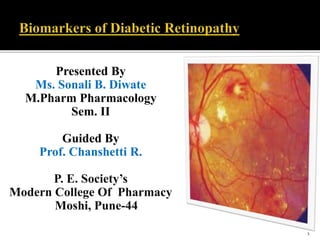
DR Biomarkers Guide Insight Into Retinopathy Risk
- 1. Presented By Ms. Sonali B. Diwate M.Pharm Pharmacology Sem. II Guided By Prof. Chanshetti R. P. E. Society’s Modern College Of Pharmacy Moshi, Pune-44 1
- 2. Introduction to Diabetic Retinopathy Types of Diabetic Retinopathy Pathogenesis Risk factors Diagnosis Management of DR Introduction to Biomarkers Biomarkers of DR Conclusion References 2
- 3. Retinopathy (damage to the retina) caused by complications of diabetes. Which can eventually lead to blindness. It is an ocular manifestation of diabetes, a systemic disease. Affects up to 80 percent of all patients who had diabetes for 10 years or more. 3
- 4. 4
- 5. Definition: Is a complication of diabetes and a leading cause of blindness. It occurs when diabetes damages the tiny blood vessels inside the retina, the light-sensitive tissue at the back of the eye. (See diagram below.) A healthy retina is necessary for good vision. 5
- 6. 6
- 7. Clinical classification: 1. Non-proliferative diabetic retinopathy 2. Proliferative diabetic retinopathy. 7
- 8. 8
- 9. 1. Non-proliferative diabetic retinopathy: The lesions in the retina at this stage are within the retina and include: micro-aneurysms, small ‘dot and blot’ hemorrhages, ‘splinter’ hemorrhages, Intraretinal Microvascula Abnormalities (IRMA) and ‘cotton wool’ spots. 9
- 10. Proliferative Diabetic Retinopathy: The unchecked progression of proliferative diabetic retinopathy can lead ultimately to tractional retinal detachment, which may or may not involve the macula. Vitreous haemorrhage may require B-scan ultrasonography to determine if a tractional or rhegmatogenous (retinal break or hole) retinal detachment is present. 10
- 11. Four stages: 1. Mild Nonproliferative Retinopathy. At this earliest stage, microaneurysms occur. They are small areas of balloon-like swelling in the retina's tiny blood vessels. 2. Moderate Nonproliferative Retinopathy. As the disease progresses, some blood vessels that nourish the retina are blocked. 11
- 12. 3. Severe Nonproliferative Retinopathy. Many more blood vessels are blocked, depriving several areas of the retina with their blood supply. 4. Proliferative Retinopathy. At this advanced stage, the signals sent by the retina for nourishment trigger the growth of new blood vessels. This condition is called proliferative retinopathy. 12
- 13. Diabetic retinopathy is the result of microvascular retinal changes. Hyperglycemia-induced intramural pericyte death and thickening of the basement membrane lead to incompetence of the vascular walls. These damages change the formation of the blood-retinal barrier and also make the retinal blood vessels become more permeable. 13
- 14. 14
- 15. Duration of Diabetes Poor control of Diabetes Pregnancy Hypertension Nephropathy Obesity & Hyperlipidemia Smoking 15
- 16. Diabetic retinopathy is detected during an eye examination that includes: 1. Visual acuity test 2. Pupil dilation 3. Ophthalmoscopy 4. Fundus Fluorescein angiography(FFA) 5. Digital Retinal Screening Programs 6. Slit Lamp Biomicroscopy Retinal Screening Programs 16
- 17. 1.Laser surgery, 2.Injection of corticosteroids or Anti-VEGF into the eye 3.Vitrectomy 17
- 18. A biomarker is a substance or activity that can be measured and serves as a marker of a specific biological activity. A biomarker may be a substance measured in the blood or urine, for example, or may be a measurement of a parameter such as blood pressure or brain activity. 18
- 19. It improve the understanding of a disease process. It predicts disease severity/complications. Improves treatment targeting. Monitor treatment efficacy. 19
- 20. Novel Biomarkers 1. Plasma alpha 2 antiplasmine complex(PAP) 2. fibrinogen 3. Serum Apolipoprotein AI and B 4. Retinal arteriolar tortuosity 5. Urinary Albumin-to-Creatinine (UAC) ratio 20
- 21. Inflammatory biomarkers: 1. C- Reactive Protein (CRP) 2. IL6- Interleukin 6 3. PgE1- Prostaglandin E1 4. PgE2- Prostaglandin E2 21
