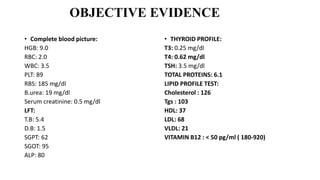
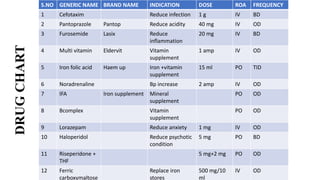
A 55-year-old female was admitted with complaints of breathlessness, generalized swelling, and abdominal distension. Laboratory tests revealed pancytopenia (low red blood cells, white blood cells, and platelets), along with vitamin B12 deficiency. She was diagnosed with pancytopenia and gross anemia due to vitamin B12 deficiency. Her treatment plan included blood transfusions, antibiotics, diuretics, vitamins, and medications to stimulate blood cell production and manage her psychiatric conditions. Close monitoring was needed due to potential drug interactions and complications from her low blood cell counts.