not tolerating systemic therapy
Updates On Upper Gastrointestinal Malignancies 2015

Updates On Upper Gastrointestinal Malignancies 2015
Tanios Bekaii-Saab, MD
Chief , Section of Gastrointestinal Cancers
Disease Specific Research Group Leader
Professor of Medicine and Pharmacy
OSUCCC- Arthur James Cancer Hospital
Prostate cancer 

Academic Discussion on the management of Prostate cancer by Dr. Abhishek Basu (MD, DNB) for Radiation oncology & Medical oncology residents.
Establishing the Collaborative Benchmark for HCC Care: Critical Discussions B...

Establishing the Collaborative Benchmark for HCC Care: Critical Discussions B...PVI, PeerView Institute for Medical Education
Co-Chairs Riad Salem, MD, MBA, and Mark Yarchoan, MD, discuss liver cancer in this CME/MOC activity titled “Establishing the Collaborative Benchmark for HCC Care: Critical Discussions Between Interventional Radiologists and Oncologists to Maximize Therapeutic Benefit.” For the full presentation, downloadable Practice Aids, and complete CME/MOC information, and to apply for credit, please visit us at https://bit.ly/3IOQvQ6. CME/MOC credit will be available until June 14, 2025.Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...

Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...PVI, PeerView Institute for Medical Education
Co-Chairs, Brett Elicker, MD, and David E. Griffith, MD, ATSF, ACCP, OFRSM, prepared useful Practice Aids pertaining to non-cystic fibrosis bronchiectasis for this CME/MOC activity titled “Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: Ensuring Prompt Diagnosis Through Accurate Interpretation of CT Imaging.” For the full presentation, downloadable Practice Aids, and complete CME/MOC information, and to apply for credit, please visit us at https://bit.ly/48WUULu. CME/MOC credit will be available until June 4, 2025.More Related Content
Similar to It Takes a Team for HCC: Improving Outcomes Through Multidisciplinary Collaboration & Modern Therapeutics
El futuro del tratamiento del cáncer renal metastásico: inmunoterapia y terap...

Ponencia en el primer simposio de la Asociación Colombiana de Hematología y Oncología (ACHO) de cáncer genitourinario, Bogotá, septiembre 23 y 24 de 2016.
Treatment of radioactive iodine-refractory metastatic differentiated thyroid ...

En el marco del Simposio de Cáncer de Cabeza y Cuello y Pulmón de la Asociación Colombiana de Hematología Oncología, ACHO, Bogotá, 28.07.2016
Actualización en el abordaje terapéutico ante un cáncer colorrectal metastásico

Ponencia en el VII Congreso internacional de coloproctología, Bogotá, 18.08.2016. Con énfasis en los estudios recientes en terapia antiangiogénica, y el impacto del lado del primario en el pronóstico (y aspectos predictivos) de la enfermedad metastásica.
Making an Impact in Bladder Cancer Care: Integrating the Latest Evidence and ...

Making an Impact in Bladder Cancer Care: Integrating the Latest Evidence and ...PVI, PeerView Institute for Medical Education
Chair and Presenters Matthew D. Galsky, MD, Shilpa Gupta, MD, and Andrea Necchi, MD, prepared useful Practice Aids pertaining to bladder cancer for this CME/MOC/AAPA/IPCE activity titled “Making an Impact in Bladder Cancer Care: Integrating the Latest Evidence and Modern Therapeutic Advances Across the Disease Continuum.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/AAPA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3QlbwW0. CME/MOC/AAPA/IPCE credit will be available until February 26, 2025.STEREOTACTIC BODY RADIATION THERAPY USING CYBERKNIFE® FOR LIVER METASTASES: A...

Zhi-Yong Yuan, MD, PhD
Chun-Lei Liu, MD Ma0-Bin Meng, MD, PhD
CyberKnife Center, Department of Radiation Oncology, Tianjin Medical University Cancer Institute & Hospital
Hitting the Target in HER2-Positive Metastatic Colorectal Cancer

i3 Health is pleased to make the speaker slides from this activity available for use as a non-accredited self-study or teaching resource.
This slide deck will share the latest data and strategies for hitting the target in HER2-positive metastatic colorectal cancer. Dr. Christopher Lieu, Associate Professor at the University of Colorado Cancer Center, explores actionable targets to inform personalized care plans, guideline-recommended combination and sequencing strategies, adverse event monitoring and management, and more.
STATEMENT OF NEED
An estimated 153,020 new cases of colorectal cancer (CRC) are diagnosed annually, and 52,550 people die of the disease (Siegel et al, 2023). Approximately 22% of patients present with metastatic disease, which is associated with a dismal 5-year survival rate of 15% (SEER, 2022). Targeting biomarkers is a key strategy for expanding therapeutic options and improving outcomes in metastatic CRC. Human epidermal growth factor receptor 2 (HER2) amplification status and treatments targeting HER2 are some of the most recent additions to the arsenal of targeted therapy for this disease. This activity chaired by Christopher Lieu, MD, Associate Director of Clinical Research at the University of Colorado Cancer Center, will provide expert perspectives and practical guidance on treating HER2-positive metastatic CRC.
TARGET AUDIENCE
Oncologists, gastroenterologists, nurse practitioners, physician assistants, oncology nurses, and other health care professionals involved in the treatment of patients with colorectal cancer (CRC).
LEARNING OBJECTIVES
Upon completion of this activity, participants should be able to
Distinguish actionable targets that can inform personalized care plans in metastatic CRC
Evaluate practice guidelines on treatment combinations and sequences for patients with metastatic CRC
Appraise emerging efficacy and safety data on novel targeted therapies for patients with HER2-positive metastatic CRC
Assess strategies for optimizing the safety and tolerability of novel targeted therapies for HER2-positive metastatic CRC
Breaking the Paradox: Expanding Options and New Questions in HCC Management—M...

