This study evaluated the intermediate and long-term results of femoral neck lengthening (Morscher osteotomy) in 18 patients (20 hips) with a median follow-up of 7 years. Postoperatively, the Trendelenburg test was negative in most patients and the median Harris Hip Score improved significantly. Radiographic examination found progression of osteoarthritis in 3 patients, while one operation failed and required total hip replacement after 4 years and two others required it at 10 years. The procedure successfully reduced leg length discrepancy in most patients. The study concluded that Morscher osteotomy can effectively treat patients with short femoral neck and overgrown greater trochanter with a positive Trendelenburg test and mild leg length
![Intermediate to Long-Term Results of Femoral Neck
Lengthening (Morscher Osteotomy)
Mark Eidelman, MD,* Doron Keshet, MD,w Scott Nelson, MD,z and Noam Bor, MDy
Background: Femoral neck lengthening and transfer of the
greater trochanter were introduced by Morscher as treatment
for patients with coxa breva and overgrowth of the greater
trochanter. In this study we evaluated intermediate and long-
term results of this operation.
Methods: We reviewed clinical and radiographic results of 18
patients (20 hips) who were treated by Morscher osteotomy. Ten
patients had Perthes disease, 4 had developmental dysplasia of
the hip, and 4 had avascular necrosis of the hip. The median age
at surgery was 16 years [interquartile range (IQR): 14 to 17.5].
The median follow-up period was 7 years (IQR: 4.5 to 10). All
patients were evaluated clinically by means of Harris Hip Score
(HHS) before and after surgery.
Results: Preoperative clinical examination revealed that all pa-
tients had a limp and a positive Trendelenburg test. Median
HHS was 72.5 (IQR: 69 to 83). Postoperatively, the Trende-
lenburg test was negative in 14 hips and positive in 6 hips.
Postoperative median HHS was 94.5 (IQR: 89 to 96). Radio-
graphic examination showed progression of osteoarthritis in 3
patients. One operation failed and was converted to total ar-
throplasty (total hip replacement) after 4 years. Two hips re-
quired total hip replacement 10 years after the operation. Leg
length discrepancy was reduced in 17/20 hips. Overall patient
satisfaction level was good-excellent in 12 patients, fair in 4, and
bad in 2 patients. Postoperative complications included blade
migration (1 patient (and wire breakage (2 patients).
Conclusions: Morscher osteotomy can be effective for the
treatment of patients with short femoral neck and overgrowth of
the greater trochanter with a positive Trendelenburg test and
mild leg length discrepancy. A congruent nonarthritic hip joint
is a prerequisite for the success of the operation.
Level of Evidence: Level IV.
Key Words: femoral neck lengthening, Morscher osteotomy,
coxa breva
(J Pediatr Orthop 2016;00:000–000)
Coxa brevis (short femoral neck) and overgrowth of
the greater trochanter are deformities of the proximal
femur believed to be related to an ischemic impairment of
the upper femoral epiphysis. Several pathologies can
cause this deformity: Perthes disease, developmental
dysplasia of the hip (DDH), postinfectious state, post-
traumatic state and idiopathic avascular necrosis
(AVN).1,2 Regardless of the underlying cause, the ische-
mic necrosis of the proximal femoral epiphysis leads to
morphologic changes of the femoral head and femoral
neck. These changes include diminished longitudinal
growth of the femoral neck and a relative greater tro-
chanteric “overgrowth.” Subsequently, these morpho-
logic changes have direct influence on hip biomechanics
and clinical presentation.
The short femoral neck reduces the lever arm of the
hip abductor muscles and the high greater trochanter
reduces the tension of the abductor muscles, contributing
to abductor muscle insufficiency and subsequent
Trendelenburg sign and gait. Other common clinical
findings are mild leg length discrepancy (LLD), reduced
hip range of motion, impingement of the overgrown
greater trochanter in abduction, and anterior impinge-
ment in forward flexion.1–3
The purpose of surgical treatment for coxa brevis
and overgrowth of the greater trochanter is restoration of
the normal anatomy of the proximal femur and restora-
tion of limb length, thereby improving hip biomechanics,
gait, abductor force, and hip range of motion. In 1980,
Morscher developed the femoral neck lengthening os-
teotomy (FNLO) for correction of this complex de-
formity. The principle of the surgical technique is
lateralization of the femoral shaft along a double os-
teotomy, thereby lengthening the neck and the limb si-
multaneously due to the obliquity of the osteotomy.4 The
purpose of this study was to evaluate the intermediate to
long-term results of the operation,by assessing Harris Hip
Score (HHS), LLD and satisfaction at long-term follow-
up compared with preoperative assessment, and to de-
termine what proportion of hips have gone on to ar-
throplasty at long-term follow-up. To the best of our
knowledge this study contains the largest group of pa-
tients with the longest follow-up.
