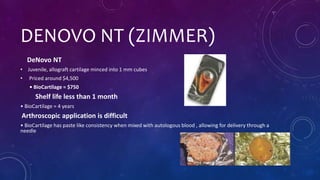
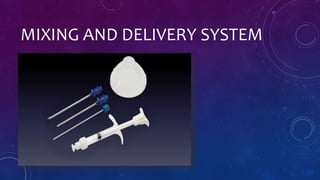
This document discusses biocartilage as a potential treatment for cartilage damage and diseases. Biocartilage is made of micronized allogeneic cartilage that has been dehydrated. It is implanted along with platelet rich plasma over a microfractured cartilage defect. This allows mesenchymal stem cells to attach to the cartilage extracellular matrix scaffold. Research in baboons found biocartilage implants led to hyaline-like new cartilage formation within 9 weeks. Biocartilage may provide a lower-cost and more effective alternative to other cartilage treatments like microfracture alone or products using minced juvenile cartilage. Further clinical studies in humans are still needed but biocartilage shows promise as a cartilage repair