Breaking the Paradox: Expanding Options and New Questions in HCC Management—M...PVI, PeerView Institute for Medical Education
Richard S. Finn, MD, Anthony El-Khoueiry, MD, and Josep M. Llovet, MD, PhD, prepared useful practice aids pertaining to hepatocellular carcinoma for this CME activity titled "Breaking the Paradox: Expanding Options and New Questions in HCC Management: Mapping the Pathways to Better Patient Outcomes." For the full presentation, monograph, complete CME information, and to apply for credit, please visit us at http://bit.ly/2HU6L5K. CME credit will be available until February 14, 2020.Breaking New Ground in RCC Management: Expert Guidance on Leveraging Therapeu...

Breaking New Ground in RCC Management: Expert Guidance on Leveraging Therapeu...PVI, PeerView Institute for Medical Education
Chair, Sumanta Kumar Pal, MD, FASCO, David F. McDermott, MD, and Tian Zhang, MD, MHS, prepared useful Practice Aids pertaining to renal cell carcinoma for this CME/MOC activity titled “Breaking New Ground in RCC Management: Expert Guidance on Leveraging Therapeutic Strategies.” For the full presentation, downloadable Practice Aids, and complete CME/MOC information, and to apply for credit, please visit us at http://bit.ly/3AB7i5r. CME/MOC credit will be available until March 16, 2024.Advanced & metastatic bladder cancer - Dr Alok Gupta

This presentation discusses case scenarios of how to manage advanced and metastatic urinary bladder cancer.
Epatocarcinoma: nulla di nuovo sotto il sole - Gastrolearning®

Gastrolearning II modulo/13a lezione
Epatocarcinoma: nulla di nuovo sotto il sole
Relatore: Prof. Massimo Colombo (Milano)
Discussants: Prof. F. Farinati (Padova), Prof.ssa E. Villa (Modena), Prof. A. Grieco (Roma).
Liver

CyberKnife is an option in inoperable or medically not suitable for surgery
& in patient with progression / not tolerating systemic therapy
Updates On Upper Gastrointestinal Malignancies 2015

Updates On Upper Gastrointestinal Malignancies 2015
Tanios Bekaii-Saab, MD
Chief , Section of Gastrointestinal Cancers
Disease Specific Research Group Leader
Professor of Medicine and Pharmacy
OSUCCC- Arthur James Cancer Hospital
Prostate cancer 

Academic Discussion on the management of Prostate cancer by Dr. Abhishek Basu (MD, DNB) for Radiation oncology & Medical oncology residents.
Similar to It Takes a Team for HCC: Improving Outcomes Through Multidisciplinary Collaboration & Modern Therapeutics (20)
El futuro del tratamiento del cáncer renal metastásico: inmunoterapia y terap...

El futuro del tratamiento del cáncer renal metastásico: inmunoterapia y terap...
Treatment of radioactive iodine-refractory metastatic differentiated thyroid ...

Treatment of radioactive iodine-refractory metastatic differentiated thyroid ...
Actualización en el abordaje terapéutico ante un cáncer colorrectal metastásico

Actualización en el abordaje terapéutico ante un cáncer colorrectal metastásico
Making an Impact in Bladder Cancer Care: Integrating the Latest Evidence and ...

Making an Impact in Bladder Cancer Care: Integrating the Latest Evidence and ...
STEREOTACTIC BODY RADIATION THERAPY USING CYBERKNIFE® FOR LIVER METASTASES: A...

STEREOTACTIC BODY RADIATION THERAPY USING CYBERKNIFE® FOR LIVER METASTASES: A...
Hitting the Target in HER2-Positive Metastatic Colorectal Cancer

Hitting the Target in HER2-Positive Metastatic Colorectal Cancer
Breaking the Paradox: Expanding Options and New Questions in HCC Management—M...

Breaking the Paradox: Expanding Options and New Questions in HCC Management—M...
Breaking New Ground in RCC Management: Expert Guidance on Leveraging Therapeu...

Breaking New Ground in RCC Management: Expert Guidance on Leveraging Therapeu...
Advanced & metastatic bladder cancer - Dr Alok Gupta

Advanced & metastatic bladder cancer - Dr Alok Gupta
Epatocarcinoma: nulla di nuovo sotto il sole - Gastrolearning®

Epatocarcinoma: nulla di nuovo sotto il sole - Gastrolearning®
Updates On Upper Gastrointestinal Malignancies 2015

Updates On Upper Gastrointestinal Malignancies 2015
management of advanced cervical cancer [Autosaved].pptx![management of advanced cervical cancer [Autosaved].pptx](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
![management of advanced cervical cancer [Autosaved].pptx](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
management of advanced cervical cancer [Autosaved].pptx
More from PVI, PeerView Institute for Medical Education
Establishing the Collaborative Benchmark for HCC Care: Critical Discussions B...

Establishing the Collaborative Benchmark for HCC Care: Critical Discussions B...PVI, PeerView Institute for Medical Education
Co-Chairs Riad Salem, MD, MBA, and Mark Yarchoan, MD, discuss liver cancer in this CME/MOC activity titled “Establishing the Collaborative Benchmark for HCC Care: Critical Discussions Between Interventional Radiologists and Oncologists to Maximize Therapeutic Benefit.” For the full presentation, downloadable Practice Aids, and complete CME/MOC information, and to apply for credit, please visit us at https://bit.ly/3IOQvQ6. CME/MOC credit will be available until June 14, 2025.Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...

Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...PVI, PeerView Institute for Medical Education
Co-Chairs, Brett Elicker, MD, and David E. Griffith, MD, ATSF, ACCP, OFRSM, prepared useful Practice Aids pertaining to non-cystic fibrosis bronchiectasis for this CME/MOC activity titled “Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: Ensuring Prompt Diagnosis Through Accurate Interpretation of CT Imaging.” For the full presentation, downloadable Practice Aids, and complete CME/MOC information, and to apply for credit, please visit us at https://bit.ly/48WUULu. CME/MOC credit will be available until June 4, 2025.Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...

Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...PVI, PeerView Institute for Medical Education
Co-Chairs, Brett Elicker, MD, and David E. Griffith, MD, ATSF, ACCP, OFRSM, discuss non-cystic fibrosis bronchiectasis in this CME/MOC activity titled “Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: Ensuring Prompt Diagnosis Through Accurate Interpretation of CT Imaging.” For the full presentation, downloadable Practice Aids, and complete CME/MOC information, and to apply for credit, please visit us at https://bit.ly/48WUULu. CME/MOC credit will be available until June 4, 2025.Applying Advances in PET Imaging to Facilitate the Early Diagnosis of Alzheim...

Applying Advances in PET Imaging to Facilitate the Early Diagnosis of Alzheim...PVI, PeerView Institute for Medical Education
Co-Chairs, Jonathan E. McConathy, MD, PhD, and Gil Rabinovici, MD, discuss Alzheimer's disease in this CME/AAPA activity titled “Applying Advances in PET Imaging to Facilitate the Early Diagnosis of Alzheimer’s Disease: Preparing Nuclear Medicine and Radiology Specialists for New Diagnostic Workflows.” For the full presentation, downloadable Practice Aids, and complete CME/AAPA information, and to apply for credit, please visit us at https://bit.ly/45RFl6g. CME/AAPA credit will be available until June 15, 2025.A Pharmacist’s Take on Navigating the Expanding Therapeutic Landscape for End...

A Pharmacist’s Take on Navigating the Expanding Therapeutic Landscape for End...PVI, PeerView Institute for Medical Education
Co-Chairs Sarah Hayward, PharmD, BCOP, and Ambar Khan, PharmD, BCOP, discuss endometrial and cervical cancers in this CME/CPE/IPCE activity titled “A Pharmacist’s Take on Navigating the Expanding Therapeutic Landscape for Endometrial and Cervical Cancers: Insights on Coordinating and Delivering Effective Modern Care.” For the full presentation, downloadable Practice Aids, and complete CME/CPE/IPCE information, and to apply for credit, please visit us at https://bit.ly/3wGBPQp. CME/CPE/IPCE credit will be available until May 27, 2025.
“Four-Ward” Progress in NDMM: New Developments With CD38 Antibody Quadruplets

“Four-Ward” Progress in NDMM: New Developments With CD38 Antibody QuadrupletsPVI, PeerView Institute for Medical Education
Co-Chairs, Suzanne Lentzsch, MD, PhD, and Joshua Richter, MD, discuss multiple myeloma in this CME activity titled “‘Four-Ward’ Progress in NDMM: New Developments With CD38 Antibody Quadruplets.” For the full presentation and complete CME information, and to apply for credit, please visit us at https://bit.ly/3x3oWA3. CME credit will be available until May 23, 2025.Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...

Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...PVI, PeerView Institute for Medical Education
Co-Chairs, Jessica Donington, MD, and Jonathan D. Spicer, MD, PhD, FRCSC, prepared useful Practice Aids pertaining to lung cancer for this CME/MOC/AAPA activity titled “Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable NSCLC: A Case Exploration of New Standards and Emerging Approaches.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/AAPA information, and to apply for credit, please visit us at https://bit.ly/3TxdcP5. CME/MOC/AAPA credit will be available until June 7, 2025.Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...

Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...PVI, PeerView Institute for Medical Education
Co-Chairs, Jessica Donington, MD, and Jonathan D. Spicer, MD, PhD, FRCSC, discuss lung cancer in this CME/MOC/AAPA activity titled “Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable NSCLC: A Case Exploration of New Standards and Emerging Approaches.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/AAPA information, and to apply for credit, please visit us at https://bit.ly/3TxdcP5. CME/MOC/AAPA credit will be available until June 7, 2025.On Target: Understanding the Impact of PSMA for Diagnostic and Therapeutic St...

On Target: Understanding the Impact of PSMA for Diagnostic and Therapeutic St...PVI, PeerView Institute for Medical Education
Chair Oliver Sartor, MD, discusses prostate cancer in this CME activity titled “On Target: Understanding the Impact of PSMA for Diagnostic and Therapeutic Strategies in Prostate Cancer.” For the full presentation, downloadable Practice Aids, and complete CME information, and to apply for credit, please visit us at https://bit.ly/49oY4IJ. CME credit will be available until May 23, 2025.Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...

Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...PVI, PeerView Institute for Medical Education
Chair and Presenters, Neal D. Shore, MD, FACS, Ashish M. Kamat, MD, MBBS, and Joshua J. Meeks, MD, PhD, prepared useful Practice Aids pertaining to bladder cancer for this CME/MOC/NCPD/AAPA/IPCE activity titled “Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Implementing Modern Therapeutic Advances Across the Disease Continuum.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/NCPD/AAPA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3PH0RVQ. CME/MOC/NCPD/AAPA/IPCE credit will be available until June 2, 2025.Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...

Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...PVI, PeerView Institute for Medical Education
Chair and Presenters, Neal D. Shore, MD, FACS, Ashish M. Kamat, MD, MBBS, and Joshua J. Meeks, MD, PhD, discuss bladder cancer in this CME/MOC/NCPD/AAPA/IPCE activity titled “Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Implementing Modern Therapeutic Advances Across the Disease Continuum.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/NCPD/AAPA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3PH0RVQ. CME/MOC/NCPD/AAPA/IPCE credit will be available until June 2, 2025.Striking Back at ALL: Achieving Lasting Benefits with Bispecific Antibodies &...