METHODS
The study is a retrospective case series. All data
were extracted in 3 medical centers by 3 orthopaedic
From the *Pediatric Orthopedics Unit; wRambam Health Care Center,
Haifa; yPediatric Orthopedics Unit, Ha-Emek Hospital, Afula,
Israel; and zOrthopaedic Surgery, Loma Linda University, Loma
Linda, CA.
No funding received for this study from any organization.
None of the authors received financial support for this study.
The authors declare no conflicts of interest.
Reprints: Doron Keshet, MD, Rakefet 14, Atlit, Israel. E-mail: doron.
keshet@gmail.com.
Copyright r 2016 Wolters Kluwer Health, Inc. All rights reserved.
ORIGINAL ARTICLE
J Pediatr Orthop Volume 00, Number 00, ’’ 2016 www.pedorthopaedics.com | 1
Copyright r 2016 Wolters Kluwer Health, Inc. Unauthorized reproduction of this article is prohibited.](https://image.slidesharecdn.com/eidelman2016-220326231205/75/eidelman2016-pdf-1-2048.jpg)
![surgeons, using the same criteria. We used both electronic
and paper charts, x-rays were assessed on digital software
and on hard copy radiographs. Between the years 1990
and 2013, we operated on 18 patients (20 hips). The me-
dian age at surgery was 16 years [interquartile range
(IQR): 14 to 17.5]. The median follow-up period was 7
years (IQR: 4.5 to 10). Three patients had prior pelvic
osteotomies to address acetabular pathologies. All pa-
tients that had FNLO were included in the study.
Clinical evaluation included measurement of LLD,
Trendelenburg sign and hip range of motion. Level of
function, pain and restriction of daily activity were
documented and expressed via the HHS. This was eval-
uated at the last examination before the surgery and at
the latest follow up after surgery.5,6
Radiologic assessment included plain pelvic radio-
graphs and long limb x-rays, taken preoperatively and
during follow-up.
Surgical Technique
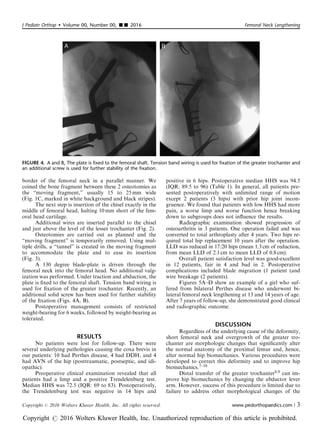
The patient lies in the supine position on a radio-
lucent operating table, with a 20-degree tilt toward the
contralateral side. The key point of the procedure is ac-
curate placement of the first K-wire. This wire should
create a neck-shaft angle of 130 degrees to assure the
correct final neck-shaft angle (Fig. 1A). It should also be
positioned in the correct anteversion, parallel to the ref-
erence wire (Fig. 1B).
Additional proximal wires are inserted at the level
of the greater trochanter and at the level of the proximal
FIGURE 1. Placement of the first K-wire. This wire should create a neck-shaft angle of 130 degrees to assure the correct final neck-
shaft angle (A). It should also be positioned in the correct anteversion, parallel to the reference wire (B). Additional proximal wires
are inserted, at the level of the greater trochanter and at the level of the proximal border of femoral neck in a parallel manner, the
“moving fragment” is marked in white background and black stripes (C).
FIGURE 2. Additional wires are inserted parallel to the chisel
and just above the level of the lesser trochanter.
FIGURE 3. Using multiple drills, a “tunnel” is created in the
moving fragment to accommodate for the plate and to ease its
insertion.
Eidelman et al J Pediatr Orthop Volume 00, Number 00, ’’ 2016
2 | www.pedorthopaedics.com Copyright r 2016 Wolters Kluwer Health, Inc. All rights reserved.
Copyright r 2016 Wolters Kluwer Health, Inc. Unauthorized reproduction of this article is prohibited.](https://image.slidesharecdn.com/eidelman2016-220326231205/85/eidelman2016-pdf-2-320.jpg)