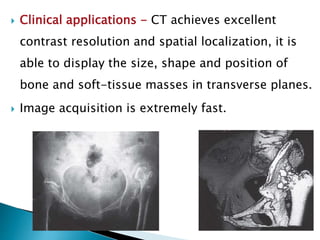
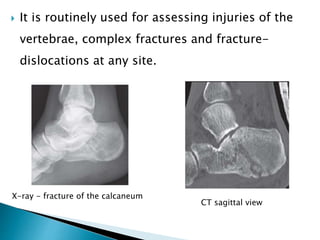
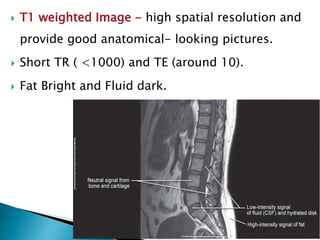
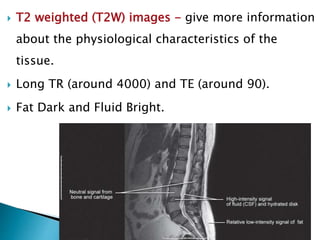
The document outlines various imaging modalities essential for diagnosing orthopedic conditions, starting from X-rays discovered in 1895 to advanced techniques like MRI and CT. It discusses the characteristics, benefits, and limitations of each imaging method, including sensitivity, specificity, and the types of tissue evaluated. Furthermore, it highlights specific applications for imaging in assessing injuries, fractures, and joint diseases, while also addressing safety concerns related to ionizing radiation.