Striking Back at ALL: Achieving Lasting Benefits with Bispecific Antibodies &...PVI, PeerView Institute for Medical Education
Chair, Nicholas J. Short, MD, discusses acute lymphoblastic leukemia in this CME/NCPD/CPE/AAPA/IPCE activity titled “Striking Back at ALL: Achieving Lasting Benefits with Bispecific Antibodies & MRD-Guided Strategies Across Disease Settings.” For the full presentation, downloadable Practice Aids, and complete CME/NCPD/CPE/AAPA/IPCE information, and to apply for credit, please visit us at https://bit.ly/42QsTDT. CME/NCPD/CPE/AAPA/IPCE credit will be available until May 22, 2025.
Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...

Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...PVI, PeerView Institute for Medical Education
Chair, Sharon Cohen, MD, FRCPC, prepared useful Practice Aids pertaining to Alzheimer’s disease for this CME/MOC/AAPA activity titled “Specialty Training for the New Era in Alzheimer’s Disease: Building Skills for Making an Early Diagnosis and Implementing Disease-Modifying Treatment.” For the full presentation, downloadable Practice Aids, monograph, and complete CME/MOC/AAPA information, and to apply for credit, please visit us at https://bit.ly/472bp8g. CME/MOC/AAPA credit will be available until May 20, 2025.
Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...

Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...PVI, PeerView Institute for Medical Education
Chair, Sharon Cohen, MD, FRCPC, discusses Alzheimer’s disease in this CME/MOC/AAPA activity titled “Specialty Training for the New Era in Alzheimer’s Disease: Building Skills for Making an Early Diagnosis and Implementing Disease-Modifying Treatment.” For the full presentation, downloadable Practice Aids, monograph, and complete CME/MOC/AAPA information, and to apply for credit, please visit us at https://bit.ly/472bp8g. CME/MOC/AAPA credit will be available until May 20, 2025.Ten Steps for Highly Successful Myeloma Care: Guidance on the Road to Remissi...

Ten Steps for Highly Successful Myeloma Care: Guidance on the Road to Remissi...PVI, PeerView Institute for Medical Education
Chair and Presenter, Beth Faiman, PhD, MSN, APN-BC, AOCN, BMTCN, FAAN, FAPO, Donna D. Catamero, ANP-BC, OCN, CCRC, and Charise Gleason, MSN, NP-C, AOCNP, discuss multiple myeloma in this CME/MOC/NCPD/ILNA/IPCE activity titled “Ten Steps for Highly Successful Myeloma Care: Guidance on the Road to Remission With Antibodies, BCMA Immunotherapy, and Other Innovations.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/NCPD/ILNA/IPCE information, and to apply for credit, please visit us at https://bit.ly/47mtUnM. CME/MOC/NCPD/ILNA/IPCE credit will be available until May 25, 2025.Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...

Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...PVI, PeerView Institute for Medical Education
Co-Chairs and Presenter Marianne Davies, DNP, ACNP, AOCNP, FAAN, Beth Sandy, MSN, CRNP, FAPO, and Matthew A. Gubens, MD, MS, FASCO, prepared useful Practice Aids pertaining to NSCLC for this CME/MOC/NCPD/ILNA/IPCE activity titled “Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices for Patient Education, irAE Management, and Survivorship Care.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/NCPD/ILNA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3RDokbZ. CME/MOC/NCPD/ILNA/IPCE credit will be available until May 24, 2025.Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...

Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...PVI, PeerView Institute for Medical Education
Co-Chairs and Presenter Marianne Davies, DNP, ACNP, AOCNP, FAAN, Beth Sandy, MSN, CRNP, FAPO, and Matthew A. Gubens, MD, MS, FASCO, discuss NSCLC in this CME/MOC/NCPD/ILNA/IPCE activity titled “Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices for Patient Education, irAE Management, and Survivorship Care.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/NCPD/ILNA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3RDokbZ. CME/MOC/NCPD/ILNA/IPCE credit will be available until May 24, 2025.Modern Team-Based Therapeutic Management for Bladder Cancer Care: Expert Stra...

Modern Team-Based Therapeutic Management for Bladder Cancer Care: Expert Stra...PVI, PeerView Institute for Medical Education
Co-Chairs, Sia Daneshmand, MD, and Matthew D. Galsky, MD, discuss bladder cancer in this CME/MOC/NCPD/AAPA/IPCE activity titled “Modern Team-Based Therapeutic Management for Bladder Cancer Care: Expert Strategies for Integrating the Latest Evidence and Treatment Advances.” For the full presentation, downloadable Practice Aids, and complete CME/MOC/NCPD/AAPA/IPCE information, and to apply for credit, please visit us at https://bit.ly/3OOeYbO. CME/MOC/NCPD/AAPA/IPCE credit will be available until May 13, 2025.Nurses at the Forefront of Maximizing the Potential of TROP2-Targeted Therapy...

Nurses at the Forefront of Maximizing the Potential of TROP2-Targeted Therapy...PVI, PeerView Institute for Medical Education
Chair Jamie Carroll, APRN, CNP, MSN, discusses breast cancer in this NCPD/ILNA/AAPA activity titled “Nurses at the Forefront of Maximizing the Potential of TROP2-Targeted Therapy in TNBC and HR+, HER2- Breast Cancer: Best Practices for Adverse Event Management and Patient Education.” For the full presentation, downloadable Practice Aids, and complete NCPD/ILNA/AAPA information, and to apply for credit, please visit us at https://bit.ly/3SdnvWt. NCPD/ILNA/AAPA credit will be available until May 8, 2025.BTK Inhibition Transforming the Landscape of Chronic Spontaneous Urticaria Tr...

BTK Inhibition Transforming the Landscape of Chronic Spontaneous Urticaria Tr...PVI, PeerView Institute for Medical Education
Chair Jonathan A. Bernstein, MD, discusses chronic spontaneous urticaria in this CME activity titled “BTK Inhibition Transforming the Landscape of Chronic Spontaneous Urticaria Treatment.” For the full presentation, downloadable Practice Aids, and complete CME information, and to apply for credit, please visit us at https://bit.ly/3P0cnvi. CME credit will be available until May 6, 2025.More from PVI, PeerView Institute for Medical Education (20)
Establishing the Collaborative Benchmark for HCC Care: Critical Discussions B...

