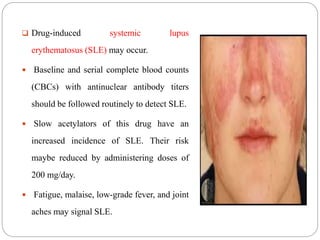
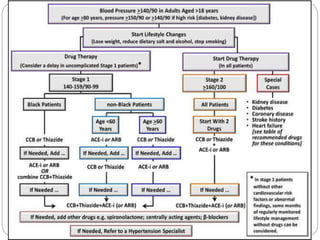
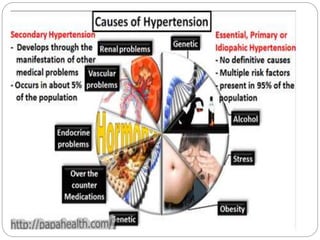
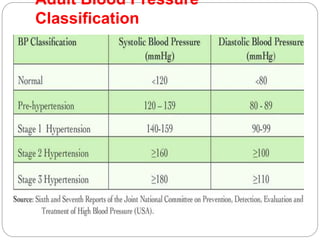
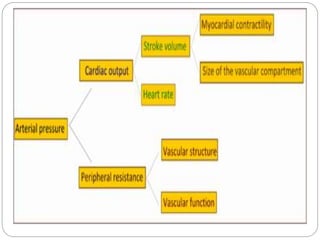
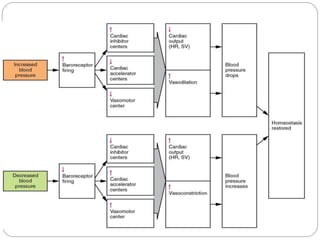
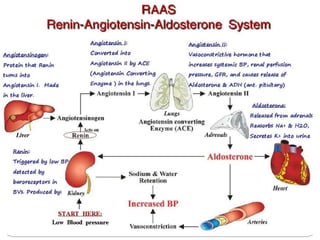
This document provides information on hypertension (high blood pressure), including its types, classification, pathophysiology, diagnosis, and treatment. It discusses the mosaic theory of hypertension and factors involved in fluid volume regulation. It outlines the clinical presentation of hypertension and diagnostic evaluation. Finally, it provides details on non-pharmacological and pharmacological treatment approaches for hypertension, describing specific drug classes like diuretics, beta-blockers, ACE inhibitors, and others.







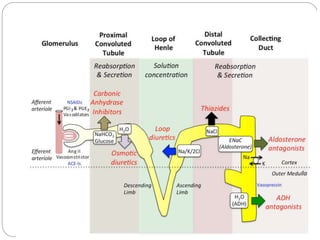
![DIURETICS
Thiazide diuretics
JNC-7 recommends initiating therapy with a low dose (12.5 mg)
of hydrochlorothiazide [Microzide®]),
increasing the dose if necessary, and not exceeding a dose of 50
mg of hydrochlorothiazide or its equivalent.](https://image.slidesharecdn.com/hypertensionppt-191123052153/85/Hypertension-ppt-19-320.jpg)