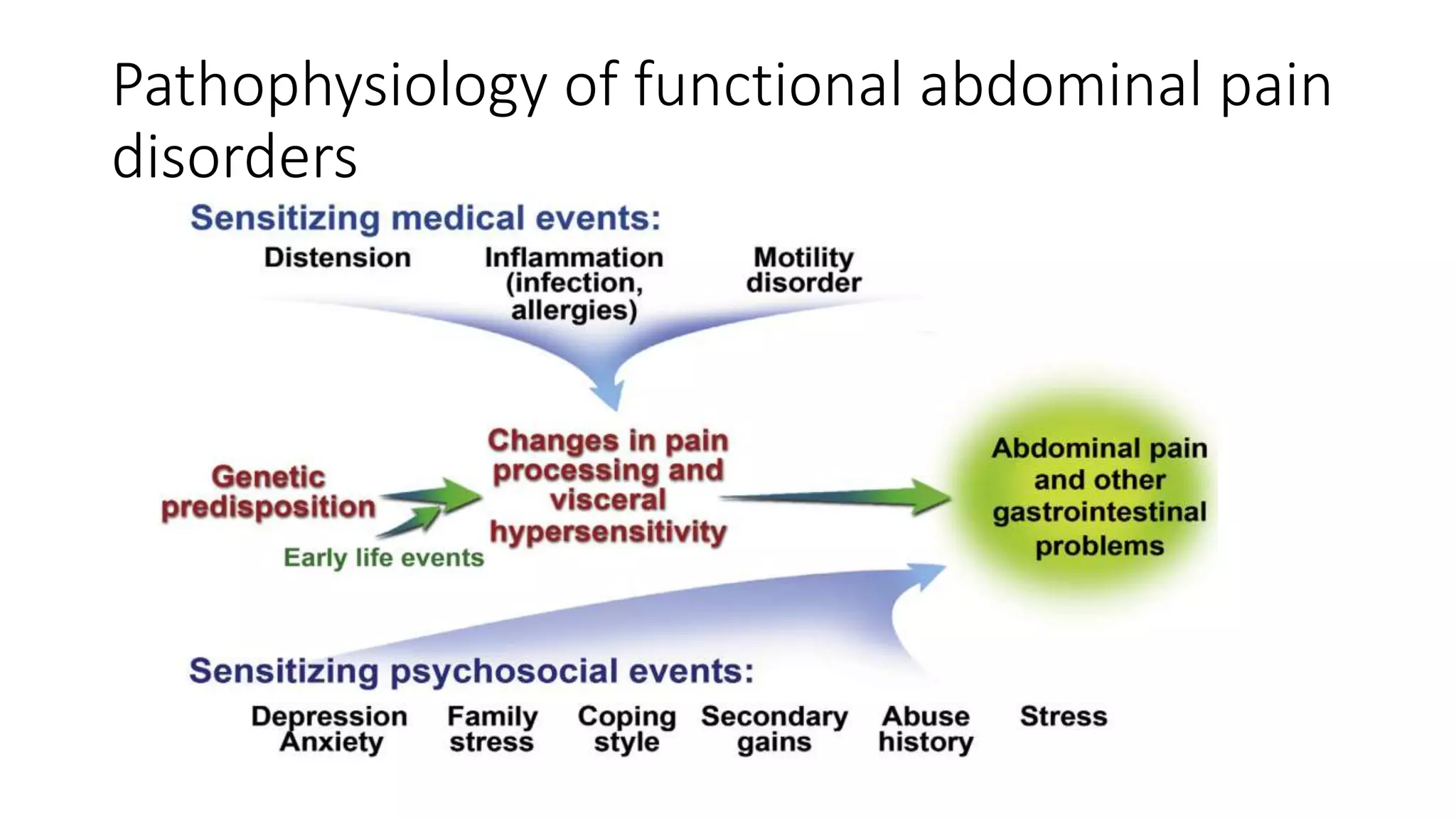
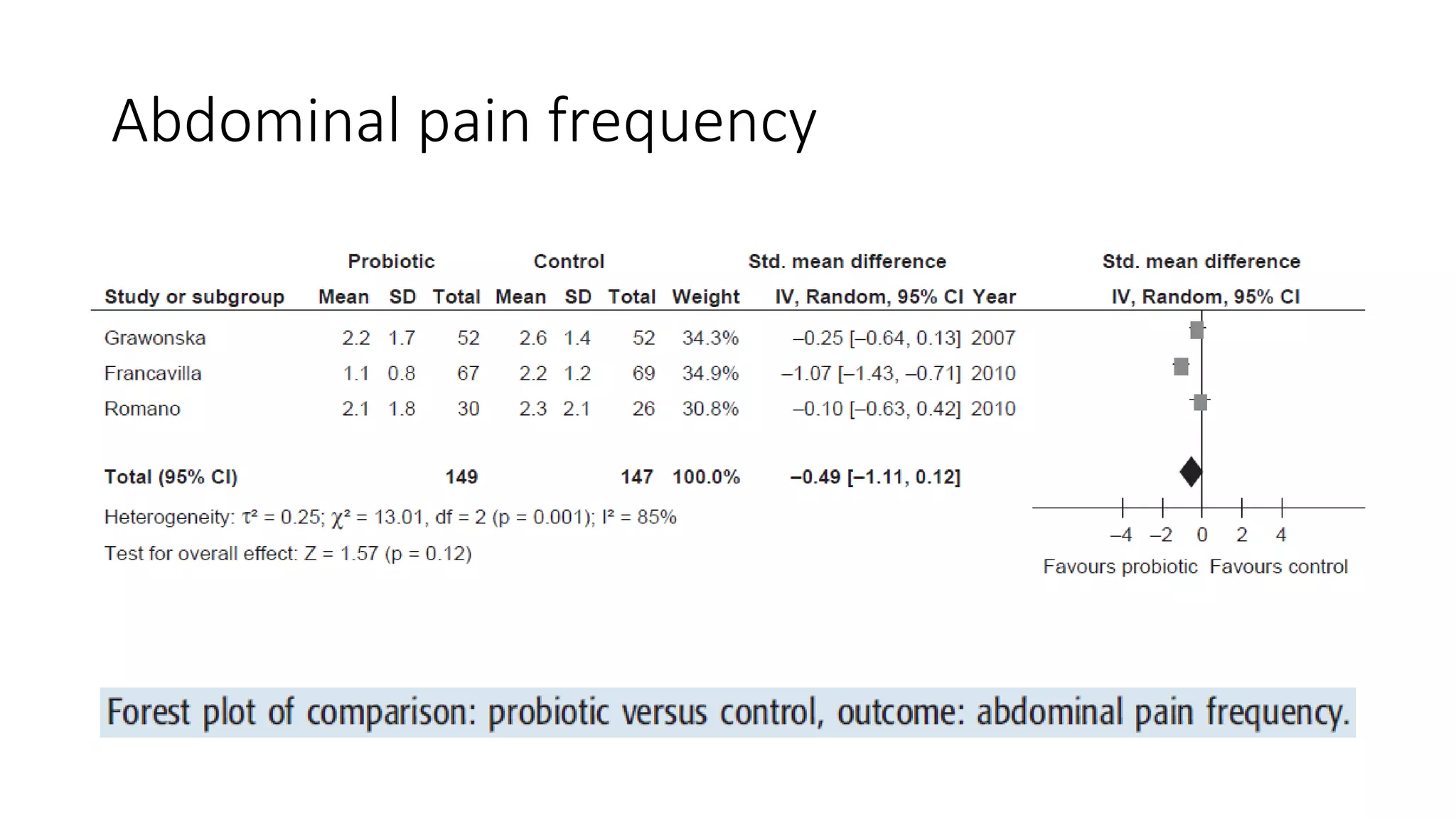
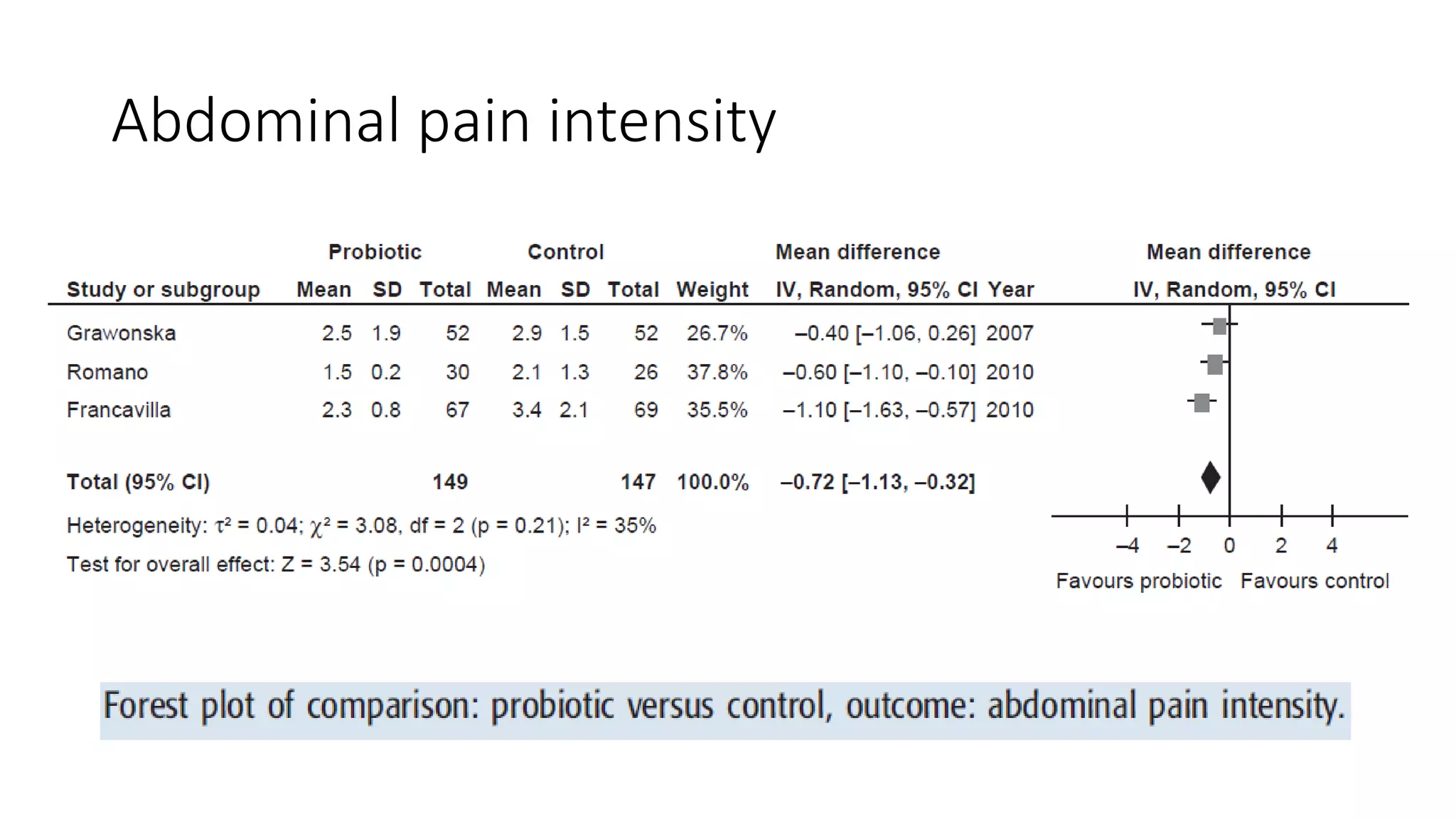