Establishing the Collaborative Benchmark for HCC Care: Critical Discussions B...
Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...

Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...
Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...

Bridging the Gap to Improved Outcomes in Non-Cystic Fibrosis Bronchiectasis: ...
Applying Advances in PET Imaging to Facilitate the Early Diagnosis of Alzheim...

Applying Advances in PET Imaging to Facilitate the Early Diagnosis of Alzheim...
A Pharmacist’s Take on Navigating the Expanding Therapeutic Landscape for End...

A Pharmacist’s Take on Navigating the Expanding Therapeutic Landscape for End...
“Four-Ward” Progress in NDMM: New Developments With CD38 Antibody Quadruplets

“Four-Ward” Progress in NDMM: New Developments With CD38 Antibody Quadruplets
Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...

Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...
Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...

Transforming Care and Outcomes With Immunotherapy in Stage I-III Resectable N...
On Target: Understanding the Impact of PSMA for Diagnostic and Therapeutic St...

On Target: Understanding the Impact of PSMA for Diagnostic and Therapeutic St...
Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...

Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...
Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...

Harnessing Innovation in Bladder Cancer Care: Strategies for Effectively Impl...
Striking Back at ALL: Achieving Lasting Benefits with Bispecific Antibodies &...

Striking Back at ALL: Achieving Lasting Benefits with Bispecific Antibodies &...
Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...

Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...
Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...

Specialty Training for the New Era in Alzheimer’s Disease: Building Skills fo...
Ten Steps for Highly Successful Myeloma Care: Guidance on the Road to Remissi...

Ten Steps for Highly Successful Myeloma Care: Guidance on the Road to Remissi...
Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...

Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...
Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...

Making Patient-Centric Immunotherapy a Reality in Lung Cancer: Best Practices...
Modern Team-Based Therapeutic Management for Bladder Cancer Care: Expert Stra...

Modern Team-Based Therapeutic Management for Bladder Cancer Care: Expert Stra...
Nurses at the Forefront of Maximizing the Potential of TROP2-Targeted Therapy...

Nurses at the Forefront of Maximizing the Potential of TROP2-Targeted Therapy...
BTK Inhibition Transforming the Landscape of Chronic Spontaneous Urticaria Tr...

BTK Inhibition Transforming the Landscape of Chronic Spontaneous Urticaria Tr...
Recently uploaded
micro teaching on communication m.sc nursing.pdf

Microteaching is a unique model of practice teaching. It is a viable instrument for the. desired change in the teaching behavior or the behavior potential which, in specified types of real. classroom situations, tends to facilitate the achievement of specified types of objectives.
Are There Any Natural Remedies To Treat Syphilis.pdf

Explore natural remedies for syphilis treatment in Singapore. Discover alternative therapies, herbal remedies, and lifestyle changes that may complement conventional treatments. Learn about holistic approaches to managing syphilis symptoms and supporting overall health.
Non-respiratory Functions of the Lungs.pdf

These simplified slides by Dr. Sidra Arshad present an overview of the non-respiratory functions of the respiratory tract.
Learning objectives:
1. Enlist the non-respiratory functions of the respiratory tract
2. Briefly explain how these functions are carried out
3. Discuss the significance of dead space
4. Differentiate between minute ventilation and alveolar ventilation
5. Describe the cough and sneeze reflexes
Study Resources:
1. Chapter 39, Guyton and Hall Textbook of Medical Physiology, 14th edition
2. Chapter 34, Ganong’s Review of Medical Physiology, 26th edition
3. Chapter 17, Human Physiology by Lauralee Sherwood, 9th edition
4. Non-respiratory functions of the lungs https://academic.oup.com/bjaed/article/13/3/98/278874
ANATOMY AND PHYSIOLOGY OF URINARY SYSTEM.pptx

Valuable Content of Human Anatomy and Physiology of Urinary system as per PCI Syllabus for Pharmacy and PharmD Students.
TEST BANK for Operations Management, 14th Edition by William J. Stevenson, Ve...

TEST BANK for Operations Management, 14th Edition by William J. Stevenson, Verified Chapters 1 - 19, Complete Newest Version.pdf
TEST BANK for Operations Management, 14th Edition by William J. Stevenson, Verified Chapters 1 - 19, Complete Newest Version.pdf
Phone Us ❤85270-49040❤ #ℂall #gIRLS In Surat By Surat @ℂall @Girls Hotel With...

Phone Us ❤85270-49040❤ #ℂall #gIRLS In Surat By Surat @ℂall @Girls Hotel With 100% Satisfaction
Ozempic: Preoperative Management of Patients on GLP-1 Receptor Agonists 

Preoperative Management of Patients on GLP-1 Receptor Agonists like Ozempic and Semiglutide
ASA GUIDELINE
NYSORA Guideline
2 Case Reports of Gastric Ultrasound
Hemodialysis: Chapter 3, Dialysis Water Unit - Dr.Gawad

- Video recording of this lecture in English language: https://youtu.be/lK81BzxMqdo
- Video recording of this lecture in Arabic language: https://youtu.be/Ve4P0COk9OI
- Link to download the book free: https://nephrotube.blogspot.com/p/nephrotube-nephrology-books.html
- Link to NephroTube website: www.NephroTube.com
- Link to NephroTube social media accounts: https://nephrotube.blogspot.com/p/join-nephrotube-on-social-media.html
The hemodynamic and autonomic determinants of elevated blood pressure in obes...

Christopher Hearon
The University of Texas Southwestern Medical Center
The POPPY STUDY (Preconception to post-partum cardiovascular function in prim...

