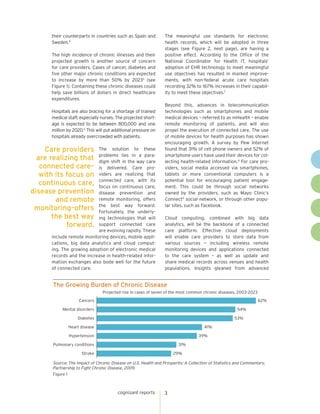
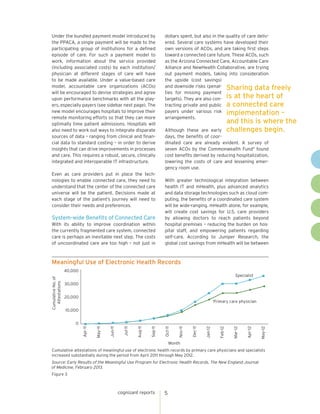
The document discusses the rise of connected care in the U.S. healthcare system. Regulatory changes and new technologies are driving a shift towards a more connected and collaborative system focused on quality of care. Connected care aims to provide the right care at the right time and place through greater data sharing and care coordination between providers. Key technologies like electronic health records, mobile devices, analytics and cloud computing will enable connected care by facilitating access to patient information across settings. However, connected care also faces challenges in standardization, physician buy-in, and integrating fragmented systems.