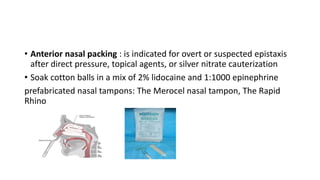
Epistaxis, or nosebleed, is bleeding from the nose that can occur from rupture of small blood vessels in the nasal cavity. Most nosebleeds are minor and self-limiting, but some may be recurrent or require medical attention. The majority occur in the front of the nose due to rupture of vessels in an area called Little's area or the Kiesselbach's plexus. Causes can include local trauma, medications, inflammation, or systemic issues. Treatment depends on severity but may involve direct pressure, cauterization, nasal packing, or arterial ligation for severe cases. Prevention focuses on avoiding dry environments and minor trauma to the inside of the nose.