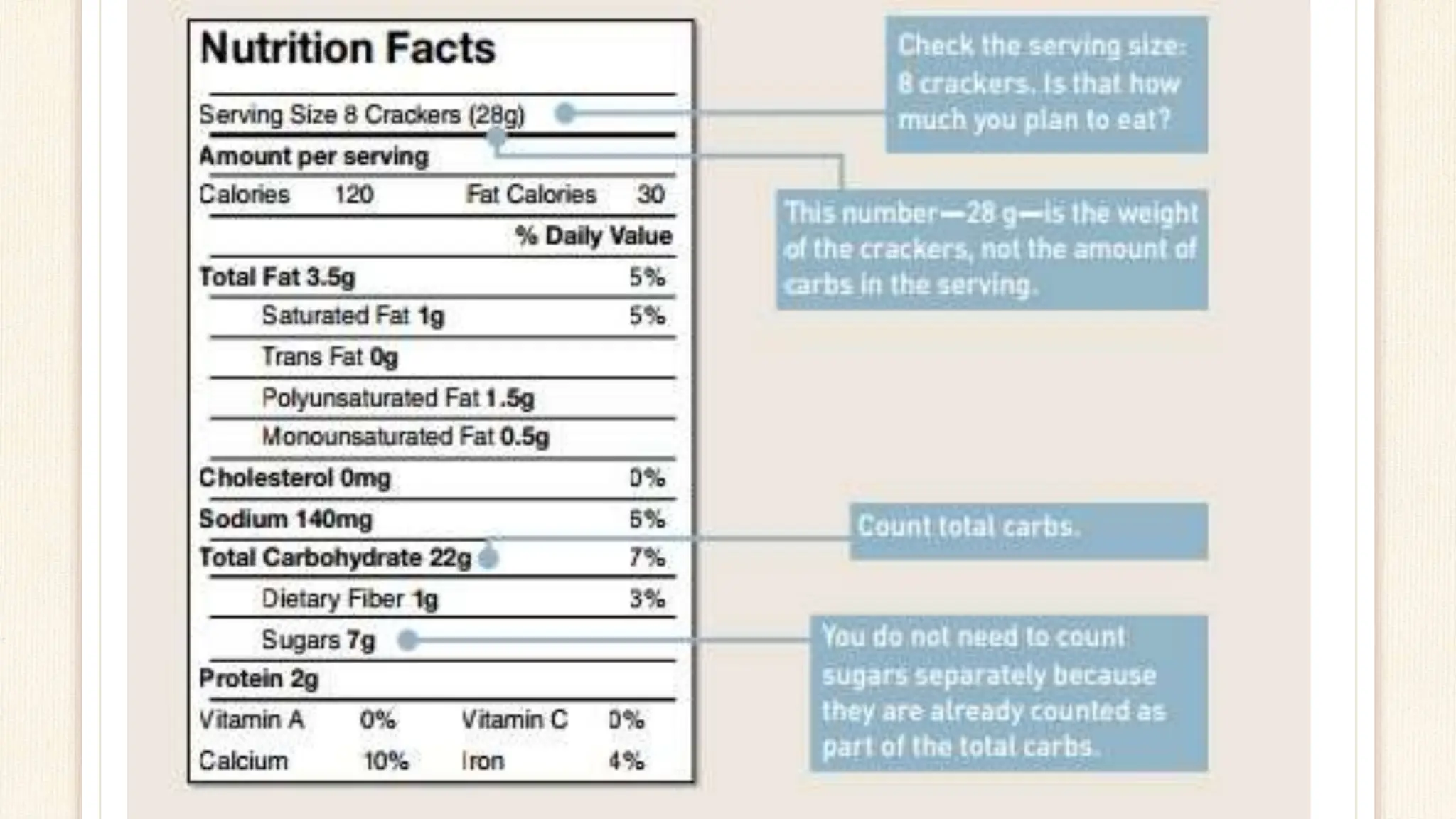
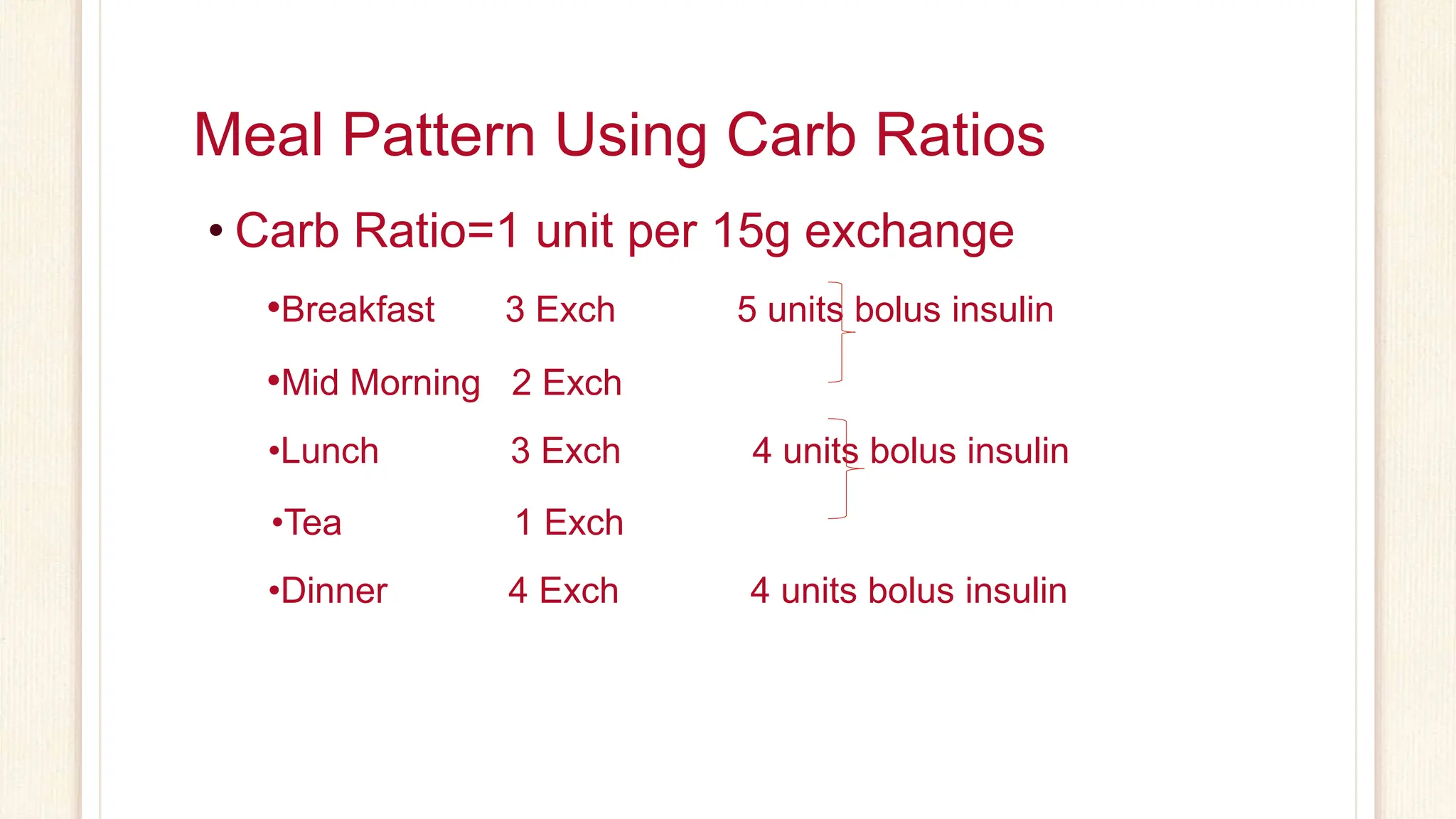
This document provides information on carbohydrate counting and calculating insulin-to-carbohydrate ratios and insulin sensitivity factors for people with diabetes. It explains that counting carbohydrates allows for flexibility in meal planning while controlling blood glucose. Examples are given for determining carbohydrate servings and exchanging units. The 1500 and 1800 rules are described for calculating insulin sensitivity factors based on a person's total daily insulin dose. Worked examples demonstrate how to use insulin-to-carbohydrate ratios and sensitivity factors to determine corrective insulin doses.