- 22. Serum lipids: 1. Triglycerides 2. Low density lipoprotein 3. Total cholesterol 22
- 23. Other Biomarkers: 1. Vascular Endothelial Growth Factor (VEGF) 2. Homocysteine 3. Cytokinine 23
- 24. Fibrinogen (factor I) is a soluble, plasma glycoprotein, that is converted by thrombin into fibrin during blood clot formation. Fibrinogen is synthesized in the liver by the hepatocytes. The concentration of fibrin in the blood plasma is 200-400 mg/dL . 24
- 25. An increased blood viscosity due to high fibrinogen level as well as an elevated intravessel pressure play a role in the development of diabetic retinopathy the patients with the severest retinopathy had the highest fibrinogen concentrations fibrinogen metabolism is increased in diabetes and bears a relationship to diabetic retinopathy 25
- 26. The apolipoproteins associated with serum lipoprotein particles give structural stability as well as regulatory control in lipid metabolism. The association between lipids and diabetic retinopathy (DR) remains unclear. 26
- 27. Only a few studies have reported the association between proliferative diabetic retinopathy (PDR) and the serum concentrations of apolipoprotein A1 (apoA1), apolipoprotein B (apoB) and apolipoprotein E (apoE). 27
- 28. Low apolipoprotein A1/apolipoprotein B ratio in serum was associated with PDR in type 2 diabetic patients of long duration. ApoA1 overexpression is an early event in the retina of diabetic patients and can be involved in the physiopathology of diabetic retinopathy. 28
- 29. The blood vessels become tortuous, i.e. they become dilated and take on a serpentine path. The dilation is caused by radial stretching of the blood vessel and the serpentine path occurs because of longitudinal stretching. In persons with diabetes, increased arteriolar tortuosity was associated with mild and moderate stages of DR. This suggests that retinal vascular tortuosity might be an early indicator of microvascular damage in diabetes 29
- 30. C-reactive protein (CRP) is a protein found in the blood, the levels of which rise in response to inflammation (i.e. C-reactive protein is an acute-phase protein). higher levels of CRP were more likely to have PDR 30
- 31. Acts as both a pro-inflammatory cytokine and an anti-inflammatory myokine. In humans, it is encoded by the IL6 gene. IL-6 is secreted by T cells and macrophages to stimulate immune response, e.g. during infection and after trauma, especially burns or other tissue damage leading to inflammation. 31
- 32. Increased levels of interleukin-6 (IL-6) are detected in vitreous fluid of patients with PDR and diabetic macular edema. 32
- 33. Diabetic retinopathy is a complication of diabetes and a leading cause of blindness. It occurs when diabetes damages the tiny blood vessels inside the retina, the light-sensitive tissue at the back of the eye. The prevalence of diabetic retinopathy is increasing worldwide. interleukin 6 (IL-6), and C-reactive protein (CRP) are two inflammatory markers which have been shown to predict the development of diabetic retinopathy. 33
- 34. Recent studies have suggested that,Plasma alpha 2 antiplasmine complex, fibrinogen, Serum Apolipoprotein AI and B,Retinal arteriolar tortuosity,Urinary Albumin-to- Creatinine (UAC) ratio are the novel biomarkers for DR and that might be a better predictor of diabetic retinopathy. 34
- 35. 1)Harsh Mohan, Textbook of Pathology, 5th edition 2005, published by JAYPEE brother’s medical publishers (P) LTD, 133. 2)Thanh T., Ekaterina A., Inflammatory, Hemostatic, and “Other Novel Biomarkers for Diabetic Retinopathy” Diabetes care, volume 32, number 9, September 2009. 3)Izuora KE, Chase HP, Jackson WE, Coll JR, Osberg IM, Gottlieb PA, Rewers MJ, Garg SK. Inflammatory markers and diabetic retinopathy in type 1 diabetes. Diabetes Care 2005;28:714–715 35
- 36. 4)Mohamed Q, Gillies MC, WongTY. Management of diabetic retinopathy: a systematicreview.JAMA2007;298:902–916. 5) Brazionis L, Rowley K, Sr, Itsiopoulos C Harper CA, O’Dea K. Homocysteine and diabetic retinopathy. Diabetes Care 2008; 31:50–56 36
- 37. 37 Thank You