Carmel McEniery
University of Cambridge
Flu Vaccine Alert in Bangalore Karnataka

As flu season approaches, health officials in Bangalore, Karnataka, are urging residents to get their flu vaccinations. The seasonal flu, while common, can lead to severe health complications, particularly for vulnerable populations such as young children, the elderly, and those with underlying health conditions.
Dr. Vidisha Kumari, a leading epidemiologist in Bangalore, emphasizes the importance of getting vaccinated. "The flu vaccine is our best defense against the influenza virus. It not only protects individuals but also helps prevent the spread of the virus in our communities," he says.
This year, the flu season is expected to coincide with a potential increase in other respiratory illnesses. The Karnataka Health Department has launched an awareness campaign highlighting the significance of flu vaccinations. They have set up multiple vaccination centers across Bangalore, making it convenient for residents to receive their shots.
To encourage widespread vaccination, the government is also collaborating with local schools, workplaces, and community centers to facilitate vaccination drives. Special attention is being given to ensuring that the vaccine is accessible to all, including marginalized communities who may have limited access to healthcare.
Residents are reminded that the flu vaccine is safe and effective. Common side effects are mild and may include soreness at the injection site, mild fever, or muscle aches. These side effects are generally short-lived and far less severe than the flu itself.
Healthcare providers are also stressing the importance of continuing COVID-19 precautions. Wearing masks, practicing good hand hygiene, and maintaining social distancing are still crucial, especially in crowded places.
Protect yourself and your loved ones by getting vaccinated. Together, we can help keep Bangalore healthy and safe this flu season. For more information on vaccination centers and schedules, residents can visit the Karnataka Health Department’s official website or follow their social media pages.
Stay informed, stay safe, and get your flu shot today!
Ocular injury ppt Upendra pal optometrist upums saifai etawah

This ppt are composed by upendra pal to provide help future optometrist of india
MANAGEMENT OF ATRIOVENTRICULAR CONDUCTION BLOCK.pdf

Cardiac conduction defects can occur due to various causes.
Atrioventricular conduction blocks ( AV blocks ) are classified into 3 types.
This document describes the acute management of AV block.
Prix Galien International 2024 Forum Program

June 20, 2024, Prix Galien International and Jerusalem Ethics Forum in ROME. Detailed agenda including panels:
- ADVANCES IN CARDIOLOGY: A NEW PARADIGM IS COMING
- WOMEN’S HEALTH: FERTILITY PRESERVATION
- WHAT’S NEW IN THE TREATMENT OF INFECTIOUS,
ONCOLOGICAL AND INFLAMMATORY SKIN DISEASES?
- ARTIFICIAL INTELLIGENCE AND ETHICS
- GENE THERAPY
- BEYOND BORDERS: GLOBAL INITIATIVES FOR DEMOCRATIZING LIFE SCIENCE TECHNOLOGIES AND PROMOTING ACCESS TO HEALTHCARE
- ETHICAL CHALLENGES IN LIFE SCIENCES
- Prix Galien International Awards Ceremony
New Directions in Targeted Therapeutic Approaches for Older Adults With Mantl...

i3 Health is pleased to make the speaker slides from this activity available for use as a non-accredited self-study or teaching resource.
This slide deck presented by Dr. Kami Maddocks, Professor-Clinical in the Division of Hematology and
Associate Division Director for Ambulatory Operations
The Ohio State University Comprehensive Cancer Center, will provide insight into new directions in targeted therapeutic approaches for older adults with mantle cell lymphoma.
STATEMENT OF NEED
Mantle cell lymphoma (MCL) is a rare, aggressive B-cell non-Hodgkin lymphoma (NHL) accounting for 5% to 7% of all lymphomas. Its prognosis ranges from indolent disease that does not require treatment for years to very aggressive disease, which is associated with poor survival (Silkenstedt et al, 2021). Typically, MCL is diagnosed at advanced stage and in older patients who cannot tolerate intensive therapy (NCCN, 2022). Although recent advances have slightly increased remission rates, recurrence and relapse remain very common, leading to a median overall survival between 3 and 6 years (LLS, 2021). Though there are several effective options, progress is still needed towards establishing an accepted frontline approach for MCL (Castellino et al, 2022). Treatment selection and management of MCL are complicated by the heterogeneity of prognosis, advanced age and comorbidities of patients, and lack of an established standard approach for treatment, making it vital that clinicians be familiar with the latest research and advances in this area. In this activity chaired by Michael Wang, MD, Professor in the Department of Lymphoma & Myeloma at MD Anderson Cancer Center, expert faculty will discuss prognostic factors informing treatment, the promising results of recent trials in new therapeutic approaches, and the implications of treatment resistance in therapeutic selection for MCL.
Target Audience
Hematology/oncology fellows, attending faculty, and other health care professionals involved in the treatment of patients with mantle cell lymphoma (MCL).
Learning Objectives
1.) Identify clinical and biological prognostic factors that can guide treatment decision making for older adults with MCL
2.) Evaluate emerging data on targeted therapeutic approaches for treatment-naive and relapsed/refractory MCL and their applicability to older adults
3.) Assess mechanisms of resistance to targeted therapies for MCL and their implications for treatment selection
Recently uploaded (20)
Are There Any Natural Remedies To Treat Syphilis.pdf

Are There Any Natural Remedies To Treat Syphilis.pdf
TEST BANK for Operations Management, 14th Edition by William J. Stevenson, Ve...

TEST BANK for Operations Management, 14th Edition by William J. Stevenson, Ve...
Phone Us ❤85270-49040❤ #ℂall #gIRLS In Surat By Surat @ℂall @Girls Hotel With...

Phone Us ❤85270-49040❤ #ℂall #gIRLS In Surat By Surat @ℂall @Girls Hotel With...
Ozempic: Preoperative Management of Patients on GLP-1 Receptor Agonists 

Ozempic: Preoperative Management of Patients on GLP-1 Receptor Agonists
Hemodialysis: Chapter 3, Dialysis Water Unit - Dr.Gawad

Hemodialysis: Chapter 3, Dialysis Water Unit - Dr.Gawad
The hemodynamic and autonomic determinants of elevated blood pressure in obes...

