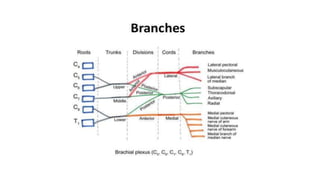
This document provides information about various upper limb nerve blocks, including anatomy, indications, techniques, advantages, and disadvantages. It discusses interscalene, supraclavicular, infraclavicular, costoclavicular, and axillary brachial plexus blocks. Landmark-guided, peripheral nerve stimulator-guided, and ultrasound-guided techniques are described for each block. Complications are also outlined.