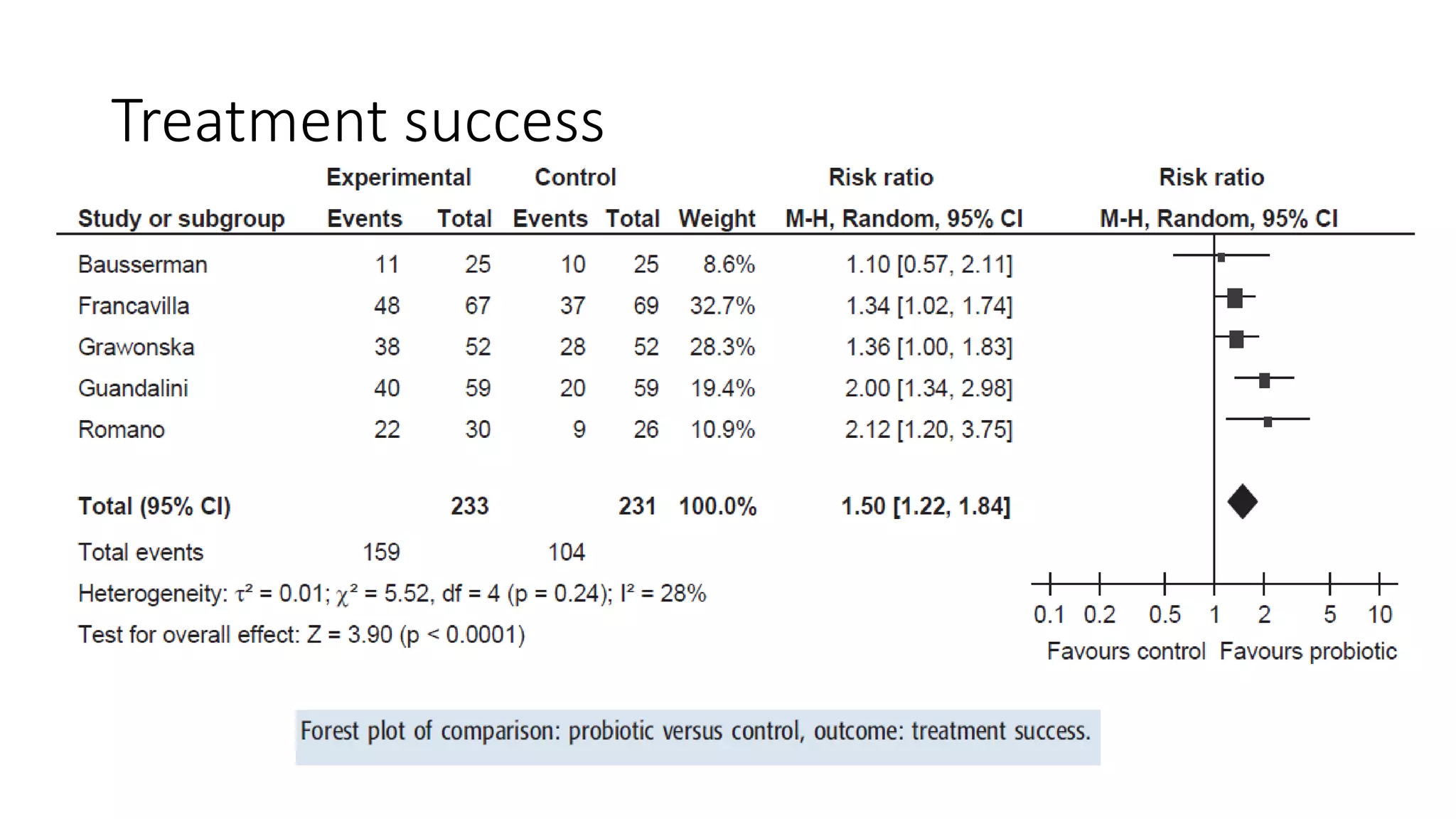
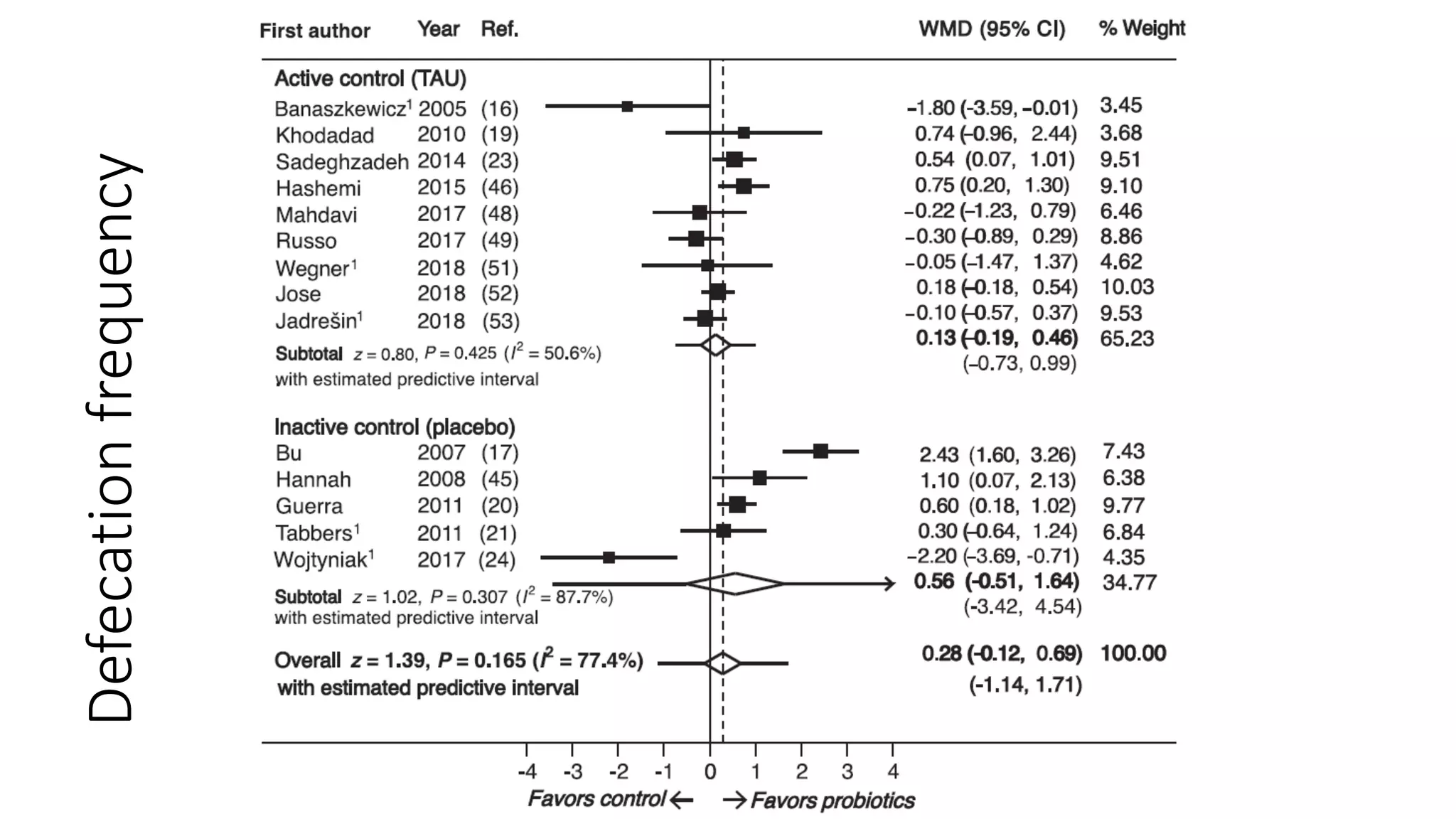
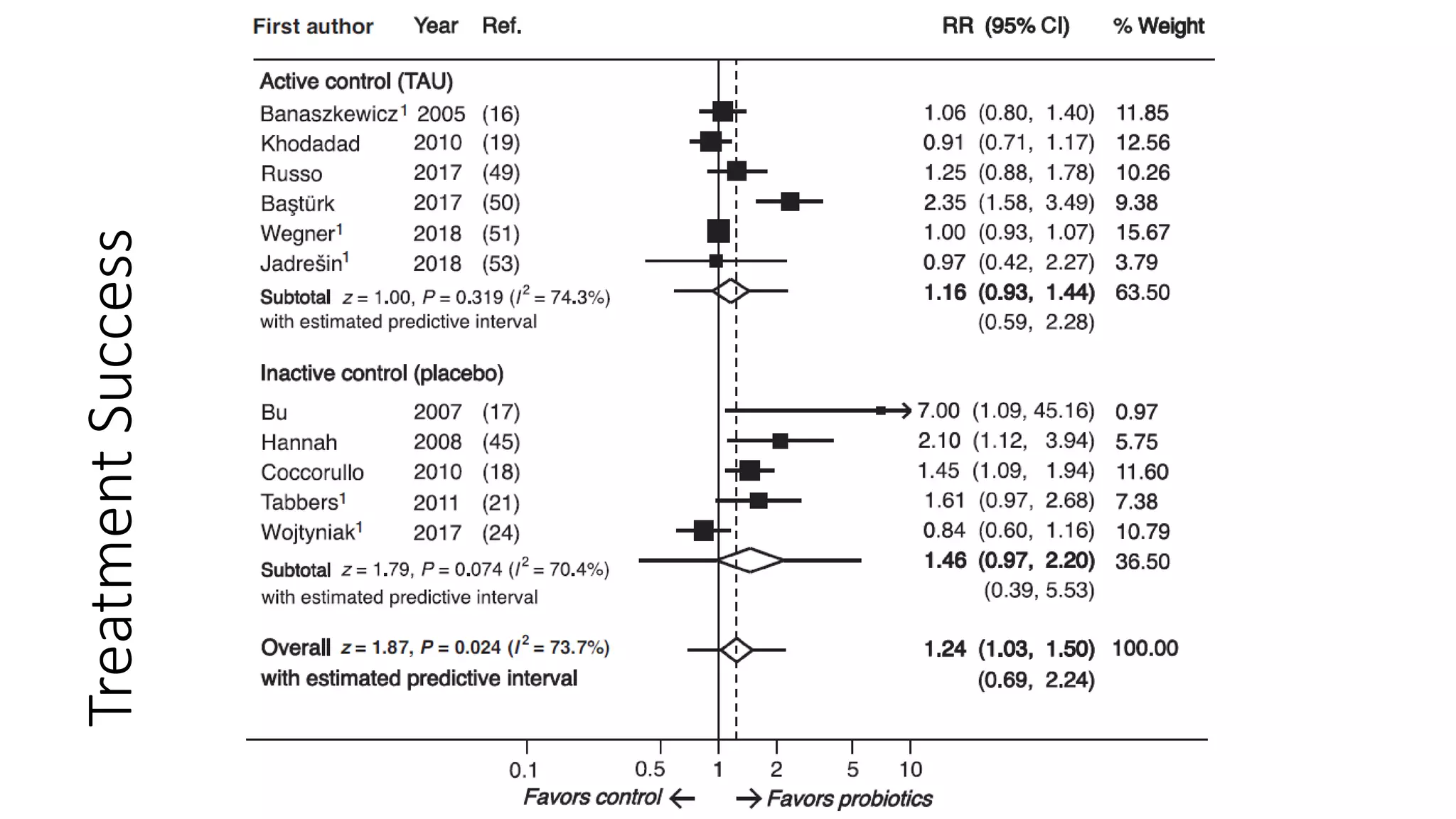
The document discusses functional gastrointestinal disorders (FGIDs) in children, providing updated classifications, diagnostic criteria, and treatment approaches for various disorders including functional nausea, vomiting, abdominal pain, and defecation issues. It highlights changes in diagnostic criteria from the Rome IV guidelines and emphasizes the importance of a thorough clinical evaluation and psychological considerations in treatment. The recommended management strategies include medication options, behavioral therapies, and lifestyle modifications tailored to specific FGIDs.