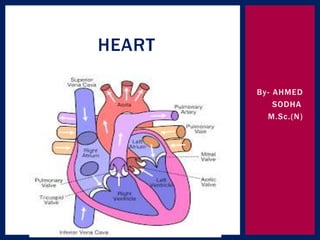
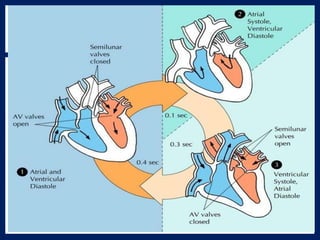
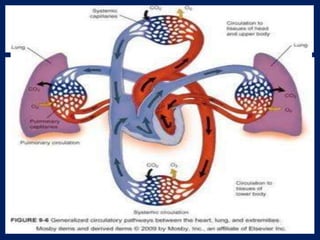
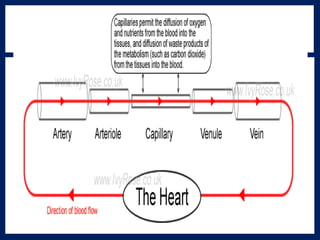
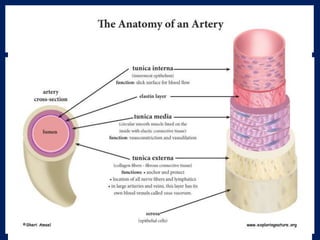
The document provides information on the anatomy and physiology of the human heart. It discusses the heart's location in the thoracic cavity, its structure which includes three layers (pericardium, myocardium, and endocardium), and its four chambers. It describes the flow of blood through the heart via the superior vena cava, inferior vena cava, pulmonary arteries, and aorta. It also covers the heart's conductive system, including the sinoatrial node, atrioventricular node, and Purkinje fibers. Finally, it briefly discusses cardiac output, blood pressure regulation, and the pulmonary and systemic circulations.