The hemodynamic and autonomic determinants of elevated blood pressure in obes...
The POPPY STUDY (Preconception to post-partum cardiovascular function in prim...

The POPPY STUDY (Preconception to post-partum cardiovascular function in prim...
Triangles of Neck and Clinical Correlation by Dr. RIG.pptx

Triangles of Neck and Clinical Correlation by Dr. RIG.pptx
Ocular injury ppt Upendra pal optometrist upums saifai etawah

Ocular injury ppt Upendra pal optometrist upums saifai etawah
MANAGEMENT OF ATRIOVENTRICULAR CONDUCTION BLOCK.pdf

MANAGEMENT OF ATRIOVENTRICULAR CONDUCTION BLOCK.pdf
New Directions in Targeted Therapeutic Approaches for Older Adults With Mantl...

New Directions in Targeted Therapeutic Approaches for Older Adults With Mantl...
Maxilla, Mandible & Hyoid Bone & Clinical Correlations by Dr. RIG.pptx

Maxilla, Mandible & Hyoid Bone & Clinical Correlations by Dr. RIG.pptx
It Takes a Team for HCC: Improving Outcomes Through Multidisciplinary Collaboration & Modern Therapeutics
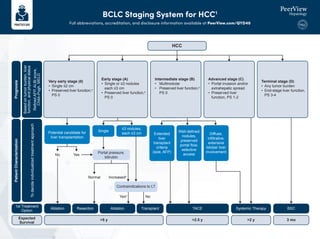
- 1. BCLC Staging System for HCC1 Full abbreviations, accreditation, and disclosure information available at PeerView.com/QYD40 Yes No Normal Increasedb HCC Very early stage (0) • Single ≤2 cm • Preserved liver function,a PS 0 Potential candidate for liver transplantation Single Contraindications to LT Yesb 1st Treatment Option Ablation Resection Ablation Transplant TACE Systemic Therapy BSC 3 mo >2 y >2.5 y >5 y Expected Survival No ≤3 nodules, each ≤3 cm Portal pressure, bilirubin Extended liver transplant criteria (size, AFP) Well-defined nodules, preserved portal flow, selective access Diffuse, infiltrative, extensive bilobar liver involvement Early stage (A) • Single or ≤3 nodules each ≤3 cm • Preserved liver function,a PS 0 Intermediate stage (B) • Multinodular • Preserved liver function,a PS 0 Advanced stage (C) • Portal invasion and/or extrahepatic spread • Preserved liver function, PS 1-2 Terminal stage (D) • Any tumor burden • End-stage liver function, PS 3-4 To decide individualized treatment approach Based on tumor burden, liver function, and physical status Refined AFP, ALBI score, Child–Pugh, MELD Prognosis Patient Characterization
- 2. a Except for those with tumor burden acceptable for transplant. b Resection may be considered for single peripheral HCC with adequate remnant liver volume. 1. Reig M et al. J Hepatol. 2022;76:681-693. BCLC Staging System for HCC1 Full abbreviations, accreditation, and disclosure information available at PeerView.com/QYD40 1st Treatment Option Ablation Resection Ablation Transplant TACE Successful downstaging Not feasible or failure TACE Radioembolization (only for single lesion ≤8 cm) Systemic Therapy BSC 3 mo >2 y >2.5 y >5 y Not feasible or failure Expected Survival Treatment Stage Migration primes lower priority options due to non–liver-related clinical profile (age, comorbidities, patient values, and availability) Clinical Decision-Making 1st Line • Atezolizumab–bevacizumab/durvalumab–tremelimumab If not feasible, sorafenib or lenvatinib or durvalumab 3rd Line • Cabozantinib 2nd Line • Post sorafenib Regorafenib (sorafenib-tolerant) Cabozantinib Ramucirumab (AFP ≥400 ng/mL) Clinical trials Not feasible Alternative sequences could be considered but they have not been proved • Post atezolizumab-bevacizumab • Post durvalumab-tremelimumab • Post lenvatinib Not feasible Not feasible
- 3. New Concepts and Emerging Modalities in HCC1-3 Full abbreviations, accreditation, and disclosure information available at PeerView.com/QYD40 Tumor Treating Fields (TTFields) Are an Antimitotic Therapy New cell TTFields • Living cells contain ions and polar or charged molecules • Charged particles and dipoles can be influenced by electric fields • TTFields are alternating electric fields that can disrupt charged particles during mitosis, which may lead to cell death in dividing cancer cells but spare quiescent cells G0 Resting state G2 Premitosis G1 Interphase initiation S DNA synthesis M Mitosis and cytokinesis New cell
- 4. New Concepts and Emerging Modalities in HCC1-3 Full abbreviations, accreditation, and disclosure information available at PeerView.com/QYD40 1. Gutin PH et al. Am Soc Clin Oncol Educ Book. 2012;32:126-131. 2. Kirson ED et al. Proc Natl Acad Sci USA. 2007;104:10152-10157. 3. https://www.cancernetwork.com/view/novottf-200t-delivery-system-given-a-breakthrough-designation-by-the-fda-for-advanced-liver-cancer. Non-Invasive, Wearable Device Targeting the Liver Phase 2 HEPANOVA Trial TTFields (150 kHz) Concurrent With First-Line Sorafenib for Advanced/Unresectable HCC • Results showed response greater than historical control • Phase 3 RCT being planned with new SOC: atezolizumab + bevacizumab • TTFields + atezolizumab + bevacizumab granted FDA breakthrough therapy designation in advanced HCC3 HCC N = 25 Until PD per RECIST in the liver Screening and baseline evaluation TTFields + daily sorafenib CT/MRI scan every 12 wk until PD Survival follow-up • Primary endpoint: overall radiological response rate • Secondary endpoints: in-field control rate, OS • 27 patients enrolled • 52% Child-Turcotte-Pugh: 7-8 • Median duration of therapy: 9 weeks
