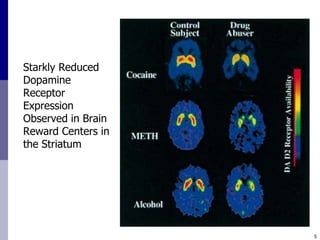
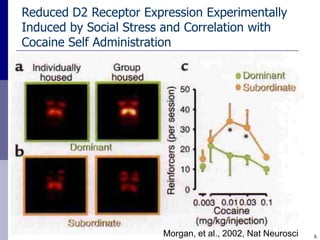
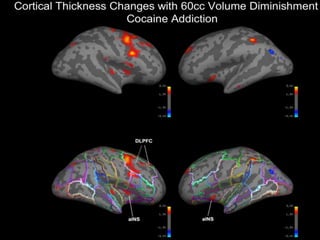
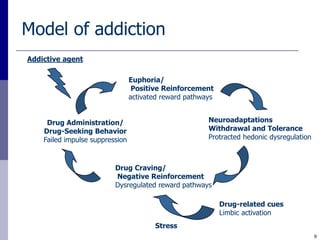
The document discusses substance misuse as the nation's number one public health problem, noting the disease of addiction, population risk factors, treatment options, and initiatives at the Center for Addiction Medicine. It provides statistics on the prevalence and economic burden of substance use disorders and details factors influencing vulnerability, effective treatment models, and the cost-effectiveness of addiction treatment.