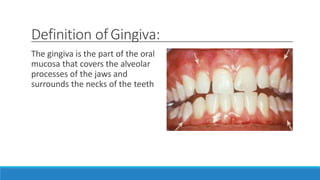
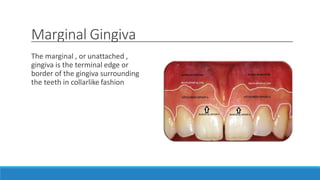
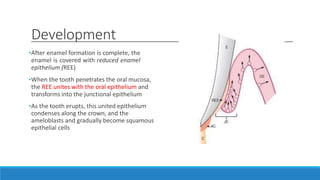
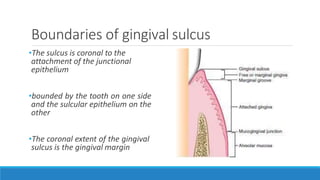
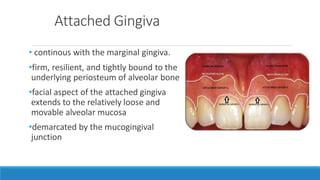
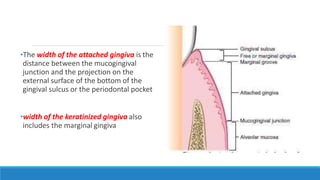
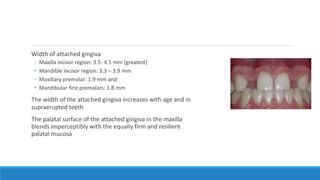
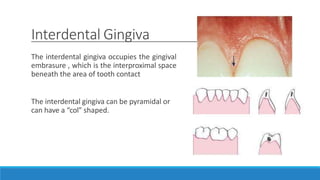
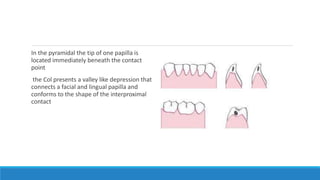
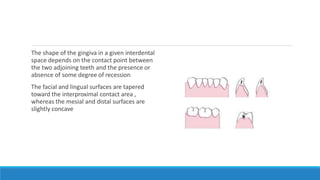
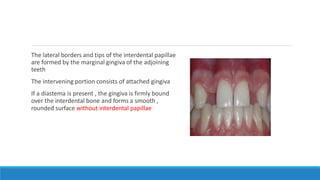
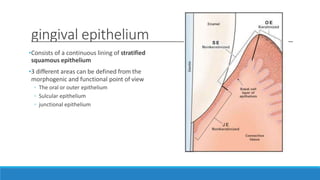
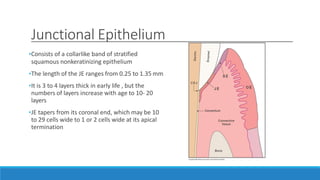
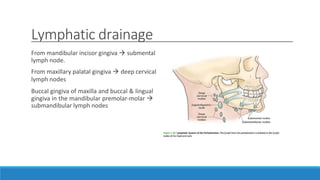
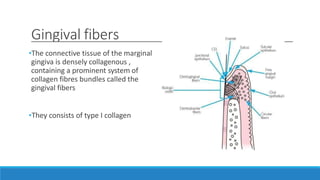
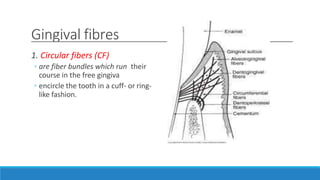
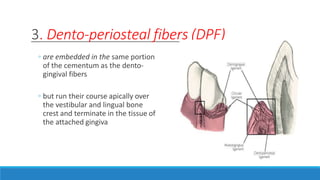
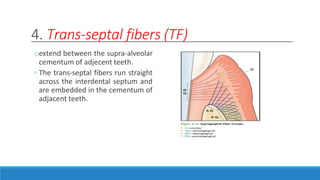
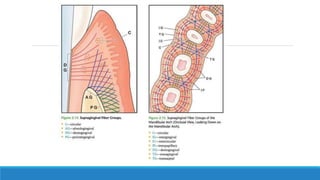
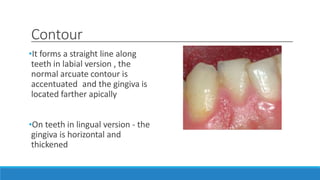
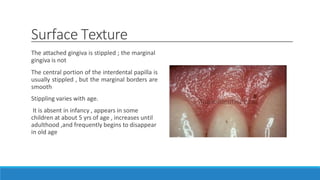
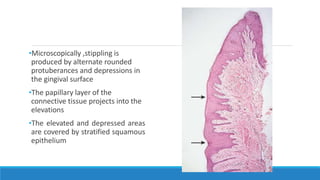
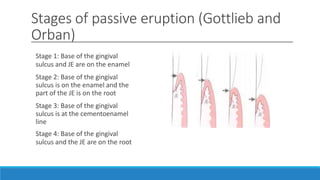
This document discusses the anatomy, histology, and biology of the gingiva. It defines the gingiva and divides it anatomically into the marginal, attached, and interdental gingiva. Microscopically, the gingiva consists of stratified squamous epithelium and underlying connective tissue. The document describes the development, microscopic features including the different areas of gingival epithelium, gingival fibers, blood supply, lymphatics and nerves of the gingiva. It correlates the clinical features of color, size, and contour to the microscopic structure of the gingiva.