- 5. Considerations for Selecting and Sequencing Treatments for Advanced HCC Full abbreviations, accreditation, and disclosure information available at PeerView.com/QYD40 Current NCCN Guidelines1 All recommendations are category 2A unless otherwise noted First-Line Systemic Therapy Subsequent-Line Therapy if Disease Progression Preferred Regimens • Atezolizumab + bevacizumab (Child–Pugh A only) (category 1) Other Recommended Regimens • Sorafenib (Child–Pugh A [category 1] or B7) • Lenvatinib (Child–Pugh A only) (category 1) • Durvalumab • Pembrolizumab (category 2B) Useful in Certain Circumstances • Nivolumab (if ineligible for TKls or other anti-angiogenics) (Child–Pugh A or B) (category 2B) Options • Regorafenib (Child–Pugh A only) (category 1) • Cabozantinib (Child–Pugh A only) (category 1) • Ramucirumab (AFP ≥400 ng/mL and Child–Pugh A only) (category 1) • Lenvatinib (Child–Pugh A only) • Sorafenib (Child–Pugh A or B7) Other Recommended Regimens • Nivolumab + ipilimumab (Child–Pugh A only) • Pembrolizumab (Child–Pugh A only) (category 2B) Useful in Certain Circumstances • Nivolumab (Child–Pugh B only) (category 2B) • Dostarlimab (for MSI-H/dMMR tumors) (category 2B) • For RET gene fusion–positive tumors: – Selpercatinib (category 2B)
- 6. Considerations for Selecting and Sequencing Treatments for Advanced HCC Full abbreviations, accreditation, and disclosure information available at PeerView.com/QYD40 Second-Line Treatment and Beyond Drug Supporting Evidence First-Line Treatment Dosing Indication Atezolizumab + bevacizumab3 IMbrave150 Atezolizumab 840 mg every 2 weeks, 1,200 mg every 3 weeks, or 1,680 mg every 4 weeks, administered prior to bevacizumab when given on the same day; bevacizumab 15 mg/kg every 3 weeks Sorafenib5-7 SHARP 400 mg orally twice daily without food Treatment of patients with unresectable HCC HIMALAYA Adult patients with unresectable HCC Durvalumab+ tremelimumab4 Lenvatinib6 12 mg orally once daily for patients ≥60 kg or 8 mg orally once daily for patients <60 kg REFLECT First-line treatment of patients with unresectable HCC Regorafenib7 RESORCE 160 mg orally once daily for the first 21 days of each 28-day cycle after a low-fat meal Treatment of patients with HCC who have been previously treated with sorafenib Cabozantinib8 CELESTIAL Treatment of patients with HCC who have been previously treated with sorafenib Ramucirumab9 REACH-2 8 mg/kg every 2 weeks IV administered over 60 minutes; if the first infusion is tolerated, all subsequent infusions may be administered over 30 minutes Treament of HCC in patients who have an AFP ≥400 ng/mL and have been treated with sorafenib FDA-Approved Systemic Therapy in HCC2 Treatment of patients with unresectable or metastatic HCC who have not received prior systemic therapy For patients weighing ≥30 kg: durvalumab 1,500 mg + tremelimumab 300 mg as a single dose at cycle 1/day 1, followed by durvalumab 1,500 mg as a single agent every 4 weeks; for patients weighing <30 kg: durvalumab 20 mg/kg + tremelimumab 4 mg/kg as a single dose at cycle 1/day 1, followed by durvalumab 20 mg/kg as a single agent every 4 weeks 60 mg orally once daily; 40 mg orally once daily in pediatric patients with BSA <1.2 m2 ; administer at least 1 hour before or at least 2 hours after eating
- 7. Considerations for Selecting and Sequencing Treatments for Advanced HCC Full abbreviations, accreditation, and disclosure information available at PeerView.com/QYD40 1. National Comprehensive Cancer Network (NCCN) Clinical Practice Guidelines in Oncology. Hepatobiliary Cancers. Version 3.2022. https://www.nccn.org/professionals/physician_gls/pdf/hepatobiliary.pdf. 2. https://www.accessdata.fda.gov/. 3. Finn RS et al. N Engl J Med. 2020;382:1894-1905. 4. Abou-Alfa G et al. 2022 American Society of Clinical Oncology Gastrointestinal Cancers Symposium (ASCO GI 2022). Abstract 379. 5. Llovet JM et al. N Engl J Med. 2008;359:378-390. 6. Kudo M et al. Lancet. 2018;391:1163-1173. 7. Bruix J et al. Lancet. 2017;389:56-66. 8. Abou-Alfa G et al. N Engl J Med. 2018;379:54-63. 9. Zhu AX et al. Lancet Oncol. 2019;20:282-296. 10. El-Khoueiry AB et al. 13th Annual Conference of the International Liver Cancer Association (ILCA 2019). Abstract O-13. 11. Yau T et al. 2019 American Society of Clinical Oncology Annual Meeting (ASCO 2019). Abstract 4012. 12. Keytruda (pembrolizumab) Prescribing Information. https://www.accessdata.fda.gov/drugsatfda_docs/label/2022/125514s133lbl.pdf. Drug Supporting Evidence Second-Line Treatment and Beyond Dosing Indication Nivolumab 1 mg/kg followed by ipilimumab 3 mg/kg on the same day every 3 weeks for 4 doses, then nivolumab 240 mg every 2 weeks or 480 mg every 4 weeks Nivolumab + ipilimumab10,11 Pembrolizumab12 KEYNOTE-224 200 mg every 3 weeks or 400 mg every 6 weeks CheckMate -040 Treatment of patients with HCC who have been previously treated with sorafenib Treatment of patients with HCC who have been previously treated with sorafenib
